Janitors and other nonclinical hospital workers feel forgotten in coronavirus battle: ‘They’re terrified’

- Share via
When Andre Ross gets home from his shift at Southern California Hospital at Hollywood, he immediately strips off his scrubs, puts them in a bag and runs to the washing machine.
He showers as fast as he can. He disinfects the bathroom.
Ross, 30, is terrified of catching the novel coronavirus at work and spreading it to other tenants of his South Los Angeles apartment building.
He can’t afford to get sick and miss work. He’s a floor-care specialist, part of the hospital’s janitorial team, who makes $18.31 an hour. Finances are tight. Work is scary.
“We don’t know what patients are going to come in with the virus. It’s a nightmare,” Ross said. “I’m on the front lines every day. I’m just trying to stay as healthy and positive as I can.”
As the number of coronavirus-related hospitalizations and deaths skyrocket across the U.S., the experience of doctors and nurses has been rightfully framed within the context of a great war to save lives while not being sickened or killed by COVID-19.
But less attention is paid to thousands of lower-paid nonclinical hospital workers — such as janitors, food-service workers and clerks — who also worry about contracting the virus and spreading it.
“I see my co-workers, doctors, nurses, housekeepers; they come to work every day,” Ross said. “Me cleaning my floors and making my floors look nice, keeping them disinfected, I do it for them and the patients. I feel like we are at war.”
Hospitals across the country have scrambled for personal protective equipment and other gear in short supply. Nurses and doctors have pleaded for donations online, telling stories of reusing masks and rigging trash bags as gowns.
Many nonclinical hospital staffers say they, too, are woefully unprotected but feel like second-class citizens.
One emergency room doctor at Los Angeles County-USC Medical Center, who spoke to The Times on the condition of anonymity out of concern for his job, said he is fearful for the minimum-wage support staff there who are facing many of the same potential risks as higher-paid medical professionals.
“There’s a huge number of people who are putting themselves at risk, and they didn’t sign up for it the way nurses and doctors did,” he said.
Nonclinical hospital staffers “likely face similar to higher risks as others who still have to report to work,” said Steven Wallace, a professor in the community health sciences department at the UCLA Fielding School of Public Health.
“Almost everyone in a hospital comes into contact with someone who has patient contact,” Wallace said in an email.
A study published Monday in the Annals of Internal Medicine showed that nonclinical hospital workers in Singapore, including clerical staff and maintenance workers, were at a higher risk of anxiety, depression and stress related to the COVID-19 outbreak than doctors and nurses.
Researchers said the reasons may include less intensive training on personal protective equipment and infection-control measures, reduced access to formal psychological support, and less firsthand medical information on the outbreak.
In the U.S., nonclinical workers also face concerns about having their hours cut or losing their jobs. Hospitals nationwide have seen a lower patient volume — and are losing money — because elective procedures and tests have largely been stopped. Dozens of hospitals have furloughed nonclinical employees.
As a shop steward for Service Employees International Union-United Healthcare Workers West, Ross has heard a lot of fear and frustration from his colleagues in the janitorial department.
Hospitals preparing for coronavirus confront empty promises and scams as they try to buy masks and other protective equipment.
In the early days of the coronavirus’ spread in California last month, some housekeepers tried to get masks at work but were told they were being given only to doctors and nurses, he said.
One housekeeper, who is in her 70s and has worked for the hospital for decades, was refused a mask early on, Ross said. She brought one from home, kept it in her lunch pail and kept reusing it.
“They’re terrified,” Ross said. “They’re upset. They feel like they’re being treated differently.”
Many, he said, don’t want to speak out because they worry they will face retaliation.
Initially, Ross said, the only way a nonclinical employee could get a mask was if he or she did not get a flu shot, which was provided by the company in the fall, Ross said. He had declined one, in large part, because he knows some people feel ill after getting the vaccination, and he couldn’t afford to take a day off.
A spokesperson for Southern California Hospital at Hollywood told The Times that a new policy requiring all employees, including nonclinical staff, to wear masks went into effect March 27.
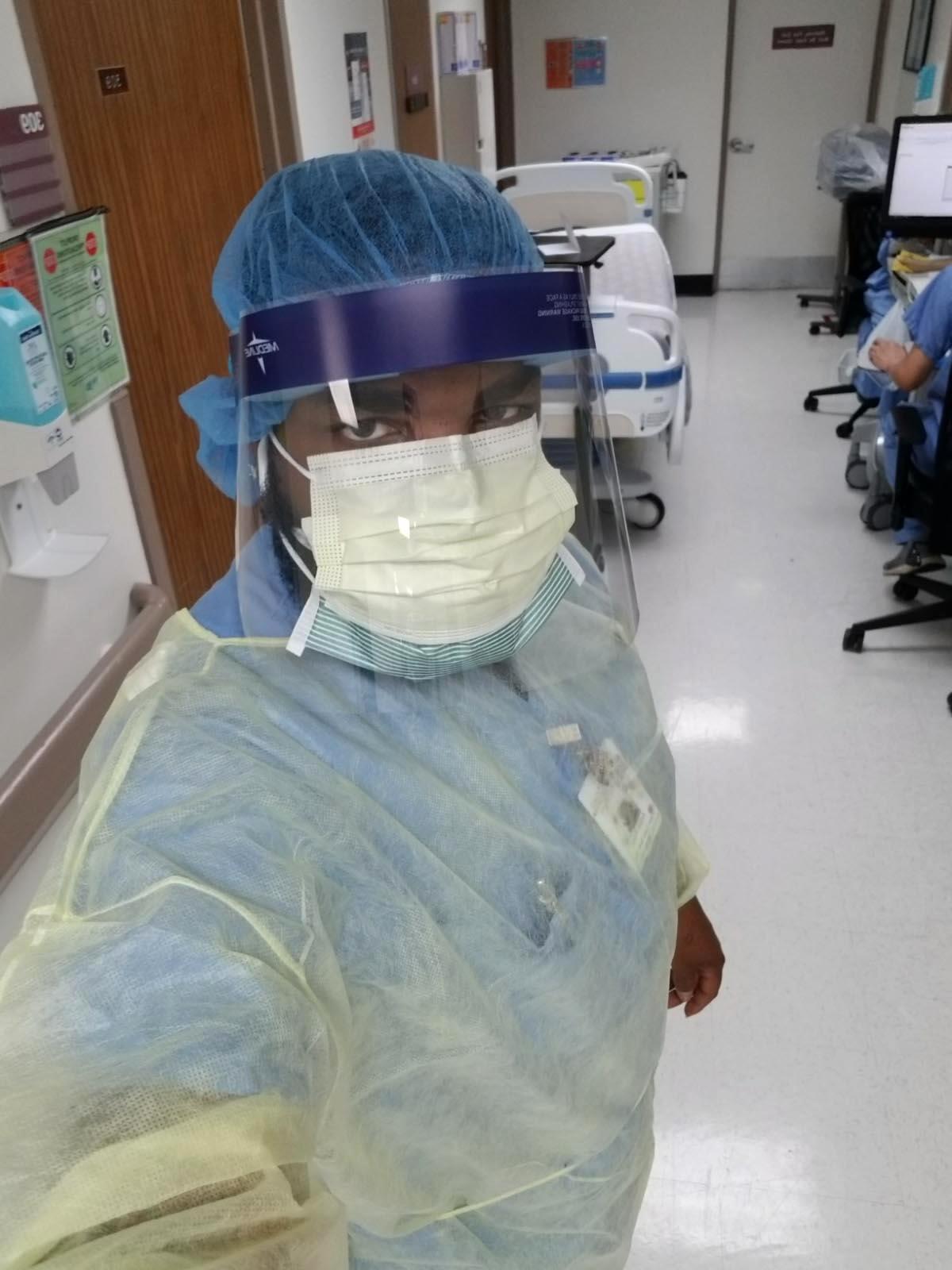
Ross, who disinfects hospital floors, elevators and the kitchen, knows his work is vital. The coronavirus can last on some surfaces, such as plastic and stainless steel, for up to three days.
He said the only time he is allowed to wear full safety gear — a gown, coverings for his hair and shoes, a face shield — in addition to his surgical mask and gloves is when he disinfects the rooms of possible COVID-19 patients.
Leah Reily, executive director of the Assn. for Healthcare Foodservice, a trade group for self-operated healthcare eateries, said hospital cafeterias and kitchens are adjusting as best they can to continue feeding doctors, nurses and patients.
“Our facilities have contingency plans in place. They’re trying to keep morale up,” Reily said.
Many cafeterias have closed seating areas and gone entirely to individually packaged to-go meals, she said.
Evelia Rodriguez, a records clerk who has worked at Kaiser Permanente South Bay Medical Center in Harbor City for 29 years, said that even as a nonclinical worker, she has always interacted with patients, helping them get medical records, disability forms and other paperwork.
A shop steward for SEIU-UHW, Rodriguez, 48, of Carson, said she pressured her bosses to close the intake desk and have patients call or email. Initially, she said, nonclinical workers were told not to wear gloves and masks because of shortages.
“It was concerning because they forgot about us silo departments, thinking we don’t deal with patients. Yes, we do,” Rodriguez said.
In a statement to The Times, Kaiser Permanente said: “We continue to provide all of our staff — including nonclinical employees — with protective equipment in accordance with the latest science and guidance from public health authorities that are appropriate for the tasks and work they are performing.
“While we currently have the personal protective equipment needed to protect our staff and patients, we are prudently managing our resources, and are actively pursuing the acquisition of additional supplies as we continue to deliver high-quality care to our members.”
California is fighting to supply hospitals with needed personal protective equipment, or PPE. Fierce competition and a lack of central coordination is hampering efforts.
Rodriguez said she had to advocate on behalf of a disability claims processor who was exposed early on to two patients who were quarantined with possible COVID-19.
“Our administrator who came in and asked her a few questions didn’t come back and say, ‘Go to the doctor’ because it was less than four minutes of contact and no droplets,” Rodriguez said. “They can’t assume that. We don’t know if they coughed on the paperwork, sneezed on it. You don’t know. She’s still at work.”
At home, Rodriguez has a 10-year-old son with special needs and a 4-month-old granddaughter. After work, she leaves her shoes outside and sprays them with Lysol. She sprays herself, too.
“I close my eyes, and I spray from head to toe,” Rodriguez said.
Ivan Yepez, 63, does patient registration in the emergency room at Dignity Health Northridge Hospital Medical Center.
Initially, Yepez said, nonclinical workers in the ER were told to take off masks because of possible shortages. Yepez, who has diabetes, said he is grateful the policy has since changed.
In a statement to The Times, Northridge Hospital Medical Center said there is “no higher priority than the safety of all of our staff members, not just those that are on the front lines treating patients.”
“Northridge Hospital Medical Center has been working nonstop to ensure that all team members who need personal protective equipment ... have the right equipment, at the right time, regardless of the staff member’s role.”
Yepez said he has argued with relatives he lives with in Valencia who worry about him bringing the coronavirus home from work. When he gets home, he sprays himself with Lysol and showers immediately.
A few weeks ago, Yepez said, his hospital set up tents outside to screen patients. If they have COVID-19 symptoms, their identification cards are sent inside to him in a red infectious-waste bag. He feels safer now that he is not directly interacting with possible coronavirus patients.
“It is very weird,” Yepez said. “And then you realize this patient might be infected, and that’s a life there, and who knows if this patient will make it or not? We say a prayer or two and go on.”
Speaking on the phone, he began to weep.
Times staff writer Harriet Ryan contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.
















