Coronavirus Today: We’re not out of the woods yet
- Share via
Good evening. I’m Amina Khan, and it’s Tuesday, Dec. 15. Here’s what’s happening with the coronavirus in California and beyond.
They were the shots heard ‘round the state. Five healthcare workers in Los Angeles became the first in the area Monday to receive the COVID-19 vaccine developed by Pfizer and BioNTech outside of a clinical trial. In San Francisco, Dr. Anthony Gomez, medical director of critical care at Zuckerberg San Francisco General Hospital, and Phung Ngyuen, a registered nurse in intensive care there, were the first in their city to roll up their sleeves for a jab.
But while the shots offered a dose of hope, they didn’t change the fact that California is currently facing the worst wave yet of the COVID-19 pandemic. Record numbers of people are being infected and hospitalized, causing beds in intensive care units to become vanishingly scarce in many parts of the state.
Gov. Gavin Newsom, who was on hand for the first vaccinations in Los Angeles, said he was “enthusiastic that there is light at the end of the tunnel, but mindful that we’re still in the tunnel.”
“We are in the midst of the worst moment of this pandemic,” he added.
Indeed, the five Kaiser staffers didn’t get a break after receiving their landmark shots — they went straight back to work. “It’s way busier now than it was initially,” said Kim Taylor, a 53-year-old nurse in the emergency department.
Taylor and her colleagues know all too well that the pandemic is far from over. After getting her shot, she stood in front of television cameras and asked the public to keep wearing masks, stay home for Christmas and get vaccinated as soon as they could.
“We front-line workers have been working around the clock over the past nine months, sacrificing so much of what we do and love to take care of our patients,” she said. “We’ve been doing this while trying to take care of our own families and keep them safe. ... We can’t win this fight alone. We need your help to keep our numbers down.”
Experts estimate it will be mid-2021 by the time Californians who aren’t on a priority list will be able to get vaccinated whenever they want. That’s several months more of coronavirus infections, hospitalizations and deaths — a burden that these medical workers will have to bear until we achieve herd immunity. In the meantime, ordinary Californians can help reduce the burden by wearing masks and engaging in good social-distancing behaviors.
“The choices every person and every business make throughout each day have an impact on what happens in our hospitals,” said L.A. County Public Health Director Barbara Ferrer. “If you’re not playing by the rules, to put it blunt, at this point you’re part of the problem, and you’re contributing to the distressing increases that we see in cases, hospitalizations and deaths.”
By the numbers
California cases and deaths as of 5:52 p.m. PST Tuesday:

Track the latest numbers and how they break down in California with our graphics.
Across California
In Southern California, the number of available ICU beds is plunging to critical levels. There are none left in Riverside County, and just 1% of Ventura County’s beds are empty. In L.A. County, home to 10 million people, fewer than 100 ICU beds are available. The 935 COVID-19 patients currently being treated in the county’s ICUs are more than quadruple the number from Nov. 1.
That may sound very bad, but experts say the worst of the surge is still to come. L.A. County has more than 4,400 people hospitalized with COVID-19, and that number could hit 5,000 by the weekend. “Our reality is frightening at the moment,” Ferrer said.
Cases continue to surge across the state. An L.A. Times tally logged an unprecedented 42,129 cases Monday, shattering the single-day record of 35,400 new cases set on Dec. 8.
Such alarming trends haven’t stopped some folks from engaging in the kinds of dangerous behaviors that helped fuel the surge. The city of Los Angeles has sued the people it says are behind an underground nightclub called LA Party Society. Sequestered behind an empty storefront in the Fashion District, it has been violating COVID-19 restrictions under the cover of night, authorities say.
The venue has allegedly held crowded events for months, said City Atty. Mike Feuer. There’s even evidence of multiple shootings at the site, he said. Authorities are seeking millions of dollars in damages from the venue’s manager and others associated with it. “Beyond the bullets and the assaults and the other criminal activity, I want to emphasize that packing people into an indoor space — an unlicensed club — during the pandemic, is the height of irresponsibility,” Feuer said.
Meanwhile, L.A. Unified School District officials say that due to pandemic hardships, any failing grades from this semester will be deferred until at least Jan. 29, giving students extra time to avoid getting an F in their classes. The move is the latest attempt by the nation’s second-largest school district to avoid punishing students while the coronavirus outbreak continues to disrupt their education and worsen family hardships, my colleague Howard Blume writes.
Grades have dramatically deteriorated compared with last year, particularly for Latino and Black students, English learners, students with disabilities, foster youths and those experiencing homelessness, according to a directive sent to secondary school principals Monday.
Santa Ana Unified in Orange County has also adjusted its grading practices to help more students pass their classes. Overall, though, fewer school systems appear to be offering grading relief than in the spring, when the sudden shutdown of campuses made it difficult to pivot to online learning.
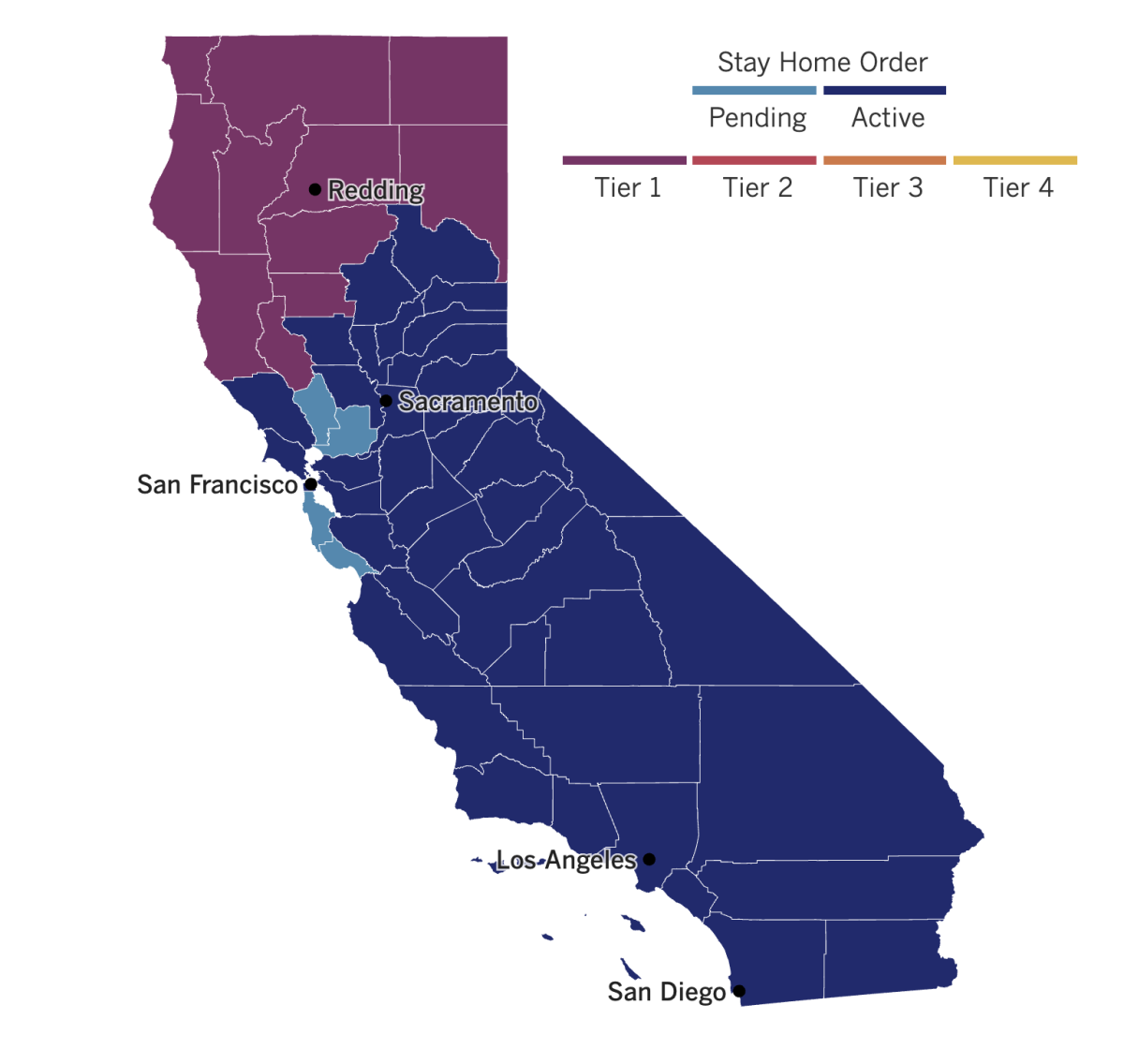
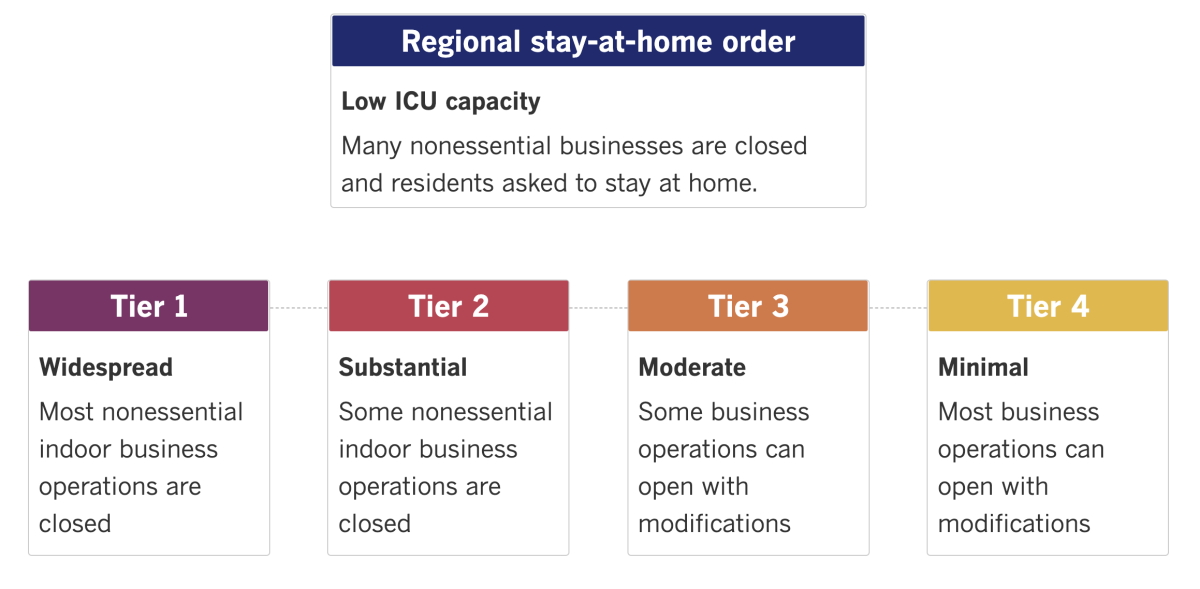
See the latest on California’s coronavirus closures and reopenings, and the metrics that inform them, with our tracker.
Consider subscribing to the Los Angeles Times
Your support helps us deliver the news that matters most. Become a subscriber.
Around the nation and the world
If the COVID-19 vaccine from Pfizer and BioNTech was good enough to get a nod from the U.S. Food and Drug Administration, the vaccine from Moderna and the National Institutes of Health is almost certain to follow in its footsteps.
The FDA on Tuesday released its detailed analysis of the Moderna vaccine’s performance in a Phase 3 clinical trial of more than 30,000 people. The bottom line: It was 94.5% effective at preventing cases of COVID-19.
Like the Pfizer vaccine, the one from Moderna proved to be effective across a wide range of study participants. Notably, it was 100% effective in Black and Latino volunteers, and it was 100% effective in preventing COVID-19 in senior citizens. Check out our head-to-head comparison to see how the two vaccines match up.
An advisory group of independent scientists and other experts will pore over the data on Thursday before voting on whether to recommend emergency use authorization for the Moderna offering. An endorsement would clear the way for FDA authorization within days.
In Sweden, which famously took a much more laissez-faire approach to pandemic restrictions, health officials misjudged the virus’ staying power, the country’s prime minister said Tuesday.
“I think that most people in the profession didn’t see such a wave in front of them,” Prime Minister Stefan Lofven told the Aftenposten newspaper. The country of just over 10 million has logged more than 341,000 infections and more than 7,600 deaths — a toll far higher than its neighbors Norway, Finland and Denmark.
Sweden attracted worldwide attention for its decision not to impose stringent restrictions, instead relying on residents to maintain hygiene and follow social distancing protocols. While people around the world remained in their homes and wore masks when required to go out in public, Swedes continued to head to work, restaurants and bars without wearing masks or staying several feet apart. Now it’s facing one of the highest per-capita COVID-19 death rates in the world.
With COVID-19 vaccination campaigns underway in Britain, the U.S. and Canada, some are asking European Union regulators why they haven’t gotten their doses yet. Germany has demanded that EU authorities approve the vaccine faster than planned, and it may get its wish.
The European Medicines Agency said it is moving its previously scheduled Dec. 29 meeting on the Pfizer vaccine to Monday. The agency said the decision was made because it had received additional data from the vaccine makers — but the move also came after Berlin and other European capitals expressed growing impatience with the agency’s timetable.
“Our goal is an approval before Christmas,” German Health Minister Jens Spahn said Tuesday. “We want to still start vaccinating this year.”
If you’re also wondering why the EMA is taking so long, here’s a handy explainer on the process. According to EMA Executive Director Emer Cooke, while the U.S., British, Canadian and EU regulators are all largely looking at the same data, “we may not have all gotten it at the same time.”
Your questions answered
Today’s question comes from a reader who wants to know: If I had COVID-19 several months ago but still have symptoms now, am I still likely to be contagious?
Dr. Hana Akselrod, an infectious disease physician at the George Washington University School of Medicine and Health Sciences, said it’s unlikely for the virus to hang around in most folks’ systems for that long.
“Studies of viral shedding in people during and following COVID-19 show that the virus is no longer present in a form capable of infecting others after about 10 days in most people,” Akselrod said in an email. “It takes longer to clear in people with severe disease (e.g. those requiring hospitalization) or in those with compromised immune systems — about 20 days. It is vanishingly rare for the virus to be detected for longer than that.”
However, a lot of people — roughly 1 in 10 by some estimates — still experience symptoms well after they were infected, she said, referring to it as long COVID or post-COVID syndrome.
“These people should not be treated as contagious, but should still take all standard recommended precautions outside of their household, such as masking and social distancing — since we do not know to what extent they are at risk of becoming infected a second time, and if that could trigger a worsening of their symptoms,” she explained.
The Centers for Disease Control and Prevention recommends that people diagnosed with COVID-19 isolate themselves to avoid transmitting the virus for a minimum of 10 days if they have a mild infection. They should remain isolated for at least 20 days if their disease is severe (i.e. if they require hospitalization) or if they’re immunocompromised, because their bodies may have a tougher time clearing the virus, Akselrod said. There’s no official guidance on the maximum duration of isolation, she added.
“Although molecular tests can pick up on bits of viral material in people for longer, evidence suggests that after the above duration of time the virus is no longer capable of replicating itself or infecting others,” she said.
Of course, in complicated situations, it’s important to consult with your personal physician about the best course of action to take, Akselrod said.
We want to hear from you. Email us your coronavirus questions, and we’ll do our best to answer them.
Resources
Practice social distancing using these tips, and wear a mask. Here’s how to do it right.
Watch for symptoms such as fever, cough, shortness of breath, chills, shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. Here’s what to look for and when.
Need to get tested? Here’s where you can in L.A. County and around California.
Americans are hurting in many ways. We have advice for helping kids cope, resources for people experiencing domestic abuse and a newsletter to help you make ends meet.
For our most up-to-date coverage, visit our homepage and our Health section, get our breaking news alerts, and follow us on Twitter and Instagram.




