What happens if the coronavirus outbreak becomes a pandemic?

- Share via
Roughly 50 million people are under quarantine in China. Thousands of travelers are being screened at airports every day. Armies of disease detectives are knocking on doors around the world in hopes of halting the new coronavirus in its tracks.
Despite all the colossal efforts to contain the virus, scientists are quietly preparing for a grim — and increasingly likely — outcome: a full-blown global pandemic.
Since the novel virus was isolated in December in the Chinese mega-city of Wuhan, the pathogen has reached four continents and infected more than 24,000 people. At least 493 of them have died as a result. With the outbreak continuing to expand, authorities acknowledge that efforts will soon shift from trying to squelch the coronavirus to learning to live with it.
“We’re proceeding as if things go really sour on us in the coming weeks and months,” said Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases. “We’re working for the worst-case scenario.”

The World Health Organization raised the stakes last week by declaring a public health emergency of international concern. The Trump administration responded by proclaiming a public health emergency in the United States, restricting incoming flights from China and ordering the country’s first mandatory quarantine in more than 50 years.
Yet the outbreak shows no signs of slowing down.
Infectious disease experts at Imperial College London have calculated that each person infected with the virus early in the outbreak spread it to 2.6 others, on average. For the sake of comparison, in the early days of the 1918 Spanish flu outbreak, each person who became sick is thought to have infected 1.8 others.
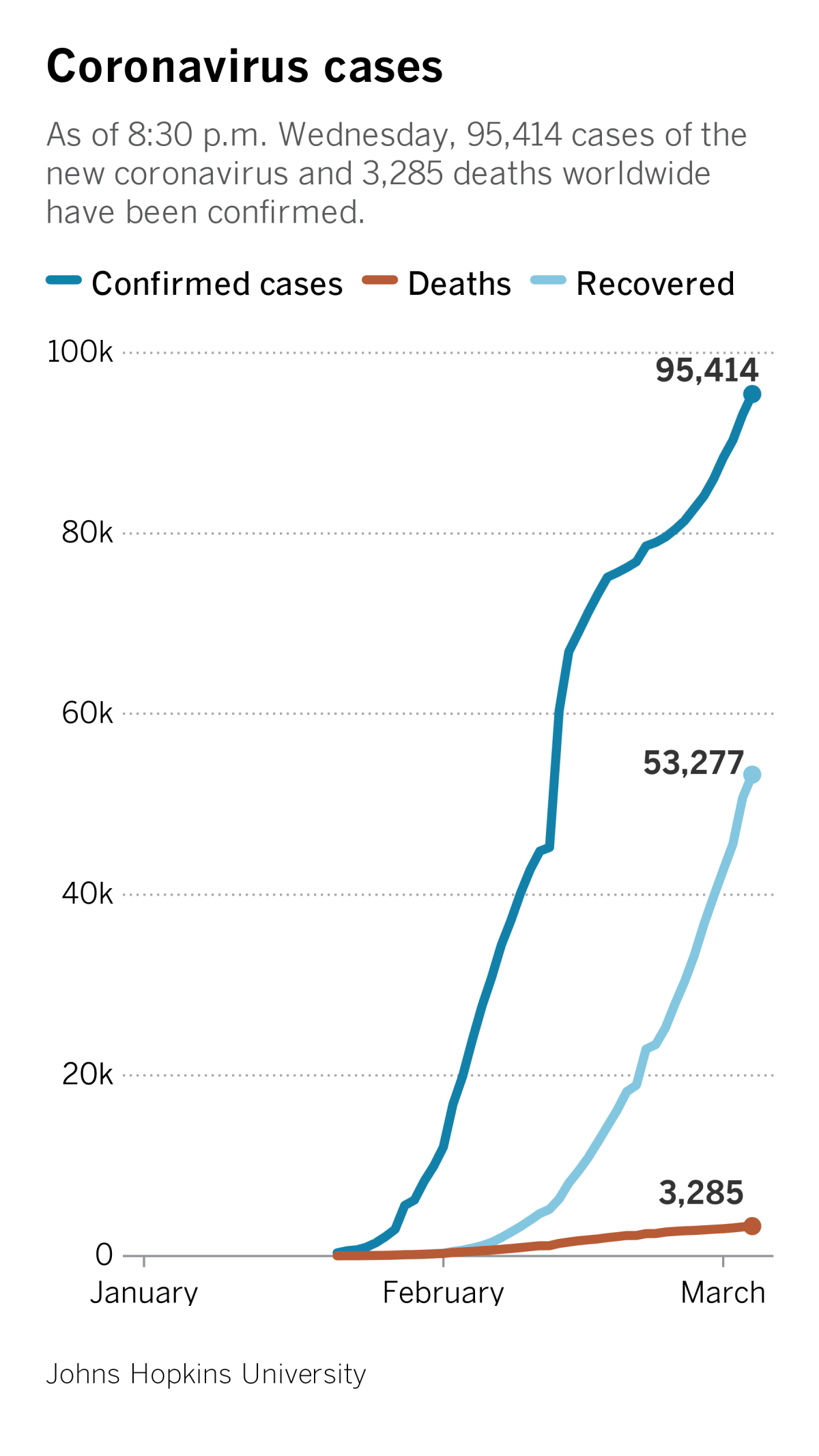
Lab-confirmed cases of coronavirus have increased more than 300-fold in the last three weeks. And while two-thirds of early cases were linked to a single market, that proportion quickly dropped, suggesting human-to-human transmission is widespread. Researchers believe individual epidemics are already self-sustaining in several major Chinese cities and could appear around the globe in regions where travelers from China arrived before showing any symptoms of illness.
“Containment is an increasingly remote possibility,” said Dr. Richard Hatchett, chief executive of the Coalition for Epidemic Preparedness Innovations, or CEPI, which is coordinating work on a vaccine for the strain known as 2019-nCoV. “This is not a China problem. It’s a global problem.”
And although the overwhelming majority of those infected so far have recovered, it’s certainly possible that the virus could become more dangerous.
“The nightmare scenario here is if it mutates into a highly pathogenic strain,” said Lawrence Gostin, director of the World Health Organization Collaborating Center on National and Global Health Law. “These kinds of viruses are very adaptable and can swap genes to become much more lethal. We can’t be complacent.”
Health officials aren’t waiting around to see if that will happen. Their preparations for sustained global spread of the coronavirus are already underway.
If the coronavirus outbreak in China were a Hollywood movie, now would be time to panic. But in real life, most Americans have no need, experts say.
For starters, doctors and epidemiologists will need reliable, rapid diagnostic tests that can distinguish between people who have influenza or pneumonia and those who are infected with the new virus. That would help ensure patients get the appropriate treatment and allow health officials to map the outbreak accurately.
The Centers for Disease Control and Prevention has already created a test based on the coronavirus genome shared by Chinese scientists and used it to confirm the 11 cases in the U.S., said Dr. Nancy Messonnier, director of the agency’s National Center for Immunization and Respiratory Diseases.
But in a pandemic scenario, that test won’t cut it. Doctors will need a faster, simpler tool that’s as easy to use as a pregnancy test or a rapid strep test. Otherwise they’ll struggle to keep up with the throngs of people who could turn up in emergency rooms and medical clinics with pneumonia-like symptoms. So far, no companies appear to be working on such a test for 2019-nCoV.
Doctors would also need easy access to medicines that can treat the novel coronavirus. Physicians on the front lines have been testing several antiviral drugs that are used for diseases such as HIV and Ebola, and researchers are tracking their effectiveness.
Scientists at Northwestern University are examining the protein structure of the coronavirus itself, looking for vulnerable places where existing drugs might be able to latch on and halt its replication inside human cells.
National Institutes of Health researchers will try to design monoclonal antibody drugs that can target the new virus, Fauci said. They’ll also test whether similar drugs developed to fight the SARS coronavirus have any potency against the new strain, he said.
A formal clinical trial would be necessary to establish a drug’s efficacy. That could take years, so in the meantime, doctors would probably fill the gap by sharing their successes and failures in meetings, conference calls and preliminary reports in medical journals.
Demand for a coronavirus vaccine would ratchet up if containment is no longer possible. But experts say that even on the fast track, it would take at least a year to develop one, manufacture it in large quantities, and distribute it around the world.
At the NIH’s Vaccine Research Center, scientists are working with biotechnology company Moderna Inc. to design a vaccine based on a protein found on the coronavirus’ surface. Fauci said a Phase 1 trial could begin within three months to see whether it elicits an immune response. “That would be rocket speed,” he said.
CEPI, based in Oslo, has asked its partners to take what they’ve learned creating vaccines for the Middle East respiratory syndrome coronavirus, known as MERS, and use it to fight the novel virus.
There are many things scientists really wish they knew about the coronavirus that has sickened thousands of people and caused at least 132 deaths.
Pharmaceutical innovations are only part of the story. Hospitals will need larger inventories of patient masks, protective suits for doctors and nurses, and spaces to quarantine patients suspected of being infected, according to a CDC checklist. They’ll also need to review their isolation protocols to prevent the virus from spreading to healthcare workers, other patients or visitors.
The emergency response arm of the Department of Health and Human Services is assessing the inventory of the Strategic National Stockpile, an $8-billion portfolio of drugs and medical supplies that can be tapped in the event of a severe crisis. The stockpile is housed in warehouses across the country — their exact locations and contents are kept confidential for national security reasons — and it’s continuously refreshed as products expire and equipment goes out of date.
If the pandemic threshold is crossed, the World Health Organization would need to begin operating as — or enlist — a logistics company to coordinate a global stockpile system. Dozens of countries would all need the same medicines and equipment at the same time, and that increase in demand could quickly outpace the available supply. Under such circumstances, ensuring that resources make their way from wealthy countries to vulnerable ones is a major challenge.
Another arena in which global officials will undoubtedly spar: international travel and trade. When the WHO declared a global health emergency, officials emphasized that there was no cause for placing limits on either.
Groups such as the International Air Transport Assn. and the World Trade Organization are currently examining how best to halt the virus’ spread while avoiding “unnecessary restrictions on international traffic” that could snarl supply chains and bring factory production lines to a screeching halt.
“It would be one thing to suffer through a pandemic, but another to deal with potential shortages and major economic fallout coming from prolonged trade interruptions,” said Dr. Tom Inglesby, director of the Center for Health Security at the Johns Hopkins Bloomberg School of Public Health. “That would inadvertently hurt ourselves further.”









