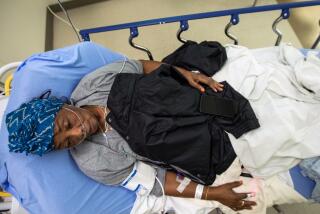
Another racial disparity that may be heightened by the pandemic: access to outpatient care
- Share via
As COVID-19 sent a growing number of sick patients into hospitals, it also kept away many others who were afraid of becoming infected at medical centers. Now researchers are reporting a worrisome pattern: During the first six months of the pandemic, hospitalizations for health problems that could have been avoided fell dramatically among white people in the Los Angeles area — but hardly at all among Black residents.
The disparity is a sign that Black patients may be getting poorer access to outpatient care — the kind that could have helped maintain their health and prevented it from deteriorating so much that they landed in a hospital bed, said Dr. Richard Leuchter, an internal medicine resident at UCLA Health and one of the researchers who led the new study.
“While a decrease in potentially avoidable hospitalizations may be perceived as beneficial on a population level, what these findings show is that any potential benefits from reducing them were not shared equally among racial groups,” Leuchter said.
The findings, published this month in the American Journal of Preventive Medicine, suggest yet another way the pandemic has worsened racial disparities in how healthcare is delivered in the United States.
While there’s been mounting evidence that patients of color have worse health outcomes and receive poorer care relative to their white peers, the pandemic has made the differences impossible to ignore — and often exacerbated them. COVID-19 disproportionately claims the lives of Black and Latino Americans, and it does so at younger ages than for white Americans.
The disparities show up even among children, a relatively low-risk group: Black children are hospitalized with COVID-19 at a rate five times higher than white children. The COVID-19 hospitalization rate for Latino children is eight times higher.
The vaccine rollout has also suffered from inequities, prompting the state to set aside 40% of its doses for residents of the most disadvantaged communities.
Over the last year, much research has understandably focused on the inequities affecting COVID-19 patients, Leuchter said.
“But I think something that has been relatively understudied is how the pandemic is worsening disparities among those without COVID,” he said. To address that concern, “we started looking at admission rates for people without COVID-19.”
The researchers examined hospitalization records at Ronald Reagan UCLA Medical Center and the UCLA Santa Monica Medical Center in 2019 and 2020. They focused on hospitalizations for conditions like chronic obstructive pulmonary disease, hypertension, congestive heart failure, pneumonia, uncontrolled diabetes and urinary tract infections.
All of these conditions have one thing in common: With proper preventive medical care, they can often be managed successfully enough to avoid hospitalization. (Surgical procedures such as diabetes-related amputations were not included in the analysis.)
The researchers found that between March 1 and Aug. 31 of last year, 347 out of 4,838 hospitalizations (or 7.2%) were potentially avoidable, compared with 557 out of 6,248 (8.9%) during the same six-month period of 2019.
Overall, potentially avoidable hospitalizations dropped by nearly 38%. Theoretically, that’s a good thing, Leuchter said: Perhaps patients were getting such good care for their conditions that they were able to head off a trip to the hospital.
But that improvement was not shared equally by members of different racial and ethnic groups. Non-Latino whites saw the biggest drop, with a 50.3% reduction from 2019. Black patients dipped by just 8% in 2020 — statistically indistinguishable from no change at all.
“What this is telling us is the COVID-19 pandemic may have exacerbated racial disparities in access to outpatient care,” Leuchter said.
A number of these conditions — such as heart disease and diabetes — carry a higher risk of death for African American patients in non-pandemic times.
The reasons for this inequity are complex, Leuchter said, though he pointed to some possible contributing factors. Among them:
- Some patients might be more apt to visit an outpatient clinic if they had a car and didn’t have to rely on public transportation, which is more likely to be the case for people of color.
- Many people of color, including Black patients, may be more likely to have jobs that don’t allow them to take time off in the middle of the day to see a doctor.
- Black patients may be suffering from the weathering effect — essentially, the cumulative impact of the discrimination and socioeconomic disadvantage that has plagued them throughout their lives and worsens the severity of other illnesses.
“These disparities of potentially avoidable hospitalizations predate the pandemic, but these findings are new to suggest that these disparities may have been exacerbated by COVID-19,” Leuchter said.
Though the study results were not unexpected, they do highlight a long-standing gap between Black and white patients, said Dr. Joseph Ouslander, a geriatrician at Florida Atlantic University in Boca Raton who was not involved in the study.
“This is a chronic situation,” Ouslander said, and it needs to be tackled by improving access to a range of healthcare services, including home care.
Because this was an observational study limited to two UCLA hospitals, researchers couldn’t identify which exact factors contributed to the disparity in these patients. “I think these findings should definitely raise alarm and spur on a lot of further research,” Leuchter said.
Ouslander offered a suggestion to probe the factors at play: Provide patients with a particular type of health service and test whether it makes a difference to their health.
“It could be a single intervention, like providing periodic telephone check-ins; or it could be a multifactorial intervention, which would provide a primary care clinician, transportation, regular telephone and in-person visits,” he said.
The first approach would narrowly target one intervention and show whether it works. The second would essentially be “a big black box” — if it works, it won’t be clear which service (or services) in the bundle made the difference.
Either way, Ouslander said, “we need to focus on trying to develop interventions that will help.”