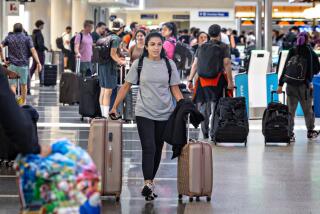California’s COVID-19 hospitalizations are near historic lows. Will the lull last?

- Share via
COVID-19 hospitalizations are close to record lows in California, an optimistic sign as the state attempts to navigate its first surge-free summer of the coronavirus era.
It’s difficult to say what the rest of the season will bring, however. The coming weeks will help determine whether some kind of uptick in coronavirus transmission is on tap, or if conditions will remain relatively calm until the autumn and winter.
The rate of new weekly COVID-19 hospitalizations in California — though near an all-time low — has been flat over the most recent two weeks for which data are available.
Nationally, weekly declines are starting to level off, too, with hospitalizations on the rise in some parts of the country.
Throughout the pandemic, hospitalization numbers have proved a useful, if lagging, indicator of coronavirus spread. A significant or sustained jump in patient counts would probably mean the coronavirus is circulating more widely in a community.
There are hopeful signs in Los Angeles County that this summer will not be the harbinger of an increase in coronavirus cases, as has happened in each of the last three years.
Dr. Peter Chin-Hong, a UC San Francisco infectious-disease expert, said he suspects that signs of an increase in coronavirus transmission are probably real in some locations, although “it’s not at a high level yet. And we don’t really know how high it will go.”
“Maybe it’s just an up-and-down thing,” he said in an interview. “But it’s just a symbol that it’s something we can’t just forget about.”
Regions to watch nationally include the South and Pacific Northwest. In the Southeast, the rate of weekly new COVID-19 hospital admissions hit a record low in June but has since climbed 12%. In the central South — the states of Texas, Louisiana, Oklahoma, Arkansas and New Mexico — the rate has risen by 7% from its all-time low in recent weeks. In the Northwest, it’s up 10%.
Despite those increases, hospitalization rates remain very low. In fact, 6,220 new hospitalizations were recorded nationally for the week that ended July 1, the most recent period available. That’s a record low, and a 0.8% decrease from the previous week.
The national record high of new weekly COVID-19 hospitalizations was 150,674 for the week ending Jan. 15, 2022, during the first Omicron wave.
In California, there were 1,181 new hospitalizations for the most current week available — low, but not quite to the all-time record of 870 recorded during the week ending April 16, 2022. The record high, seen the week ending Jan. 9, 2021, was 16,663.
Experts don’t expect anywhere near the sort of spikes observed earlier in the pandemic.
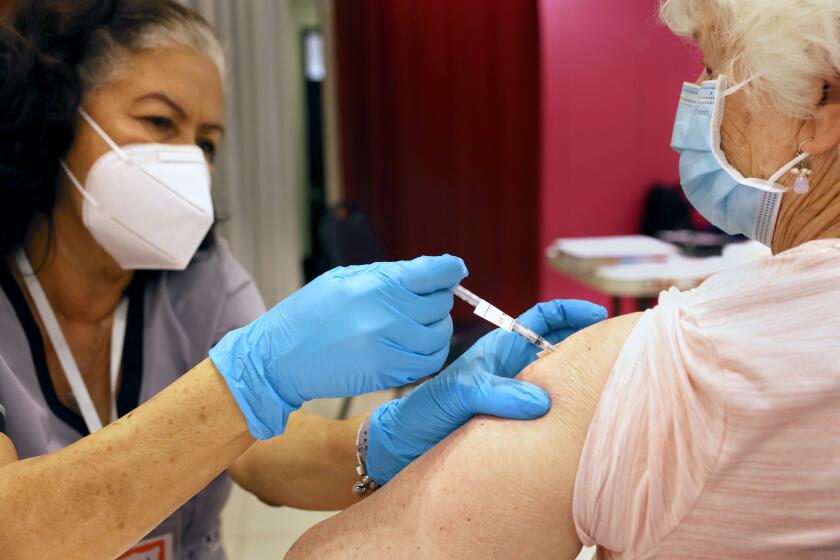
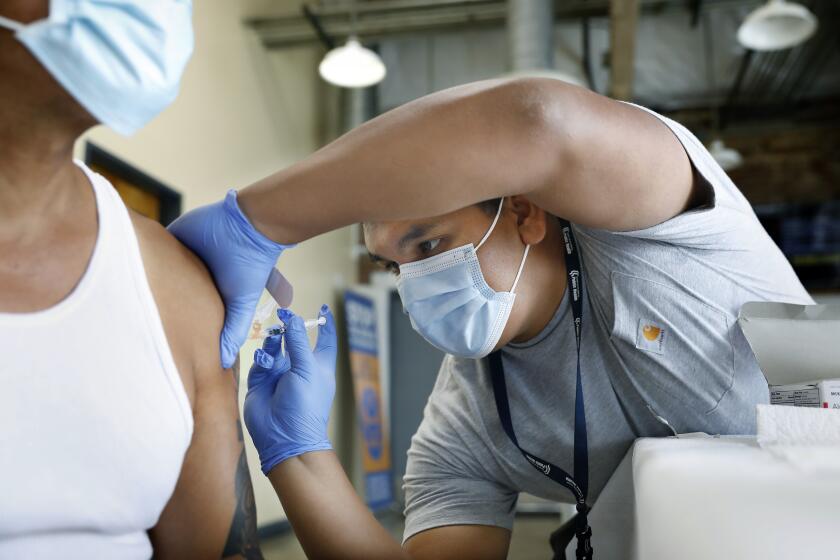
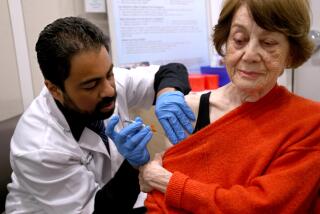
But they note it’s important for people, especially those who are older or otherwise at high risk of falling seriously ill, to have a COVID-preparedness plan and for everyone to stay up to date on their vaccinations.
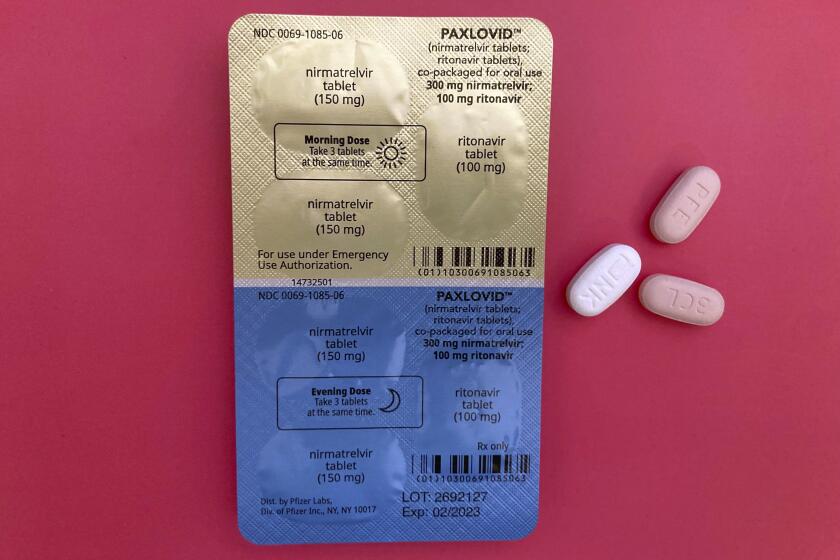
“You won’t see a huge flood into the hospitals of people [with COVID], but you would probably see an increase,” Chin-Hong said. “But it could be quietened if they can stay away from the hospital by taking early therapy, like Paxlovid.”
A pandemic allows the Food and Drug Administration to authorize vaccines and drugs for emergency use, even after the health emergency ends.
Everyone age 6 years and older should get one updated Pfizer-BioNTech or Moderna COVID-19 vaccination, officials say. The most recent updated shot became available last September.
Doctors say it also remains wise to take sensible measures to ward off infection, such as avoiding sick people and getting tested if you have COVID symptoms. Keeping a mask handy so you can wear it if needed — like if you’re unlucky enough to sit on a plane next to coughing people spraying droplets in your face — would also be a good idea.
It’s become increasingly difficult to monitor COVID trends in the post-emergency era, as many jurisdictions have either cut back or eliminated contemporary reporting of cases or other metrics.
There have been anecdotal reports of notable COVID outbreaks, including one on a cruise ship that recently docked in San Francisco, as well as one that affected a Bay Area television station, Chin-Hong said.
But it’s unclear whether those point to any kind of larger trend.
Santa Clara County, the Bay Area’s most populous, reports that coronavirus levels in wastewater are at a “medium” level in recent weeks and have stayed relatively stable over the last month.
The CDC has ended routine reporting of coronavirus case and death counts. Here’s how to figure out how to assess COVID conditions in your area.
The coronavirus test positivity rate in California over the most recent seven-day period available is 6.5%, up from 4.6% a week earlier. However, it’s possible that increase is partly affected by hospitals testing only those suspected of having a coronavirus infection, rather than every single patient.
Now that Paxlovid, an anti-COVID oral drug that can be taken after infection, has been approved by the U.S. Food and Drug Administration, higher-risk people can talk to their healthcare providers about getting Paxlovid in advance of, say, an overseas trip if they think it’ll be hard to obtain the drug later, Chin-Hong said. That would enable people to take the pills quickly should they test positive for the coronavirus.
Given the situation, Chin-Hong said he wouldn’t advise his elderly mother to go on a cruise ship unless she’s armed with a pack of Paxlovid.
It can be helpful to have the Paxlovid conversation in advance of becoming sick with COVID-19, Chin-Hong said. That way, patients can talk with their regular healthcare providers about the possibility of interactions with other drugs they are taking. Clearing the use of Paxlovid will also help the patient get access to the drug sooner rather than later.
Without that pre-clearance, it’s possible healthcare providers unfamiliar with a patient’s medical history could rule out a Paxlovid prescription based on a mild drug interaction that isn’t clinically relevant, Chin-Hong said.
It can be challenging to determine whether mental health illness is the result of long COVID, but “treating symptoms is vital to recovery,” said an advisory by the Substance Abuse and Mental Health Services Administration.
The FDA says Paxlovid significantly reduces the percentage of people with COVID-related hospitalization or death from any cause. In one study of 977 patients who received Paxlovid and 989 who received only a placebo, fewer than 1% of patients who got Paxlovid were hospitalized with COVID-19 or died from any cause, compared with 6.5% of people who got the placebo.
With many people vaccinated or having previously survived a coronavirus infection, COVID-19 poses less of a threat than it once did. People need not panic if there is a rise in infections, Chin-Hong said, “because we have the tools. It’s just that you need to be aware of the tools.”
Still, infection can still lead to significant consequences, especially for older people.
Dr. Robert Wachter, chair of UC San Francisco’s Department of Medicine, recently came down with COVID-19 for the first time and fainted while taking a shower.
U.S. intelligence agencies weren’t able to determine whether researchers in Wuhan, China, who fell sick in the fall of 2019 had COVID-19, according to a declassified report.
In a recent Twitter thread, Wachter said taking a hot shower while dehydrated and having COVID symptoms “can cause your blood vessels to dilate, leading to a dangerous drop in blood pressure.”
He lost consciousness and woke up in a pool of blood, apparently after falling to the floor and hitting his head on the lid of a bathroom trash can. He said he suffered “a small subdural hematoma, a little rim of bleeding in the space around the brain,” and a cervical fracture.
Wachter said he doesn’t know how he became infected. He hasn’t treated COVID patients and wears a KN95 mask in clinical areas. However, he has taken off his mask for meetings in non-crowded rooms and has been dining and socializing indoors.
Given his experience, “COVID continues to be worth avoiding if you can,” Wachter wrote.
The CDC now estimates XBB sublineages comprise nearly 99% of circulating coronavirus in the U.S., displacing the BA.5 subvariant that dominated the nation for much of last year.
In Los Angeles County, COVID-19 hospitalization levels have fallen to a record low. And the concentration of coronavirus in local wastewater is just 8% of last winter’s peak, according to the county Department of Public Health.
“Although transmission is still occurring, there is low concern for rapid spread of the virus at this time,” the agency said in a statement this week.
Weekly COVID-19 deaths remain relatively low, with 13 reported for the week that ended Tuesday — down from 29 the previous week.
“The L.A. County metrics are reassuring, especially when compared to the last three summers when we experienced increases in transmission and hospitalizations in July,” Public Health Director Barbara Ferrer said in a statement. “This may reflect, in part, the effectiveness of our tools against the Omicron strains currently circulating. Vaccines, tests and therapeutics continue to provide powerful protection against COVID-19.”
Coronavirus infections have been found in at least 32 animal species in 39 countries. Some can transmit the virus to humans.
Californians who don’t have insurance or are having a hard time getting a prescription for anti-COVID medication can make a free phone or video appointment through the state’s COVID-19 telehealth service, reachable through sesamecare.com/covidca or by calling (833) 686-5051.
L.A. County has similar free telehealth services, which are accessible at (833) 540-0473. Free at-home COVID tests also can still be picked up at county libraries and vaccination sites operated by the county Department of Public Health, as well as at many food banks and senior centers.
Most insurance plans in California are still required under state law to reimburse insured people for the cost of eight at-home COVID tests for every covered person monthly.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.