That pain in your back? It’s really a pain in your brain

- Share via
As a chronic pain sufferer, I sometimes surprise people by telling them that my pain doesn’t have a physical cause. It’s a mind-body thing, I say, related to stress and emotions. To many, this sounds like admitting to being a little bit crazy. And when I up the ante by suggesting they’ve probably had this kind of pain too, some become outright angry, interpreting my words to mean their pain is “all in their head.”
All of which makes a new study published in the Journal of Pain a big deal. It offers robust evidence that the overwhelming majority of chronic back and neck pain cases — among the most common chronic pain complaints — come from the mind, despite the fact that most diagnoses cite a physical cause, such as bulging disks or bone spurs.
In the new study, doctors assessed 222 consecutive pain patients at an orthopedic care clinic in Louisiana — everyone who showed up, as long as they could complete a questionnaire. Just 12% showed evidence of a structural problem as the root of their pain. Eighty-eight percent, on the other hand, had what the researchers call “primary pain,” which refers to symptoms generated by neural circuits in the brain rather than by “structural” damage to the body.
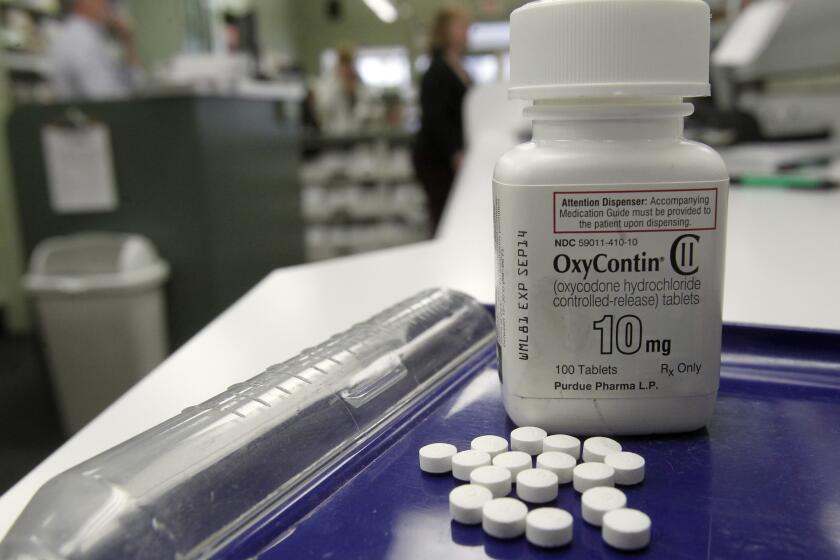
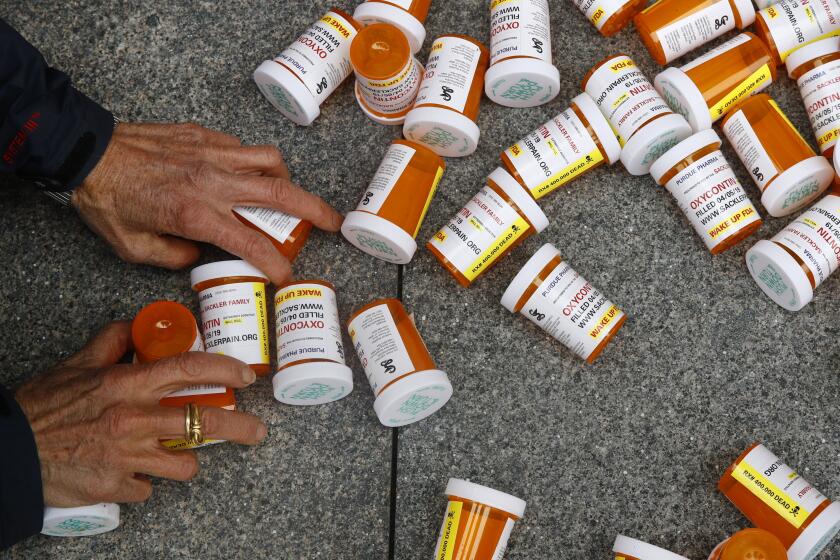
This year brought progress for safely getting opioids to people with debilitating pain.
Based on this and prior research, the authors believe that a process in the brain initiates the non-structural pain. The sensations could be the residual pain from a bodily wound that healed but didn’t notify the brain. Or the brain may have generated pain in the absence of any injury, perhaps in an effort to protect the patients from emotional wounds by occupying their attention with physical sensations instead.
The role of the brain and emotions in producing pain has long been known, and it has been validated by neuroimaging that shows that the brain processes physical pain and emotional distress in the same regions. Observational studies indicate that people feel more pain when primed with negative emotional stimuli. And additional research has shown that therapeutic interventions that help patients understand and reinterpret their pain can significantly reduce the symptoms. The theory is that pain is a danger signal, so as we come to feel safer and less threatened, our nervous systems shift out of fight-or-flight mode, and stop firing the pain signals.
As a result, scientists now believe that all pain is essentially brain pain. The idea is that just as the brain generates sensory experiences such as vision and hearing, it also generates pain by consulting our memories, expectations and emotions, as well as whatever physical inputs our nerves may sense, and creating pain when it determines we are under threat. While our nerves detect sensations, it’s the brain that decides if we’ll experience them as pain.
Exercise and different types of cognitive and physical therapy are proven to be more effective for pain patients than opioids and other pain medications.
The implications for healthcare are profound. Chronic pain is among the top reasons people seek medical care. More than 1.5 billion people worldwide suffer from chronic pain, including 50 million to 100 million Americans. For the most part, these patients are spending billions of dollars pursuing physical treatments. If the cause is non-physical, the money is wasted and the suffering only mounts.
And not only are we failing to alleviate the pain, we are creating dangerous side effects that include the opioid crisis as well as surgeries that may be unnecessary and can leave patients worse off.
Of course, sometimes chronic pain does have a physical cause, and distinguishing between when it does and doesn’t is crucial. To address this key challenge, the researchers at the Louisiana clinic devised a rule-out/rule-in diagnosis method that should be adopted far and wide.
Mind and body are both implicated when your body hurts. Recognizing the connection is crucial to treating pain.
The process starts with a thorough patient exam and review of scans to rule out physical causes of the pain. There is a nuance: Just because an anomaly — a squished disk in your back, for example — shows up on a scan, it is not necessarily the cause of pain. As the study explains, research repeatedly shows that the majority of people without pain show similar anomalies. In other words, doctors diagnosing the source of chronic pain need to be aware of the poor correlation between scary scans and pain.
The rule-in process further clarifies whether a patient has structural or mind-body pain. It consists of taking a detailed history of the patient’s pain and life. Doctors need to know if prior treatments that should have resolved structural causes have failed; if treatments associated with a placebo response brought relief; if a patient’s history contains significant stress or adversity; if they have other ailments associated with mind-body causes (headaches, gut and bladder conditions, fibromyalgia, chronic fatigue, tendonitis and more can have such associations). And they need to know if the pain is inconsistent — does it move around in the body or come and go; is it triggered by biologically irrelevant stimuli like the weather, smells or sounds? These variables don’t track well with structural causes.
The process may sound a bit subjective, and it is. But no more than any other diagnostic approach. Medicine is not an exact science, and doctors must act on imperfect information. “We deal in probabilities,” said Dr. Howard Schubiner, lead investigator of the Louisiana study and a clinical professor at Michigan State University College of Human Medicine. Using the careful criteria developed for the study offers as well-grounded a basis for action as anything: “When there is strong evidence using these criteria, a physician can be confident that what they’re seeing is a mind-body problem.”
The existing medical paradigm assumes a physical cause for most chronic pain. The findings in the Louisiana study suggest that’s often wrong.
Fortunately, my pain is much improved after years of pain education and good therapy helped my brain dial down my nervous system. Everyone deserves access to this new pain paradigm. And that requires ending the stigma still associated with mind-body symptoms, and understanding them as a universal human condition, not as the lot of people who are a little bit crazy.
Nathaniel Frank is the director of the What We Know Project at Cornell University’s Center for the Study of Inequality. He is writing a book about mind-body pain to be published by Mayo Clinic Press.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.