Your iPhone could save your life

- Share via
There’s no doubt smartphones have changed the way we interact -- for better and for worse. Despite the advantages, like the quick and easy ability to keep in touch with people throughout the day, chronic text messaging has also driven us apart and bred an impersonal culture.
When we’re not ignoring the person we’re with because we’re getting texts, tweets, emails and updates from someone else, we’re fooling ourselves into thinking that smartphones can give us carte blanche to weasel out of our commitments or treat people like they’re as disposable as avatars. (If you have no idea what I’m talking about, I envy you. But also, may I also recommend reading this horrifying dating story -- “The End of Courtship?” -- by the New York Times’ Alex Williams.)
Some days I want to chuck my phone into the Pacific Ocean and go back to the simpler days of Nokia flip phones. But then I come across smartphone innovations that make me wonder how we ever lived without them.
Thursday’s episode of the NBC News program “Rock Center” pointed me to one such development that not only has the potential to change the future of healthcare, but could also transform one of our most important relationships -- the ones with our doctors -- into more personal connections. The results could save patients’ money and their lives.
“Why do we have people being treated like cattle herds?” asked Dr. Eric Topol, described by “Rock Center” correspondent Dr. Nancy Snyderman as “one of the world’s foremost cardiologists.” Instead of dumbing down medicine and treating everyone the same, Topol said, doctors should appreciate that “each of us are truly unique in every way.”
His cure for the medical profession? Modified smartphone devices and apps.
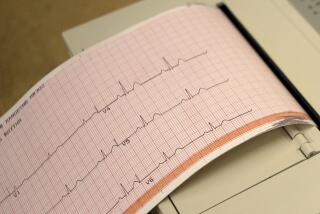
On the program Topol showed viewers how he modified a smartphone to allow him to administer cardiogram tests, saving his patients $100 in technician fees. “The device,” said the reporter, “was approved by the FDA in December and is now sold to physicians for $199.” (See the video below.)
“These days I’m actually prescribing a lot more apps than I am medications,” Topol said. “You can take the phone and make it a lab on a chip. You can do blood tests, saliva tests, urine tests, all kinds of things. Sweat tests through your phone. This is a powerful device.”
Preventive medicine of the future not only puts more power and knowledge in the hands of patients; it also will allow them to keep in touch with their doctors in real time. What’s more personal than that?
Topol is not alone. At the Consumer Electronics Show earlier this month, my colleague Jon Healey noted that the “tech industry is pouring money into medical devices.”
“The approach enables providers to detect and respond to signs of trouble at an early, less serious stage,” he wrote. “That makes for more efficient treatment.”
So why haven’t all doctor’s offices gone digital yet? In a word, money. As Healey explains: “If you’re paid a fee for each service you provide in your office, why would you invest in technologies and procedures that led to fewer billable services?”
But it doesn’t have to be this way. Instead of inflated medical charges and the reckless practice of throwing around “funny money,” doctors should be rewarded for their preventive, and cost-saving measures.
“What’s needed is a different reimbursement model, one that rewards providers who manage chronic diseases so well that their patients require fewer office visits, treatments and hospitalizations” argues Healey.
And the sooner we get that, the sooner we can all have doctors who are just a touch screen away.
ALSO:
You go, military girls -- to the front lines
Want to fight terrorism? Educate women
Follow Alexandra Le Tellier on Twitter @alexletellier
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.