Experimental decoy drug tricks coronavirus, then destroys it
- Share via
The coronavirus has been a shifty foe, with new variants and subvariants rapidly evolving to evade vaccines and treatments. Researchers at Boston’s Dana-Farber Cancer Institute are working on an experimental drug that takes one of the virus’ most dangerous traits — its talent for mutation — and turns it back on itself.
When the coronavirus binds to a specific type of receptor on the surface of a cell, it drives its spike protein in like a switchblade and initiates an infection.
The drug is designed to mimic that receptor, working like an assassin in an attractive disguise. When the coronavirus attempts to bind to it instead of to the real thing, it destroys the structure of the spike protein, permanently disabling the mechanism that would make that switchblade, according to a report published Wednesday in the journal Science Advances.
This approach backs the coronavirus into a corner: If it adopts a mutation that makes it bind less effectively with the decoy drug, it will also bind less effectively to the human cell.
The virus has found ways around antibody treatments by evolving new versions of its spike protein. But to get around this decoy, it would have to seek out and bind with a completely different receptor — a highly unlikely possibility “that would involve super-drastic changes” to the virus, said Gordon Freeman, an immunologist at Dana-Farber and Harvard Medical School and the study’s senior author.
“We’re not trying to fight evolution,” added Dr. James Torchia, a clinical fellow at Dana-Farber and Harvard Medical School and the paper’s lead author. “We’re trying to design this drug in a way that it harnesses evolution.”
The Biden administration is boosting efforts to identify and track coronavirus variants to help scientists see where the pandemic is heading next.
The receptor in question is called angiotensin-converting enzyme 2, or ACE2, and the drug is an ACE2 receptor decoy. Known at this stage as DF-COV-01, it has so far been tested only on animals.
In those experiments, coronavirus-infected hamsters that did not receive the treatment lost roughly 10% of their body weight — a measure of the severity of their infection — in the first five days. By contrast, infected hamsters that received the drug lost less weight and gained it back more quickly. The treated hamsters also had lower viral loads in their lungs.
Several research teams have pursued a strategy of fielding decoys to disrupt infection by the SARS-CoV-2 virus, said Jun Wang, a medicinal chemistry professor at Rutgers University. But while “the idea is simple,” he said, “the devil is in the details,” and none have yet come to fruition as a COVID-19 therapy.
Decoys can’t be packaged as pills that a patient could use at home because they are proteins and won’t survive a trip through the GI tract. Instead, they would need to be administered either by injection or intravenously.
That said, “this paper has made a lot of progress” in advancing the prospects for such a therapy’s use, Wang said. The researchers made changes to the decoy molecule so it can survive for as long 52 hours inside a mouse’s body. If the same were true in humans, it could mean the experimental therapy would need to be administered every two days rather than daily.
From a patient’s perspective, “this is a big plus,” he said.
But it’s not clear yet if the improvements seen in the hamsters will translate to humans.
“I was excited when I first read the paper,” said Dr. Paul Insel, a pharmacologist at UC San Diego who raised the possibility of ACE2 decoys as potential COVID treatments early in the pandemic. But then he became “crestfallen when I actually looked at the results.”
“As much as there’s a lot of elegant science in this paper,” he added, “it’s not really biologically significant.”
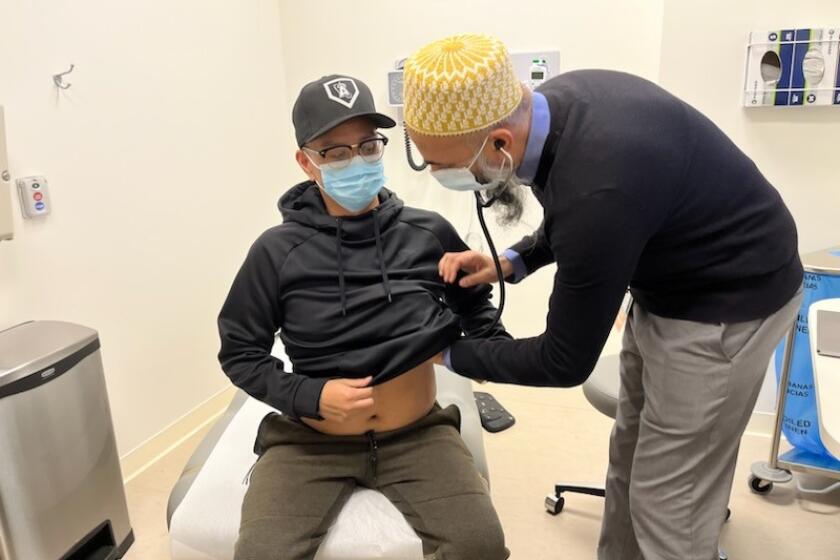
When everyone around them stops taking pandemic precautions, it gets harder for immunocompromised Americans to protect themselves against COVID.
The study authors acknowledged that the reduction in viral load was modest. But they pointed out that their results are similar to those seen in animal studies of antibody drugs that went on to be successful in humans.
That “bodes well for its likelihood of achieving a similar therapeutic effect in humans but with the added benefit of lasting efficacy in the context of a constantly changing virus,” they wrote.
The appeal of the decoy approach has grown as the coronavirus exploited its penchant for mutation. Across the pandemic, the virus has undergone prolific changes, especially in the structure of the spike protein it uses to break into a cell and infect its victims.
But while the virus has changed, the homing beacon it looks for in human cells — the ACE2 receptor — has not. That means the experimental drug ought to work equally well no matter how the coronavirus mutates, and the study suggests it does, Wang said.
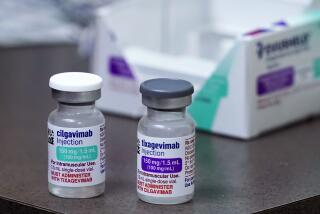
The virus’ shape-shifting ways have ratcheted up the need for a more resilient treatment. The BQ.1 and BQ.1.1 subvariants, which account for nearly two-thirds of the coronavirus specimens now circulating in the U.S., are resistant to all monoclonal antibody treatments currently available. In earlier stages of the pandemic, those medications were vital to unvaccinated patients and to immunocompromised patients who do not produce enough antibodies in response to vaccinations to protect them from serious illness.
Scientists searching for a medicine to treat patients with COVID-19 are looking for it in the blood of people who have already survived the disease.
Cancer researchers have been most active in developing decoy therapies, said Dr. Timothy J. Cardozo, a professor of biochemistry and molecular pharmacology at NYU’s Grossman School of Medicine. Their aim has been to trick cancer-promoting growth molecules to bind with decoys, thereby blocking the signals that fuel uncontrolled growth of malignant cells.
That research has produced a host of useful drugs, mostly to tamp down inflammation in autoimmune diseases, Cardozo said. He called the use of decoys to block viruses “fairly new” and said the researchers’ focus on the ACE2 receptor makes it a “promising” way to block or limit a runaway infection.
But Cardozo warned that since ACE2 receptors appear in many different tissues and play a variety of signaling roles, researchers will need to proceed with care. The ACE2’s natural function is to modulate blood pressure, and Torchia altered the decoy version precisely so that it wouldn’t influence blood pressure, a common concern with this kind of protein-based drug.
The team is currently working on the preclinical studies that are necessary to begin human trials in 2023, Torchia said.
ACE2 is the target site for many other coronaviruses found in humans and — crucially — nonhuman mammal hosts. If the ACE2 decoy approach works, it could serve as a ready form of treatment against any other coronaviruses that make the jump across species, Torchia said.
“This cross species viral transmission ... may increase over time as changes in climate and land use continue globally,” he said. “We really want to be much more prepared for going forward.”