Coronavirus Today: A life-or-death social experiment
- Share via
Good evening. I’m Amina Khan, and it’s Tuesday, Jan. 26. Here’s what’s happening with the coronavirus in California and beyond.
As of yesterday, Californians are in the midst of what you might call an uncontrolled experiment brought on by Gov. Gavin Newsom’s sudden move to lift the state’s regional stay-at-home order, allowing outdoor dining and other business operations to resume. It’s a high-risk, high-reward bet that we can avoid another deadly surge in the coming months even if the rules are relaxed amid a slow and frustrating vaccine rollout and the spread of more contagious strains of the virus.
The good news: After a fall-and-winter surge that left roughly 20,000 people dead, it looks like California may be rapidly bending the curve. COVID-19 hospitalizations began falling about 2½ weeks ago, and much of that progress may be thanks to residents who changed their behavior by avoiding travel, staying home and following the new rules.
Newsom said Monday that conditions have improved enough that it’s worth giving reopening a shot. “We’re seeing a flattening of the curve. Everything that should be up is up; everything that should be down is down — case rates, positivity rates, hospitalizations, ICUs. Testing is starting to go back up, as well as vaccination rates in this state,” he said.
Here’s the thing, though: California is just clawing itself out of a devastating surge that made it the epicenter of Americans’ COVID-19 pandemic. All but four of the state’s 58 counties are in the highest-risk purple tier, where transmission of the virus is “widespread.” (Yesterday we mistakenly called this the red tier — sorry! The map we shared was correct.) Hospitals were overflowing, ambulance patients faced up to 17-hour waits just to get into emergency rooms, hospital morgues were filled to capacity and funeral homes were forced to turn families away. So many people were dying that officials even had to suspend air-quality regulations that limit the number of cremations in Los Angeles County earlier this month.
All this raises the question: Are we really out of the woods?
UC Berkeley epidemiologist Dr. John Swartzberg doesn’t sound too sure. He said he worried that lifting the stay-at-home order was “premature” because the new coronavirus cases, while declining, are still very high. It might make more sense to wait a few weeks until cases go down further and California can begin reopening with a lower baseline level of virus in the community, he said.
Another key point: After last year’s spring and summer surges, California reopened without bringing its case numbers to a low level. That meant that when the next surge hit, it became even bigger than the one before it, he said.
“It’s like we’re climbing this mountain. We go two steps up and we just take one step back, and we take two steps up from there and one step back, and we keep just having more cases,” Swartzberg said. “We’re doing a lot better than we were doing 2½ weeks ago, but we’re doing terrible compared to three months ago. We need to knock these cases down so as we get more and more people vaccinated, we’ll get to a safer environment much more quickly.”
For now, though, it looks like many counties are liking the state’s odds. Los Angeles County officials quickly moved to reopen outdoor dining, with the city of L.A. following its lead; so did San Francisco, although a curfew and travel quarantine requirement will remain in place there. (Angelenos: Here’s what you need to know about what’s happening to restrictions in L.A. County.)
Ultimately, state and local officials are betting on people, not the virus. Their actions amount to a wager that this time, Californians will exercise restraint when they’re given more freedom. The stakes of this bet are literally life and death.
As L.A. County Public Health Director Barbara Ferrer said, “We’re anxious, as is everyone, to move forward.” But “this all depends on all of us” she stressed, and if the county’s coronavirus situation starts deteriorating again, “we’ll be in the horrible position of once again needing to backtrack.”
By the numbers
California cases, deaths and vaccinations as of 7:21 p.m. PST Tuesday:
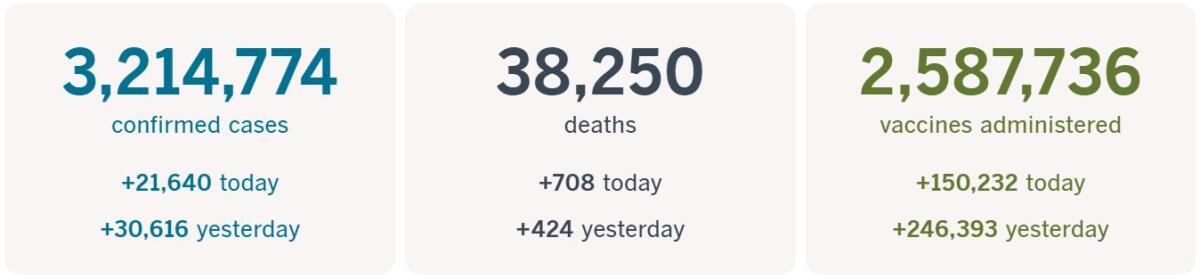
Track the latest numbers and how they break down in California with our graphics.
Across California
Los Angeles-area restaurant owners are wasting no time in flinging open their doors to customers (figuratively speaking, anyway — indoor dining is still banned). Angela Marsden, owner of Pineapple Hill Saloon & Grill in Sherman Oaks, is one of them: She became famous after posting a video in which she tearfully described how the county’s rules were upending her business. On Monday, she was once again verklempt — except this time, she was overcome with joy and anxiety as she spoke about being able to reopen.
“I don’t want to get overexcited. I just don’t know what’s going to happen next,” Marsden said. “But if they were to let us open and keep us open outdoors, and not shut us down again, it definitely would give hope to me and to other businesses.”
She had already started staking out a game plan: The electrical equipment to power her patio set-up had been rained on and would need sorting out; tables would need cleaning; staff would have to be called back — if they were even still available. If she didn’t have enough hands, she’d wait tables herself. “I’ll do whatever it takes to keep my business going,” she said.
Some key news on the vaccine front: California officials said the next round of COVID-19 inoculations will be prioritized based on age instead of specific occupations considered higher-risk. The shift, which Newsom announced Monday, leaves unchanged the current priority list, which focuses on healthcare workers and people 65 and older before expanding to teachers, farmworkers and first responders.
After them, though, things will change. The original plan’s next tier of priority would have opened the queue to workers in manufacturing, transportation and commercial and residential settings, along with people who are incarcerated or homeless. But under the new plan, the next priority will be people under 65. No details about the criteria have been released yet, but they could end up focusing on people over 50 first.
The move comes as the state struggles to get enough vaccine doses to meet demand. State officials said just last week that it could take until June to vaccinate all those 65 and older. And L.A. County said that unless more supply becomes available, it may take until next year to vaccinate everyone. “We realize we have got to increase throughput here,” Newsom said.
A new analysis of 50,000 students from 18 school districts across California is adding to evidence of the harm that campus closures have wrought to student learning. Researchers with Policy Analysis for California Education, based at Stanford University, found significant learning loss, especially in younger students, students from low-income families and students learning English.
That last group was particularly hard-hit: English learners, who make up nearly 20% of California’s public school students, lost the equivalent of about 30% of their typical learning growth, compared to a roughly 10% loss for other students.
The analysis also suggested that some higher-income students actually had learning gains during distance learning — accelerating an already steep learning gap between those with more and fewer resources, my colleagues Howard Blume and Paloma Esquivel write.
The findings come as both Los Angeles schools Supt. Austin Beutner and leaders of the teacher’s union make the case that students should not return to class until teachers have been vaccinated. (The teachers union also says coronavirus case rates will need to come down significantly before campuses can reopen.) Some officials have expressed frustration that teachers are not being prioritized.
“We’re never going to get back if teachers can’t get vaccinated,” said Assemblyman Patrick O’Donnell (D-Long Beach), who chairs the state’s Assembly Education Committee and has two high schoolers learning from home. Incidentally, Long Beach, which has its own independent health agency, has begun letting teachers get shots.
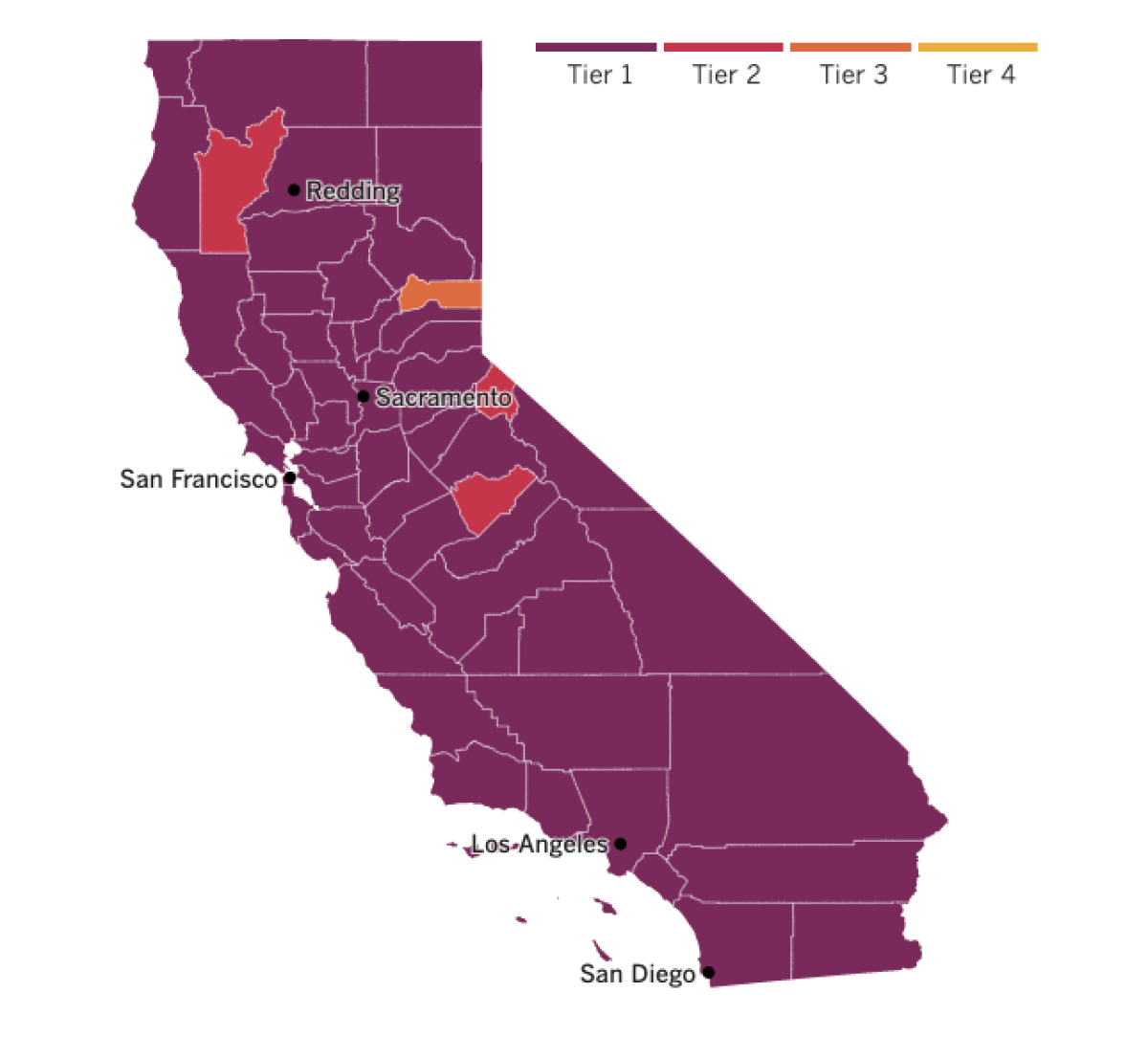
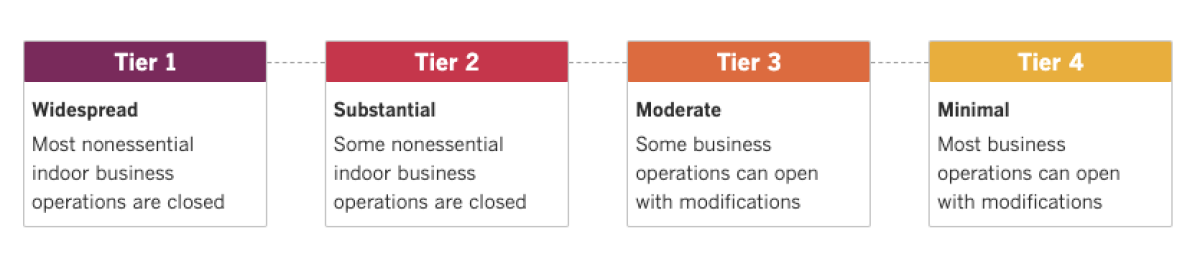
See the latest on California’s coronavirus closures and reopenings, and the metrics that inform them, with our tracker.
Consider subscribing to the Los Angeles Times
Your support helps us deliver the news that matters most. Become a subscriber.
Around the nation and the world
In Washington, the Biden administration plans to rush more COVID-19 vaccine doses to states, territories and tribal governments and to buy another 200 million, my colleague Chris Megerian reports.
The plan calls for 10 million doses to be distributed each week for the next three weeks, up from the current 8.6 million — part of an administration effort to inoculate more Americans more quickly. Biden said the additional 200 million doses he plans to buy would be delivered this summer — half from Pfizer and half from Moderna. Because each vaccination requires two doses to be fully effective, the additional supply would be enough to inoculate an additional 100 million Americans.
The moves come as the new president sets a more ambitious goal for COVID-19 vaccinations in his first 100 days in office, raising the target from 1 million to 1.5 million per day. The country has already surpassed the 1-million-doses-per-day mark over the last week. As of Sunday, the federal government had distributed 41.4 million vaccine doses to states and other jurisdictions, according to the Centers for Disease Control and Prevention. Of those, 21.8 million doses — nearly 53% — had been administered.
“The brutal truth is, it’s going to take months before we can get the majority of Americans vaccinated,” Biden said Tuesday. “In the next few months, masks — not vaccines — are the best defense against COVID-19.”
In less optimistic news, a new Brazilian coronavirus variant has made its way to the U.S. in a person who recently returned home to Minnesota after traveling there, officials said Monday. The Brazil P.1 variant was found in a specimen from a patient living in the Minneapolis-St. Paul area who fell ill in the first week of January, the state’s health department said. There was no immediate sign that the variant was spreading in Minnesota.
The Brazil variant would be among the latest in a suite of unwanted viral visitors to the U.S. It contains a set of mutations that may affect its ability to be recognized by antibodies that are sometimes used to treat patients, according to the CDC.
Some researchers have already expressed concern that compared to its viral predecessors, the Brazilian variant may have an easier time sneaking past the immune systems of people who have already survived a bout with COVID-19, making reinfection more likely. If confirmed, “that would be disturbing,” said Dr. William Schaffner, an infectious disease specialist at Vanderbilt University.
Either way, the case underscores the importance of testing and the need to for everyone to remain vigilant, said Jan Malcolm, Minnesota’s health commissioner. “The fewer people who get COVID-19, the fewer opportunities the virus has to evolve,” Malcolm said in a statement.
In Mexico, three of the country’s most powerful men — the president, the billionaire Carlos Slim and a retired archbishop — are suffering from COVID-19, my colleague Kate Linthicum writes. It’s a sign of how thoroughly the virus has managed to infiltrate the country, even those occupying its traditional axis of power — church, state and commerce.
Mexico has recorded nearly 150,000 official COVID-19 deaths — the fourth-highest death toll in the world — but officials say the true count is much higher. The country logged 274,486 more deaths of all types in 2020 than in a normal year, and health experts said the vast majority are probably attributable to the pandemic.
The current surge appears linked to the Christmas holidays, when families gathered in large groups despite health officials’ pleas. For days, hospitals in several of the country’s major cities have been near capacity, with many forced to turn away desperate patients.
President Andrés Manuel López Obrador’s government has been criticized worldwide for its lackadaisical response to the pandemic. Mexico has refused to invest in widespread testing, allowing the contagion to spread undetected, and the president has opted not to wear a mask even in public settings. He announced that he had tested positive shortly after returning from a multistate tour, holding several meetings and attending two events.
Your questions answered
Today’s question comes from readers who want to know: What happens if my second dose of vaccine is delayed?
Both of the COVID-19 vaccines authorized for emergency use in the U.S. require recipients to get two doses, spaced three weeks apart for the Pfizer-BioNTech shot and four weeks apart for the Moderna offering. Many folks have been worried about what might happen if they can’t get their second shot on their target date.
Dr. Diane Griffin, a virologist at the Johns Hopkins Bloomberg School of Public Health who studies immune responses to viral infections and vaccines, said you do not have to get the second dose exactly three or four weeks after your first one.
“The first dose ‘primes’ the immune system to respond to the second dose with a better response, but that can also occur if the second dose is later,” Griffin said.
“Basically, the first dose stimulates proliferation of the small number of virus-specific immune cells, and these expanded cell populations can then respond to the second dose by proliferating to produce even more cells,” she explained. “This ‘boosting’ effect can occur for quite a long time after the first dose.”
The problem is that in the clinical trials for the Pfizer and Moderna vaccines, study participants got their second shots on time. Other intervals between the two doses simply haven’t been tested in the same way as the current recommended intervals, she said. That means we don’t know if a significant delay results in a reduction in efficacy, or how long you can really wait.
Based on what’s known about other vaccines and immune responses, a gap of six to 10 weeks “is probably still OK,” she said. An even longer gap might work too, she said.
“The bottom line is that people should try to get the second dose on time, but it is probably never too late to get it,” she said. “Getting a second dose late is better than not getting it at all.”
We want to hear from you. Email us your coronavirus questions, and we’ll do our best to answer them.
Resources
Need a vaccine? Keep in mind that supplies are limited, and getting one can be a challenge. Sign up for email updates, check your eligibility and, if you’re eligible, make an appointment where you live: City of Los Angeles | Los Angeles County | Kern County | Orange County | Riverside County | San Bernardino County | San Diego County | San Luis Obispo County | Santa Barbara County | Ventura County
Practice social distancing using these tips, and wear a mask. Here’s how to do it right.
Watch for symptoms such as fever, cough, shortness of breath, chills, shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. Here’s what to look for and when.
Need to get tested? Here’s where you can in L.A. County and around California.
Americans are hurting in many ways. We have advice for helping kids cope, resources for people experiencing domestic abuse and a newsletter to help you make ends meet.
For our most up-to-date coverage, visit our homepage and our Health section, get our breaking news alerts, and follow us on Twitter and Instagram.




