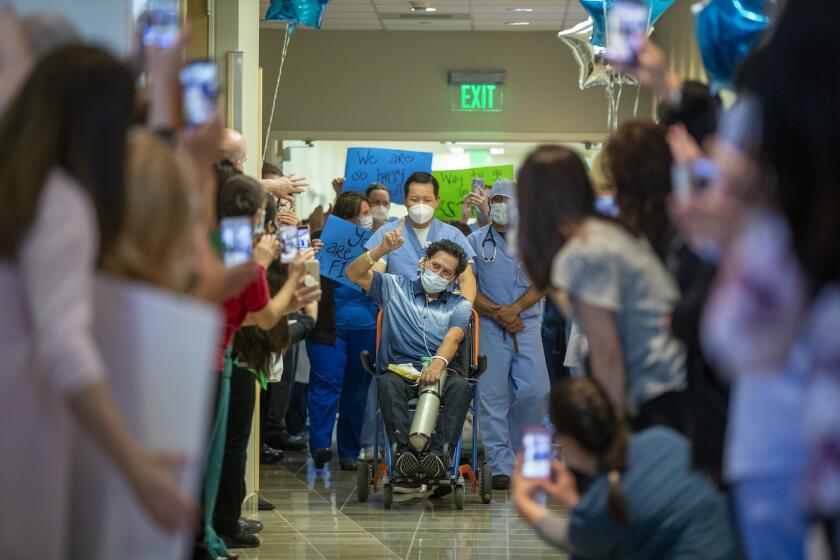
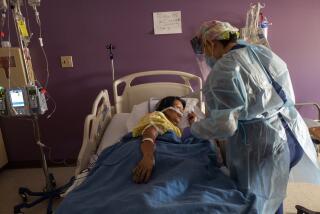‘Long on fear, short of gear’: Inside California hospitals as they wait for coronavirus surge

- Share via
Nurses, doctors and thousands of medical workers inside California hospitals are already struggling through intense days — and intense emotions — as the wave of expected COVID-19 patients turns from a distant shadow to a roaring peril.
Gov. Gavin Newsom says more than 140,000 people in the state might need a hospital bed by the end of May, with about 26,000 requiring a high level of care — a scenario that predicts nearly two months until a peak. As of Friday, California had more than 12,000 positive cases of the novel coronavirus, with nearly 2,200 people hospitalized and 900 in intensive care.
So far, even as Los Angeles becomes a hot spot for the highly infectious pathogen, the number of serious coronavirus patients at most facilities in Southern California has been in the dozens. It’s a lull leaving ominously empty wards and frayed nerves.
“It’s like a pressure cooker,” said a nurse at UCLA. “Long on fear and short of gear.”
The wait, many said, verges on unbearable.
As those inside the vacant hospitals brace for what’s next, there is a rush to buy supplies, repurpose space for makeshift intensive care zones and even train staffers who may be called on to perform tasks that are only distant memories from their days in school.
These are some of the unusual new scenes across the Southland during the coronavirus outbreak.
There is also growing concern from some frontline workers that not enough is being done to protect them and suspicion that their institutions may not be telling them the truth about how effective work-around safety measures are.
At St. Francis Medical Center in Lynwood, the emergency room has not been as crowded as it normally is, according to a nurse there, yet the scramble for gear is already on.
“It’s very scary inside the hospital,” said the nurse, who, like some of those interviewed, requested anonymity because he was not authorized to speak publicly. “Everyone is looking at each other, we’re just waiting.”
The nurse said he has heard from friends in the profession elsewhere that a surge can come in a matter of hours, a crush of patients can engulf the hospital in an instant.
“I don’t know what’s going to be the straw that breaks the camel’s back when we get down to it,” he said. “Every place becomes an ICU, that’s what we’re waiting for, that’s what everyone is anticipating.”
In our effort to cover this pandemic as thoroughly as possible, we’d like to hear from the loved ones of people who have died from the coronavirus.
A hospital administrator in the San Fernando Valley said she begins each day by looking over the updated accounting of what is left of their COVID resources — face shields, intensive care unit beds, isolation gowns, ventilators — and then goes department to department to buck up the exhausted and fearful staff.
“When you walk around on the floors of the hospitals, it is the most eerie sense of what is to come,” she said. “It is just palpable.”
On the COVID-19 wards, the nurses are busy and professional, she said, but “if they get a moment to sit down, to grab coffee, they just crumble.”
She said that for now she tells them the hospital has what it needs. She doesn’t tell them she thinks it’s possible, even likely, that they will run out of N95 masks in the near future or that she worries “every night, every day, every hour” about what that will mean.
“It’s like sending your soldiers into battle without weapons,” the administrator said. “How do you prepare people for something like that?”
Nurses who’ve been exposed to the virus ask to be tested, but “we simply don’t have enough tests,” the administrator said.
So they keep working, and she fears that they may be infecting other patients. She said she has decided that she will not force anyone to work without protection if they do run out, but she will remind them of their duty to the public.
“I will explain what’s before us and see who is willing to step up,” she said.
Los Angeles Times’ visual coverage of the coronavirus crisis
Dr. James Keany, an emergency room physician at Providence Mission Hospital in Mission Viejo, said his facility is in a similar holding pattern. They have COVID-19 patients, including some in the ICU and on ventilators, but not many.
“I feel like we’re not anywhere near capacity right now,” he said. “But the COVID patients are definitely on the increase and it’s increasing daily.”
Some staff members are anxious and want to wear N95 masks whenever treating COVID-19 patients, but the hospital is recommending their use only for high-risk situations.
He said they are now weighing whether it is better to have the staff wear N95s more often and reuse them or to try to stick to the policy of wearing a surgical mask with a face shield. He prefers the latter, saving the coveted filtered mask for when it might really matter.
“People don’t want to hear that,” he said. “There will be anxiety among the staff. ... Emotionally, I think the [N95] mask feels better.”
A nurse at UC Davis Medical Center in Sacramento said he feels discouraged for the first time in his career by the lack of protective gear. The nurse, who was not authorized by his institution to speak to the media, said he has been punched, kicked, scratched and bitten by patients and even faced down weapons during his years on the job. But this is worse.
“One thing I never signed up for was bringing something home that could kill my family,” he said. “Healthcare workers [are] without adequate [personal protective equipment] and their families are going to pay the price.”
Pamela Wu, spokeswoman for UC Davis Medical Center, said in an email Friday that the facility “currently has sufficient supplies of personal protective equipment (PPE),” but has “revisited our storage of PPE, specifically masks, after some instances of theft, so they are now kept more securely.”
As administrators, doctors and staff navigate the shortages, trust and patience are also drying up.
UCLA emergency room nurse Marcia Santini said she and other nursing staff recently received an email from UCLA that their N95 masks will be sterilized using ultraviolet irradiation. Each nurse will label her mask, place it in a paper bag and it will be put in a machine for ultraviolet germicidal irradiation, according to the email.
“The nurses are very, very concerned about that,” she said. “Does it get all the nooks and crannies? Will the integrity of the mask hold up? Will it still fit your face the same way?”
UCLA confirmed in a statement that it was using UV light to disinfect N95 masks.
“This is a validated process to kill viruses,” the statement read, adding that it is one of the first healthcare systems in the nation to use the method.
A nurse who works at USC’s Keck Hospital said her facility is changing “how we are using our PPE on a daily basis.”
That, she said, has led to “a lot of anxiety, and I think a lot of anger.”
The nurse said it had been long-standing custom to dispose of an N95 mask after treating a patient with an infectious disease. Now, the rules keep shifting. First, nurses were told to wear the mask for four hours, then eight hours. Then the hospital started instructing nurses to put their N95 masks in a UV light box and zap the bacteria off, a process that took about 60 seconds.
“We said OK, but the masks smelled like they were burning,” she said.
After nurses questioned whether the UV light was frying the filter and compromising the efficacy of the mask, the hospital rolled out a new policy, she said.
Masks are put in a brown paper bag after each use and picked up by housekeeping, she said. The next day, a nurse returns to find a white paper bag with their name on it, and the cleaned mask inside.
“It feels like they are making it up as they go,” she said.
In a statement, Keck Medicine of USC did not dispute the account and said it was following guidelines set by the University of Nebraska Medical Center for extending the use of N95 masks. The masks were being disinfected with UV light from Xenex robots.
“As we believe that Los Angeles has not yet peaked in COVID-19 case volume, we are therefore continuously assessing our PPE resources, while ensuring the health and safety of our health care providers,” Keck said in the statement.
Other nurses are frustrated by being asked to do jobs they aren’t comfortable with. One nurse without experience in intensive care said that with elective surgeries canceled and his normal work dwindling, he’s now being pushed to handle serious cases of COVID-19.
“I’ve never done ICU,” he said. “I’ve never wanted to.”
A nurse at Cedars-Sinai Medical Center, where there are a few dozen COVID-19 patients, complained that doctors there have had more consistent access to N95 masks and other more sophisticated protection gear while nurses caring for such patients often are told to wear simple surgical masks.
It seemed wrong to her, she said, because nurses spent more time in the patients’ rooms.
“We are the ones face-to-face with these people,” she said.
She said nurses are told to clean and reuse some face shields, and that the protective sheets become dimpled upon repeated washing, leaving her wondering if it’s working.
“By the end of the day, I can smell medicines through the [shield],” she said.
Cedars-Sinai said in a statement that it offers “a single standard of protection for doctors, nurses, respiratory therapists, environmental health personnel, chaplains and other staff who work in patient areas” and that its procedures are “consistent with guidance from national, state and local public health authorities.”
Despite the doubts and creeping trepidation, medical providers who spoke to The Times shared one resolve: to remain on the job, providing care, even as the risks mount.
When Dr. Amit Gohil, a pulmonary critical care doctor at Santa Clara Valley Medical Center, dons his full protective gear to enter a COVID-19 patient’s room, it is quiet and still, with only the sound of a ventilator.
His county has been one of the hardest hit so far with more than 1,000 positive cases as of Friday, with 245 patients in hospitals and 92 in intensive care.
At those bedsides, Gohil finds calm and purpose.
“Even if people are dying, you really feel like you can care for them,” Gohil said. “Your whole life has come to this pinnacle.”
Times staff writers Paul Pringle and Phil Willon contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.