Coronavirus Today: A virus that knows no bounds
- Share via
Good evening. I’m Amina Khan, and it’s Thursday, Nov. 5. Here’s what’s happening with the coronavirus in California and beyond.
The COVID-19 pandemic has proven itself to be a border-defying affair — and that’s a dangerous reality that feels especially true for Americans living on the border itself.
Residents of El Paso are suffering from one of the biggest coronavirus outbreaks in the country. The city and surrounding county, with a population of 840,000, reported 3,100 new cases Wednesday — topping the previous daily record by more than 1,000. The 1,041 hospitalized patients and 311 in intensive care also broke records.
It’s the worst crisis to hit the city since a white supremacist entered a Walmart with a semiautomatic rifle last year and killed 23 people.
That killing was a binational tragedy, with victims from El Paso and its Mexican sister city of Juárez. So is the COVID-19 pandemic, claiming victims on both sides of the U.S.-Mexico border. That’s partly because the border, for those who live on it, has always been “somewhat intangible,” my colleague Kate Linthicum writes, “an arbitrary line crossed daily by tens of thousands of people for work, school and family.”
An effort by both nations to limit nonessential trips has cut border crossings somewhat, but infections have still spread amid the comings and goings. When Jazmín Cabrera traveled from El Paso to Juárez to pick up medication for her ailing — and pregnant — wife, she unknowingly infected a cousin during her trip.
The record numbers come in stark contrast to El Paso’s relative success only a few months ago; in September, the city‘s positivity rate fell as low as 4.5%. But then the city’s Republican mayor got in a public spat with a county judge who ordered nonessential businesses to close.
Now, close to a quarter of all coronavirus tests come back positive, and officials have had to build a makeshift hospital inside the city convention center and call in mobile morgues. Downtown is empty, but the cemeteries are seeing a steady stream of mourners.
Experts say that certain cultural mainstays, such as backyard barbecues and watch parties for the beloved Dallas Cowboys, helped fueled the rise in infections. So did local traditions in a place where tight familial structures and multigenerational family gatherings are common. (In some ways, it’s reminiscent of the outbreak in Italy, which was at one point the worst-hit country in Europe. There, experts also suggested that multigenerational households and gatherings could have fueled the alarming rate of deaths among the elderly in the country. )
Juárez Mayor Armando Cabada recently wrote a letter to Mexico’s foreign secretary asking him to stop Americans from entering the country, warning that “indiscriminate crossings” were contributing to the virus’ spread in his city. Cabada himself wound up hospitalized with COVID-19, leaving this week in a wheelchair.
People on both sides of the border are staying home if they can afford to do so — but many simply can’t. Javier Corral, a 34-year-old electrician, said while on break from a nearby construction site that several of his co-workers had tested positive for the virus.
“Everybody’s going to end up getting sick there,” he said. “We share the same tools.” He hated going to work, but felt he had little choice. “The bills don’t stop coming,” he said.
Cabrera said she hopes Joe Biden wins the presidential election and does a better job of getting the pandemic under control. In the meantime, she said, her focus was on the health of her wife and their child. “Just stay healthy — that’s all we have to do,” she said.
By the numbers
California cases and deaths as of 4:50 p.m. Thursday:

Track the latest numbers and how they break down in California with our graphics.
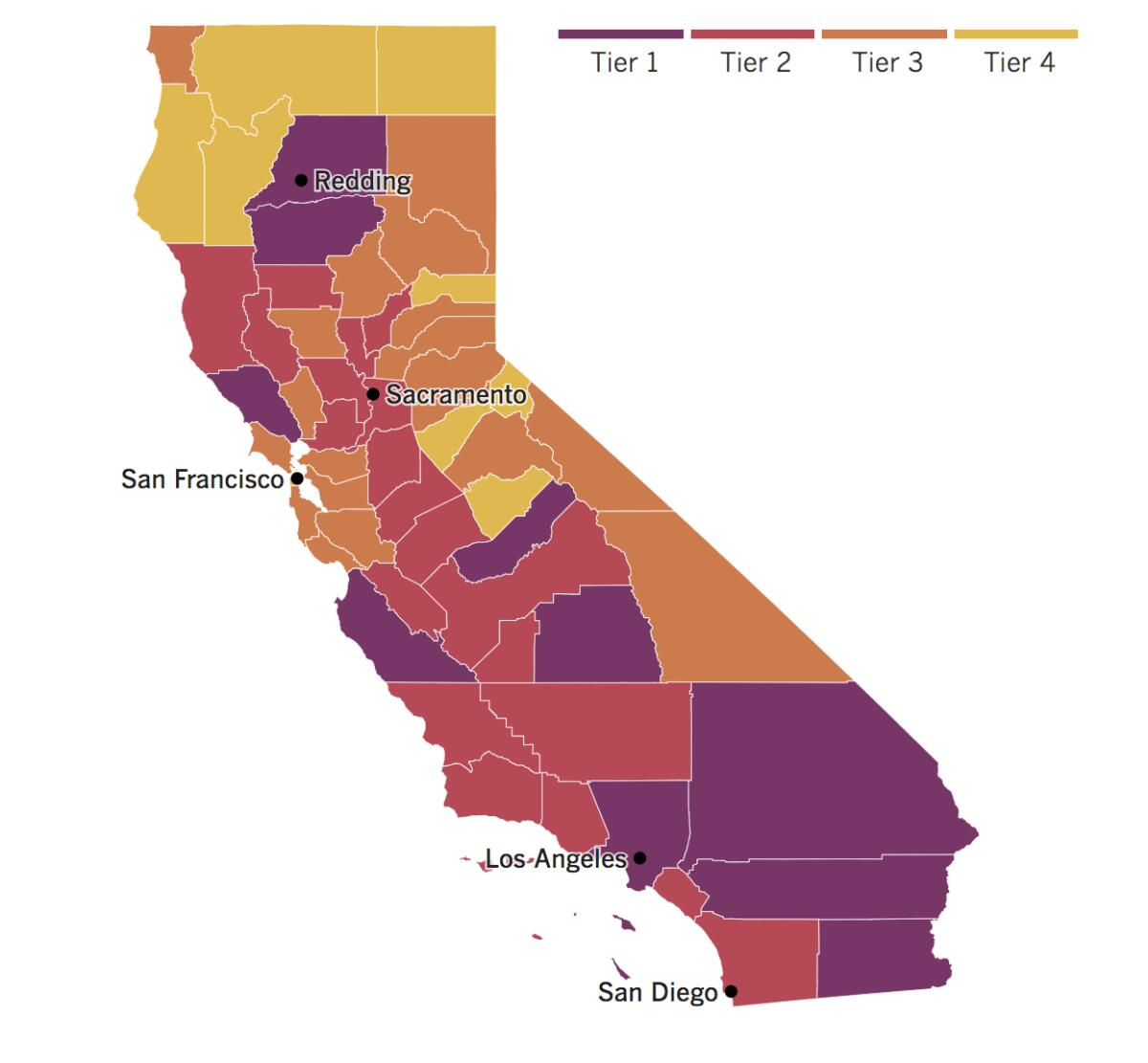
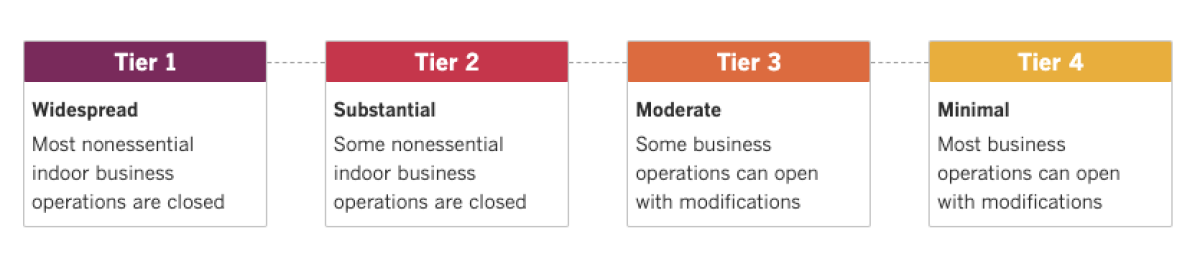
See the current status of California’s reopening, county by county, with our tracker.
Consider subscribing to the Los Angeles Times
Your support helps us deliver the news that matters most. Become a subscriber.
Across California
Los Angeles County officials have been hoping to get new coronavirus cases low enough that they could finally escape the dreaded, most restrictive “purple” tier on California’s four-tier roadmap for reopening the state. Those hopes have suffered a setback; officials reported 2,065 new coronavirus infections Thursday, a single daily case count one health official said hasn’t been seen in the region for months, and 25 additional deaths.
Once again, the county’s transmission rate has surpassed 1.0 — meaning that the number of people who could be infected by a single person is on the rise.
Last week, 1 in 1,000 residents were currently infected with the virus. Now it’s risen sharply, to 1 in 670.
“Unfortunately, the continued significant increase in cases reflects many instances where basic prevention measures were lacking,” said county Public Health Director Barbara Ferrer. “Unless we can all get back to protecting each other, our recovery will stall.”
The backsliding comes as the country enters a particularly dangerous point in the pandemic. Falling temperatures will push people indoors, where the coronavirus spreads more readily. And the holiday season will tempt people to gather with family and friends from outside their households, providing new routes for transmission.
California at large is also seeing some concerning patterns, with the statewide number of hospitalizations rising by 13.5% over the past 14 days and the number of intensive care patients growing by nearly 20%. These increases are troubling because hospitalizations are a lagging indicator that the virus is spreading. What’s more, the most recent statewide positivity rate for new infections rose from 2.6% to 3.3% over the prior 14 days. That’s low compared to the national average of 6.7%, but even a slight uptick can hamper — or even reverse — progress, my colleague Colleen Shalby writes.
San Diego County has so far avoided the purple tier, but an elevated case rate this week means it could fall from the “red” tier next week. State health officials said Wednesday that San Diego’s case rate currently sits at 7.4 per 100,000 — slightly higher than the limit of 7, which is the boundary between the red and purple tiers of the risk-ranking system. However, since it takes two consecutive weeks above the limit to trigger a demotion, the county still has a shot at staying in the red.
What’s going on? People are tired of the pandemic and letting down their guard — not wearing masks, not maintaining their distance, and generally not adhering to the precautions laid out by public health authorities, said County Supervisor Greg Cox. “Frankly, we need to do better, we need to do a lot better, and we can do better,” he said. If San Diego does wind up in the purple tier, businesses and other organizations would need to move their operations outdoors just as the weather turns cooler and wetter.
In Pac-12 football news, UC Berkeley‘s season-opening game against the University of Washington on Saturday has been canceled after one of the Golden Bears players tested positive. It triggered a contact-tracing effort involving a “significant” number of players, said Cal head coach Justin Wilcox.
The player who tested positive is asymptomatic. This was the first positive test on the football team since practices began last month.
Resources
— For general safety, wash your hands for at least 20 seconds (here’s a super-fun how-to video). Stop touching your face, and keep your phone clean. Practice social distancing, maintaining a six-foot radius of personal space in public. And wear a mask if you leave home. Here’s how to do it right.
— Watch for symptoms including fever, cough, shortness of breath, chills, repeated shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. If you’re worried you might be infected, call your doctor or urgent care clinic before going there.
— Need a COVID-19 test? Here’s how to receive a free test if you’re in L.A. County. And here’s a map of testing sites across California.
— Here’s how to care for someone with COVID-19, from monitoring their symptoms to preventing the virus’ spread.
— If your job has been affected by the pandemic, here’s how to file for unemployment.
— Here are some free resources for restaurant workers and entertainment industry professionals having trouble making ends meet.
— Advice for helping kids navigate pandemic life includes being honest about uncertainties, acknowledging their feelings and sticking to a routine. Here’s guidance from the CDC.
— In need of mental health services? Here are resources for coping during the crisis from the CDC and the L.A. County Department of Mental Health. L.A. County residents can also call (800) 854-7771 or text “LA” to 741741.
— For domestic violence victims, the pandemic can pose a “worst-case scenario,” advocates say. If you or someone you know is experiencing such abuse, call the National Domestic Violence Hotline at 1-800-799-SAFE (7233) or L.A. County’s hotline at 1-800-978-3600. Here are more ways to get help.
Around the nation and the world
Here’s a chilling story at the intersection of election and pandemic: A suburban St. Louis election official worked at a polling place Tuesday despite having tested positive for a coronavirus infection. Now that official has died, raising concerns for the 1,858 people who voted there.
The person who died was an election judge supervisor at the Blanchette Park Memorial Hall polling site in St. Charles, around 25 miles northwest of St. Louis, officials said. The poll worker had tested positive on Oct. 30 and had been advised to isolate for 14 days.
“The election judge nevertheless failed to follow the advice” and worked throughout the day on Nov. 3, a county spokeswoman said. The cause of death, age and gender of the individual were not given.
Contact tracing has begun, and the nine other election workers at the site were advised to be tested. The infected worker’s duties did not typically include handling iPads or otherwise having close contact with voters, officials said. All poll workers were required to wear masks or shields, the county’s elections director said.
This wasn’t the first sign that election workers there were taking a lax approach to the pandemic. The election authority came under fire in September for an email urging poll workers to “act surprised” if voters asked why they weren’t wearing masks. The email further instructed workers to apologize as they put their mask on, and to continue wearing it “until the voter leaves the polling place.”
Cost pressures are forcing media companies to cut jobs and reconfigure their business models. Lionsgate said it was laying off 15% of the staff in its film division as the company deals with pandemic-triggered changes in the movie industry. And ESPN is cutting 500 jobs and accelerating its move into streaming. The company lost a huge chunk of its programming when the coronavirus shortened the NBA and Major League Baseball seasons. The cuts are the latest within Walt Disney Co., which said in September that it would lay off 28,000 domestic employees at its parks, experiences and products division, which includes Disneyland Resort and Disney California Adventure Park in Anaheim and Walt Disney World in Orlando, Fla.
In slightly more hopeful news, AstraZeneca officials say the company hopes to show that its COVID-19 vaccine is effective by the end of this year and is ramping up manufacturing now to supply potentially hundreds of millions of doses in January.
The European drugmaker is working with Oxford University to develop one of the most-watched vaccines, which is in late-stage trials to determine its safety and effectiveness. A successful vaccine could be a formidable weapon in the arsenal of public health authorities.
The United Nations voted overwhelmingly on Thursday to hold a summit on the COVID-19 pandemic in early December. The goal, they said, is to encourage stronger action against the coronavirus and its “unprecedented” effects on societies, economies, jobs, global trade and travel. The special session will be “a belated first step” and a test for multilateralism, according to General Assembly President Volkan Bozkir.
Efforts to coordinate a response among leaders of the 20 major industrialized nations fizzled in March, depriving the world of its best chance to suppress the coronavirus in all countries.
Instead, said U.N. Secretary-General Antonio Guterres, the coronavirus moved “every way, everywhere.”
Your questions answered
Today’s question comes from a reader who wants to know: What is the difference between isolation and self-quarantine?
This reader says she hears the terms used interchangeably. We’ll turn to the U.S. Centers for Disease Control and Prevention, which offers a handy explanation:
- Quarantine is when you feel fine, but you separate yourself from others because there’s a high chance you’ve been exposed to someone with the disease.
- Isolation is when you avoid people because you have symptoms of the disease, or have tested positive for the virus, and don’t want to get other people sick.
Keep in mind, isolating also means separating yourself from members of your own household so that you can avoid passing the virus on to them, to the extent possible.
This may explain why many states ask people entering their borders to “self-quarantine” for 14 days before resuming their normal activities, rather than using the term “isolate.” While travelers may feel just fine, there’s a chance they’ve been exposed to the virus and just don’t know it yet.
But it’s true that many people seem to use the terms interchangeably, possibly because the goals and practices of both largely overlap, Dr. George Rutherford of UC San Francisco told my colleague Deborah Netburn.
“They have the same end game, which is that you are sequestered from the rest of the public for a period of time,” he said.
It can be a bear, but self-quarantining and isolating are a very important means to prevent further spread of the virus.
Our reporters covering the coronavirus outbreak want to hear from you. Email us your questions, and we’ll do our best to answer them. You can find more answers in our Frequently Asked Questions roundup and in our reopening tracker.
For the most up-to-date coronavirus coverage from The Times over the weekend, visit our homepage and our Health section, sign up for our breaking news alerts, and follow us on Twitter and on Instagram.




