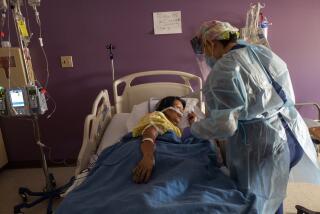Coronavirus spreading rapidly through California nursing homes, assisted-living centers

- Share via
Nursing homes and assisted-living centers across California continued to see significant increases in coronavirus cases, alarming officials who are trying to slow the spread.
The older populations of these facilities almost always have underlying health problems, making them particularly vulnerable to the coronavirus. They often live in close quarters. Administrators have responded by banning visitors, confining patients to their rooms and scrambling to create sterile wings to treat residents who contract the disease.
Still, there have been outbreaks at facilities from Redondo Beach to Burlingame.
Twenty-seven people at a skilled nursing facility in the East Bay city of Orinda have tested positive for the coronavirus.
“We are very, very concerned,” said Dr. Chris Farnitano, the Contra Costa County health officer. “This is a virus without a vaccine. This is a virus without a medical treatment.”
He said the residents who have tested negative have been separated from those who are infected, and the staff also has been separated. Staff who have tested positive have been told to isolate at home, but if they have no symptoms, they may, with protective gear, continue to serve the residents who also tested positive.
At least 57 residents and staff of a Yucaipa nursing home were infected with the virus, including two people who died, and officials have told the facility to assume all of its patients have COVID-19, San Bernardino County public health officials said earlier this week.
A cluster of infections also has been reported at a San Diego senior living home, where four residents and two employees at the Stellar Care memory-care center tested positive for the coronavirus in recent days.
Other residents showing signs of having acquired the sometimes-deadly sickness are being isolated in their rooms, an administrator for the memory-care home said.
But some of them inevitably wander downstairs to the familiar confines of the dining room, searching for a communal meal or one of the home’s many activities.
When that happens, which is multiple times a day, they are gently directed back to their quarters.
“Given that every resident has memory impairment, we can give an instruction to stay in their room but five minutes later they will forget and do what they always do — walk down to the dining room to have an activity or a meal,” said Jerald Harris, a Stellar Care administrator and attorney.
“Obviously it’s a difficult situation,” he said.
In Los Angeles County, the Department of Public Health was investigating 321 cases of the coronavirus among staff, residents and guests of 67 institutions as of Friday.
A resident of the California Veterans Home in West Los Angeles was taken to a VA hospital after testing positive for the virus, the state Department of Veterans Affairs said Saturday.
No other infections have been reported among residents of the department’s eight homes; but earlier in the week, two staffers at the California Veterans Home in Redding tested positive, officials said.
Hospitals are desperately trying to discharge patients to clear space for an expected wave of people infected with COVID-19. But nursing homes are reluctant to accept any new patients — or even returning residents — until it is proved that they are coronavirus-free.
On Monday, the California Department of Public Health sided squarely with the hospitals, ordering skilled nursing facilities to accept residents even if they have tested positive for the novel coronavirus. After an outcry from elder advocates, one of whom called the directive “nothing less than a death sentence” for nursing home residents, state officials issued new guidance late Wednesday.
“The final determination lies with the local health department,” the state Department of Public Health said in an email to The Times. “Local public health officers have this authority in an emergency.”
Elder advocates, who say most nursing homes lack the equipment and training to properly quarantine patients with the virus, are not satisfied. Many want the state to set up entirely separate living spaces — such as empty hotels, dormitories or cruise ships — for nursing home residents with the virus.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.