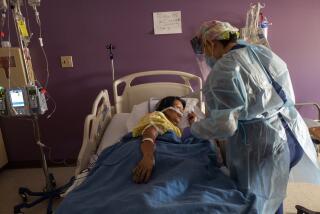Why COVID-19 has left so many hospitals running low on oxygen
- Share via
Can California address the shortage of life-saving oxygen at some hospitals overwhelmed by coronavirus cases?
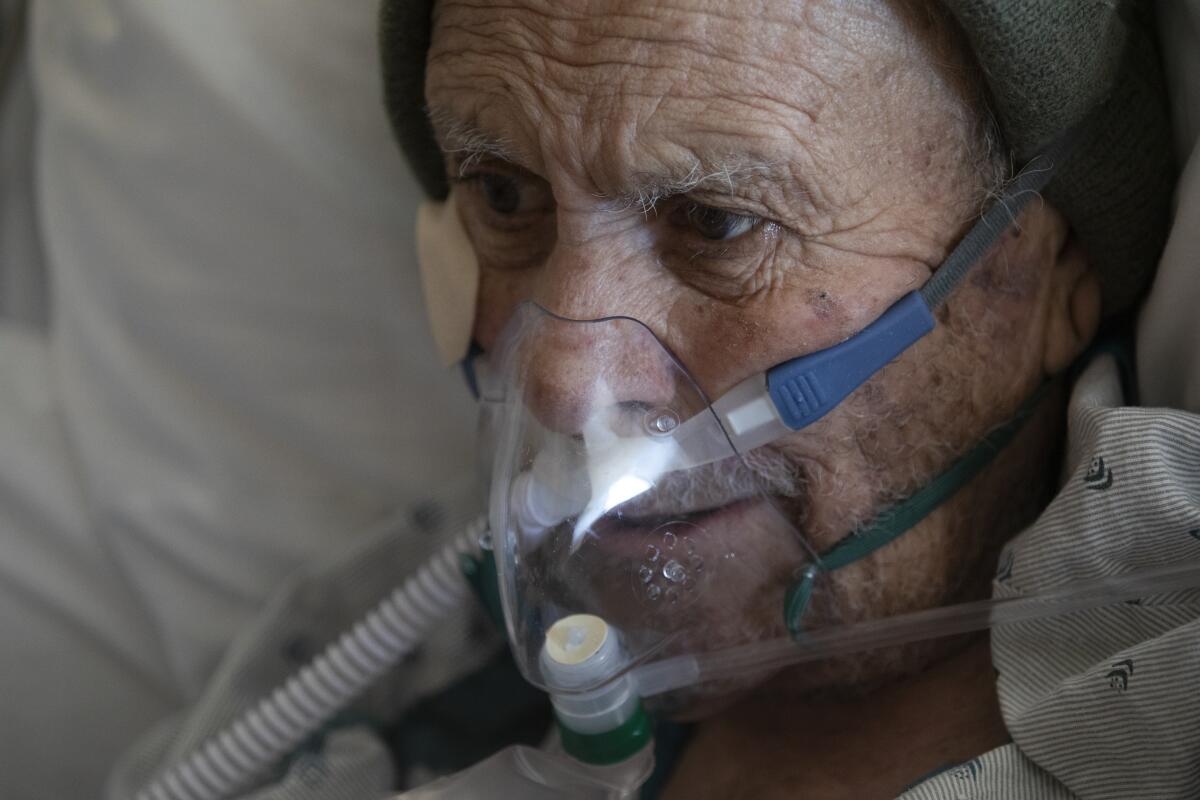
The demand for oxygen has skyrocketed, as critically ill COVID-19 patients often need high rates of oxygen flowing into their lungs to keep them alive, helping them to overcome a perilous moment when their lungs are inflamed and their oxygen levels in the body become dangerously low.
Problems on Dec. 27 with hospital oxygen systems caused five hospitals in L.A. County to declare an “internal disaster,” which allows a facility to close its emergency room to all incoming ambulance traffic. That’s a rare situation; traditionally, when emergency rooms are full, only certain types of ambulance traffic are diverted elsewhere.
Fully repairing the crippled oxygen distribution systems at aging hospitals throughout Southern California may end up being a complicated endeavor.
The U.S. Army Corps of Engineers last week was wrapping up assessing 11 aging Southern California hospitals in urgent need of evaluation, largely focused on oxygen distribution systems that have had significant problems and are essential for critically ill COVID-19 patients gasping for air as their inflamed lungs fail.
Some of the oxygen systems evaluated were found to be heavily frosted “just from the constant increased demand for oxygen,” said Mike Petersen, spokesman for the Army Corps of Engineers.
Some of the systems were in particularly rough shape, Petersen said, and the accumulation of frost and ice was significant. “We’re doing everything we can to keep them operating.”
Compressed oxygen is very cold, and can freeze condensation that builds up around pipes. The freezing can worsen with ever-more increasing amounts of compressed oxygen that flows through the system. Frozen pipes can lead the oxygen distribution system in a hospital to stop working.
But it’s not easy to remove the frost or ice that has built up around the pipes. It wouldn’t be wise, for example, to take a blowtorch to melt the ice around a pipe containing compressed amounts of highly flammable purified oxygen.
The Army Corps of Engineers was also asked to evaluate how to address the potential need for greater bed space at hospitals.
The teams have begun to send their evaluation reports to the Federal Emergency Management Agency, which asked the Army to undertake the evaluations, and will await further instructions.
The Army Corps of Engineers was asked to evaluate the hospitals on Dec. 31 and began evaluating hospitals by Jan. 1. Reports are being written and filed with FEMA.
Initially, the Army Corps of Engineers was asked to evaluate six hospitals; that has since been expanded to a total of 11 hospitals. Here is a list of the hospitals.
Beverly Hospital, Montebello
Mission Community Hospital, Panorama City
San Antonio Regional Hospital, Upland
Lakewood Regional Medical Center, Lakewood
Adventist White Memorial Medical Center, Boyle Heights
Good Samaritan Hospital , Westlake
Emanate Health Queen of the Valley Hospital, West Covina
PIH Health Downey Hospital, Downey
Providence Saint Joseph Medical Center, Burbank
Providence Holy Cross Medical Center, Mission Hills
Providence Little Company of Mary Medical Center, Torrance
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.