Are homeless shelters ‘a nasty experiment’ during coronavirus? L.A. says no and opens more

- Share via
It started in late March with a driver at Union Rescue Mission. He complained of flu-like symptoms and was brought to a hospital, where he eventually died of COVID-19, sending one of skid row’s largest shelters into high alert.
As of Friday, 79 homeless residents and four staff members have tested positive for the coronavirus, said the Rev. Andy Bales, the mission’s chief executive officer. He has to move people around like puzzle pieces to set up isolation and quarantine rooms inside the massive, five-story building, Bales said. Some are now living in a boardroom and a staff kitchen, while nearly 200 others have been sent to temporary housing elsewhere.
The outbreak is what critics of Mayor Eric Garcetti’s plan to convert dozens of city recreation centers into homeless shelters have feared — and what other cities have already experienced.
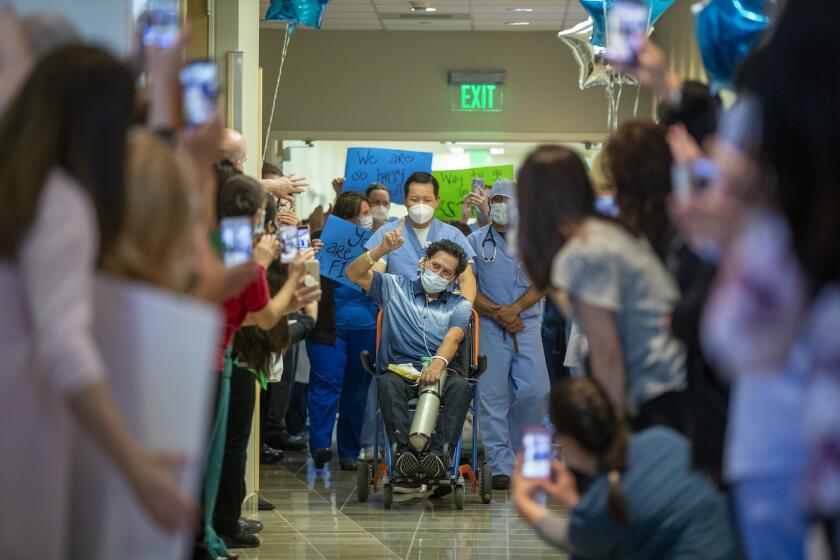
These are some of the unusual new scenes across the Southland during the coronavirus outbreak.
Across the country, large congregant shelters have struggled to contain spikes in coronavirus cases. In San Francisco, about 100 homeless people and 10 staffers tested positive at that city’s largest shelter. In Boston earlier this month, researchers tested 408 people at a shelter and 147 of them tested positive for the virus — although the majority were asymptomatic.
As a result, there is a growing concern in many cities about the use of congregant shelters during the pandemic. Many shelters across the country also have stopped accepting new homeless clients.
Still, officials in Los Angeles remain convinced that homeless people are safer in shelters than on the streets because it’s easier for outreach workers and medical professionals to provide care. And so the city is moving forward with plans to open more congregant shelters.
So far, 20 are up and running out of the 42 that Mayor Eric Garcetti originally announced. The city is set to open four more in the coming days, he said, bringing the total to about 1,000 beds — far less than the initial goal of 6,000 beds.

On Monday, Garcetti said that the shelters, each of which holds far fewer homeless people than Union Rescue Mission, are 97% full.
“It is working exactly how we hoped it would,” he said. “And I’ve always said too that doesn’t mean that we will never have cases, but we haven’t yet had large-scale outbreaks.”
The Los Angeles County Department of Public Health is in charge of conducting investigations at shelters run by the city and an assortment of nonprofits.
It is currently examining eight, though Director Barbara Ferrer did not specify which ones. Neither did she cite the number of coronavirus cases investigators have found at each shelter,
Earlier this week, Ferrer characterized it as “a very small number, with the exception of what we’ve seen at the Union Rescue Mission. And that’s really because, at the Union Rescue Mission, we did test everybody who was there.”
In general, testing on skid row has increased since the opening of a pop-up facility on Monday. The county still lacks the capacity to test everyone in homeless shelters, but Ferrer said that may change soon.
“It just makes sense now that we’re able to do more testing both of symptomatic people and asymptomatic people who are very high-risk and live in these congregate living situations,” she said.
At 76, Judge David Carter knows he shouldn’t be on skid row exposing himself to the coronavirus. But he wants more for L.A.’s homeless people.
Advocates and even some public health experts say large congregant shelters are powder kegs waiting to explode.
“I had a vivid nightmare of this happening,” said Chris Herring, a sociology doctoral candidate at UC Berkeley who is assisting the San Francisco Coalition on Homelessness. “Now that we’re learning more and how it keeps going worse, it just sounds like a nasty experiment that we’re doing with a group of people that we wouldn’t do ever with another group of people.”
In doing his research, Herring stayed for weeks in the San Francisco shelter, known as Multi-Service Center or MSC South, where the outbreak occurred. He described how it housed about 350 people per night and that more than 200 would sleep in bunk beds, scarcely two feet apart with no partitions. There was one hall for bathrooms.
“It’s incredibly difficult to sleep there, because you’re hearing all your neighbors sleeping, all piled up on top of you,” he said.
Dr. Allen Cooper, an emeritus professor in medicine at Stanford University, had been volunteering at MSC South, and said government officials should’ve known that the place was ripe for disaster. In January, he watched an outbreak of norovirus spread there, leaving dozens thinking they had stomach flu. In one day, he said he saw about 15 people get sick — a clear indication of how fast the highly contagious coronavirus could spread.
At a time when the world isn’t in the midst of a pandemic, Cooper said he recognizes that such shelters are an imperfect but necessary solution to homelessness. But not right now.
“This is a cruise ship without walls between the bedrooms. This is an aircraft carrier,” he said, referring to locations of coronavirus outbreaks. “In a nursing home, at least people are in their own rooms. Big shelters like this for outbreaks are probably the worst thing.”
Last week, public officials told the San Francisco Chronicle that none of the people at MSC South showed serious symptoms of COVID-19 when they were tested. The shelter closed weeks ago after the outbreak, but recently reopened to accept people recovering from the disease.
John Maceri, executive director of The People Concern, said not all sites are like MSC South or Union Rescue Mission. His organization manages a network of smaller shelters across L.A. County that have drywall separating sleeping spaces into what resemble cubicles. It’s not completely enclosed, but it’s easier to self-isolate there than in a room with bunk beds, he said.
The number of homeless people living in The People Concern’s shelters has been reduced in recent weeks, moving the oldest and most medically fragile into hotels and motels. The biggest remaining risk in the shelters, he said, is probably the shared bathrooms.
“I think it’s highly unlikely that we will get through the current situation without having some of our residents who test positive and who may even get sick,” Maceri said. “I am reasonably confident that we are not going to have a massive outbreak.”
Garcetti on Friday said he has followed Ferrer’s guidance in rolling out his plan to use recreation centers to get homeless people off the streets.
Even though the shelters have no barriers between cots, he said the spacing of six feet and health screenings have, so far, been effective in the month since the initial eight opened. The coronavirus has been detected at only two of the city’s 20 shelters, but there have been no reports of the virus spreading from one resident to another.
After a homeless man staying at the Granada Hills Recreation Center tested positive this month, about 14 people who had been near him and those who arrived with him were tested, said Ken Craft, chairman and CEO of Hope of the Valley, a nonprofit that operates four of the city shelters in the West San Fernando Valley.
The man, who has not been named, was transported to Holy Cross Hospital, where his condition improved, Craft said. No other cases have been detected.
County public health officials are testing anyone with symptoms, Craft said. Staff also are provided masks, gloves and body suits.
“We provide masks for all clients to wear at all times,” he said. “We only allow two people per six-foot table to maintain social distancing.”
To make such social distancing possible, the initial plan for 110 beds in the Granada Hills shelter was scaled back to 38 — a readjustment that has happened at a similar scale at all city recreation centers, causing Garcetti to revise his initial promise for 6,000 beds.
The recreation center shelters are part of a loosely integrated system of homeless housing and services that have been designed to achieve two goals during the pandemic: getting the most vulnerable people off the streets and relieving existing, dormitory-style shelters that cannot meet the spacing requirements to slow the spread of the virus.
Coronavirus: L.A. launches new effort to move 15,000 people out of overcrowded shelters and encampments and into hotel rooms.
For example, Craft said Hope of the Valley moved homeless residents into the four recreation centers it operates, reducing its 138-bed shelter in Pacoima to only 52 beds.
Los Angeles County and the Los Angeles Homeless Services Authority also are working to secure safer lodging in hotels for homeless people who are elderly or have health conditions that put them at higher risk for COVID-19. That effort is progressing slowly, however. At the current pace, the county’s goal of securing hotel rooms for 15,000 people will not be reached until summer.
For Union Rescue Mission, Bales says changes are coming more immediately. The shelter, which typically has a population of about 1,000, is now down to fewer than 500. It also has stopped taking in new homeless residents for the time being.
The second floor, where more than 200 men slept on bunk beds in a single room, will never be the same, he said.
“From now on it will be 80 single beds,” Bales said. “That’s how drastically the COVID-19 has reshaped our world and likely reshaped it permanently.”
But Bales said he had no regrets about housing so many people.
“I think the benefits outweigh the risks, especially if they’re able to keep the six-foot distance, if they have more than a couple restrooms, especially if their guests are capable of hearing us cry out and wear their masks and taking precautions,” he said. “We just don’t believe in leaving people on the streets.”
Times staff writer Melanie Mason contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.