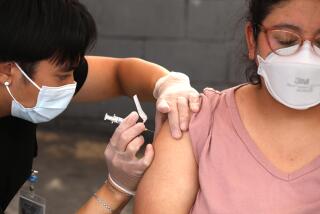
What if I get sick? Coronavirus adds new anxieties for pregnant women

- Share via
I hate crying in public.
But there I was — 17 weeks pregnant with my first child — with tears streaming down my face as I stood among a crowd of anxious shoppers in a Long Beach Target. I had tried to push down that all-too-familiar lump that rises in my throat before the tears began, but a mix of hormones and coronavirus-induced anxiety proved too much.
My colleagues at The Times have written extensively about the apprehension surrounding the outbreak, including people flocking to stores to stockpile food and other essentials. So when my husband and I walked into the store that day, we expected certain aisles would be empty. I didn’t anticipate nearly all the infant Tylenol would be gone.
In a complete panic, but still months away from my due date, I picked up one of the last boxes on the shelf in an attempt to find some sense of control.
My husband looked at me with confusion as I unleashed a string of irrational fears. He countered, kindly, that perhaps the medicine should be saved for a family with a sick baby at home. Of course, he was right. I pictured a panicked new mother searching for medication for her child and finding none among the sea of empty shelves. I put the box back.
That’s when the tears started. Pregnancy in the time of coronavirus seems especially cruel.
Pregnancy, though joyous, is filled with so much unspoken anxiety in the best of times. Am I eating the right food? Am I drinking too much caffeine? Will my baby be healthy? Will I be a good mother?
Coronavirus adds another question into the mix: What happens if I get sick?
If you’ve been infected with the coronavirus, the chances that you will become critically ill depend on many factors.
Dr. Neil Silverman, a clinical professor of obstetrics and gynecology at the David Geffen School of Medicine at UCLA, has heard similar questions at his practice from many worried mothers-to-be.
“It’s all about the fact that there’s so many things in the setting of a pregnancy that women have no control over,” Silverman said during a recent phone interview. “Women, especially in their first pregnancy, are understandably concerned in general about all the things that cannot go according to plan.”
There is little data available on how the coronavirus, which causes a respiratory illness known as COVID-19, affects pregnant women. Women experience physiological changes during pregnancy that can weaken their immune systems and place them at higher risk for severe complications if exposed to viruses, especially if they have underlying heath conditions.
Past studies have shown that pregnant women who contract influenza are at higher risk for severe complications, and in 2009, women who contracted H1N1 — the swine flu — during pregnancy also became sicker than non-pregnant women, according to Dr. Denise Jamieson, chair of the department of gynecology and obstetrics at the Emory University School of Medicine in Georgia.
Still, doctors said that researchers have not seen early signals suggesting an increased risk of complications or birth defects associated with pregnant women and fetuses exposed to the coronavirus.
“Pregnant women can become severely ill, but I think pregnant women should be reassured as there doesn’t seem to be related birth defects like we saw with Zika,” Jamieson said during a phone call last week. “These are scary times, and I think a lot of people, including pregnant women, are afraid. Luckily this is not a virus that seems to disproportionately affect pregnant women. They can take solace in that.”
In a recent study published in the Lancet, researchers followed nine pregnant women who had tested positive for the novel coronavirus in Wuhan, China — the epicenter of the outbreak — during their third trimester. Researchers found that none of the infants, all delivered via caesarean, had the virus at birth. There also was no evidence of the virus in the mothers’ breast milk, cord blood or amniotic fluid, according to the study.
The new mothers had experienced the same symptoms as nonpregnant women, the study showed, with fever in seven, cough in four, myalgia in three and sore throat and malaise in two. They developed pneumonia, but none of the cases were considered severe.
Researchers suggest these data indicate that mothers diagnosed with COVID-19 do not pass along the virus to their unborn babies through the placenta. However, it is possible for mothers to pass the virus to infants after birth from respiratory droplets or particles that leave the mouth or nose when a sick person coughs, sneezes or talks.
While the virus has not been detected in breast milk, the Centers for Disease Control and Prevention said it’s still not clear whether the virus can be transmitted to infants during feedings. The CDC recommends infected mothers wash their hands before touching their babies and wearing a face mask, if possible, while breastfeeding. Another option is having a healthy person feed expressed breast milk to the infant.
Health officials are urging pregnant women, along with the elderly and others with weakened immune systems, to do their best to avoid exposure to the coronavirus. Doctors suggest staying home as much as possible, avoiding crowds — including long lines at supermarkets and other stores — and staying away from emergency rooms. And, of course, frequent hand washing.
Here’s a visual look at how life in Southern California has changed during the coronavirus crisis.
Dr. Karin Nielsen-Saines, professor of clinical pediatrics in the Division of Infectious Diseases at UCLA Children’s Hospital, suggests women reach out to their doctors to see if routine labs or physical assessments can be done without a visit to clinics or hospitals to limit their risk of exposure.
Some doctors, including mine, have already instituted this practice. The Kaiser Permanente in Gardena was nearly empty when I arrived Wednesday afternoon for a monthly exam and ultrasound. Medical staff wearing paper gowns, masks and gloves screened patients for symptoms of the virus before they walked in the front door.
I was one of a few people that day who had to physically visit the office because I had to have blood drawn.
“Get in and out quickly,” a nurse told me as she placed a sticker allowing my entry into the building on my blouse.
Another woman who was having an ultrasound was video-chatting with her husband, who was stuck in the lobby, during the exam. The medical center has stopped allowing visitors in exam rooms in an effort to help protect patients and staff members from the spread of the illness.
A similar visitor policy also extends to hospitals when women are giving birth. Kaiser will allow one visitor, typically a spouse or partner, for the duration of a woman’s hospital stay. But family and friends are being asked to wait until the new parents are at home to meet their bundle of joy. Hoag Hospital in Orange County has also instituted the one-visitor policy.
Despite the new restrictions and disappointments — especially for women whose baby shower plans and “babymoon” trips have been thwarted by the virus — Nielsen-Saines emphasized the importance of keeping to a routine, even during times of uncertainty.
“Exercise, talk with friends, try to keep a sense of normalcy,” she told me. “This feeling of impending doom doesn’t help anyone. It’s important to keep it all in perspective.”
At least we can all try.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.