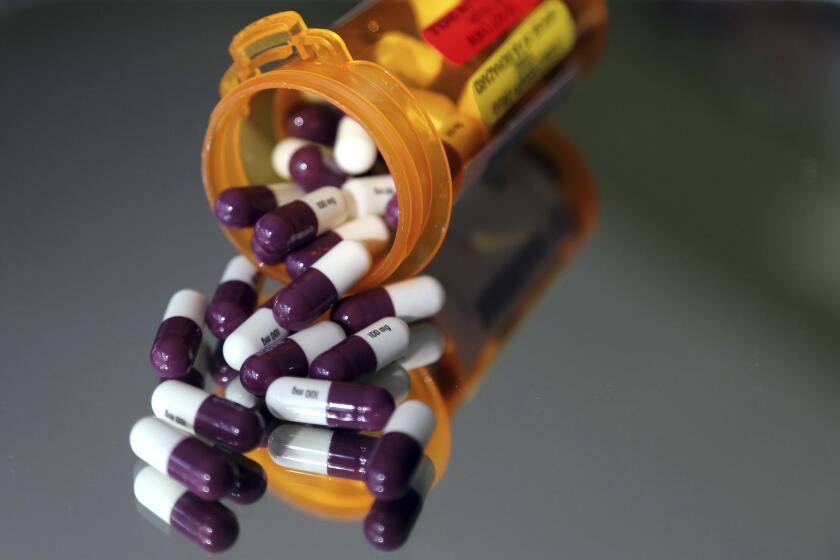
A huge spike in the cost of an old drug reignites the pharma pricing debate
- Share via
Until last month, patients suffering from the parasite-borne disease toxoplasmosis -- which in its worst manifestations can cause blindness, neurological problems or death -- had reasonable access to a remedy: a six-week, two-pill-a-day course of the drug Daraprim, at a cost of about $1,130.
Then an entrepreneurial company called Turing Pharmaceuticals acquired the exclusive rights to Daraprim and raised its price from $13.50 per pill to $750, bringing the total treatment cost to $63,000. For longer-term patients such as sufferers from HIV, the annual cost can go as high as $634,000, according to a joint statement from the Infectious Diseases Society of America and the HIV Medicine Assn.
“This cost is unjustifiable for the medically vulnerable patient population in need of this medication and unsustainable for the healthcare system, the organizations said in a letter to Turing executives.
They’re right, especially since Daraprim isn’t a new drug, but one that was approved by the Food and Drug Administration in 1953. Turing CEO Martin Shkreli defends the price hike in Daraprim’s case -- more on that in a moment -- but it underscores how deeply broken the American system of drug pricing and distribution has become.
Daraprim isn’t the first drug to be priced out of the reach of many patients, even those with insurance, and arguably not even the most egregious case. Immediately after acquiring rights to two staple heart drugs, the Canadian company Valeant trebled the cost of one and increased the other six-fold. That has elicited a letter from Rep. Elijah Cummings (D-Md.) and Sen. Bernie Sanders (I-Vt.), demanding that Valeant provide Congress with justification for the increases.
SIGN UP for the free California Inc. business newsletter >>
The poster child for pricing a drug at what the market will bear -- or even higher -- is the Bay Area firm Gilead Sciences, which more than doubled the price of the highly effective hepatitis C drug Sovaldi to $84,000 for a 12-week treatment, or about $1,000 per daily pill, after acquiring its developer in 2011; Harvoni, a follow-on formulation that is more effective than Sovaldi, is priced even higher. We explored the Sovaldi/Harvoni case here, and later reported that Sovaldi alone had a material effect on rising prescription drug spending nationwide.
There are some differences between the Sovaldi and Daraprim cases. The potential market for hepatitis C drugs may be as large as 3 million patients in the United States, which so unnerves Medicare and private insurers that they have placed strict limits on the conditions for which they would approve the wonder drugs, limiting them to patients who already have suffered severe liver damage.
The market for Daraprim may be much smaller. Although as many as 60 million Americans may harbor the toxoplasma parasite, which can be picked up from undercooked meats, unwashed fruits and vegetables or contaminated soil or litter boxes (cat feces is a major vector), the vast majority never will experience symptoms.
The risk population is the extremely elderly, infants who may acquire the bug from their mothers, and immunosuppressed patients such as those with HIV. The Centers for Disease Control and Prevention estimated the number of hospitalizations due to the bug at about 4,400 a year and deaths at 327.
Turing’s Shkreli says those figures justify the firm’s pricing strategy following its acquisition of Daraprim for $55 million. He says that at its previous price, the drug produced only $5 million in annual revenue for its rights holder. That made it a quintessential orphan drug, since no manufacturer could justify an investment either to improve the formula or bring out a generic version. The result was no improvement in treatment for toxoplasmosis in 62 years.
Shkreli says Turing expects its Daraprim deal to be profitable, but will put at least some of the new revenue into research and development for an improvement and toward new drugs for other parasitical diseases. “We’re not going to take this money and put it in our pocket or pay ourselves a dividend,” the 32-year-old entrepreneur told me. “We’re not going to stop until we’ve eliminated toxoplasmosis.”
He also says the company has taken steps to ensure that no patients go without Daraprim because of its cost or the unwillingness of pharmacy managers to stock it. Last week the company announced a special program aimed at ensuring “quick, efficient access for patients in need” and served by federally funded health programs. Shkreli says that Turing discounts about half of Daraprim sales to about $1 per 100-pill bottle. Rima MacLeod, a toxoplasmosis expert at the University of Chicago, was quoted in USA Today last week saying that none of her patients has yet lost access to Daraprim because of the price increase. “Turing’s people have been helpful every single time,” she said.
SIGN UP for the free Opinion newsletter >>
Shkreli, as it happens, was embroiled in a similar pricing controversy last year, when his former company, Retrophin, acquired rights to an old drug named Thiola, which is used to control a condition that produces incessant kidney stones in its sufferers. Retrophin jacked up the price from $1.50 per pill to more than $30. The increase in the annual treatment cost from about $2,700 to $54,750 for patients doomed to remain on the drug all their lives earned Shkreli a broadside from -- among others -- urologist Benjamin Davies of the University of Pittsburgh, who accused him of having “grabbed an old drug, made no changes to it at all, and hiked the price exorbitantly.” Shkreli says that after he was ousted from Retrophin (the company is suing him for alleged self-dealing), its board discontinued efforts he had begun to provide financial support for researchers and patients.
It’s proper to examine whether the public is served by allowing pharmaceutical companies to charge whatever they choose for life-saving drugs, then deciding on their own whether patients warrant their sufferance and a lower price. That’s especially true given that government money funds the initial research of many new drugs, which are then marketed at a profit by private corporations.
It was the Bayh-Dole Act of 1980 that opened the floodgates for private exploitation of the taxpayers’ contribution. But it’s policy that allows this to continue without oversight. Only recently have legislators at the state or federal levels started to offer measures forcing drug companies to disclose more about their products’ R&D costs and profits to make it easier for the public to examine their justifications for high prices.
Patient advocates such as the Center for American Progress are urging federal officials to start using the government’s “march-in” rights over federally-funded drugs. Bayh-Dole allows the government to take action when it finds that a drug company has not made such products “available to the public on reasonable terms.” The steps could involve the government’s licensing the patent to generic manufacturers.
Turing’s Shkreli acknowledges that the public thinks of drug companies in different terms from other commercial enterprises. “There’s this expectation that drug companies should act differently from other companies, because you have to buy their products,” he says. “That notion needs to disappear. The only thing that can really work is that if people hold companies and CEOs like myself to task on what you do with the money. As long as that is beneficial for society, there should be no worries.”
Keep up to date with the Economy Hub. Follow @hiltzikm on Twitter, see our Facebook page, or email michael.hiltzik@latimes.com.
MORE FROM HILTZIK:
How a rich water district beat the federal government in a secret deal
It’s time for Carly Fiorina to apologize to Planned Parenthood
No surprise: Conservative sneers that public employees like their pensions
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.