Long waits outside L.A. County psychiatric units stall patients, police
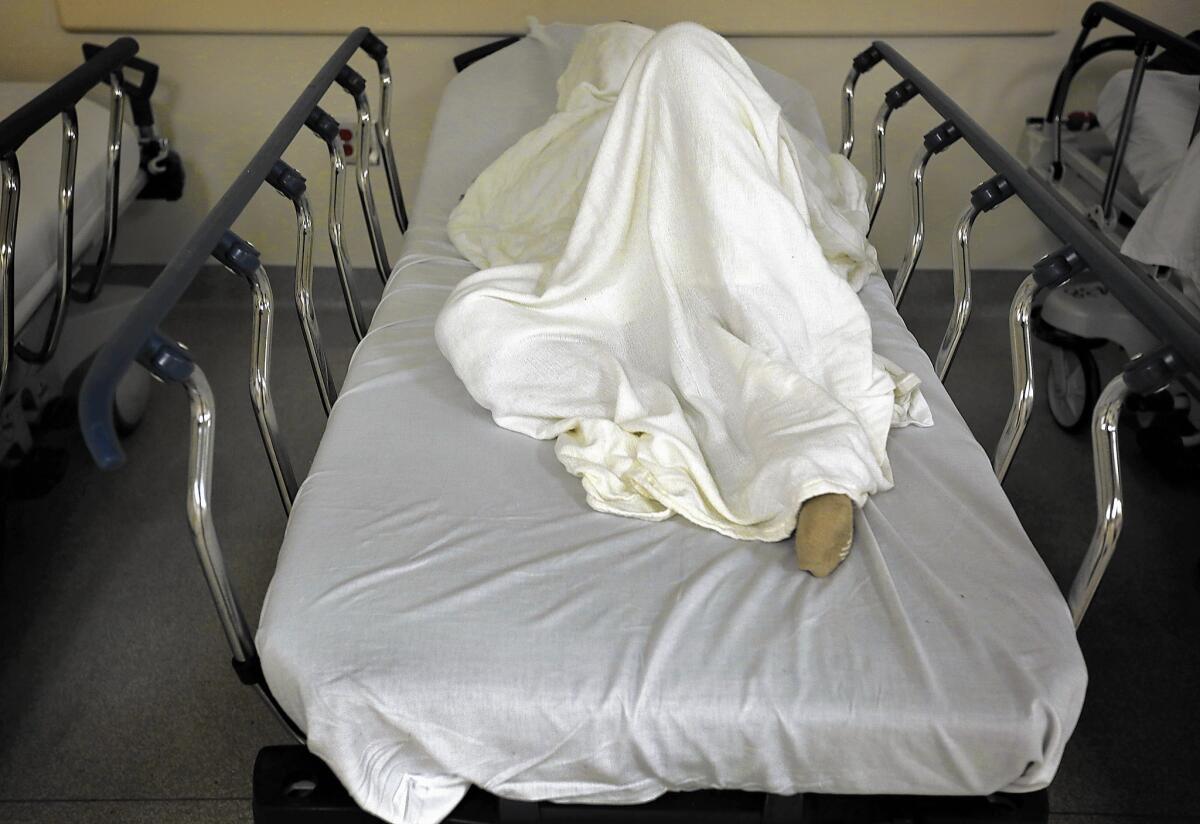
A patient at L.A. County-USC Medical Center is in the psychiatric unit on a 5150 hold, a mandatory 72-hour evaluation period for those deemed to be dangerous to themselves or others. Some of these patients face hours-long waits to be admitted.
- Share via
When Los Angeles police Det. Jim Hoffman arrived at the L.A. County-USC Medical Center’s psychiatric emergency department on a Saturday morning in March, he found a small crowd waiting.
Two police officers from the LAPD’s Central Division were sitting in a narrow hallway outside the locked psychiatric unit with a man and woman in handcuffs. Both patients had been brought to the hospital overnight on so-called 5150 holds, a forced 72-hour detention for mental evaluation of those deemed to be a threat to themselves or others.
But the ward was full. The man — and a rotating series of cops with him — had been waiting for 11 hours for a bed to open up. The woman had been there for more than eight hours.
The male patient was “psychotic, but in a calm way,” sitting quietly on a bench, Hoffman recalled. He had just finished a fast-food meal that one of the officers had bought across the street. The woman appeared to be asleep on the floor with her hands free and her ankle shackled to the bench. She woke up and became agitated, swearing at the officers, who took her outside and in again, in an attempt to calm her down.
“Quite frankly, I empathized with her,” said Hoffman, a supervisor with the LAPD’s special mental health team. “At that point, I probably would have been cursing too.”
Despite Hoffman’s efforts, which included calling the head of the psychiatric emergency unit on his cellphone, it took another hour for the man to be taken into the unit. The woman waited another two hours.
Los Angeles Police Department officers transported 15 psychiatric patients to county-run hospitals that day and spent more than 64 hours waiting to hand those patients off to hospital staff, department records show.
It was an unusually bad day. But officials agree it illustrated a common problem.
Increasingly overburdened psychiatric emergency units are taking patrol officers and firefighters off the streets as they get caught in backups outside facility doors. At L.A. County-USC, the average psychiatric patient count per day has increased by 60% over the last three years.
The patient load has grown, some police and hospital officials said, partly because of recent state and local policy changes intended to shift nonviolent offenders — including many who are mentally ill — out of prisons and jails. So far, local mental health treatment services haven’t been able to catch up with the increased need for community treatment programs and psychiatric beds.
Hoping to make a point about the problem, the LAPD has enlisted the help of the city attorney’s office to put pressure on hospitals and county officials, and has started asking officers to log their wait times at county psychiatric emergency departments. From March through May the average wait was two hours, according to data the department provided in response to a Times request.
“It’s costing us thousands and thousands of dollars in overtime and lost work hours because officers are just sitting at a hospital,” said Lionel Garcia, who recently retired as lead lieutenant of the LAPD’s mental health unit.
During the extended waits, patients’ mental state often deteriorates, police say.
“You’re trying not to get assaulted, and you’re trying to tell the staff, ‘Hurry up, this is inhumane,’” Hoffman said.
At L.A. County’s three public hospitals with emergency psychiatric departments — L.A. County-USC, Harbor-UCLA and Olive View-UCLA — there are about 60 psychiatric beds in total. L.A. County-USC is the busiest of the three units, treating a steady stream of cases: people threatening suicide or harm to family members; others found wandering aimlessly, sometimes naked or bleeding, down the middle of a busy street.
Hospital workers triage patients as they arrive, giving priority to those whose symptoms are most severe and those who arrive with law enforcement.
When the 20 beds in the psychiatric unit are full, some patients are taken to the regular medical emergency department, where they are often kept in restraints because the area is not locked. Others remain in the waiting areas, frequently strapped to gurneys or handcuffed, until they can be taken into the two-room emergency psychiatric unit. Hospital staff won’t administer medication until patients are inside the secure psychiatric ward.
Some patients come in under the influence of drugs or alcohol and can be released from the ward within hours, once they sober up. Others require longer treatment and may be transferred to a private mental health facility if and when a bed can be found.
Each morning, the hospitals take a count of psychiatric patients in the system, including in psychiatric emergency departments and the overflow in regular emergency rooms. The trend has moved upward for three years. In 2012, the average count at L.A. County-USC was 19 patients. So far in 2015, the average is 31. On March 14, the day of the LAPD officers’ marathon waits, the morning count was 46 patients.
“Law enforcement is trapped in the middle of this very difficult, complicated societal conundrum, but our providers are as well,” said Brad Spellberg, chief medical officer of L.A. County-USC. The hospital’s psychiatric ward once took in as many as 24 patients at a time, with beds squeezed in. But since January, following a surge in assaults on staff and patients inside the unit, the number of beds was reduced to 20 to ease crowding.
Police and patients aren’t the only ones left waiting. Paramedics who transport 5150 patients, and family members or friends who drive loved ones to hospitals for voluntarily psychiatric care, often wait as long or longer than police officers for beds to become available, although those times are not systematically tracked.
Judy Nahman-Stouffer, whose 26-year-old son was diagnosed with paranoid schizophrenia, said she drove him to Harbor-UCLA Medical Center in February because he was hearing voices. They waited for four hours before her son was taken into the locked psychiatric unit, at 3 a.m. Other patients who came in with police were seen more quickly, Nahman-Stouffer said. Hospital staff explained that the officers had to get back to their duties.
“That seemed reasonable to me,” she said.
Her son, Erik, recalled being anxious during the wait and was relieved once he was inside the psychiatric ward. “They took care of me,” he said of the county hospital workers. “It’s a place where I could rest and I didn’t have any responsibilities. I could just focus on getting better.”
In some cases, police can drop patients at one of four county-funded psychiatric urgent-care centers instead of waiting at a hospital. Those centers, with a total of 60 beds, take patients who are not violent or in need of medical care. But they can legally keep them for only 23 hours at most.
Since last July, the centers have logged more than 17,000 visits. An additional five centers are expected to open in the next year, which would double the capacity for such treatment. That’s likely to reduce waits at county hospitals, but probably won’t eliminate the backups, officials said.
County officials also are trying to relieve the pressure on the government-run psychiatric system by seeking increased rates of reimbursement from the state Medi-Cal program for private hospitals that take in patients discharged from county wards.
County mental health Director Marvin Southard said he hopes greater financial incentives will help, but he stressed it will take time to get state and federal government approvals.
“If the genie popped out of the bottle, you would have more facilities across the continuum,” L.A. County-USC’s Spellberg said. “But we don’t have a bottle and we don’t have a genie, so there isn’t a simple fix.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.











