These machines to help people breathe were recalled a year ago. Many still use them

- Share via
In Rochester, N.Y., Diane Coleman has relied on a machine to help her stay alive, but she worries that it might be slowly undermining her health.
Her ventilator was among millions of breathing devices that Philips Respironics recalled last summer over safety concerns about numerous models of its ventilators, BiPAP and CPAP machines.
The reason: Polyester-based polyurethane foam used to muffle noise in those machines could degrade, giving off chemical gases and bits of black debris that could be swallowed or inhaled.
The possible risks: headaches, dizziness, nausea, irritated eyes and airways, and “toxic or cancer-causing effects,” according to federal regulators. The Food and Drug Administration put the recall in its most serious category, involving “a reasonable probability” that a product “will cause serious adverse health consequences or death.”
Yet a year later, many patients are still awaiting replacements — and some are using the recalled machines despite those possible risks.
Coleman said her machine underwent some initial repairs, but she is seeking a new one after federal regulators sought more safety testing of the replacement foam used for such fixes. The 68-year-old, who is president and chief executive of the disability rights group Not Dead Yet, has a form of muscular dystrophy and uses her ventilator roughly 22 hours each day.
She is nervous about how it could affect her, but “it’s not like I can stop using it.”
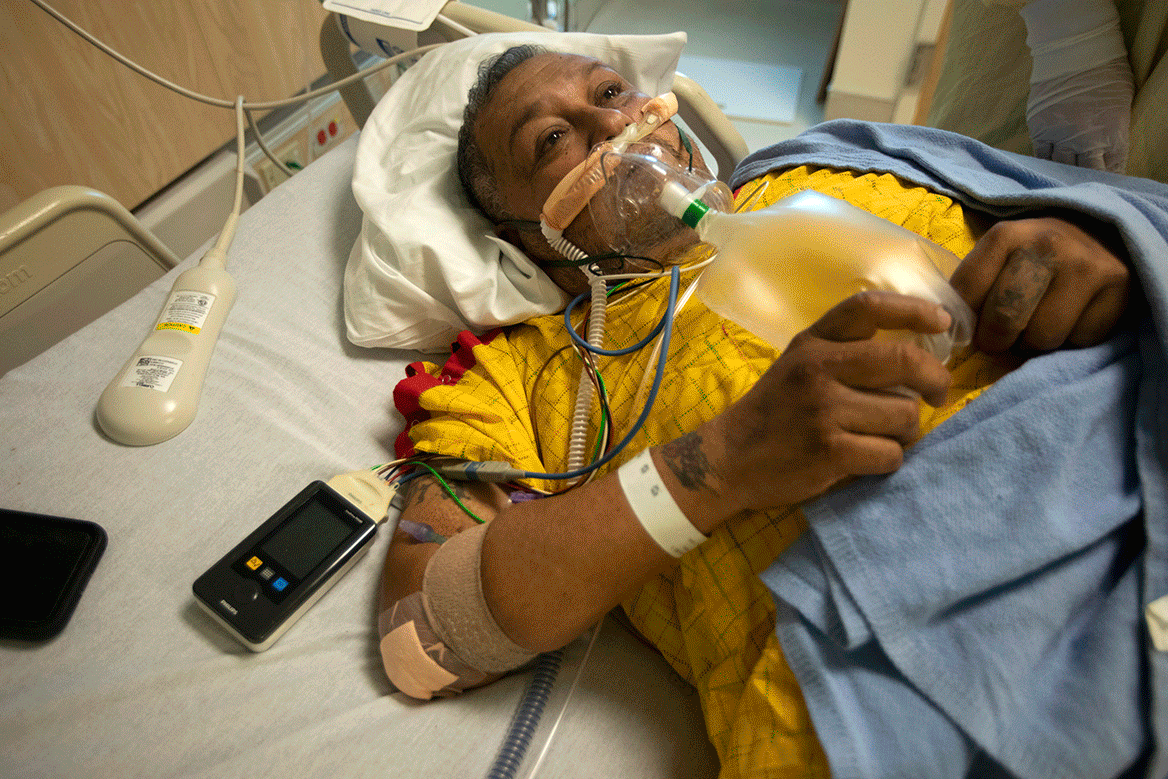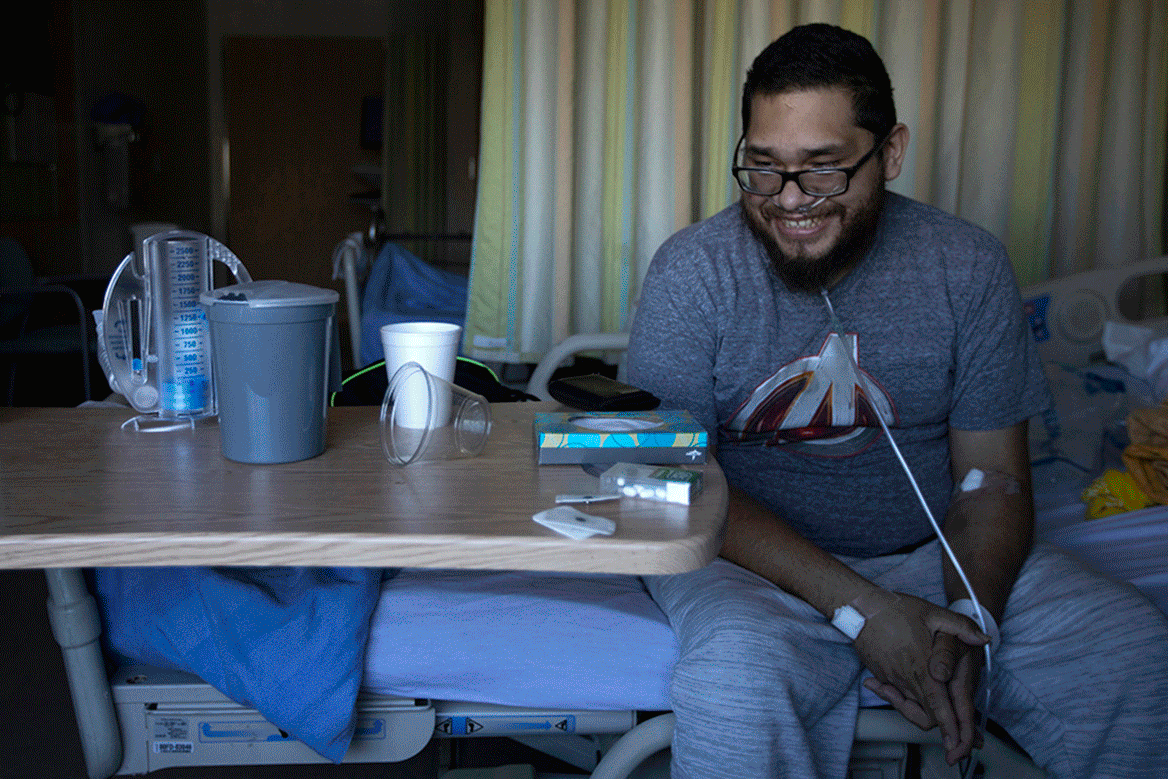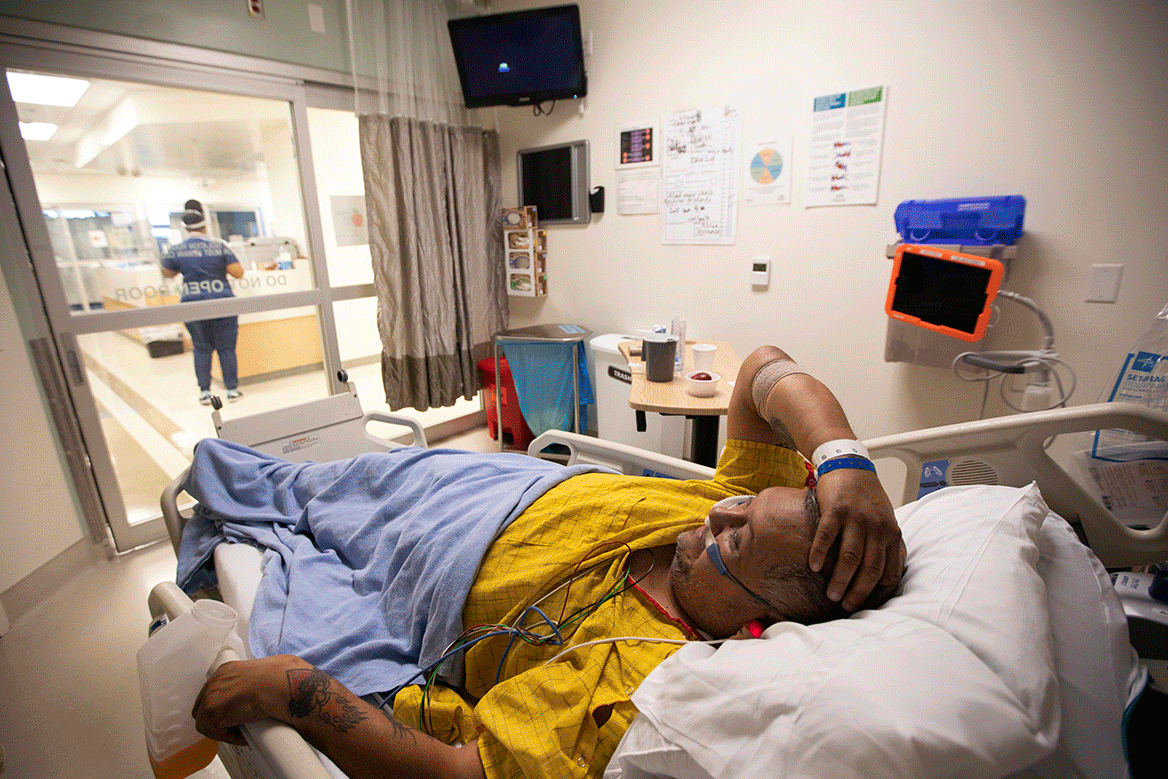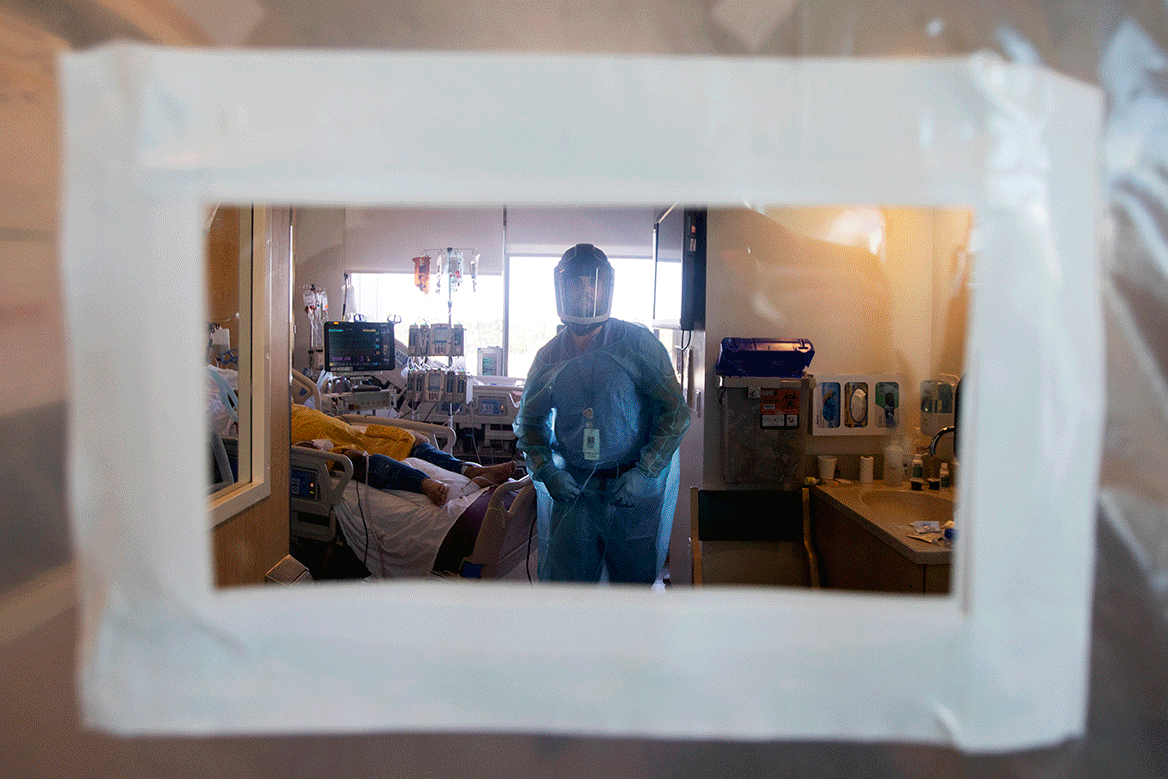
For many patients, intubation can be a last effort to stave off death. But that doesn’t mitigate how terrifying the experience can be.
Home ventilators are typically provided through an equipment vendor rather than being owned by the patient, complicating the process of changing machines. And even used ones cost thousands of dollars, online listings show. The CPAPs and BiPAPs that help people breathe while they sleep can cost more than $1,000, and insurance companies limit how often they will pay for replacements.
The vast scope of the Philips recall — which covers numerous models manufactured for more than a decade — has sent a flood of people to seek new machines at a time when supply chains are already strained.
As of this spring, Philips said that repairing and replacing devices would take until “approximately the end of 2022” for the majority of users. Philips spokesperson Steve Klink said in a statement that the recall was “a complex undertaking because of the sheer volume of devices to be remediated, and the outreach to every individual patient.” The company said it expects to replace or repair roughly 5.5 million devices globally, the bulk of which are CPAP or BiPAP machines.
“In an average year, we produce and distribute around 1 million sleep devices,” Klink said. Despite challenges with the supply chain, “we have scaled up by more than a factor of three, but inevitably it still takes time to remediate over 5 million devices. While we are working as fast as we can, we acknowledge that this has been worrying for patients.”
The danger of stopping a ventilator that sustains someone’s oxygen flow is obvious. Even switching to a different model can be precarious. Halting recalled CPAP or BiPAP machines can also be “unacceptably risky” for certain patients, physicians warned in the American Journal of Respiratory and Critical Care Medicine.
Sleep apnea, brief disruptions of breathing during the night that affect as many as 12 million Americans, increases the risk of death four- to sixfold, according to two new studies released today.
The devices are commonly used to treat sleep apnea, a disorder in which breathing is repeatedly interrupted during sleep, which can increase the risk of heart problems and leave people dangerously drowsy during the day. The FDA has advised patients who use the recalled CPAP or BiPAP machines to talk to their doctors about whether to stop.
Tom Wilson, who administers a Facebook support group for CPAP users affected by the recall, said he has read comments from group members who say they haven’t had any communication with Philips despite registering their devices with the company as much as a year ago. Some have paid out of pocket to get other devices.
“It becomes a choice between continuing to use a potentially cancer causing device or spending $1,000 or more, especially for those with severe obstructive sleep apnea,” Wilson said in an email.
In New Jersey, Chloe Berger said she stopped using her CPAP machine and suffered debilitating migraines and exhaustion. “I couldn’t maintain a job. I was just too tired,” said Berger, 30, a therapist who said she had to give up one job, then another, because she was struggling to stay awake.
Berger said she paid out of pocket for a different machine in April, roughly two months before Philips sent her a replacement. Waiting had taken an emotional and mental toll on her, she said. “You feel like you’re swimming upstream, and nothing is happening.”
The massive recall has already spurred class-action lawsuits from users across the country.
“They’ve botched the whole thing,” said Dena Young, senior counsel at Berger Montague, who said that most of the people represented by her firm had not gotten a replacement or repair. As they wait, “some of them are still using the Philips because they don’t have a choice.”
Federal investigators have also taken interest: In April, Philips said the U.S. Department of Justice had subpoenaed the company in regards to events leading to the recall.
Consumer safety advocates argue that the halting process underscores the shortcomings of the recall system, which relies heavily on private companies to inform consumers and take action.
“It isn’t actually easy for the FDA to take products off the market,” said Diana Zuckerman, president of the National Center for Health Research, a nonprofit research center that has raised concerns about the safety of medical products. “It should be a lot easier than it is.”
But the actions that the FDA has taken so far in the Philips recall also show that the agency “has more power in recalls than they usually use,” Zuckerman said.
The FDA’s Center for Devices and Radiological Health told Philips last month that it was seeking to order the company to turn in a plan that could include not only repairing and replacing the recalled devices, but also providing refunds. In a November report, an FDA investigator found that Philips had failed to start taking appropriate action years earlier when the company first became aware the foam could be breaking down. Emails showed that the company was aware of “foam degradation issues” as early as October 2015, the FDA investigator found.
Within three years, more emails indicated that Philips had gotten more complaints about crumbling foam in ventilators and said that testing had confirmed that it broke down in high heat and high humidity, but the firm “made the decision not to change the design,” according to the FDA report in November. The FDA investigator noted that dating to 2008, Philips had gotten more than 222,000 consumer complaints that included keywords such as “contaminants, particles, foam, debris, airway, particulate, airpath and black.”
Klink, the Philips spokesperson, said there had been “limited complaints” about foam breakdown in prior years that were assessed on “a case-by-case basis.” He said the 220,000 complaints mentioned by the FDA were identified through “broad word searches” and that a company review found that a much smaller number — about 3% of them — were about alleged foam degradation. The company said that when its executive committee became aware of the issue and its possible significance early last year, it took “adequate actions” that led to the voluntary recall.
This year, the FDA found that Philips’ efforts to alert patients were insufficient, concluding that many patients were probably still unaware of the health risks nine months after the recall had begun. In March, it ordered the company to notify health professionals, device distributors and users of the recalled machines after estimating that only 50% of patients and consumers who had gotten recalled CPAPs and BiPAPs within the last five years had registered with the company for a replacement.
Philips said it had some 2.6 million devices registered for the recall in the U.S. — which it said represented the “vast majority” of affected devices nationwide — but was continuing to try to increase awareness, including by working with durable medical equipment suppliers to reach out to patients.
Craig Lykens, whose 6-year-old son, Gil, uses a recalled ventilator, was dismayed recently to discover that their unit had yet not been registered for replacement. The device is provided through a medical equipment vendor, which hadn’t registered it based on the mistaken belief that Philips was not replacing machines, Lykens said.
The family, who live outside Washington, D.C., could have tried to switch to another kind of ventilator, but Lykens said that probably would involve Gil staying overnight at a hospital so doctors could monitor how he fared with a different machine — something the family was reluctant to do amid COVID-19, which is especially risky for kids with his genetic condition.
Some kids do better on certain models of ventilators, Lykens said. Fearing their child might fare poorly on the wrong one, when faced with the possible risks from foam particles, “we stay and face the long-term threat.”
In Philadelphia, Meghann Luczkowski likewise worried about what would happen if Miles, her 8-year-old son, were switched to a different ventilator. Miles has a rare form of dwarfism that causes a “floppy airway” that needs to be reopened with mechanical ventilation. He had briefly been put on a different ventilator in the past but couldn’t maintain safe levels of oxygen and suffered “blue spells” in which his skin changed color.
His Philips machine has been “his lifeline,” allowing him to live at home with his family. But Luczkowski said they had begun noticing black buildup when they changed a filter in the machine.
“It’s a very scary thing to hear that the machine that keeps your child alive could suddenly be the thing that’s harming them,” Luczkowski said.
Dr. Alon Y. Avidan, director of the UCLA Sleep Disorders Center, estimated that roughly a fifth of his patients have been affected by the recall, which has caused a significant imbalance between supply and demand “that is affecting our patients’ ability to receive treatment from CPAP in a timely and efficient manner.”
He urged patients to talk to their doctors to weigh the risks and benefits of continuing to use a recalled device. Some patients “do not have good alternatives except to stop the therapy,” he said, which “is not a good situation by any means.”
In December, Philips said that its testing of one set of CPAP and BiPAP devices included in the recall found that the level of chemical emissions “is not typically anticipated to result in long-term health consequences for patients.” That testing did not explore the health risks from ingesting bits of foam, however, nor did it look at other devices covered by the recall. The Center for Devices and Radiological Health said in May that it was not convinced that such testing was enough to downgrade the estimated harm from the tested machines.
Philips has also pointed to two analyses that did not find a higher incidence of cancer among patients who used Philips devices rather than those of other manufacturers. Another study from Sweden found signs of an increased incidence of lung cancer, but said the findings were inconclusive and might be related to regional differences in cancer risks.
Concerns have continued to mount. From April 2021 through April 2022, federal regulators have gotten more than 21,000 reports about medical issues potentially tied to the recalled devices — or malfunctions likely to cause injuries if they recurred — including 124 reports linking them to deaths. Cancer has been a stated concern: Since 2020, more than 1,100 such reports about Philips CPAP or BiPAP machines have included the words “cancer,” “tumor” or “tumour,” said Madris Kinard, chief executive of Device Events, which gathers data to track problems with medical devices.
Those medical device reports, which can be submitted by health professionals and patients as well as manufacturers, do not require verification that the device caused the injury or death; Philips stressed that submitting such reports “is not evidence that the device caused or contributed to the adverse outcome or event.”
However, Zuckerman said “it’s assumed that a lot of deaths and other serious injuries don’t get reported at all.”
In La Quinta, Matthew P. Stone counts himself as relatively lucky. The 61-year-old, who had been using a Philips CPAP machine for sleep apnea, had been able to fall back on an old device from another manufacturer.
But Stone, like others, has been galled by the way the recall has played out. At one point, Stone said, he tried to lodge a complaint with federal regulators and was referred to a Southern California number that kept cutting out before he could leave a message.
“I am so incredibly disappointed,” he said, “at the lack of advocacy by anybody involved.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.