Coronavirus offers new challenges to people trying to manage diabetes and kidney disease

- Share via
After nearly six years waiting for a kidney transplant, Amar Abu-Samrah found out late last year that she was near the top of the list. In mid-March, the coronavirus outbreak forced the transplant center to postpone most procedures.
Since then, Abu-Samrah, 24, has been trying to limit her potential for exposure to the novel coronavirus as much as possible: She’s doing more doctor appointments over the phone and avoiding hospital waiting rooms when she goes in for lab work. The Westminster resident, who lives with her parents, is even limiting contact with family members to mealtimes, knowing her kidney failure puts her at high risk if she contracts COVID-19.
“It makes me anxious,” she said. “I’m like, OK, how much longer do I have to wait?”
The coronavirus outbreak has placed an additional emotional and safety burden on people with underlying health conditions, like chronic kidney disease, diabetes and high blood pressure. The pandemic has pushed routine doctor visits to telemedicine and made outings for picking up medicine, getting blood drawn or dialysis treatment yet another risk for exposure.
Stay-at-home orders and social distancing guidelines have caused many surgeries and in-patient treatments to be postponed. The University Medical Center of Southern Nevada, where Abu-Samrah hopes to get a kidney transplant, stopped performing transplants for all but the hardest to match individuals in mid-March to protect the health of its immunocompromised patients. The center resumed transplants this week, according to a spokesman.
A diagnosis of breast cancer is always accompanied by angst and uncertainty. It’s even more fraught when it comes in the midst of the coronavirus crisis.
Early data suggest that people with underlying health conditions who contract the coronavirus are more likely to be hospitalized and suffer adverse outcomes. An April 22 report published by the Journal of the American Medical Assn. found that, among COVID-19 patients admitted to 12 New York City metropolitan area hospitals from March 1 to April 4, 33.8% had diabetes and 56.6% had high blood pressure.
“People with diabetes are so aware of the risks that they face in daily life with different types of conditions or things like coronavirus,” said Mila Clarke Buckley, who runs the Hangry Woman blog on living with diabetes. “While it’s scary and we’ve never seen this before, we’re all just trying to do the best we can in this really stressful situation, and that’s all that we can do at this point.”
Clarke Buckley, a 30-year-old Houston resident who was diagnosed four years ago, said her blood sugar levels have been trending higher than usual because of stress and a lack of sleep. Having to adapt her diet due to shortages at the grocery store hasn’t helped, but she said she’s focused on managing her levels to reduce the risk of complications that might require a hospital visit.
Her doctors’ office is open and observing social distancing practices, and Texas has started a phased reopening, but she said she plans to stick to telemedicine appointments, even if it means missing or postponing her quarterly blood work.
“I know that that comes with the risk of not getting all of my labs done,” she said. “But especially because Texas is so lax about it, I just don’t feel safe going outside or being in a place where I know there might be a lot of people.”
Many clinics, including the Joslin Diabetes Center in Boston, have transitioned to conducting routine visits, such as those to discuss lab results or refill prescriptions, over the phone or by videoconference. But the center is still prepared to see people in-person when necessary. If, for example, a person with diabetes experiences changes in eyesight — such as floaters and blurry or obstructed vision — those could be caused by a burst blood vessel and must be treated immediately to prevent loss of vision, said Dr. Robert Gabbay, the chief medical officer and senior vice president of the center.
And although some questions can be answered in a phone call, teaching newly diagnosed patients how to inject insulin requires a personal touch that can’t be replicated digitally.
“Although they can watch a video, it’s not quite the same, because there’s sort of an emotional component, where having that connection to somebody and trust to guide them on the process is important,” Gabbay said.
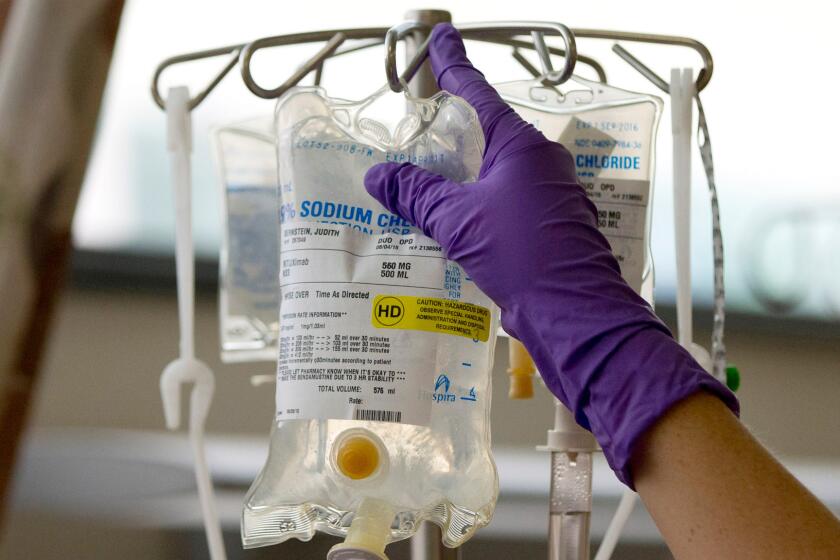
Other critical services have continued, with enhanced safety precautions. The Centers for Disease Control and Prevention estimates that about 15% of American adults, or about 37 million people, have chronic kidney disease. About 500,000 with end-stage renal disease need to visit dialysis clinics three times a week for hemodialysis treatments that filter waste and extra fluids from their blood. A much smaller number of patients undergo nightly peritoneal dialysis treatments at home using a catheter in their abdomens.
Skipping some of those appointments could lead to complications like high potassium levels in the blood or heart failure that would require hospitalization, said Dr. Joseph Vassalotti, the National Kidney Foundation’s chief medical officer.
“In this time, when people are trying to stay home most of the time and pay attention to social distancing, we do have to emphasize the importance of dialysis treatments as being part of maintaining health,” he said.
Due to Coronavirus, many patients have stopped going to community clinics, putting funding at risk
At clinics run by DaVita, one of two major for-profit dialysis centers, patients are screened before entering the building, and people with confirmed or suspected coronavirus infections are treated in separate areas. Everyone in the clinic must wear a new mask and gloves, and patients are no longer allowed to have visitors during their sessions, which last about four hours.
Even with the new precautions, employees at DaVita and other clinics say there have been shortages of personal protective equipment and a lack of transparency about cases at clinics, said Steve Trossman, a spokesman for the SEIU-UHW, a union that represents healthcare workers.
The new process is “tedious, but it’s necessary,” said Andrew Cunningham, a 69-year-old from Laguna Woods, who has been on hemodialysis since being diagnosed with kidney failure in 2018.
He said he recently joked to one of the nurses at the DaVita clinic he visits near his home that he felt like calling in sick to dialysis that morning. “I said, ‘I forgot, I don’t have any sick days,’” he said. “We have to go. If you miss two, three sessions, it could be deadly.”

Cunningham is part of a kidney disease support group based out of Saddleback Church in Lake Forest that meets twice a month. The coronavirus outbreak has forced the group to move meetings to Zoom, and attendance has doubled at a recent session, said Helen Mills, who founded the group nine years ago with her husband, Bill.
The group includes people whose kidney failure was caused by autoimmune diseases, polycystic kidney disease and diabetes, as well as members like Bill Mills, 84, who are now living with transplants.
Several attendees said they rarely go out, except for doctor visits, and rely on their family and friends to run errands. People with kidney failure receiving dialysis and kidney transplant recipients have weakened immune systems and higher risks of infection, and many family members are keeping that in mind as they try to limit their own exposure to the virus.
“The spouses of all the transplant people that we know are staying as quarantined, almost as quarantined, as the patient themselves,” Helen Mills, 71, said. “It doesn’t do Bill any good to stay home if I’m going to go out without a mask and bring germs. So we’re both exceptionally cautious.”
Jacquie Woolsey, 71, said she’s been avoiding crowds during the flu season since 2019, when she spent five days in the hospital with pneumonia. Woolsey, a member of Mills’ group who received a kidney transplant in 2016, said she and her husband have largely stayed home and are sanitizing the items they bring into the house. When her husband does run errands, he leaves his shoes outside and sprays them with alcohol.
It’s not clear when people with underlying health conditions will be able to return to their normal routines. Several states, including California, have started to loosen restrictions under their stay-at-home orders, but there are still gaps in testing and contact-tracing capacity. Without a vaccine, epidemiologists estimate that about 70% of a population would need to contract COVID-19 to develop herd immunity and protect everyone else, but it’s not clear how long immunity would last, if it exists at all.
Given the uncertainty about the future of a vaccine, people who are most at risk of complications from the coronavirus will probably have to decide for themselves whether they feel safe in reopened states. Woolsey, who lives in Orange, said she wants the government to reopen the state and trust her to protect herself.
“I like to be treated like I’ve got a brain, that I’m not going to go out and do something stupid,” she said. “I know I’m a senior. I know I have a lowered immunity system. I’m fully aware of that.”
Sharon Abar, another member of the group, said she wouldn’t feel “completely comfortable” until there is a vaccine or a better testing infrastructure. “At least there has to be some kind of baseline of knowing who’s infected and who’s not, and we don’t have that,” said the 60-year-old Long Beach resident.
Abar, whose renal failure was caused by polycystic kidney disease, said she’s concerned about the number of people not wearing masks. “The masks aren’t so much for us, it’s to protect other people,” she said. “I guess they don’t really care about protecting other people, and I feel bad about that.”
Abu-Samrah said she’s also hoping for a vaccine, and after seeing people in her area and nearby Huntington Beach push back against stay-at-home orders, she’s not sure she’ll feel at ease once the state reopens. And if she does get scheduled for a kidney transplant soon, she’s worried the anti-rejection medication she’d need to take would weaken her immune system more than her nightly peritoneal dialysis treatments at home.
“You’re going to have to pick and choose, I guess,” she said.