California vs. Florida: Who handled COVID-19 better?

- Share via
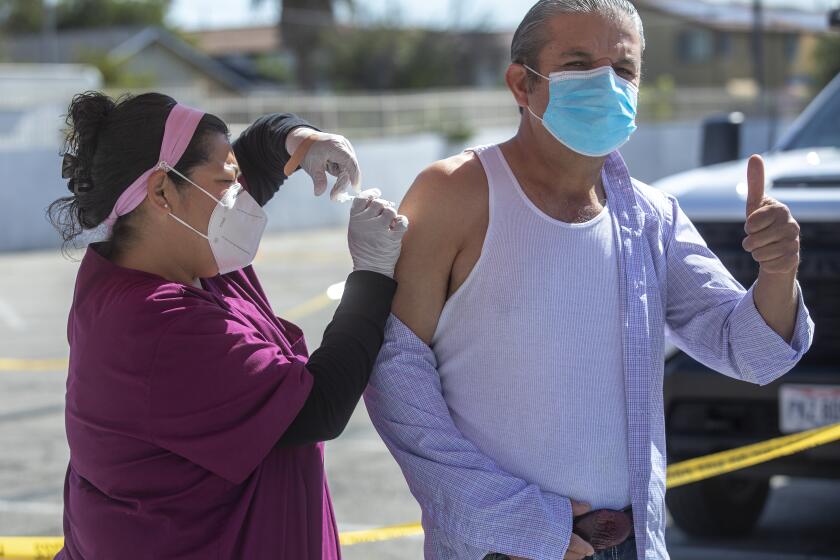
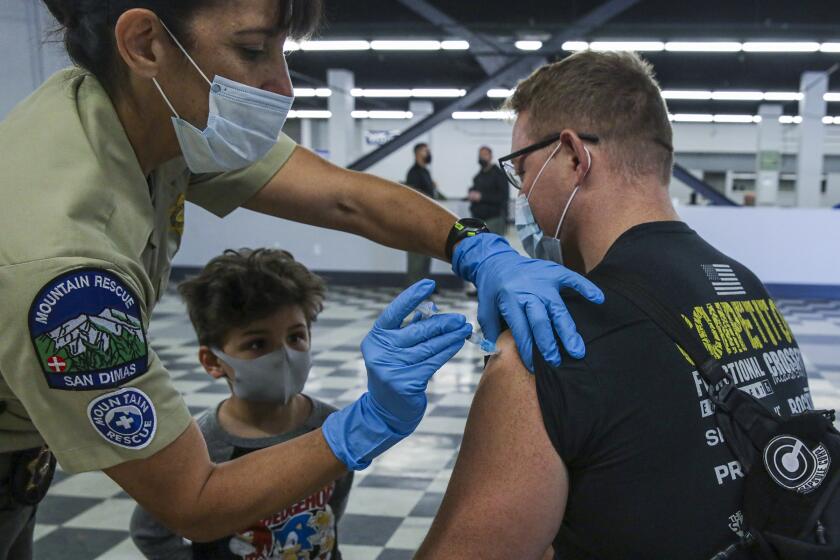
From the earliest days of the pandemic, California and Florida took significantly different courses in responding to the crisis, approaches that came to symbolize the deep divisions across America on how best to respond to the coronavirus.
California imposed myriad restrictions that battered the economy, and have left most public school students learning at home for a year. Florida adopted a more laissez-faire approach decried by public health experts — allowing indoor restaurant dining, leaving masks optional and getting children back in classrooms sooner.
For much of the last year, it seemed that California’s response under Democratic Gov. Gavin Newsom had led to a dramatically lower COVID-19 death rate. Florida had a cumulative rate as much as 84% higher than California’s last fall. But the winter surge slammed California, and that gap narrowed to 11%.
Now, Republican Florida Gov. Ron DeSantis is garnering praise in some conservative circles while Newsom is facing a potential recall over his handling of the crisis. A recent Wall Street Journal opinion article called the numerical comparison between the two states DeSantis’ “vindication.”
But experts say turning the complex evaluation of the pandemic into a blue-versus-red political showdown is unwise and deceptive, as each state had its own unique vulnerabilities and assets.
The shrinking difference in the death rates is likely the product of California’s higher levels of poverty, density, overcrowding and climate that make it particularly susceptible to coronavirus spread, experts say.
Americans are warming up to COVID-19 vaccines, with 19% saying they’ve already received at least one dose and 49% intending to do so when they get the chance.
“The comparison of California and Florida is not fair,” said Ali Mokdad, an epidemiologist at the Institute for Health Metrics and Evaluation at the University of Washington. “California is a much harder situation than what Florida has to deal with.”
And still, California better controlled the virus. If California had Florida’s death rate, roughly 6,000 more Californians would be dead from COVID-19, and tens of thousands of additional patients likely would have landed in already overburdened hospitals. And if Florida had California’s death rate, roughly 3,000 fewer Floridians would be dead from COVID-19.
That’s “a lot of people whose lives got wrecked, and a lot of people who aren’t with us anymore,” Los Angeles County Public Health Director Barbara Ferrer said. It “absolutely is worth it to do everything you can to slow the spread of a deadly virus that wreaks havoc on people’s lives and really almost took down L.A. County’s hospital care system.”
Regardless, the comparison of Florida and California has caught the eye of some public health experts. They are confident that mask wearing and staying home reduce the spread of the coronavirus but acknowledge that California’s strict rules became less effective as exhaustion set in by late 2020.
“If I had to do it again, I’d still do it the way California did it. But I do think you do have to come away with some humility,” said Dr. Robert Wachter, chair of UC San Francisco’s Department of Medicine. “One might’ve expected that the Floridas of the world would’ve done tremendously worse than the Californias of the world, and they did worse, but modestly worse, and there’s something to be learned there.”
More Coverage
California and Florida took vastly different approaches to COVID-19, generating debate about which state fared better. Here’s what the numbers show.
‘Comparing apples and oranges’
When it comes to California and Florida, it isn’t an even playing field.
About 55% of California residents live in counties with a high “social vulnerability” score — a measure of how severely a disease outbreak might affect a region — while only a quarter of Floridians do. California’s rate of overcrowding in homes, a metric linked to coronavirus spread, is also more than double Florida’s.
“In many places we have much greater vulnerability than Florida, so it’s comparing apples and oranges,” L.A. Mayor Eric Garcetti said.
The dry air in California may also be a challenge, especially compared with humid Florida. Researchers are still learning about how climate affects the coronavirus, but some studies suggest that when the air is humid, virus droplets fall to the ground faster, so people are less likely to become infected.

California also has a longer flu and pneumonia season, a pattern that the coronavirus tends to follow, Mokdad said. And in the fall, there may have been an extra-contagious strain of the virus circulating locally that further complicated matters.
Because of the many ways California is more susceptible to coronavirus spread, replicating Florida’s relaxed approach may have had devastating consequences here. Arizona, which has lax restrictions similar to Florida’s, has the nation’s fifth-highest COVID-19 death rate. An additional 38,000 Californians would be dead if the state’s per-capita deaths matched Arizona’s.
“If California had behaved like Florida, where mask use and physical distancing was not being practiced as thoroughly, our cumulative death rate would have been higher than Florida,” UCLA medical epidemiologist Dr. Robert Kim-Farley said.
“And conversely, had Florida been practicing California’s more rigorous attention to masking and physical distancing, curtailing indoor dining, et cetera, it would have followed a death rate trajectory that would have been the same or lower than California … because their vulnerability index was lower.”
Wildly different approaches to COVID-19
On Friday, the federal Centers for Disease Control and Prevention released a study of the nation’s more than 3,000 counties that found that mask mandates were linked to a significant reduction in COVID-19 deaths. Counties that allowed restaurant dining generally noted an increase in virus-related deaths within three months, the study found.
The findings have been echoed elsewhere.
A recent analysis by the American Enterprise Institute showed that since July 1, a turning point in the pandemic due to improvements in the treatment of disease, states with the highest death rates all had loose coronavirus restrictions: South Dakota, Arizona, Mississippi and Alabama. Florida ranked 19th and California 25th.
“The states that didn’t implement as stringent measures, they did pay a price for it. And I don’t think that you can explain that away,” said Dr. Scott Gottlieb, a resident fellow at the institute and a former head of the U.S. Food and Drug Administration in the Trump administration, on CBS’ “Face the Nation.”
But not all states’ death rates align perfectly with their policies. Arizona and Florida both had lax rules, but Arizona’s death rate was far worse. And Hawaii and Vermont, whose rules are similar to California’s, have the two lowest death rates in the nation.
“How do we explain that?” asked Neeraj Sood, vice dean for research at the USC Price School of Public Policy. “It is perplexing.”
Sood said other factors, such as demographics, cross-immunity to the virus or climate may be just as, if not more, important than policy in determining states’ outcomes, though he is continuing to study the trends. He added that weak enforcement of coronavirus rules might also make policies less effective than one would anticipate.
For example, under California’s patchwork of rules, “you can still go to the grocery store, hang out there. We can go to some malls but not others, get a haircut. It’s just kind of arbitrary and there’s no enforcement,” Sood said. “Ultimately, this is a very contagious respiratory virus, and if you have that amount of activity, people are going to get infected.”
Even within California, L.A. and the Bay Area counties have largely maintained generally similar policies throughout the pandemic, yet the Bay Area’s death rate is one-third that of L.A. County’s. This is likely due to L.A.’s huge number of essential workers, extreme levels of overcrowding and population less receptive to restrictions, experts say.
If L.A. County’s deaths are subtracted out of California’s total, Florida’s death rate would measure 39% higher than the state’s. It is L.A.’s vulnerabilities that drove California’s surges and pushed its total death rates so close to Florida’s.

There are a few possible reasons for Florida’s relatively lower death rates despite its lax policies. The warm weather allowed people to congregate outdoors year-round, a low-risk activity that was banned in many parts of California for months — a decision that may have backfired here, Florida epidemiologist Cindy Prins said.
“Are we creating a situation,” Prins said, “where people are just like, ‘Forget it. I’m going to have people over to my house?’”
Prins also said that Florida’s older population might have, perhaps counterintuitively, prevented the virus from spreading as quickly as it did in California. Worldwide, young adults who socialize and mingle, either at work or in social settings, tend to spread the virus the most while older people are more cautious and stay home. Florida’s population is the fifth-oldest nationwide.
Weighing the costs of saving lives
In a recent public address, DeSantis noted that state revenue in the winter far exceeded projections and that public schools had been open since August. He boasted of the state’s COVID-19 death rate that is 25th highest in the nation (California is 29th).
“We don’t want people to have to be isolated in their homes being scared. We want you to be able to have confidence to go out, see your friends and family,” he said. “You see a lot of these other states that are so intent on closing people down. We’ve lifted people up. We’ve trusted Floridians. They’ve responded.”
Since February 2020, 1.63 million jobs have been lost in California, and its unemployment rate has more than doubled to 9.3%, according to data from the U.S. Bureau of Labor Statistics. Florida’s unemployment rate increased less, from 3.3% to 5.1%.
The potentially accelerated opening in parts of Southern California, including Orange County, is possible thanks to a revamp of California’s coronavirus reopening blueprint.
But California’s state budget outlook is surprisingly robust. While unemployment rose sharply through much of 2020, millions of middle-class and high-wage workers were able to keep their jobs and work from home. Tax collections also rose after a strong stock market boosted capital gains earned by the state’s wealthiest taxpayers.
While California is forecasting a state budget windfall, Florida is grappling with a state budget shortfall.
Newsom has often defended his approach as one focused on saving lives and professed confidence that the economy would recover strongly after widespread vaccinations. The UCLA Anderson Forecast expects a post-pandemic California will enjoy a pace of economic growth faster than the nation as a whole.
“Our hotels, our restaurants, our entertainment — we’re going to come roaring back once this pandemic is behind us,” Newsom said last week.
Duke economist Duncan Thomas said the economic tolls stretched far beyond unemployment rates. Keeping millions of Californians working from home likely led to drops in productivity for many, especially for parents juggling jobs and child care, while school closures harmed students’ education and development.
The losses caused by the pandemic will probably affect both states for a long time to come, he said.
“I would not say Florida was the right model or California was the wrong model,” Thomas said. “I would say the epidemiologists have focused only on infection and mortality, and that was an error.”
Times staff writers Deborah Netburn, Sean Greene and John Myers contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.