- Share via
MEXICO CITY — The man with the hoe and shovel in the heavy white hazmat suit sweats in the tropical sun. His eyes sting beneath his face shield.
But Imang Maulana endures in his daily engagement with the red clay of Pondok Ranggon Cemetery in Jakarta, Indonesia, lowering white coffins sealed in plastic into graves reserved for victims of the coronavirus.
“It feels like it’s never going to end,” says Maulana, who often whispers an Islamic prayer on behalf of family members denied the ritual of farewell. “I feel exhausted.”
On Monday, the global death toll from the COVID-19 pandemic surpassed 1 million, a bleak milestone that is but one metric of a scourge that has ravaged lives and economies, mocked notions of stability and evoked a seemingly bygone era of plagues.
The virus has drawn out the best and worst of the human spirit. Blame and pettiness have echoed alongside moments of compassion and resolve, from the chaos of a hospital ward to the hushed quiet of a father, mother or sister dying in the bedroom of a house on an unremarkable street or on a dirt path in a distant village.


Although contagions were once blamed on the wrath of the Almighty, the origins of this 21st century blight were more prosaic. The virus was traced to a market in Wuhan, China, and may have jumped to humans from a bat or other wild animal, though scientists have not confirmed this.
Air travel and other aspects of global connectedness, esteemed markers of modernity, became viral vectors — just as amplified trade and urbanization once contributed to outbreaks of smallpox, malaria, cholera and other afflictions.
The virus’ continent-hopping trajectory saw it bounding from its origins in China through Asia, to Europe and Africa, and across oceans to the Americas and beyond.
The pandemic has brought great cities to a standstill, shuttered schools and factories, grounded air travel and unleashed ongoing social and political tumult. It triggered restrictions on where people could go and when, while also prompting mandates to wear face masks and practice social distancing to avoid spreading sickness and death.
It shut down sports and entertainment venues and forced the cancellation or suspension of iconic events, from Germany’s Oktoberfest to Mexico City’s famed Passion play to Rios de Janeiro’s Carnival.
In short, the coronavirus reshaped the world and the way people live — and die. And still it goes on.
As it swept the globe, the virus seared into the collective consciousness certain images: An eerie, locked-down Wuhan, a prescient glimpse of what was to come; Italian military vehicles transporting truckloads of coffins from devastated Bergamo, at the foot of the Alps; bodies abandoned on the streets of Guayaquil, Ecuador.
And the ubiquitous scenes of rows and rows of fresh graves, mourners set off in the distance, their physical detachment capturing a conflicting reality: Even grief was obliged to genuflect to the new norm of social distancing. Impersonal delivery of ashes supplanted time-honored rites of farewell and interment.

“The funeral home handled everything and told us they would bring the urn with the remains of my grandfather at 7 a.m., but we’ve been waiting for them here all day,” said a grieving Guadalupe García, 24, who was found with other mourners of coronavirus victims on a recent afternoon outside the San Mateo cemetery in Mexico City. “It’s a horrible sense of impotence.… My grandfather was like my father to me. He raised me. Today is one of the saddest days of my life.”
A scarcity of testing in Mexico and other countries means that the death toll of 1 million was almost certainly reached weeks ago. Many deaths were officially attributed to other causes, such as pneumonia.
Atop the global fatality rankings stands the world’s richest nation, the United States, with more than 205,000 deaths from COVID-19, the disease caused by the virus, according to the Coronavirus Resource Center at Johns Hopkins University.
President Trump’s erratic handling of the outbreak — including his frequent assurances that it would simply “go away” — has become a keynote critique of Joe Biden, his Democratic challenger, in November’s presidential election. Many fear a spike in cases as the cold-weather flu season approaches.
“We need to hunker down and get through this fall and winter because it’s not going to be easy,” Dr. Anthony Fauci, the nation’s infectious disease chief, recently told a livestream panel of doctors at Harvard Medical School. “Don’t ever underestimate the potential of the pandemic.”
Ranking second worldwide in the number of coronavirus-related deaths is Brazil, at more than 141,700, followed by India, where more than 95,500 people have succumbed.
Cases have been rising anew in India since the government eased a national lockdown that throttled the economy and battered the poorest in the nation of 1.3 billion.
Shuaib Bashir Khathib, 43, organized ambulance pickups and burials in Mumbai after cemeteries closed their gates and emergency crews refused to respond to victims stigmatized in illness and death.
“I became numb to the pain and death surrounding me,” he said.
A Muslim, he also helped arrange funeral pyres and services for stricken Hindus, a curative deed in a nation riven with sectarian tensions.
“Everybody deserves to have their last rites honored,” said Khathib, who recalled embracing a body of a virus victim early on to show volunteers that there was nothing to fear. “Why should our religion get in the way of that?”

Widespread economic displacement in India triggered epic scenes of multitudes of newly jobless returning on foot to their native villages. Among India’s collateral coronavirus victims: Sixteen migrant workers run over by a freight train in May as they slept on rail tracks, exhausted after walking more than 20 miles en route home.
As in India, health experts in Brazil are concerned that a recent uptick in cases could presage a renewed outbreak.
“I’m getting worried,” said Dr. Gustavo Treistman, an emergency room physician in the hard-hit western fringes of Rio de Janeiro who treated patients as the country’s medical system verged on collapse. “We can’t dismiss the possibility that we’re going to go back to that again.”
Brazilian President Jair Bolsonaro, a right-wing populist who dismissed the virus as a “little cold” and resisted control measures, has enjoyed rising popular support — apparently linked to generous aid payments to the poor.
Latin America and the Caribbean are among the most stricken regions, accounting for more than one-third of all deaths, according to the Pan American Health Organization.
Jakarta is the epicenter of an ongoing outbreak in Indonesia, the hardest-hit country in eastern Asia, with more than 10,400 deaths. That Indonesia is still struggling while other Asian nations — including China, South Korea and Japan — have moved toward full reopening is testament to the uneven arc of the pandemic.
Epidemiologists have linked high mortality in certain countries to myriad factors. Among them: the quality of a nation’s healthcare infrastructure, the extent of poverty, residents’ ages, their preexisting medical conditions and the effectiveness of government responses.
Predictions that the coronavirus would overwhelm Africa — previously ravaged by AIDS and tuberculosis — have so far proved erroneous, possibly due in part to the continent’s relatively young population.
By some accounts, infections in nursing homes and other long-term care facilities accounted for more than one-third of all early virus-related deaths in Europe and the United States. Authorities in Sweden initially said care homes were linked to about half of all coronavirus-related fatalities in the Nordic nation, where the government opted not to impose a strict lockdown, triggering criticism.

Even as cases have seen a recent surge in Spain, France and the United Kingdom, Italy — the nation where the contagion first exploded onto the scene in Europe — appears to have controlled the spread. Many credit Italians’ willingness to adhere to directives banning large gatherings and mandating face coverings.
“We Italians are not famous for following the rules, but we’ve done a good job,” said Dr. Luca Lorini, emergency medicine director at the Papa Giovanni XXIII hospital in Bergamo, once ground zero in Europe’s coronavirus crisis. “Seeing so many dead, so many coffins — when it comes to respecting the rules, fear helps.”
But even strict control regimens were not a panacea, as is evident in Peru. The South American nation has the highest per capita COVID-19 death rate among major countries, at almost 100 fatalities per 100,000 population, according to Johns Hopkins University.
Peru imposed a tight quarantine and curfew as cases began to multiply in March, and also rolled out a generous social aid program, earning international plaudits.


But much of Peru’s population survives off the informal economy, as street vendors and laborers, among other jobs, and lacks bank accounts. Long lines soon formed for government grants. People also queued at shops and markets, daily destinations in a country where almost half the population lacks home refrigerators.
The lines and crowded transport helped spread the contagion, especially in densely populated areas like the peripheries of Lima, the capital.
As casualties mounted, the task of collecting the dead in Peru was often left to some of the hemisphere’s most desperate denizens — Venezuelan immigrants.
Edmer Velásquez Cerpa, 28, a Venezuelan engineer who lost his job as a security guard in Lima when the pandemic struck, found work helping to gather the mounting number of corpses, often in far-flung, impoverished neighborhoods.
“At first it was terrifying, because I’d never seen a dead person,” Velásquez Cerpa said. “And there we were, with bodies on the floor, and families crying, but unable to touch their loved ones.”
He earned about $450 a month collecting as many as 30 cadavers a day.
In Peru, as in much of the world, a gradual diminution of controls has coincided with residents’ fatigue with restrictions. Many people express the desire to recoup salaries and reinvigorate economies facing their worst downturns in generations.
“Life has to continue, it doesn’t stop,” said Renato Freitas, 35, who works in Brazil at one of dozens of open-air bars along Rio de Janeiro’s Copacabana beach. The storied strand reopened in August, three months after the pandemic wiped out tourism and shuttered much of the city. “We need to work,” Freitas said.
That sentiment is also clear in Lebanon, where a recent upturn in cases has yielded to other concerns — an economy in free-fall, political gridlock and the port explosion in August that leveled part of the city and killed scores.
“With the financial situation and all the pressures … obviously those who run businesses don’t want a lockdown,” said Dr. Firass Abiad, who heads Beirut’s Rafik Hariri University Hospital, the public facility tasked with treating coronavirus patients.
In war-ravaged Syria and Yemen, meanwhile, the pandemic is poised to reach cataclysmic levels, but there are scant data from a pair of nations where years of conflict and sanctions have eviscerated public health systems.
With a surge in new cases, Israel recently tightened the country’s lockdown after Prime Minister Benjamin Netanyahu warned that the country was confronting “the edge of the abyss.”
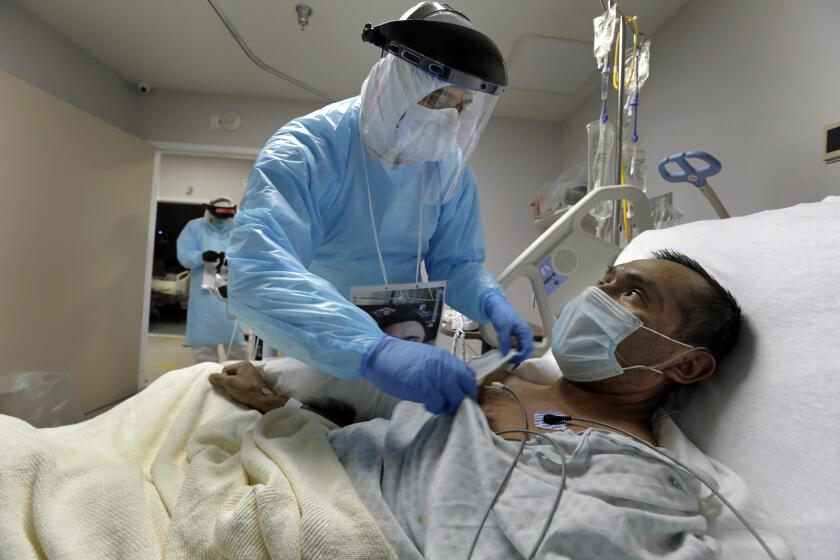
Around the world, health workers have proved to be among the most vulnerable in the pandemic. A shortage of protective equipment has contributed to the COVID-19 deaths of more than 7,000 doctors, nurses and other medical professionals, according to a report this month from Amnesty International, which called the problem “a crisis on a staggering scale.”
Dr. Iraima Márquez, a pediatrician in the Venezuelan city of Maracaibo, said she was sick for eight weeks from what she believes was COVID-19 — but the diagnosis was never confirmed, since tests weren’t available. She believes she contracted the illness from treating coronavirus patients in a hospital lacking proper ventilation and safety gear.
“They give the doctors something like ponchos — like what you wear in the rain — and asked us to reuse them,” said Márquez, 47, a mother of two.
Even for experienced hospital staff, the trauma of witnessing deaths from COVID-19 often lingers.
“It’s devastating — you detach all the medical equipment, sterilize the body and double-seal them in bags with a square of clear plastic showing just their face, and you show their families,” said Kim Hyun-ah, a veteran nurse who came out of retirement to volunteer at a hospital in Daegu, South Korea. “They can’t touch them one last time, before they’re taken away to be cremated. And that’s heartbreaking.”
In China, the state has essentially declared victory over what it calls a “people’s war” against COVID-19, and the country is hastening to win the race for a vaccine.
Wielding its authoritarian might, China tackled the outbreak in much the same way that it governs: top-down, with sweeping campaigns and absolute force, marshaling resources to perform feats like constructing hospitals in 10 days, producing billions of masks, and mobilizing granular surveillance and tracking of each citizen, with zero tolerance for straying from quarantine or failing to report close contacts. That approach largely succeeded.
COVID-19 deaths in China never topped 5,000, according to official numbers, though that excludes many uncounted early deaths in Wuhan — and the number of new cases per day is often in the single digits. Schools and offices are full, morning commutes loud and crowded, restaurant patrons with masked pulled askew chatter in Beijing’s autumn air — as if to make up for the ghastly stillness of the nationwide shutdown in January and February.
On the nightly news, hosts regularly proclaim that China’s recovery — in contrast to ever-rising caseloads in the United States and elsewhere — is due to the Communist Party’s governing structure.
Yet that system, with its intolerance of criticism, probably also contributed to the initial outbreak spinning out of control. Fear of upsetting superiors appears to have led authorities in Wuhan to cover up an unknown pathogen spreading through the industrial city of more than 11 million.
Missing from China’s official narrative of self-congratulation is the name of Li Wenliang, the 34-year-old ophthalmologist who was punished for sending an early warning about the virus to colleagues. Before dying of COVID-19, he spoke to a journalist in words that still resonate for many.
“A healthy society,” Li said, “should not have only one voice.”
Times staff writers McDonnell reported from Mexico City, Su from Beijing, and Bengali from Singapore. Staff writers David Pierson in Singapore, Victoria Kim in Seoul, Nabih Bulos in Beirut and Laura King in Washington contributed to this report. Special correspondents Mery Mogollón in Caracas, Venezuela, Adriana León in Lima, Peru, Janna Brancolini in Milan, Italy, Ana Ionova in Río de Janeiro, Tish Sanghera in Mumbai, India, Johanes Hutabarat in Jakarta, Indonesia, and Cecilia Sánchez and Liliana Nieto del Río in Mexico City also contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.