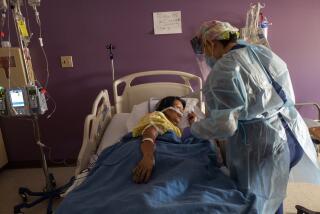Omicron brings fewer serious illnesses, but California hospitals are overwhelmed as cases soar
- Share via
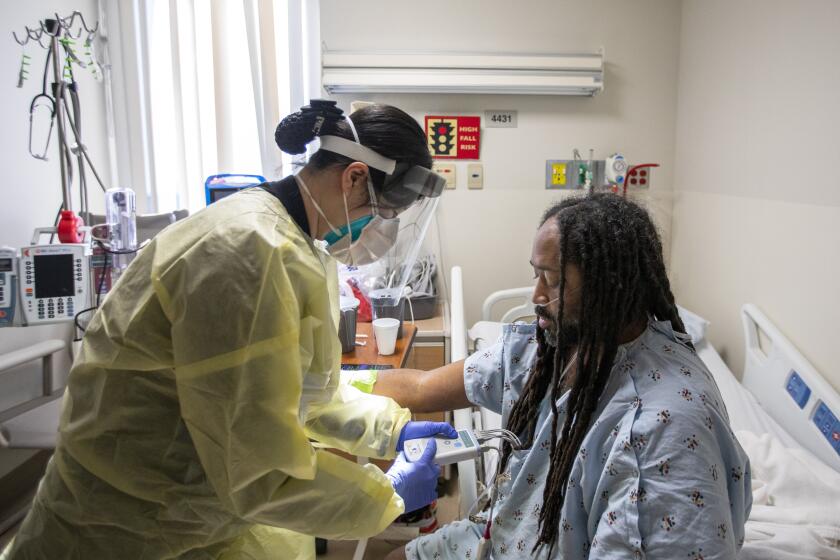
California’s healthcare system is expected to face continued stress in coming weeks as the Omicron variant spawns new waves of coronavirus infection, even as new research shows the latest phase of the pandemic is producing significantly less severe illness.
Officials say they are focusing on protecting hospital operations, which are facing severe staffing shortages as workers get infected, but they hope the system can withstand Omicron. They continue to urge people to do all they can to avoid getting infected.
Omicron “is less severe than previous variants,” Gov. Gavin Newsom said at a press briefing in Paramount on Wednesday. Intensive care units are nowhere near as busy with COVID-19 patients as they were a year ago.
But it’s also true that never before in the pandemic have so many people been simultaneously infected with the coronavirus. And that is leaving emergency rooms inundated, ambulances facing delays dropping people off at hospitals, and patients seeing their scheduled surgeries canceled.
There is “enormous pressure, ultimately, on our healthcare system,” Newsom said.
Kaiser Permanente Southern California temporarily postponed all scheduled surgeries that require an inpatient stay in the hospital after an operation. The move came after a number of hospital systems across California reported being forced to postpone at least some scheduled procedures.
And the Los Angeles County Department of Public Health has begun reporting what officials called a “troubling increase” in COVID-19 deaths. On Wednesday, L.A. County reported 39 COVID-19 deaths, the highest daily tally since Sept. 22, when the summer Delta surge was fading.
Nonetheless, Newsom and others have expressed guarded optimism that Omicron’s meteoric rise may be met with an equally quick fall — a trend experienced in other countries where the variant arrived earlier.
Newsom noted that, in some parts of the U.S., “we’re starting to see, in the last three or four days, some case leveling. That’s going to happen here in the state of California as well.”
“We’re going to get through this — just a few more weeks,” he said.
L.A. County has identified the 20 most hard-hit emergency rooms, and county employees have been dispatched to the top 10 — all privately run hospitals.
Computer models suggest that the peak of the Omicron wave may come sometime in late January — maybe next week, said Dr. Kirsten Bibbins-Domingo, chair of the UC San Francisco Department of Epidemiology and Biostatistics. And while there will likely be a lot of viral transmission in the weeks after the peak, by the time the Super Bowl is held at SoFi Stadium in Inglewood on Feb. 13, it’s possible that conditions will be similar to “where we were in the middle of December.”
“I do think it is reasonable by the middle of February that we will really be in a substantially better place,” Bibbins-Domingo said.
As more data are gathered, it’s becoming clearer that Omicron is causing less-severe illness than its Delta cousin — the culprit behind last summer’s wave.
A study of data from Kaiser Permanente Southern California released this week, for instance, “noted substantially reduced risk of severe clinical outcomes in patients who are infected with the Omicron variant compared with Delta,” according to U.S. Centers for Disease Control and Prevention Director Dr. Rochelle Walensky.
The study — which analyzed more than 52,000 Omicron cases and nearly 17,000 Delta cases within the Kaiser system from Nov. 30 to Jan. 1 — found that, compared to Delta, Omicron was associated with a 53% reduction in the risk of symptomatic hospitalization, a 74% reduction in the risk of intensive-care admission and a 91% reduction in the risk of death.
None of the studied Omicron-infected patients required mechanical ventilation. The median length of stay for a hospitalized Omicron patient in the Kaiser study was 1.5 days, compared to five days for Delta.
“The data in this study remain consistent with what we are seeing from Omicron in other countries, including South Africa and the U.K., and provide some understanding of what we can expect over the coming weeks as cases are predicted to peak in this country,” Walensky said during a briefing Wednesday.
Officials say they continue to expect an extraordinary number of infections in coming weeks.
The number of new coronavirus cases reported daily has soared in California, now averaging an astonishing 101,000 cases a day over the last week, far above last winter’s pandemic record of 46,000 cases a day.
Promisingly, a smaller percentage of coronavirus-positive patients need treatment for COVID-19 now; data show that just 4.5% of those infected with Omicron are hospitalized, Newsom said; last year, 15% to 20% of coronavirus cases led to hospitalizations, L.A. County has said.
But the staggering number of new coronavirus cases still means that there are a lot of people seeking emergency care for coronavirus-related symptoms. On Sunday, there were 12,500 people at emergency rooms in California seeking care for a coronavirus-related concern; on the same day a year earlier, there were 11,500 visits.
The number of coronavirus-positive individuals has risen rapidly since the holidays. On Tuesday, 12,317 such patients were hospitalized statewide. That figure has more than tripled since Christmas and is the highest single-day census since early February.
One model cited by Newsom earlier this week indicated it’s plausible that the number of coronavirus-patients hospitalized in California could reach 23,000 by Feb. 2 — exceeding the pandemic record of 21,938 recorded on Jan. 6, 2021.
Those people are just one piece of the puzzle. About 52,400 Californians are currently hospitalized total, according to Dr. Mark Ghaly, the state’s health and human services secretary. That’s just below the 53,000 total hospitalizations recorded at the height of the pandemic last winter.
That likely means that hospitals will continue to face challenges in coming weeks.
“Right now, we’re laser-focused on making sure those hospitals, those staff that are weary, those staff that are tired, have the kind of support they need,” Ghaly said Wednesday. “And everything we can do as a community to make sure that capacity is there for people sick with COVID, for people in car accidents who need acute care, for people with strokes or diabetes or heart attacks, we need to do all that we can.”
Experts say it’s a necessary solution to staffing shortages, yet many workers say the policy could be dangerous.
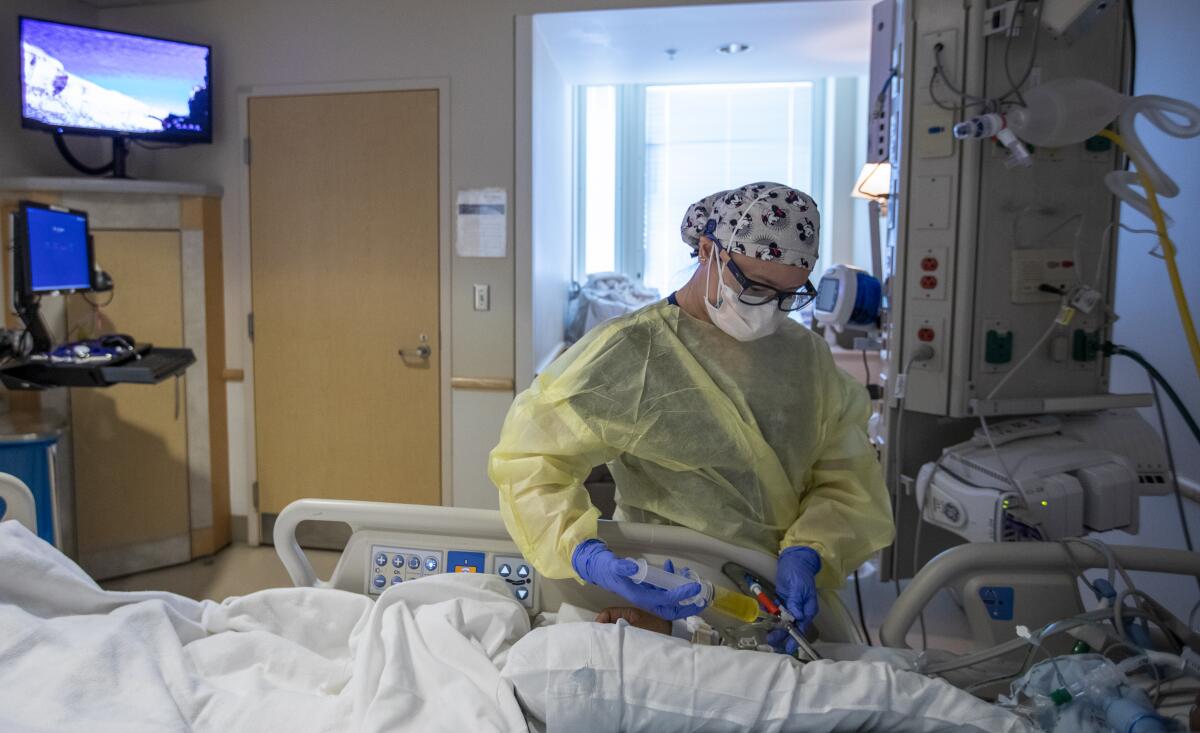
Already, L.A. County’s hospitals are straining to provide medical care, hobbled by staffing shortages far worse than last winter’s coronavirus surge.
In addition, many healthcare workers, burned out by the pandemic, have quit, and many who remain have tested positive for the virus and are at home isolating. And healthcare facilities are busier this year because there’s more demand for non-COVID care.
Among L.A. County’s four public hospitals, hundreds of coronavirus-positive health workers are in isolation, which “has made it virtually impossible to ... maintain services that are at a level of care needed to support safe patient care,” Health Services Director Dr. Christina Ghaly told the county Board of Supervisors this week.
“The numbers are due to the much higher rates of community transmission than what we have experienced at any previous point in this pandemic,” she said. “There’s just a lot more virus out there in the community. And healthcare workers, just like anybody else, are getting infected.”
The U.S. Department of Health and Human Services last week issued an alert about coronavirus testing and vaccination scams.
It’s not just nurses that are in short supply, she added. “It affects physicians, respiratory therapists, radiology techs, lab staffs — the whole gamut of what is needed to run a hospital safely.”
Ambulance companies that contract with the county to provide emergency transport through the 911 system “have experienced severe staffing shortages and are having difficulty responding to calls in a timely manner,” Ghaly said. Many employees are out sick, while other workers are not vaccinated, and “as a result, they are not able to work in line with public health orders.”
.
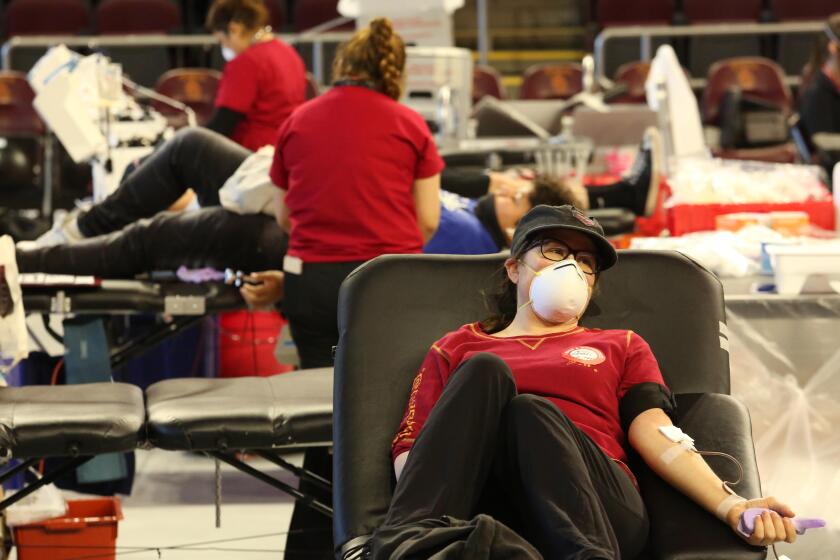
The pandemic and an unusual flu season have exacerbated the shortage, the Red Cross says, and blood donations are needed more than ever.
Omicron is now the most dominant version of the coronavirus circulating in the U.S., accounting for an estimated 98% of new cases nationwide, according to data from the CDC.
Los Angeles County health officials are urging residents to postpone nonessential gatherings and avoid some activities, especially with people who are unmasked, unvaccinated or at higher risk of severe illness.
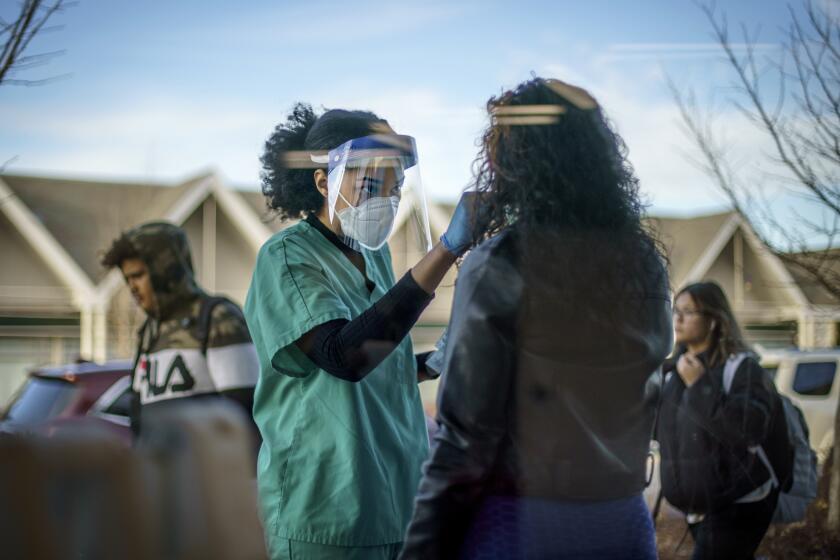
Omicron’s breakneck rise has prompted urgent calls for residents to take steps to armor themselves against transmission, including by wearing well-fitting, medical-grade masks when in crowded or indoor settings and by getting vaccinated and boosted.
L.A. County health officials are also urging residents to postpone nonessential gatherings and avoid some activities, especially those with people who are unmasked, unvaccinated or at higher risk of severe COVID-19 illness.
In Sonoma County, health officials have gone even further: enacting a 30-day ban on indoor gatherings of more than 50 people and outdoor gatherings of more than 100 people.
Scientists are seeing signals that the wave may have peaked in Britain and is about to do the same in the U.S.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.