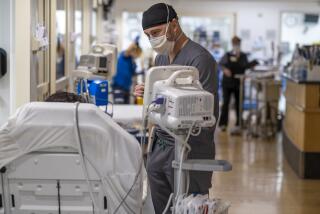
California hospitals desperate for safety supplies, fear ‘disaster’ as coronavirus wave hits

- Share via
SACRAMENTO — Dr. Frank Candela, chief of staff at West Hills Hospital in the San Fernando Valley, started a GoFundMe last week to raise money for more safety gear at his medical center, where masks and face shields are running short as coronavirus cases mount.
As of Wednesday night, he’d raised more than $48,000. But he can’t find much to buy.
“We’ve been walking around waving money and there isn’t anybody who has supply right now,” Candela said, calling it “such a difficult situation.”
Like Candela, medical providers and hospital administrations across the state and country are desperate for personal protective equipment and other essential goods as COVID-19 patients hit emergency rooms and intensive care units in growing numbers. Nurses and doctors are pleading for donations online, telling stories of reusing masks and rigging trash bags as gowns.
Gov. Gavin Newsom said Wednesday that the worst was yet to come, both in illness and need. He said he expects the state to require 66,000 hospital beds by the end of May, with 40% of those projected to be patients who may require ventilators — of which the state currently has 4,252.
With the federal government slow to act on obtaining those vital goods and largely pushing the responsibility onto governors, California has been purchasing its own. But some on the front lines say it’s not enough to stem the chaos and shortages. The state, they say, needs to step up efforts to both buy and distribute key items and ensure they go to those with the greatest need, not just to those with luck and money.
“We are seeing an incredible ad hoc approach by private hospitals — everybody is trying to go out after the same commodities,” said Nick Vyas, executive director of the Center for Global Supply Chain Management at USC. “We should have a SWAT team at the state level coordinating this effort on behalf of our hospital network.”
Without such federal or state leadership, “what you create is vacuum and void, and all the vultures will step in and try to pick it apart,” he warned.
In recent days, Newsom has touted the state’s unique buying power as the world’s fifth-largest economy, as well as his efforts to procure the protective gear while at the same time working to help other states. Newsom has said he’s secured more than 100 million of the coveted N95 masks on order and is working to rapidly increase ventilators through private manufacturing.
After Long Beach-based Virgin Orbit reached out to the state last week, California officials connected the rocket maker with academics who had designs for a simple ventilator that could work for some patients. A Virgin spokesman said Wednesday that the company had already started producing and testing them and was waiting for federal Food and Drug Administration approval before ramping production up to hundreds or even thousands of units a week.
“We are not waiting around for others,” Newsom said Wednesday.
But the state does not monitor what supplies each hospital has on hand and instead relies on requests for additional equipment to determine how to prioritize shipments, said Brian Ferguson, spokesman for the governor’s Office of Emergency Services.
Ferguson said hospitals have been sending their requests to county emergency coordinators, who decide whether they are urgent enough for state attention. If they are, California contacts the Federal Emergency Management Agency to fill those orders.
Los Angeles County, however, is able to circumvent the state’s process and directly contact FEMA to order supplies, Ferguson said. Los Angeles Mayor Eric Garcetti said the city was in good shape on Tuesday, but was concerned about the days ahead. “We can’t have certain parts of the country have a big cache and us having nothing,” he said.
Ferguson said the state has been prioritizing requests for much-needed masks and ventilators based on the outbreak in certain areas and immediate needs of individual hospitals.
“If one has three days of supplies, they are prioritized over another with five days,” Ferguson said. “There are a lot of folks who make requests for more than they need, but being in short supply we have to prioritize.”
Ferguson added: “We are sending things out the door as fast as we can get them in order to meet the needs at the local level.”
But as competition continues to snowball in the open market, the state is doing little to intervene. Hospitals are competing against each other, fake supplies are flooding the market and price gouging is rampant, said experts and those attempting to buy.
Even with the Virgin ventilators, facilitated by the state, there is no guarantee where they will go. Requests to buy them are already flooding in from across the globe, and they will probably be sold on the open market, though California may have preference.
“Here’s what I see: I see a disaster on the brink of happening,” San Mateo County Supervisor David Canepa said at a meeting of the Board of Supervisors on Tuesday, speaking of the shortage of personal protective equipment at Seton Medical Center in Daly City.
Seton, recently leased by the state to care for COVID-19 patients, is caring for eight people with the virus and six others who are suspected of having the disease. After a county official said the state had been unresponsive to calls for help, Canepa said: “Us not hearing from the state is problematic. Because we don’t have the resources — the hospital can only acquire 20% of what they need.”
Mike Callagy, San Mateo County manager, said the county had asked the state Emergency Medical Services Authority for the personal protective equipment, “and they simply do not have them.... The state really needs to push on the feds to get those supplies in so they can be distributed down through the system that’s in place here.”
But unfortunately, “they’re not fulfilling all those requests, because they themselves are rationing,” said Louise Rogers, chief of San Mateo County Health. “The state has indicated that eventually that they’re going to try to fulfill them. But that has not happened.”
With so many vying for the same supplies, some on the front lines are scrounging for gear one piece at a time.
“I’ve been working with my staff to go to Sally’s Beauty Supply, to go to Autozone, to go to all these types of places,” said Crystal Solorzano, the chief executive of ReNew Health Group, which operates skilled nursing facilities in California. “We wouldn’t have even imagined we’d have to go to these stores just to have a backup supply because we’re seeing the supplies diminished so much.”
John Thomas, president of the newly formed Blue Flame Medical, said the shortages are particularly hard on small organizations, which can’t catch the attention of buyers with so many big players in the market.
On top of that, the market is dominated by middlemen who often have little idea if the goods they are selling even exist, he said.
“Truthfully, it’s a … nightmare. It’s even worse than you believe,” Thomas said.
Thomas’ company typically supplies large orders. It also recently turned its attention to smaller buyers, because it saw no one was paying attention to their needs, he said.
“We’ve got thousands of requests from small agencies saying, ‘I need 50 masks, 100 masks,’” Thomas said. In this environment, he added, there is no supplier willing “to pay attention to the guy who needs 50 masks.”
Thomas said his company has been able to ramp up capacity by building relationships with domestic apparel manufacturers who agreed to convert their factories for full-time production of personal protective equipment.
Those kind of make-do solutions are becoming more common as those with needs and those with know-how combine in a furor of patriotism and increasing panic.
In Long Beach, a distillery has turned from vodka to raw alcohol — another basic in short supply — to make hand sanitizer. A 3-D printer in Oakland is making masks. And Gap Inc. has asked its factories to switch from consumer clothes to gowns and other medical garments.
At St. John’s Well Child and Family Center, a nonprofit that operates 18 health centers and school-based clinics in Los Angeles and Compton, the situation has become so dire that patients have offered to sew surgical masks for the staff.
In a news teleconference Tuesday, St. John’s Chief Executive Jim Mangia said it wouldn’t be enough and called on the federal government to mandate the production of protective gear and masks for healthcare workers.
“The president invoked the Defense Production Act; he’s used it to force [General Motors] to create ventilators,” Mangia said. “But he’s not using it for the production of protective gear and masks for front-line healthcare workers.”
Candela, the doctor with the GoFundMe, worries his staff will pay with their lives. He has watched with dread as doctors in other parts of the world and country die from exposure, and he sees the stress building for everyone in the hospitals, including janitors, cafeteria workers and others.
“We’re literally repeating history,” he said, referring to the hospitals overwhelmed in China, Italy, New York and other places. “I can see it in their eyes and they’re scared, yet they’re showing up.”
Late last week, Candela purchased a box of 25 coveralls, which resemble hazmat suits, for the nurses to wear. The hospital had five COVID-19 patients and many others who had the disease’s symptoms, he said.
Candela told the man who sold him the coveralls that he wanted to buy 500 more. But by Monday, the suits had been sold.
Candela believes he was bigfooted by the government or a bigger corporation.
“Somebody showed up at the warehouse and commandeered the stockpile,” he said. “What we’re finding is these times bring out the best of people and the worst of people.”
Times staff writers Adam Elmahrek and Dakota Smith contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.