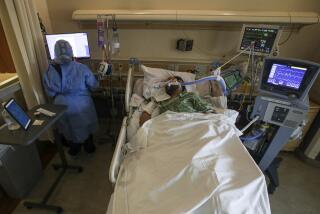
How this coronavirus kills its victims
- Share via
SAN FRANCISCO — The new coronavirus spreading rapidly around the globe can be deadly because it targets a very vulnerable and essential part of the body — the lungs.
The coronaviruses that can set you back with a common cold typically infect just the nose, sinuses and throat. But it’s more common for the one responsible for COVID-19 to spread into the cells of the airways and lungs as well.
“The virus basically hijacks the cell and reprograms it genetically to make more copies of virus,” said Dr. Otto Yang, a UCLA expert on infectious disease.
Then it begins its attack.
About 86,000 people around the world have been infected with the novel coronavirus from China, and 2,977 have died. The first fatality in the U.S. was reported on Saturday.
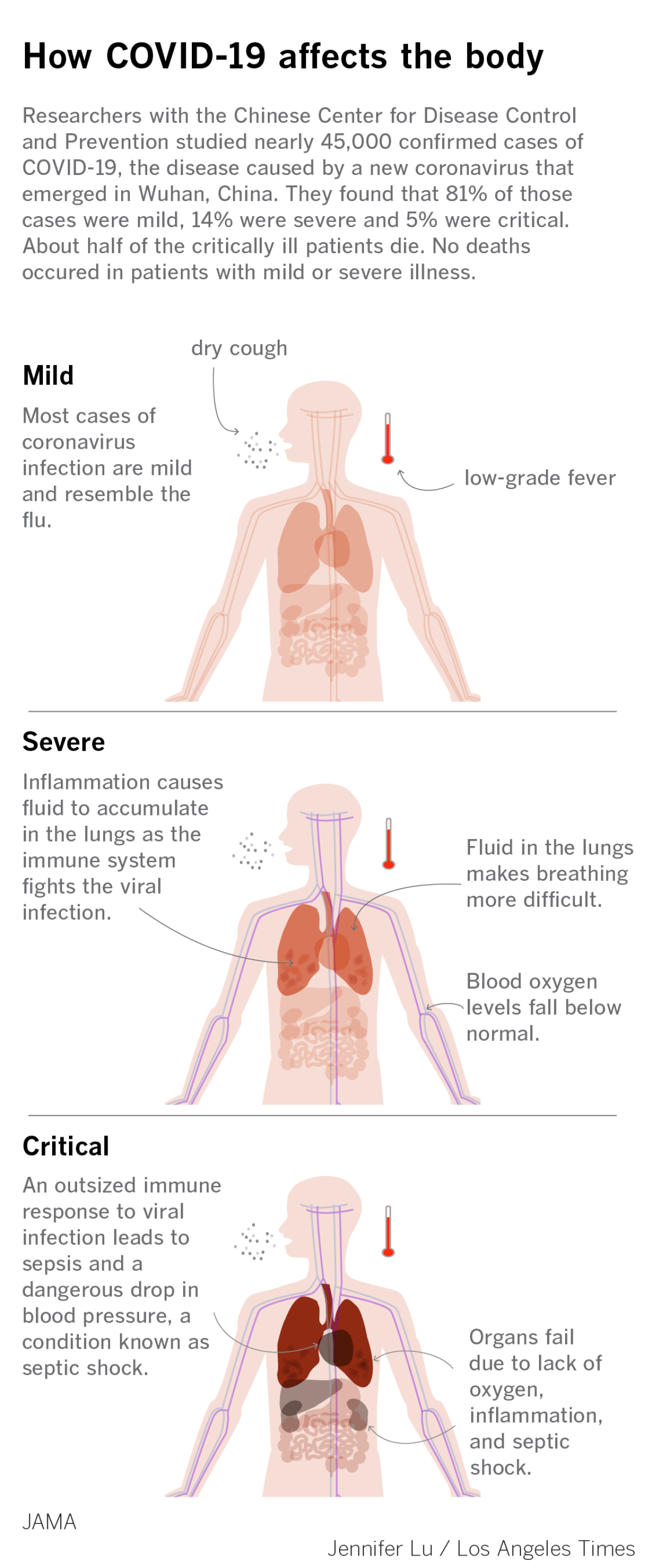
An analysis of nearly 45,000 patients in China revealed that the vast majority of those cases — 81% — caused only minor illness. An additional 14% had symptoms described as “severe.” Just 5% of the cases were deemed “critical,” and half of those infections resulted in death.
Here’s what doctors and scientists have pieced together about how the coronavirus kills.
Destruction of the lungs
As the virus starts to destroy the lungs, “people become unable to breathe properly,” Yang said.
Even worse, the body’s efforts to fight the virus can cause inflammation in the lungs — making breathing even more difficult.
Blood vessels damaged in the war between the virus and immune system may begin leaking fluid into lung tissues, which can be visible as white spots on chest X-rays.
The fluid may drown some of the lung’s tiny air sacs, preventing them from delivering oxygen to the blood and removing carbon dioxide. It is this kind of inflammation and destruction that is called pneumonia.
“The immune cells are like police officers or soldiers,” Yang said. “If you have a small infection — so a small number of criminals — they can come in and they can effectively clear out the problem people without much collateral damage.”
On the other hand, he said, “if you have a huge crowd of criminals all at once, and a huge crowd of soldiers all at once, then you have tons of collateral damage because it’s a big clash.”
Breathing problems
The analysis of patients in China reported that severely ill patients suffered from symptoms like shortness of breath and low levels of oxygen in the blood. Chest X-rays and CT scans of the lungs showed most of the organs covered in fluid.
Some of the severely ill were taking more than 30 breaths a minute — well above the normal rate of 12 to 20 breaths a minute.
“Even though each breath is not working as well as it should, if you take enough breaths, you can make up for that, and still breathe on your own,” Yang said.
Attack on the kidneys
The lungs aren’t the only target. The coronavirus also has the ability to latch on to, hijack and destroy cells of the kidneys, Yang said.
The kidneys play an essential role in removing waste from the blood. When they fail, toxic levels of waste can pile up in the body.
Respiratory failure
Patients are considered critically ill if they can no longer breathe on their own.
If this happens, patients are fitted with special masks that deliver very high concentrations of purified oxygen into the mouth, or they can be put on a ventilator, Yang said. This involves placing a tube into the throat so the machine can push oxygen directly into the lungs.
Septic shock
Despite treatment, the battle between the virus and the immune system may cause collateral damage throughout the body.
“It’s no longer just limited to the lungs,” Yang said. “There’s this inflammation that’s all throughout the whole body now.”
That starts a chain reaction that can destroy other organs and cause blood pressure to fall to dangerously low levels.
Septic shock is a bodywide response in which the immune system is trying to attack the virus everywhere. Unfortunately, the inflammation caused by the immune system damages human cells throughout the body.
“It’s a process that can be triggered by any severe infection,” Yang said.
Multiple organ dysfunction or failure
If the disease progresses, organs can start failing. This could be the result of the virus’ direct attack, as with the lungs and kidneys, or because of septic shock.
The ways in which people die of COVID-19 are actually quite similar to the way people can die of the flu — even though influenza viruses are very different from coronaviruses.
“You can think of it as a final common pathway,” Yang said. “The criminals coming in may be different. But the final effect is the same.”
The effect of age
The oldest patients have faced the greatest risk of death, according to the study of Chinese patients by researchers with the Chinese Center for Disease Control and Prevention.
While the overall case fatality rate of the patients in the study was 2.3%, it was 8% for those in their 70s and 14.8% for patients 80 or older.
In a surprise, there were no deaths among infants, toddlers or children younger than 10. That’s odd because with other respiratory illnesses such as the flu, the very young and the very old face the greatest risk of death.
“The virus seems to be really benign in children,” Yang said. “That applies even to children under the age of 1, which is really odd. Normally, children under the age of 1 are very susceptible to a lot of things.”
One possible explanation for this is that children have less-developed immune systems, he said. In this case, an immature immune system might prevent the body from triggering inflammation severe enough to result in pneumonia, septic shock and multiple organ failure.