Letters to the Editor: This is why blaming doctors is pointless: America has no healthcare system
- Share via
To the editor: Dr. Robert Pearl asserts that “doctor culture,” taught and learned in medical schools, is destroying the U.S. healthcare system. I disagree. America has no healthcare system. We have a healthcare industry that supports profit-making healthcare enterprises, regardless of whether or not they serve the public interest.
We have a non-system that allows poor and minority Americans to suffer disproportionate morbidity and mortality. Maldistribution of wealth and education have made our ZIP Codes accurate predictors of health and longevity. We have allowed poor and minority areas to become permanently polluted with lead, other toxic metals, hydrocarbons and diesel particulates.
Our insurance companies take the premiums as profit and avoid their fiduciary duty to pay for the services rendered. Our pharmaceutical industry has gouged the American public while creating an opioid epidemic. Healthcare industry executives have garnered exorbitant compensation while shortchanging patients and those providing the care.
We have spent decades debating whether healthcare is a right or a privilege, while never acknowledging that healthcare is a universal necessity. Our healthcare problems do not begin or end with doctors, nurses or any individual group. They begin where we deny that healthcare is a common good.
Brian Johnston, M.D., Los Angeles
..
To the editor: As a registered nurse and healthcare advocate with more than 40 years of experience in a variety of healthcare settings, I am concerned by Pearl’s comments.
He stresses supporting the primary care physician role over that of the specialist. While his conclusions have merit, he apparently overlooked the important role that nurse practitioners and physician assistants can play in the care of chronic conditions. These healthcare professionals can and do play an integral role in healthcare, and often the biggest roadblock to the expansion of their role in healthcare all too often are the physician groups and associations.
What surprised me most was Pearl’s failure to mention the Beyond Flexner Alliance. This group of committed physicians and other healthcare professionals is working to redefine medical training, and its stated goals are in many ways the same as those Pearl put forth in his op-ed article.
Perhaps Pearl should consider getting involved in this alliance.
Geneviève M. Clavreul, Pasadena
..
To the editor: I found Pearl’s piece remarkably tone deaf.
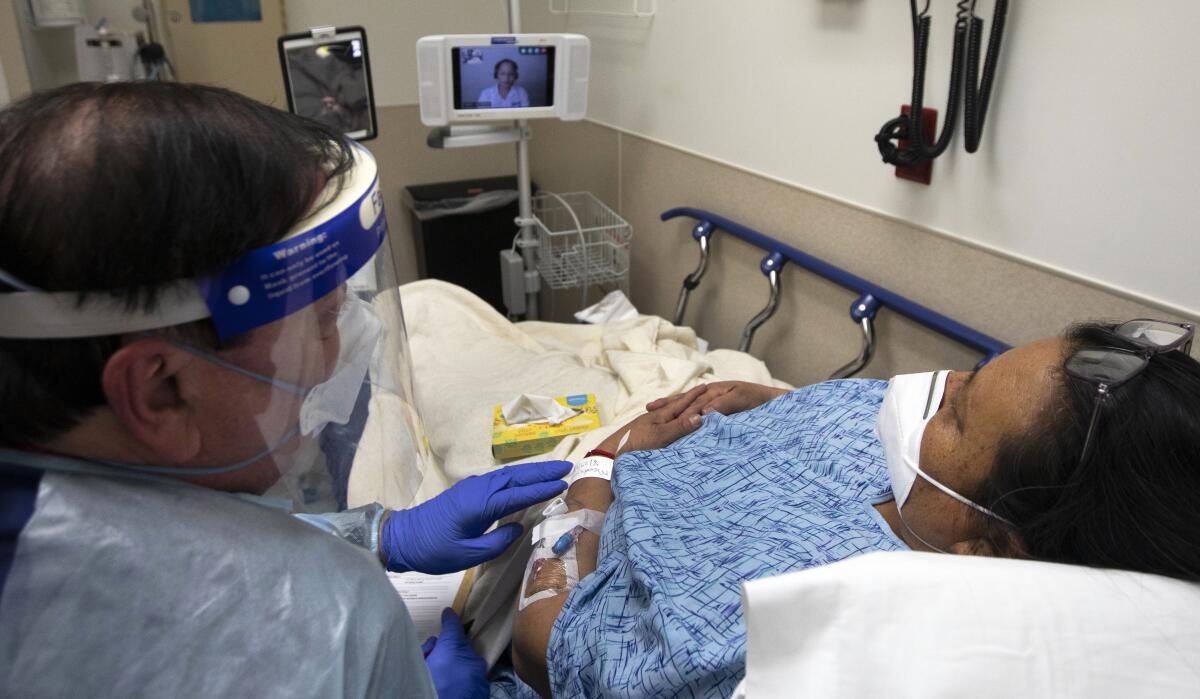
When most Americans went into shelter in place, clinicians went to work. They mastered their own fears of infection, donned ski goggles when personal protective equipment ran out, worked short staffed, pulled double shifts, held the hands of sick and terrified patients, read hundreds of articles in a daily scramble to learn how to treat this perplexing new disease, watched colleagues get ill, dreamed about the patients who didn’t survive and applauded the ones who did.
There was no greater act of compassion.
Now, as the wave of COVID-19 patients recedes, clinicians face a new wave of trauma and mental health consequences. I worry that the next wave will be an exodus of clinicians from the medical field.
As I write this, our medical facilities are filling patients who delayed care during the pandemic. We, the clinicians at the bedside, are leaning in again to deliver compassionate care.
Now is not the time to provide advice to our clinicians on how to reform their culture; rather, it is time to thank them and put them back together again. Our lives depend on it.
Mary Meyer, M.D., San Francisco
..
To the editor: As a registered nurse, I feel that Pearl confirms my view in his assessment of our flawed medical culture. When we see skyrocketing obesity, diabetes and hypertension rates, alarm bells should go off.
One glaring example of this flawed medical culture is the lack of nutritional education in medical schools. We are asked to bring in a list of our medications to our doctor appointments. Have we ever been asked to bring in a food diary?
The American Medical Assn. must be socially active in fighting for this focus on prevention and lobby for insurance coverage. Counseling that focuses on prevention should be covered as well.
Pearl mentions that we need more primary care providers, and those physicians need to be reimbursed at levels comparable to specialists. That will certainly help. Additionally, evaluating medical (and nursing) school education is the first step to provide a framework for health “promotion.”
Jackie Sarlitt, Irvine
..
To the editor: The “doctor culture” that Pearl describes is more a byproduct of for-profit healthcare than an outcome of medical training. Those like me, a registered nurse, who have worked in healthcare for years have watched the behemoth insurance and pharmaceutical industries grow to become obstacles to providing quality care, including preventive care.
Furthermore, the incentivizing of doctors by pharmaceutical companies is another unethical corporate activity. The opioid crisis was an indirect result of doctors being financially rewarded for not exercising enough caution in prescribing painkillers.
These pressures also cause burnout and moral distress because doctors and nurses must follow ethical standards in order to keep their license. Practitioners who hold a license are in their own moral space because they follow an ethical code of “first, do no harm,” which is frequently in opposition to maximizing profit.
Teresa Sanders, Long Beach
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.









