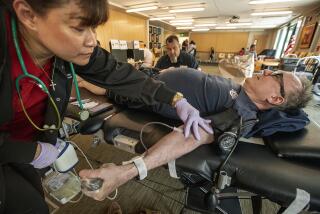
A Case for AIDS Test After a Needle-Stick
- Share via
A resolution will be presented to the California Medical Assn. Saturday urging the association to seek legislation that would allow involuntary testing of a patient for the AIDS virus following an exposure of a health-care worker to the patient’s blood or other similarly infectious fluid. Since this proposal involves involuntary (mandatory) testing, many people will reflexively debate it as an issue of patients’ versus health-care workers’ rights, and that is wrong.
Discussions about any form of involuntary testing invariably lead to intense emotional debate. This occurs because most mandatory testing proposals are clearly punitive in nature--a deliberate attempt to punish infected individuals for being infected. However, the relationship between the health-care worker and the patient is not adversarial but rather is one of mutual caring. The usual logical and valid arguments against mandatory testing must be addressed. But because of the relationship between patient and health-care worker we must recognize what is most fair: We must see this as a situation where the safety of health-care workers must be protected without adversely affecting patients. With well-thought-out and carefully drafted legislation, that can be done.
Mandatory testing of people for evidence of infection with the human immunodeficiency virus is generally opposed for three reasons: the behaviors that most commonly result in infection are consensual; there is no proven treatment to prevent infection, and fear of mandatory testing will usually convince the people most likely to be infected to stay away from testing situations, like premarital tests.
The situation of an accidental needle-stick, the most common source of a health-care worker’s accidental exposure, is obviously nonconsensual; there is now a possibly beneficial treatment, and it is doubtful that people would avoid medical care because of the very small risk of being tested involuntarily. So, the usual arguments against involuntary testing do not apply here.
On the other hand, mandatory testing could be acceptable were there to be a significant benefit, especially if that benefit were prevention of HIV infection; if the information could not be obtained in other ways, and if proper safeguards protected the person being tested.
Following a needle-stick injury, knowledge of whether a patient is infected, is beneficial to the health-care worker in two ways. The risk of infection following such exposure is about 1 in 250. While it is recognized that a negative test does not guarantee that the patient is uninfected, it clearly lowers the likelihood to less than 1%. Thus the risk of infection if the patient tests negative is less than 1 in 25,000. Current advice following a needle-stick is to recommend low-risk or no sexual behavior for 6 to 12 months while the worker has repeated tests to see if he or she had become infected. If the patient tested negative, the worry would be much less. Alternatively, if the patient tested positive, there would be greater worry and likely greater adherence to safer sex practices.
Secondly, there is now information from animal studies suggesting that starting immediate treatment with AZT for six weeks might prevent infection with the AIDS virus or at least lessen the severity of disease after a needle-stick injury from an infected patient. A few health-care workers have entered a study using AZT or a placebo if they know the needle-stick came from an infected patient. Others are taking AZT without going into the study. Many AIDS physicians would recommend AZT after such an injury but probably not if the patient tested negative. While we do not know if AZT is effective or not, the worker needs information about whether the patient is infected to make the best-informed decision about what to do.
Finally, why would such a law be necessary? The vast majority of patients, once informed about why the test was needed, would consent. The rare exception occurs, not because patients want to be stubborn or to harm a health-care worker. Rather it is because of fear that the test results, if positive, might get into the wrong hands, resulting in loss of job, insurance, home, friends. Sadly, confidentiality in hospitals, clinics, etc. needs a great deal of improvement. Perhaps even more important, some people are terrified of learning that they are infected. Many successful and unsuccessful suicide attempts, following a positive test, show this is a well-founded fear.
If we understand both patients’ and health-care workers’ concerns, legislation with appropriate safeguards of confidentiality and of the patient’s right not to know (if that is the patient’s wish) can be developed and supported. Many practical issues about how to do this need to be worked out--but it can and must be done for the legislation to be acceptable.
In making the decision to support legislation with appropriate safeguards, one overriding concept must be kept in mind: We urge or require health-care workers to care for HIV-infected patients. When the workers’ physical and mental well-being are at stake, it seems totally inappropriate not to provide them with all the information they need to care for themselves as well.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.