Will the U.S. ever have a national COVID-19 testing strategy?

- Share via
As the coronavirus epidemic worsens, U.S. health experts hope Joe Biden’s administration will put in place something Donald Trump’s has not — a comprehensive national testing strategy.
Such a strategy, they say, could systematically check more people for infections and spot surges before they take off. Health experts say it would be an improvement from the current practice, which has professional athletes and students at elite universities getting routine tests while many other Americans stand in line for hours — if they get tested at all.
“We have had no strategy for this virus. Our strategy has been no strategy,” said Dr. Michael Mina, a Harvard University researcher focused on the use of testing to track disease.
Some experts say the lack of such a system is one reason behind the current national explosion in cases, hospitalizations and deaths.
“If we’d had a more robust approach and testing was scaled up as one of the tools, I think much of this third surge would have been avoidable,” said Dr. Grant Colfax, director of the San Francisco Department of Public Health.
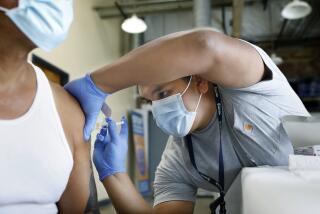
With COVID-19 cases surging and families hoping to gather safely for Thanksgiving, long lines for coronavirus tests have reappeared across the U.S.
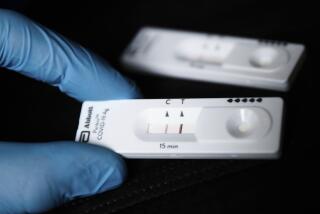
There are differing opinions on what such a strategy should look like, but many experts say rapid and at-home tests should be used so Americans can check themselves and stay away from others if they test positive.
The president-elect has endorsed that strategy, called for making testing free for all Americans, and said government experts at the Centers for Disease Control and Prevention and other agencies should be empowered to coordinate the entire effort.
“The reality is, we’re not testing enough today,” said Dr. Marcella Nunez-Smith, co-chair of Biden’s coronavirus advisory board.
Biden’s transition team so far has not gone into further detail.
Testing was one of the first — and most enduring — stumbles in the federal government’s response to the coronavirus epidemic that hit the nation early this year.
It’s true that the science about COVID-19 can be confusing and changes over time. But understanding it, and acting accordingly, are a literal matter of life and death. So why can’t our leaders get this right?
In February, the CDC distributed test kits to public health laboratories that initially were faulty. U.S. officials worked with companies to expand testing, but shortages of chemicals, materials and protective equipment meant fewer tests were available than what experts said was necessary.
Worse, some experts say, states and cities competed against one another to buy limited testing services and materials, and with little guidance or training on how best to use the tests.
In April, President Trump declared governors were responsible for testing. Amid complaints about shortages and delays, the federal government began sourcing and shipping key testing supplies to states, beginning with swabs.
In the latest phase, Trump officials are sending more than 100 million rapid, point-of-care tests to states. The government said the first shipments went out in early October.
Such tests are considered key to slowing spread, but states have distributed them differently. Alaska, for example, is sending tests to oil drilling sites, while Colorado is giving them to local public health agencies to test homeless populations, and Mississippi is using them in veterans’ homes.
California failed to establish an effective coronavirus testing system early on, leaving it far behind — even now — in the fight against COVID-19.
There’s also no federal standard for reporting test data. Some states report the number of tests administered, while others tally the number of people tested. Some have counted types of tests that others don’t, which can skew results because some tests are better than others at diagnosing active infections.
Administration officials say they are proud of the current state of testing. Last month, Vice President Mike Pence celebrated that 170 million tests had been completed and that an expanding array of tests were available.
But the focus should be less on numbers and more on action, said Dr. Ali Khan, dean of the University of Nebraska College of Public Health.
“It shouldn’t be anybody who needs a test can get a test,” Khan said. “It should be anybody who has a positive test immediately gets isolated,” and the people they’ve been in contact with are checked and placed in quarantine.
Contact tracers tell people they’ve tested positive for the coronavirus or warn they’ve been exposed to it. The conversations are confidential and sometimes surprisingly intimate.
He was echoed by Biden advisor Nunez-Smith, a health equity researcher at Yale.
“Testing is only useful when we can act on the test,” she said.
Trump himself has voiced a lack of enthusiasm for comprehensive testing. In a June tweet, the president called testing a double-edged sword that was good to have but “makes us look bad.”
And Dr. Scott Atlas — who, before he resigned Monday, was a top pandemic advisor to Trump — argued against testing people who weren’t experiencing symptoms.
But some regard such thinking as an attempt to spin a leadership failure into something else.
“The executive branch has seen test results — case counts — as a report card on its performance,” said Carl Bergstrom, a University of Washington evolutionary biologist who studies emerging infectious diseases.
The nation may be weeks away from coronavirus vaccines becoming available, but that won’t erase the need for testing, said Eileen O’Connor of the Rockefeller Foundation.
“We’re not going to get everybody vaccinated right away. And we still don’t know how long that immunity will last,” she said. So testing will still be needed to monitor where the infection is active and to see if infections are occurring in vaccinated people.
What should be done moving forward?
In July, the Rockefeller Foundation called for making cheap tests widely available to better identify people who are infected and don’t know it. That would involve developing and making cheap antigen tests, which provide quick results but are less reliable than genetic tests. Foundation officials hoped the government would push companies to manufacture tests the same way it pushed vaccine makers to mass produce experimental vaccines.
Duke University schools the country on how to use testing and stay open during the COVID-19 pandemic
A system of pooled coronavirus tests to catch asymptomatic infections among Duke University students helped keep the campus open in the midst of the pandemic.
Some Harvard researchers believe that testing half the population each week would be possible by mailing those tests to millions of U.S. households.
Participation would be voluntary, and positive results would have to be confirmed with genetic tests — the home tests are not considered as sensitive as more established lab-based testing. Even so, it could dramatically expand the amount of infection monitoring going on across the nation, its proponents say.
During an appearance on NBC’s “Meet the Press,” Dr. Anthony Fauci, of the National Institutes of Health, said Americans should have easy tests they could do in their own homes.
“We don’t have that,” he said. “We should have that.”
Versions of such an approach have been tried in some places, including Minnesota and Slovakia. But some experts note there is little precedent for screening tens of millions of people with cheap, rapid tests — which would generate a significant portion of false results. It’s also unclear whether people who test themselves at home will follow instructions to quarantine.
Nearly all experts agree that more data and coordination are needed.
“Having every state do its own thing without guidance from the federal level — from CDC in particular — I think has really hampered us,” said Scott Becker, chief executive of the Assn. of Public Health Laboratories. “It is a federal response as much as it is a state response, but it’s a shared responsibility. We need to work together.”