Coronavirus Today: California encourages vaccine “passports,” just not by name
- Share via
Good evening. I’m Melody Petersen, and it’s Monday, April 19. Here’s what’s happening with the coronavirus in California and beyond.
California health officials have repeatedly said they have no plans to issue COVID-19 vaccine “passports” — digital or paper passes that would allow vaccinated residents or those who’ve tested negative into concerts, baseball games and other arenas.
But that didn’t stop them from giving businesses a financial incentive to require them.
When state officials announced reopening rules this month, they said businesses holding indoor live events could welcome many more people — if they required proof of vaccination or a recent negative test, my colleague Maura Dolan reports.
“Of course, it is a form of a vaccine passport,” said Dr. John Swartzberg, a UC Berkeley infectious-disease expert.
The passports have become a hot political issue across the country. Republican governors in Texas and Florida have banned them, while Democratic officials in New York authorized the “Excelsior Pass” to prove vaccination or a negative test result for entry to Madison Square Garden and other large venues.
Dr. Mark Ghaly, California’s health and human services secretary, said he did not view the state’s new rules for reopening indoor venues as including a vaccine passport. A pass system would have to be carefully designed to protect privacy and ensure fairness, he said.
“We’re working through whether it makes sense in the highest-risk venues — large, indoor, random-mixing environments — where there could be an expectation to have vaccine or testing verification,” Ghaly said.
The state rules vary according to a county’s place on the government’s color-coded risk tier. In the orange tier, in which virus spread is moderate, the capacity for indoor venues is capped at 15% or 200 people. But if the operator demands proof of vaccination or a negative test, the venue can more than double capacity to 35%.
On Monday, state officials increased that “capacity bonus” even higher — to as much as 50% in the orange tier and 75% in the less restrictive yellow tier.
Under the rules, theaters, music halls and other indoor venues will have to decide whether opening at limited capacity makes financial sense and whether they want to risk blowback from customers who object to verification of vaccinations or tests.
A current hurdle for those supporting the passports is the regulatory status of the vaccines being administered. They didn’t go through the usual approval process at the Food and Drug Administration. Instead they gained emergency use authorizations, which include language that says patients “have the option to accept or refuse” the shots.
But once one or more of the vaccines gain full FDA approval, legal scholars say states can require them.
“Communicable disease creates a special imperative that authorizes things that otherwise people might be skeptical about,” said UCLA constitutional law professor Eugene Volokh.
But he added that it is not surprising that the verification systems might worry some.
“It’s just not an American thing to be constantly told, ‘Your papers, please,’” he said.
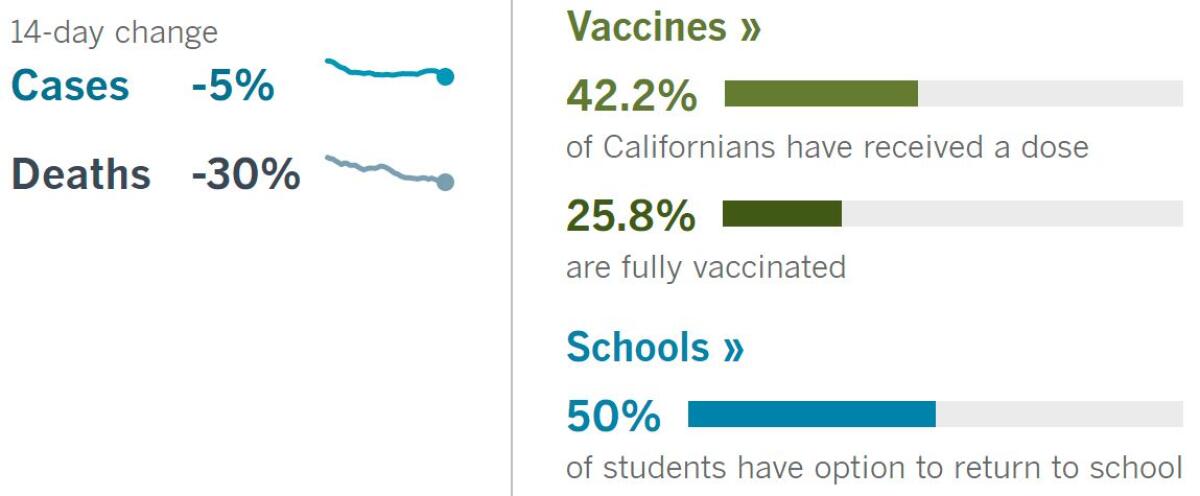
By the numbers
California cases, deaths and vaccinations as of 5:52 p.m. Monday:

Track California’s coronavirus spread and vaccination efforts — including the latest numbers and how they break down — with our graphics.
Across California
Thanks to the pandemic, L.A. County residents rate education among the worst of several factors affecting their quality of life, displaying one of the biggest drops in recent years among parents of children in public schools, according to a UCLA survey.
More than three-quarters of parents in the county with children ages 5 to 18 believe their children have been “substantially hurt” academically or socially by being away from school and taking part in distance learning for months.
“It’s a big number,” said Zev Yaroslavsky, director of the Los Angeles Initiative at UCLA’s Luskin School of Public Affairs, which publishes an annual Quality of Life index in partnership with the public-opinion firm FM3 Research. “It’s not counterintuitive; it’s intuitive, but the number surprised most of us — and it was across all the demographics.”
The Quality of Life index is a score on a scale of 10 to 100 that reflects how satisfied people are in nine categories and the weight they assign to each category. The overall score this year remained relatively steady, at 58 — meaning residents rated their overall quality of life slightly more positively than negatively — but there were notable shifts within the categories, and differences by subgroups.
For example, parents of children in public schools gave education an overall score of 52, compared with 58 last year. That’s one of the steepest declines in any category in the index’s six-year history. In large part, the change reflected dissatisfaction with the quality of K-12 education and training for “jobs of the future.”
The index also put income inequalities into stark relief. The overall Quality of Life index came in at 49 for people who said their income dropped by “a lot” in the last year, a group that represented 22% of the sample. The score for the 56% of respondents who said their income stayed the same or went up was 62.
“The pandemic has exposed the two L.A.s again,” Yaroslavsky said.
That contrast between the two sides of the city was also detailed in a story by Times reporters covering last week’s resumption of in-person classes at L.A. Unified campuses.
There are only four communities where more than 40% of students were expected to return to in-person school, according to district data collected in a parent survey: western Los Angeles, Woodland Hills, Westchester and Venice. Each is a higher-income community with majority-white populations in which COVID-19 has treaded more lightly than in neighborhoods with larger Latino and Black populations.
In Latino-majority communities such as South Gate, East L.A., Pico Union and Bell, only about 25% of students were expected to return.
At Madison Elementary School in South Gate, 10-year-old Anthony Sosa was told that only five students would be in his classroom. But that didn’t dim his excitement.
“I’m going to get to play with my friends!” he said.
Once the school day started, teachers took turns taking their classes out for recess on the blacktop. One class with just three students played hopscotch six feet apart.
“In this community there are a lot of multigenerational families, and there’s still concern about COVID,” said Principal Gretchen Young. “Our community has been hard hit because there are a lot of essential workers.
“As they start to feel it’s safe,” she added, “I suspect we’ll get more kids back.”
In San Francisco, people looking for a spot of grass to celebrate 4/20, the nationally recognized marijuana holiday, won’t be able to find any at Golden Gate Park, where the annual party has been canceled for the second year in a row.
Barriers have been erected around the park in anticipation of April 20, when throngs usually converge on its popular Hippie Hill.
“Although we’re in a better place in our fight against COVID-19 than we were last year, we are still not at the point where we can allow large, crowded events,” said San Francisco Mayor London Breed. “Please do your part to keep our community safe and celebrate from home. Anyone traveling to Golden Gate Park or Hippie Hill looking for a party will be disappointed.”
San Francisco Recreation and Park General Manager Phil Ginsburg had a sterner (if amusing) warning.
“Let me be blunt,” he said. “Hippie Hill will be completely inaccessible. Law enforcement will be patrolling the area. It will be a serious buzzkill.”
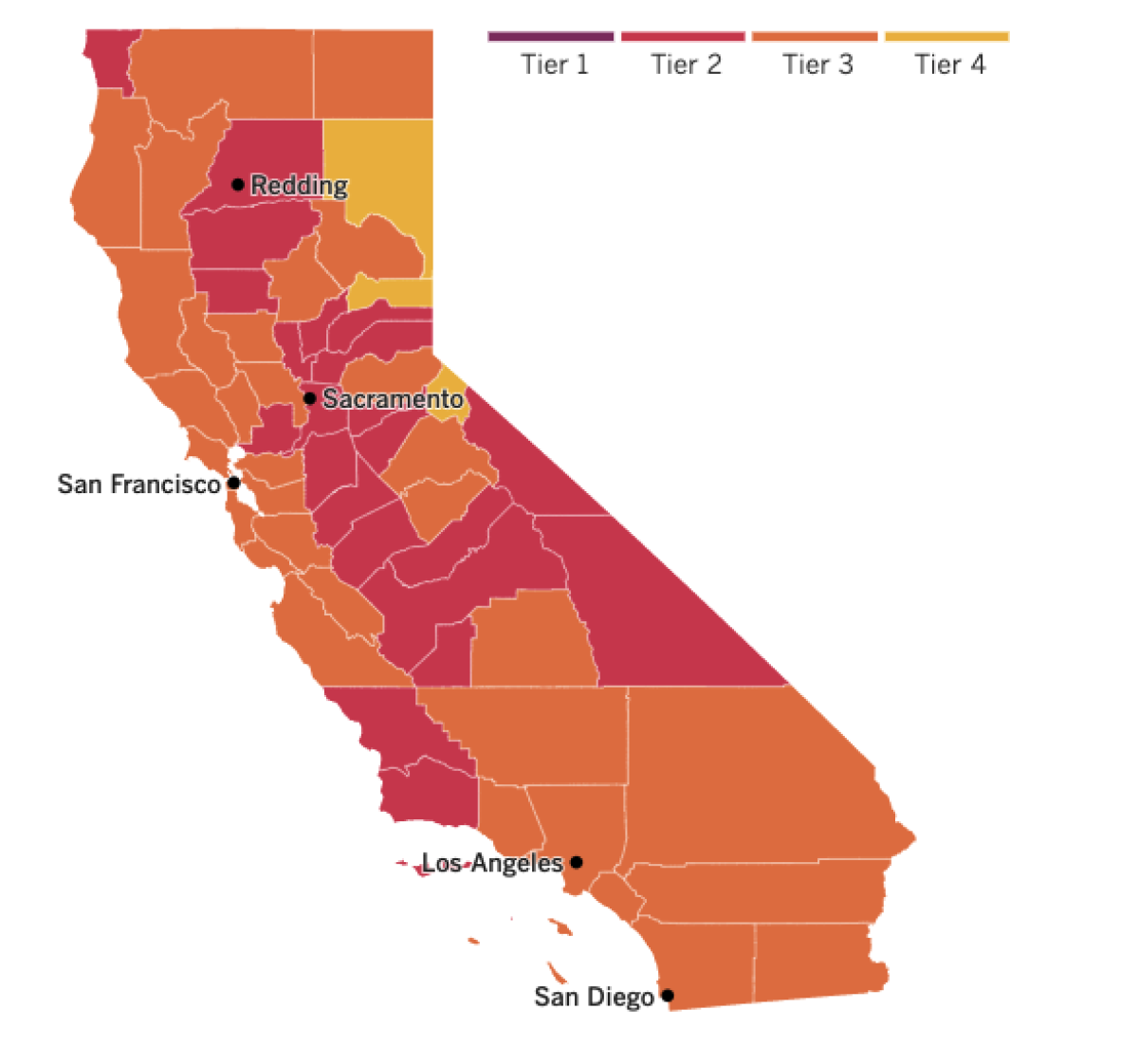
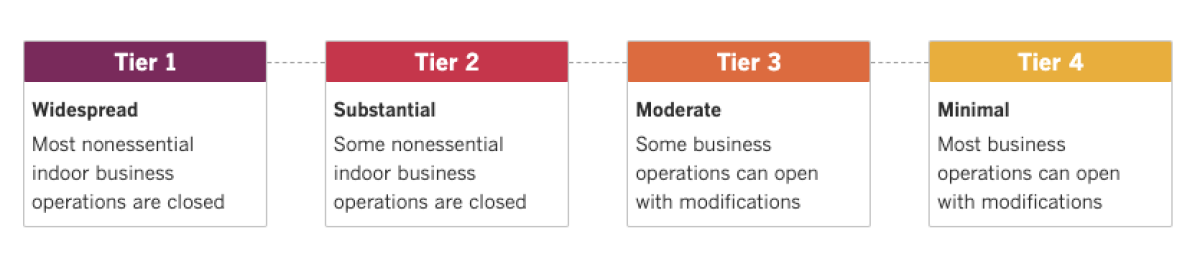
See the latest on California’s coronavirus closures and reopenings, and the metrics that inform them, with our tracker.
Consider subscribing to the Los Angeles Times
Your support helps us deliver the news that matters most. Become a subscriber.
Around the nation and the world
Congress has poured tens of billions of dollars into state and local public health departments in response to the pandemic, paying for masks, contact tracers and education campaigns to persuade people to get vaccinated.
Public health officials who have juggled bare-bones budgets for years are happy to have the additional money. Yet they worry it will soon dry up as the pandemic recedes, continuing a boom-and-bust funding cycle that has plagued the U.S. public health system for decades.
If budgets are slashed again, they warn, that could leave the nation where it was before the coronavirus: unprepared for a health crisis. “We need funds that we can depend on year after year,” said Dr. Mysheika W. Roberts, the health commissioner of Columbus, Ohio.
After the pandemic is over, public health officials say they worry they’ll be back to scraping together money from a patchwork of sources to provide basic services to their communities — much like what happened after the Sept. 11 attacks and again after the SARS and Ebola outbreaks.
“Something happens, we throw a ton of money at it, and then in a year or two we go back to our shrunken budgets and we can’t do the minimum things we have to do day in and day out, let alone be prepared for the next emergency,” said Chrissie Juliano, executive director of the Big Cities Health Coalition, which represents leaders of more than two dozen public health departments.
Other government officials are confronting another problem as businesses reopen and Americans start commuting to work: deadlier streets.
Last year, an estimated 42,000 people died in motor vehicle crashes and 4.8 million were injured. That represents an 8% increase over 2019, the largest year-over-year increase in nearly a century — even though the number of miles driven fell by 13%, according to the National Safety Council.
The COVID-19 pandemic caused roads to empty out, prompting more drivers to speed, leading to more fatalities, said Leah Shahum, executive director of the Vision Zero Network, a nonprofit group that works on reducing traffic deaths. Ironically, congested traffic, the bane of car commuters everywhere, had kept people safer before the pandemic, she said.
“This is a nationwide public health crisis,” said California Assemblywoman Laura Friedman, a Democrat from Glendale, who introduced a bill this year to reduce speed limits. “If we had 42,000 people dying every year in plane crashes, we would do a lot more about it, and yet we seem to have accepted this as collateral damage.”
In other news, some health experts say they fear the pause in the administration of the Johnson & Johnson vaccine in the U.S. could harm people in poorer nations the most.
More than a billion people around the world have been waiting for the J&J vaccine — a cheap, easy-to-transport, one-dose injection that reduces the risk from COVID-19.
But its global rollout was thrown into doubt last week when the U.S. Food and Drug Administration recommended that use of the vaccine be paused while scientists study a possible link to rare blood clots. The FDA has no authority outside the United States. But many countries follow its lead.
The fallout has begun in South Africa, where authorities also paused use of the vaccine, the only one available in the country. The country had already scrapped plans to use AstraZeneca’s vaccine, which like J&J’s is cheap and easy to transport but which tested poorly against the coronavirus variant that is dominant there.
Experts said that while the pause might make sense for the United States, where two other vaccines are widely available, stoppages in poorer countries with fewer options could wind up costing many more lives than they save.
“One of the dangers of this is how this is portrayed — that they somehow aren’t good enough for America but are good enough for the rest of the world,” said Dr. Jeremy Farrar, director of the Wellcome Trust, a British medical research charity.
Even if the FDA ultimately clears the J&J vaccine, the pause could harm the global effort by undermining general trust in COVID-19 vaccines.
“The only way to vaccinate the rest of the world in the next 12 months is through these adenovirus vaccines” like J&J’s and AstraZeneca’s, Farrar said.
Both those vaccines play a major role in Covax, a global collaboration to distribute vaccines fairly. Without them, the unchecked spread of disease in developing countries will make it more likely that new vaccine-resistant variants will emerge, Farrar said.
Your questions answered
Today’s question comes from readers who want to know: Will the pause in the administration of the J&J vaccine mean I’ll have to wait longer for a COVID-19 shot?
Probably not, since the pause will have little effect in L.A. County.
California officials decided out of an abundance of caution last week to stop administering the J&J vaccine while federal officials investigated reports of rare blood clots. But they say this will have little impact on vaccine administration locally. Only a small portion of the overall supply came from J&J.
The overwhelming majority of the vaccines that California has counted on have been made by either Pfizer-BioNTech or Moderna.
L.A. County said Monday it is actually expecting an uptick in vaccine supplies this week. The county’s latest allocation, pegged at approximately 362,000 doses, is up nearly 39,000 from last week, according to the Department of Public Health.
That number is only one piece of the local supply. Allocations sent directly from the federal government to qualified health centers and pharmacies are expected to swell the region’s total haul this week to more than 600,000 doses.
“At this pace, we’re on track to fully vaccinate 80% of the county population 16 and older by the end of June,” said Dr. Paul Simon, the department’s chief science officer.
Since the pause was announced, the county has been able to replace 70% of J&J doses with the other two vaccines, according to Public Health Director Barbara Ferrer.
“For those whose appointments were canceled last week, providers already did or will be in contact to reschedule your appointment as soon as possible,” she said Monday.
Appointments can be made online using the state’s My Turn system. A time slot can also be arranged by calling (833) 422-4255.
We want to hear from you. Email us your coronavirus questions, and we’ll do our best to answer them. Wondering if your question’s already been answered? Check out our archive here.
Resources
Need a vaccine? Keep in mind that supplies are limited, and getting one can be a challenge. Sign up for email updates, check your eligibility and, if you’re eligible, make an appointment where you live: City of Los Angeles | Los Angeles County | Kern County | Orange County | Riverside County | San Bernardino County | San Diego County | San Luis Obispo County | Santa Barbara County | Ventura County
Need more vaccine help? Talk to your healthcare provider. Call the state’s COVID-19 hotline at (833) 422-4255. And consult our county-by-county guides to getting vaccinated.
Practice social distancing using these tips, and wear a mask or two.
Watch for symptoms such as fever, cough, shortness of breath, chills, shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. Here’s what to look for and when.
Need to get tested? Here’s where you can in L.A. County and around California.
Americans are hurting in many ways. We have advice for helping kids cope, resources for people experiencing domestic abuse and a newsletter to help you make ends meet.
We’ve answered hundreds of readers’ questions. Explore them in our archive here.
For our most up-to-date coverage, visit our homepage and our Health section, get our breaking news alerts, and follow us on Twitter and Instagram.




