Will another devastating variant follow Omicron? Experts debate COVID-19 future, ‘endgame’

- Share via
As coronavirus transmission rates drop across California, indicating that the surge spawned by Omicron is flattening, many are wondering whether the latest variant will be the last surge of the COVID-19 pandemic.
There remains considerable debate around that question. Some experts are loath to make forecasts, given that prior predictions of the pandemic’s conclusion haven’t proved true.
But one thing is clear: Scientists generally say it’s too early to declare an “endgame” for COVID-19.
“There are different scenarios for how the pandemic could play out and how the acute phase could end. But it’s dangerous to assume that Omicron will be the last variant or that we are in the endgame,” Tedros Adhanom Ghebreyesus, director-general of the World Health Organization, said Monday. “On the contrary, globally, the conditions are ideal for more variants to emerge.”
“It’s true that we will be living with COVID for the foreseeable future and that we will need to learn to manage it through a sustained and integrated system for acute respiratory diseases” to help prepare for future pandemics, he said. “But learning to live with COVID cannot mean that we give this virus a free ride. It cannot mean that we accept almost 50,000 deaths a week from a preventable and treatable disease.”
L.A. County reported the highest single-day tally of COVID-19 deaths since March 2021 on Thursday.
More to come?
Dr. Eric Topol, director of the Scripps Research Translational Institute in La Jolla, is among those who say we need to be prepared for more surprises after Omicron’s surge fades.
In a blog post published Saturday, Topol cautioned against thinking that the drop in Omicron cases means the 2-year-old pandemic will be over soon.
If that happens, that’s terrific, he wrote.
But “it seems quite unlikely — with so much of the world’s population, especially in low- and middle-income countries, [having] yet to be vaccinated,” Topol wrote. “Omicron’s future trajectory isn’t clear, and we cannot rule out second surges of Omicron at this point in places around the world.”
It would be foolish to predict that high infection rates of Omicron worldwide would lead to COVID-19 becoming a disease we can all be less concerned about, Topol wrote.
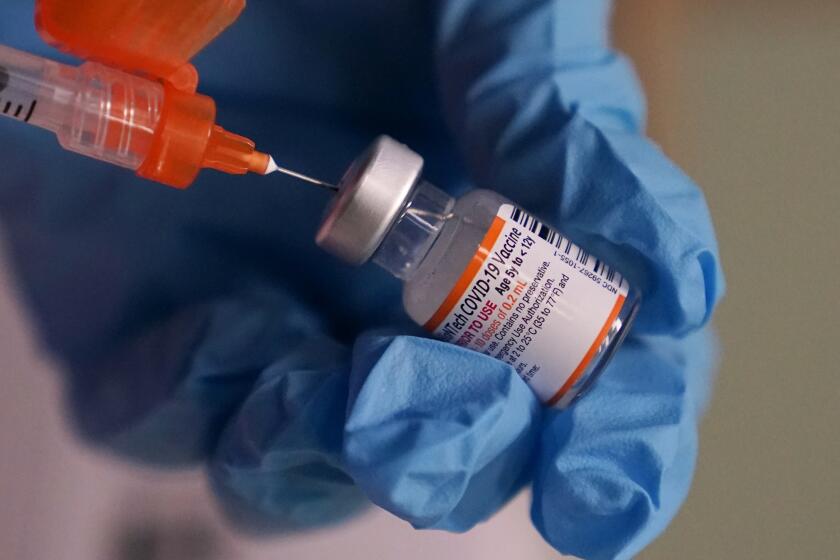
COVID-19 vaccine makers have been updating their shots to better match Omicron in case global health authorities decide the change is needed.
Growing resistance?
It’s possible that high infection rates could bring about a new variant that could be more resistant to existing immunity and vaccines. And that’s why it’s so important to make progress on a vaccine that can work on all coronaviruses; oral and nasal vaccines that can help block transmission by building immunity in our mucous; and to ramp up mass production of anti-COVID-19 pills that are probably variant-proof, Topol wrote.
“If there’s one thing we learned about predicting the path of SARS-CoV-2, it’s that it’s unpredictable. So we shouldn’t plan on a rosy picture,” Topol wrote.
Others, however, suggest the end of the pandemic is near.
From the end of November to the end of March, more than 50% of the world’s population will become infected by Omicron, Dr. Christopher Murray, director of the University of Washington’s Institute of Health Metrics and Evaluation, wrote in a commentary for the journal the Lancet.
New variants will emerge, and some might be more severe than Omicron, he wrote. Immunity will wane over time, and countries should expect that winters will be a time for increased viral transmission, he wrote.
But the effects of future coronavirus transmission on health “will be less because of broad previous exposure to the virus, regularly adapted vaccines to new antigens or variants, the advent of antivirals, and the knowledge that the vulnerable can protect themselves during future waves when needed by using high-quality masks and physical distancing,” he wrote. “COVID-19 will become another recurrent disease that health systems and societies will have to manage.”
“The era of extraordinary measures by government and societies to control SARS-CoV-2 transmission will be over,” Murray predicted. “After the Omicron wave, COVID-19 will return but the pandemic will not.”
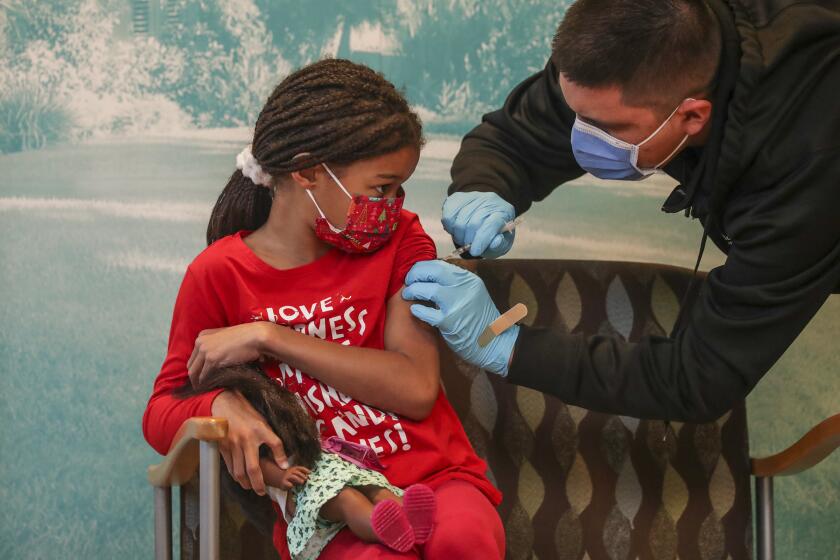
State Sen. Richard Pan (D-Sacramento) announces a bill to add COVID-19 vaccines to California’s list of required inoculations for attending K-12 schools.
More surges?
Dr. Ashish Jha, dean of Brown University’s School of Public Health, tweeted that the U.S. should be prepared for another summer surge in the South as the weather warms and people head indoors, and a surge again next winter in the North, as temperatures drop.
“Will there be another variant? I suspect yes,” Jha wrote.
Jha suggested that public health restrictions, including mask mandates, be relaxed as case numbers fall and hospital capacity improves.
“During future surges, we may need to ask people to pull back or mask up again,” Jha said. “Preserving people’s willingness to do things is critical.”
Don’t expect face mask requirements to go away any time soon, because L.A. County’s metrics are strict.
In between surges, Jha said, preparations should continue. He echoed Topol’s call for vaccines that can cover all coronaviruses or create better immunity in people’s mucous. He also advocated for a commitment by the U.S. government to buy and stockpile billions of rapid tests so there will be adequate supply for the next surge and the manufacture of a huge supply of anti-COVID-19 pills.
The positivity question
On a shorter timescale, Dr. Robert Wachter, chair of UC San Francisco’s Department of Medicine, recently tweeted the criteria he’d use to determine when to return to activities such as indoor restaurant dining.
Wachter said he’d look for a test positivity rate of 1% and a coronavirus case rate of 10 or fewer cases a day for every 100,000 residents.
L.A. County met those metrics before the Omicron surge took off in mid-December. But the county’s metrics are far worse now. According to a Times analysis of state data, L.A. County is reporting a rate of 262 daily coronavirus cases for every 100,000 residents. In comparison, the rate for San Diego County is 409; Orange County, 200; and San Francisco, 166.
And the test positive rate, although it is heading down, far exceeds 1% in many areas of California: The figure is 13.8% in L.A. County, 26.6% in San Diego County, 25.3% in Orange County and 18.3% in San Francisco.
Here are the daily coronavirus case rates, for every 100,000 residents, for other counties in Southern California, and by region elsewhere, according to a Times analysis:
- Riverside County: 268
- San Bernardino County: 237
- Ventura County: 244
- Santa Barbara County: 231
- Southern California: 271
- San Joaquin Valley: 242
- San Francisco Bay Area: 194
- Greater Sacramento: 179
- Rural Northern California: 136
The Los Angeles Unified School District, with its large testing program, offers a separate barometer of recent trends.
In baseline testing the week before school began, the rate of positive tests was 16.5%. School began after winter break on Jan. 11 and the rate for that week was 9.8%, according to data presented at Tuesday’s Board of Education meeting. For Week Two, the rate had fallen to 7.8%.
Rates in the school district are expected to be lower than in the county at large — because about 500,000 students and staff are tested every week. In the population at large, many seek tests only after the onset of symptoms or after an exposure to an infected person.
Scientists warn that Omicron’s whirlwind spread across the globe practically ensures it won’t be the last worrisome coronavirus variant.
Some experts and public health officials say there continue to be good reasons to avoid getting infected, including the potential risk of long COVID, in which symptoms of illness persist for months or longer, or passing the virus to someone who is elderly or has a weakened immune system.
It’ll take months before more is understood about a connection between Omicron and long COVID, Topol said at a recent online discussion hosted by Wachter.
There are plausible reasons in which incidence of long COVID could be worse with Omicron than earlier variants; others could argue why Omicron might be less likely to cause the syndrome, Topol said. But without adequate data, “we should plan for the worst about long COVID.”
Times staff writer Howard Blume and the Associated Press contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.