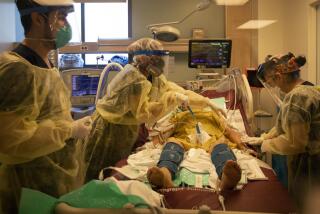
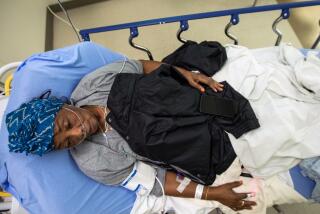
Cause of death: COVID-19, police violence or racism?

- Share via
Doctors and public health experts will tell you that, compared to white Americans, African American people die prematurely and disproportionately of many ills: heart disease, stroke, COVID-19, police violence.
The proximate causes of these early deaths vary. But there is a sameness to the pattern, experts say, and a common source of the skewed statistics.
Racism — not in its overt, name-calling form, but the kind woven deeply into the nation’s institutions — harms the 44 million Americans who identify as black and potentially shortens their lives, according to those who study racial inequities in health. For some, including Minnesotan George Floyd, it causes premature death in minutes. For others, a lifetime of disadvantage takes its toll in subtler ways.
“At the end of the day, racism is the original sin here,” said Dr. Georges Benjamin, executive director of the American Public Health Assn. “Racism attacks people’s physical and mental health,” he said. It’s “an ongoing public health crisis that needs our attention now.”
And in the midst of a pandemic, Benjamin and others fear that as crowds fill the streets to protest yet another police killing of an unarmed black man, people of color will again bear the disproportionate brunt of renewed infections.
It is an agonizing trade-off, they acknowledge. But it’s hardly a choice.
“I’ve spent the last several months of my life imploring and exhorting people to protect themselves, to reduce the spread of this virus and save lives,” said Dr. Clyde W. Yancy, a cardiologist at Northwestern University’s Feinberg School of Medicine who is African American. But after Floyd’s death under the knee of Minneapolis police officer Derek Chauvin, he said, “it dawned on me that my greatest risk is not COVID-19. It’s the color of my skin.”
It dawned on me that my greatest risk is not COVID-19. It’s the color of my skin.
— Dr. Clyde W. Yancy, cardiologist at Northwestern University
Dr. Atheendar Venkataramani, an internist and health policy researcher at the University of Pennsylvania, has plumbed the power of despair to erode the health of specific American populations. He was part of a team that assessed changes in the mental health of Americans who lived in states where at least one unarmed black man had been killed by police.
In the three months following these deaths, the team found a measurable drop in mental health among black Americans — and the more deaths there were, the greater the effect. Mental health did not suffer in cases when police killed a black person with a weapon.
The mental health of white Americans was not associated with fatal police encounters involving either armed or unarmed black Americans. The findings were published in 2018 in the medical journal the Lancet.
“It’s not like we’re giving them a choice here,” Venkataramani said of the latest spasm of protests. The neglect of African Americans’ economic, social and health problems has been “so pernicious, so ingrained and so predictable,” he added, “how could you not be out there calling attention to these issues?”
Officials fear protests are ‘super-spreader’ events for coronavirus. Marchers say worth the risk
In medical language, racism, including the kind baked into so many U.S. institutions, is a toxin. Just like polluted air, chronic stress and malnutrition — all of which often flow from racial injustice — its effect is corrosive.
An African American baby born in 2017 has a life expectancy that’s 3.5 years shorter than that of a white baby. If current inequities persist, the black baby will be nearly 2.5 times more likely to live in poverty, almost twice as likely to leave school before getting a high school diploma and more than six times as likely to be incarcerated than the white one.
Along the way, the average African American will live in poorer housing, have less access to healthy foods and be more exposed to environmental pollutants and violent crime than his or her white counterpart. He or she is more likely to suffer from obesity, asthma, diabetes, heart disease and high blood pressure.
Despite this, studies show that many physicians discount the ills reported by African American patients, engendering a mistrust that often discourages them from seeking prompt medical care.
In recent months, inequities like these have contributed to starkly higher coronavirus casualties among African Americans than white Americans. An analysis of survey data from Johns Hopkins University found that coronavirus infection rates were three times higher in counties with predominantly black populations than in predominantly white ones, and COVID-19 death rates were six times higher.
In both California and New York, African American adults have been overrepresented among COVID-19 deaths by a factor of two. In Michigan, their share of COVID-19 deaths is three times greater than their share of the population.
The death rate in Los Angeles County is far greater for Native Hawaiian/Pacific Islander, black and Latino residents than for white people, data show.
Bridget Goosby, a University of Texas sociologist who studies health disparities, said the COVID-19 pandemic has left many African American communities in a particularly depleted state.
The “essential worker” designation of many low-wage jobs filled by people of color — delivery drivers, hospital workers, grocery store clerks — had set the stage for many to feel unfairly exposed to danger.
For many, that sense was deepened by stories like those of Deborah Gatewood, an African American phlebotomist in Detroit who died after the hospital where she had worked for 31 years denied her a coronavirus test four separate times, and of Brittany Bruner-Ringo, an African American nurse who was ordered to admit a visibly sick patient to an upscale dementia care center in Los Angeles and died of COVID-19 one month later.
It took months for many states to begin collecting data that confirmed a widely held suspicion: that the pandemic was taking a far heavier toll on blacks than on whites.
Then, in mid-May, data from New York City’s Police Department revealed that 93% of their arrests made to enforce social distancing rules were of black and Latinos. Meanwhile, armed white protesters calling for their states’ “liberation” were hailed by President Trump.
Amid so much loss of life, many of the places African Americans would normally turn to for comfort and strength — including churches and beauty shops — have been closed by the pandemic, Goosby said. Even extended families have been kept apart.
“There’s a collective grief,” she said. “And you’re already deprived of having this social net, of being able to grieve with people. You don’t feel like your grief is acknowledged, or that anything has changed.”
About 1 in 1,000 black men and boys in America can expect to die at the hands of police. That risk is 2.5 times higher than for white men, new research shows.
Into this tinderbox of pain, throw the match of Floyd’s graphically documented killing.
To anyone who has been paying attention, “nothing about this is surprising,” Goosby said.
In a recent essay in the Journal of the American Medical Assn., Yancy wrote that COVID-19’s heavy toll on African Americans had brought forth a long-awaited “moment of ethical reckoning.”
The United States “has needed a trigger to fully address healthcare disparities,” he wrote. “COVID-19 may be that bellwether event.”
Now the country’s ethical reckoning is more urgent than ever.
“How does a civil society — if indeed we are civil — respond not only to disproportionate suffering but also to a legacy of injustice?” Yancy said. “We will soon know the character of our populace.”
In spite of recent events, he insisted that he remains an optimist.
“One can only hope,” he said.