Inland Empire struggling with high COVID hospitalization rates as Omicron wave arrives
- Share via
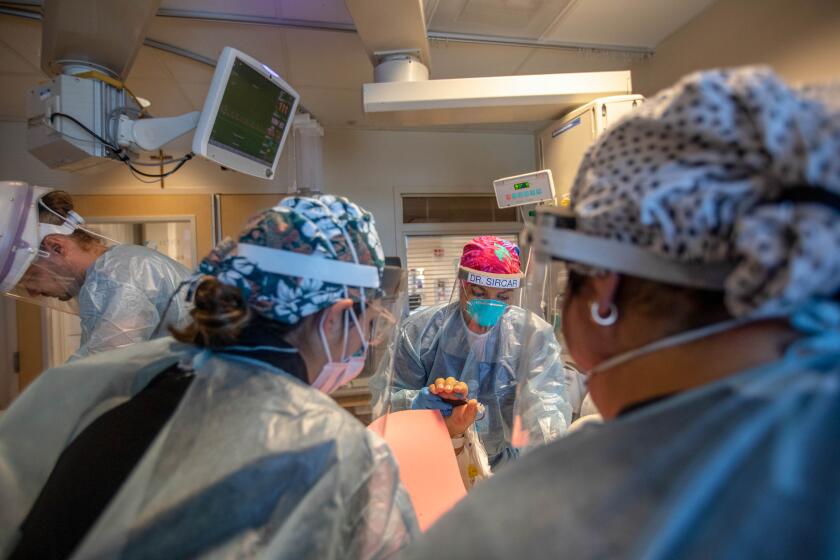
The crowded conditions at some Inland Empire hospitals are generating concern as officials get ready for the spread of the highly infectious Omicron variant.
While hospitals are in better shape now than they were during last winter’s COVID-19 surge, Riverside and San Bernardino counties are seeing a higher rate of COVID-19 hospitalizations than other areas of Southern California.
Some smaller hospitals have requested tents and portable medical facilities to help keep up with demand. And wait times for ambulances to get patients into hospitals have been at record highs in some locations — a problem that has persisted since the summer.
Officials are urging people to avoid emergency rooms unless there’s a severe problem, and to rely on urgent care centers for problems like sprained ankles.
Larger hospitals, however, appear less crowded and some officials express optimism that this winter’s wave will not be as bad as last year’s, thanks to COVID-19 vaccines available and people slowly getting booster shots.
Since Oct. 15, the number of COVID-19 hospitalizations in San Bernardino County has jumped by 74%, from 236 to 411.
In Riverside County since Dec. 1, the number of COVID-19 hospitalizations rose by 34%, from 239 to 320.
When California fully reopened at the beginning of the summer, hospitalizations were low across Southern California. But when the Delta wave began, the Inland Empire fared far worse than its coastal neighbors, such as Los Angeles and Orange counties — and it never recovered.
Now, Riverside and San Bernardino counties have the highest hospitalization rates in Southern California’s most populated areas.
The increase is likely linked to low vaccination rates, officials say. “The higher rate of vaccine hesitancy and resistance in San Bernardino County is definitely a factor,” Dr. Michael Sequeira, the San Bernardino County health officer, said in a statement.
In San Bernardino County, more hospitalizations are being reported among younger people, a trend mirrored in the Central Valley, which also suffers from low vaccination rates.
“Admissions in hospitals serving younger populations have increased more than the other hospitals,” Sequeira said.
Contributing to the rise were “people letting their guard down” with holiday gatherings and travel, said Dr. Troy Pennington, an emergency room physician with Arrowhead Regional Medical Center. The public hospital in Colton, which is run by San Bernardino County, is averaging 15 to 20 COVID-19 patients, most of whom are unvaccinated.
Pennington said he is concerned about the rise in Omicron cases, which is expected to continue; the first confirmed cases of the new variant were reported in the Inland Empire last week — a man who lives in Redlands and traveled to an out-of-state conference, as well as a 41-year-old man who lives in western Riverside County.
Conditions could lead to ‘a perfect storm for overwhelming our hospital system that is already strained,’ a health official says.
Even if Omicron infections result in milder coronavirus illnesses, “it’s much more easily transmissible,” Pennington said of the variant, and “some of those people, they’re going to have more significant illness.”
In San Bernardino County, only 59% of residents of all ages have received at least one dose of vaccine, while in Riverside County, that number is 63%. By comparison, Los Angeles and Orange counties report a vaccination rate of 75% among all residents, and Ventura County has 74%. The statewide rate is also 74%.
Those rates likely explain the Inland Empire’s hospitalization numbers, experts say. For every 100,000 residents, San Bernardino County has 19 people hospitalized with COVID-19; Riverside County has 13.
By comparison, Orange County’s rate is 6, L.A. County’s is 7 and Ventura County’s is 9, which is also the statewide rate. Some health officials say a rate of 5 or higher is cause for concern.
Prepare for big spikes in COVID-19 hospitalizations and deaths in areas with low vaccination rates, experts say.
In San Bernardino County, a number of challenges are contributing to higher COVID-19 hospitalization rates, Sequeira said.
Besides lower vaccinations, San Bernardino County has higher rates of diabetes, heart disease and obesity. In addition, many residents live in crowded homes and must go to a workplace for their jobs, putting them at higher risk of exposure to the virus and the potential to suffer from severe complications.
San Bernardino County also has a relatively high number of people living in nursing homes. Seniors living in such facilities are more likely to be hospitalized should they contract COVID-19.
Despite the challenges, Bruce Barton, Riverside County’s emergency management director, said he is optimistic things will not be nearly as bad as last winter’s surge, when vaccinations were not available to most people. While Riverside County had 320 COVID-19 patients in its hospitals Monday, there were nearly four times as many — 1,239 — this time last year. In San Bernardino County, hospitalizations tallied 411 on Monday, while one year ago, they stood at 1,545.
Still, Kaiser Permanente’s hospitals in Fontana and Ontario have seen an increase in COVID-19 patients, with 60 to 70 hospitalized in recent weeks. And between 80% and 85% of those hospitalized are unvaccinated, data show.
Dr. Timothy D. Jenkins, area medical director and chief of staff for Kaiser Permanente San Bernardino County, said staff members haven’t had a break from COVID-19 in almost two years, and it has been challenging to keep up morale and forgo traditions such as holiday parties. They are working to make sure employees get time off during the holidays to rest and see loved ones, he said.
But, Jenkins said, it will be important to sustain efforts to combat the virus in the new year. That includes encouraging community members to continue wearing masks and getting vaccinated and boosted as the Omicron variant circulates and pandemic fatigue increases.
“I would love nothing more than for COVID to be in the rearview mirror. Unfortunately, it’s still with us, and it will be well in to 2022 — and maybe beyond that,” Jenkins said. “And so I know there are questions out there about all of this and people are ready for it to be behind us, but we’re just not there yet.”
Dr. Anil Jagtiani, chief of infectious diseases for Kaiser Permanente San Bernardino County, said that severe COVID-19 infections have been staved off by high vaccination rates as well as monoclonal antibody treatments — a regimen to counteract the coronavirus before it can begin destroying the body’s organs.
The U.S. Food and Drug Administration is currently reviewing other oral medications that may be helpful, including molnupiravir and Paxlovid, both of which can reduce the risk of progression of COVID-19 in patients with mild to moderate symptoms.
Jagtiani said it’s unclear which will be more beneficial, but “a lot of us are excited about the ability to be able to treat patients in the outpatient setting before they need hospitalization.”
“[Monoclonal antibody treatments] are certainly not the answer, but they’ve helped us reduce the number of cases we’ve seen progress in severity end up in the hospital,” Jagtiani said. “Ultimately, it seems like the fight really is going to be to prevent progression of the disease, as it seems to be getting harder and harder to just completely stop transmission.”
In the Coachella Valley, doctors say a winter surge comparable to this summer’s spike will overwhelm its hospitals.
“We hope it’s not as severe as Delta because otherwise, we’ll be back in the same place we were last January, or potentially worse, with all the hospitals being overwhelmed,” Dr. Adrian Cotton, chief of medical operations for Loma Linda University Health, said. But, he added, “I do think our risk of being as bad as December, January last year is relatively low with the number of patients that have either received a vaccine or have had COVID.”
Cotton said it’s important for people to avoid using emergency rooms as much as possible as visits put patients at risk of exposure.
“If you think you’re going to die within the next 24 hours, you probably need to go to the emergency room. For almost anything other than that, you could be seen somewhere else,” Cotton said.
“A lot of people use the emergency room for things that don’t need to be seen: a mild urinary tract infection or a sprained ankle or something along those lines. Again, there’s more appropriate places to be seen than the ER for that.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.