Organ transplants plummeted as the coronavirus spread, study says

- Share via
Organ transplants plummeted as the coronavirus swept through communities, with surgeons wary of endangering living donors and unable to retrieve possibly usable organs from the dead. Even when doctors were willing and able, hospitals dealing with COVID-19 patients were sometimes too full to accommodate them.
Between late February and early April, deceased donor transplants — the most common kind — dropped by about half in the U.S. and plunged 90% in France, researchers reported Monday in the journal Lancet.
Transplants from living donors had a similarly staggering dive, according to the United Network for Organ Sharing, which runs the U.S. transplant system. There were 151 living donor transplants in the U.S. in the second week of March when a pandemic was declared. By the week of April 5, there were only 16 such transplants, according to UNOS.
It’s too soon to know how many people waiting for a lifesaving organ transplant may die not from COVID-19 infection but because the pandemic blocked their chance at a new organ. Kidney transplants make up the vast majority of the drop, but heart, lung and liver transplants declined, too.
Living donations might be rescheduled, but missed organs from a deceased donor are lost opportunities, wrote the study team led by Dr. Alexandre Loupy, a kidney specialist who heads the Paris Transplant Group.
More recent counts by UNOS show that transplants started inching back in late April, with U.S. hospitals trying to decide how to safely ramp up.
Geographic variation could offer important lessons, said Dr. Peter Reese, a transplant nephrologist and epidemiologist at the University of Pennsylvania who worked on the Lancet study.
“Transplant centers and patients really want to get going again, but there are all these questions,” said Reese, whose team is collecting data from Canada and other parts of Europe for a closer look. “We need to be finding places that maintained their transplant rates and finding out what they did.”
Hospitals worldwide postponed all kinds of medical care as they were flooded with COVID-19 patients. Decisions about transplants are among the trickiest. They’re not elective surgeries, but patients must take immune-suppressing medicines to prevent rejection of their new organ — putting them at greater risk if they encounter the virus.
During the coronavirus outbreak, people with conditions like diabetes and kidney disease are adapting their medical routines to avoid exposure.
The larger drop seen in France may be due to more centralized public health policies than in the state-by-state variations in the U.S., Reese said.
“That equation changes depending on what area of the country you’re in,” agreed Dr. Abhinav Humar, transplant chief at the University of Pittsburgh Medical Center. His transplant center, still running, has taken in patients from New York and other harder-hit areas who needed a new liver, had a willing living donor and “can’t afford the luxury of waiting two or three months at least” in hopes their original hospital could take them back.
In an average month, New York does about 220 transplants statewide. In the first weeks of April, that had dropped to 23, Samantha Delair of the New York Center for Liver Transplantation told a recent UNOS video conference.
In contrast, UC San Francisco has seen small transplant drops, said Dr. Chris Freise, the interim transplant director there.
“We’re one of the few centers that kept going through all of this, but it was not without a lot of careful thought,” said Freise, who needed daily updates in deciding what transplants were safe to schedule. He said he remains on guard as California’s social distancing restrictions are gradually lifted.
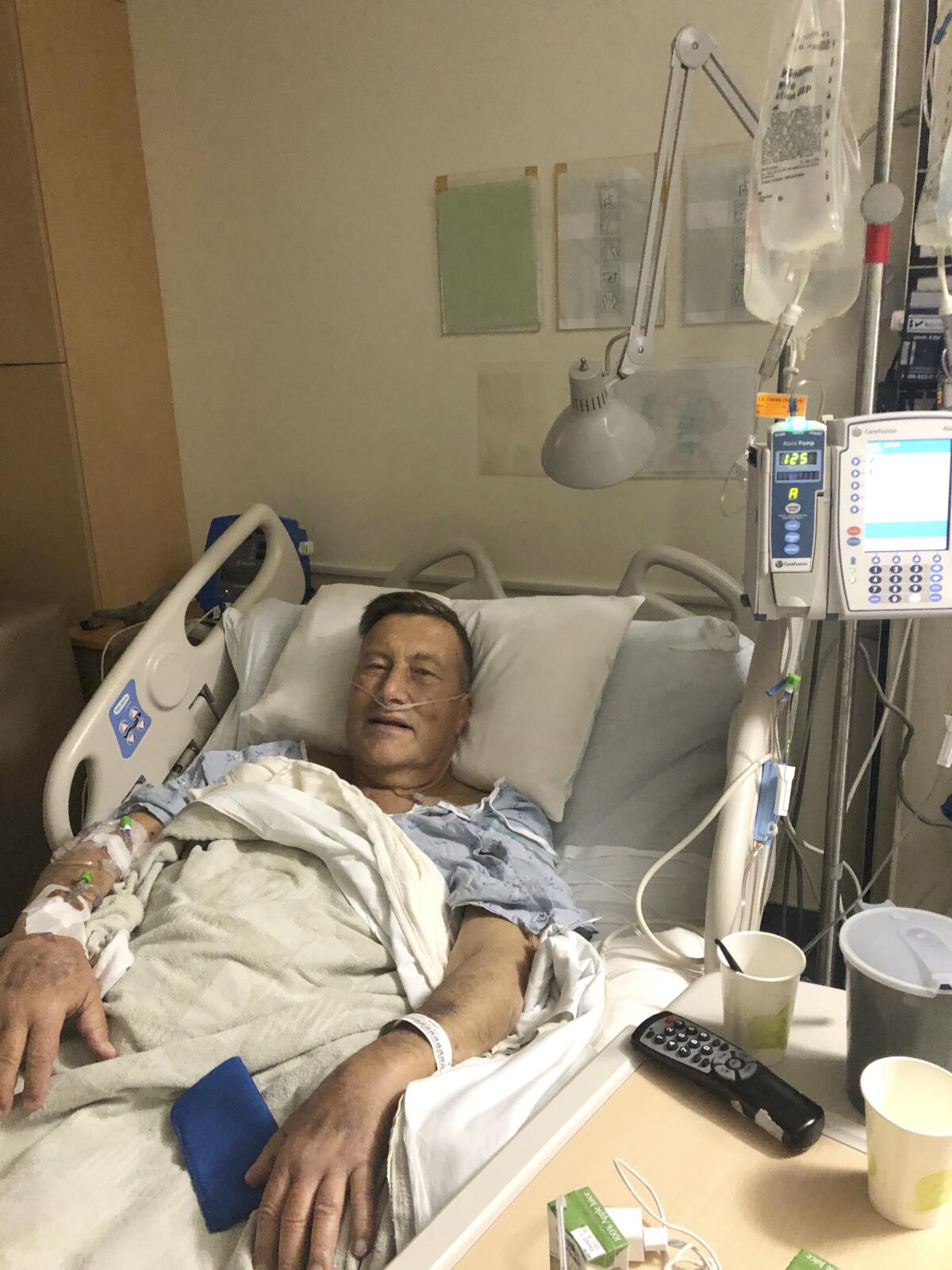
For example, Freise’s team allowed living kidney transplants for people like Herb Hoeptner, who was on the brink of needing dialysis.
“When you have kidneys that have nothing left, you either go on dialysis or you die. That was much more of a concern to me than coronavirus,” Hoeptner said.
The 66-year-old from Gilroy, Calif., realized only after his March 31 surgery how rare a transplant during the pandemic was.
“I was extremely lucky,” added Hoeptner, whose wife, Diane, was his donor and rebounded quickly from the surgery.
In places where COVID-19 is more widespread, living donors are understandably nervous. “We don’t yet have a way to talk to living organ donors about what’s a reasonable risk,” Reese said.
A diagnosis of breast cancer is always accompanied by angst and uncertainty. It’s even more fraught when it comes in the midst of the coronavirus crisis.
Deceased donations are even more complicated. Early on, testing shortages made it hard to be sure would-be donors who died of something unrelated like a car crash were virus-free, a problem that’s easing. Still, hospitals don’t want out-of-town surgeons visiting to retrieve organs and can’t always spare a local surgeon to do the job, or find a plane to fly the organs where they need to go.
Surgeons must weigh if it makes sense to accept less-than-perfect organs that might work but could keep the recipient hospitalized for longer.
Dr. David Axelrod , a University of Iowa kidney surgeon, said his team is “trying to be careful about it, trying to make sure that they’re organs that we think people can come in and get transplanted successfully and go home quickly.”