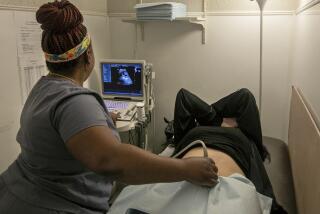
Simple prenatal genetic tests may lead to healthier babies -- and more abortions
- Share via
If reproductive technologies like in vitro fertilization and pre-implantation genetic diagnosis give you the heebie-jeebies, Booster Shots is sorry to inform you that things are about to get a lot more complicated.
In just the past month, researchers have made great strides in their ability to analyze the DNA of a fetus by collecting it from a sample of maternal blood. A study last week in the British Medical Journal reported on a simple blood test that was able to determine whether a fetus had Down syndrome; a few weeks earlier, reports in Science Translational Medicine and Nature Precedings demonstrated the technical ability to analyze thousands of genetic markers with as little as 10 milliliters of blood.
These tests are already possible, and sooner or later they’ll become inexpensive and easily accessible. It’s time to start preparing ourselves for the medical and social ramifications of this burgeoning technology, known as non-invasive prenatal genetic diagnosis, or NIPD for short.
So warns Hank Greely, director of the Center for Law and the Biosciences at Stanford Law School. Writing this week in Nature, he assures us the tests are likely to become commercially available within the next five years. If they are as popular as other non-invasive prenatal screening tests (think blood tests to identify neural tube defects), Greely estimates that the number of fetal genetic tests annually in the United States will jump from the current 100,000 to about 3 million.
RELATED: Prenatal blood test for Down syndrome shows high level of accuracy
That will give a whole lot of expectant parents a whole lot more to think about. Not only will they be able to learn whether their children have a chromosomal abnormality like Down syndrome or a single-gene disease like cystic fibrosis or Tay-Sachs disease, they can also find out whether they are boys or girls and whether their eyes are blue or brown. In the not-too-distant future, the genetic tests may even be able to provide clues about a fetus’ athletic or academic potential.
Greely is understandably concerned about how some couples might use that information. It will almost certainly lead to more abortions. In China and India, for instance, greater access to inexpensive ultrasound testing has produced a “dramatic skewing of live-birth sex ratios,” Greely writes. Prenatal paternity testing could also result in more pregnancy terminations.
And then there’s the concern that NIPD will “prevent the birth of people with particular disabilities.” That could send a damaging message to people who have those disabilities. It could also have the practical consequence of reducing the amount of money devoted to researching and treating the condition.
And while we’re on the issue of money, Greely asks, “Who will pay for millions of genetic tests, and for the abortions that follow?” The degree to which they become accepted by the medical establishment may hinge on whether they’re seen as “a way to save money by avoiding the births of high-cost children.”
One thing is for sure, he concludes:
“Whether we view NIPD gladly as a way to reduce human suffering, warily as a step towards a eugenic dystopia, or as a mix of both, we should agree that the better we prepare, the more likely we are to avoid the worst misuses of this potentially transformative technology.”
The essay is behind Nature’s pay wall, but a short summary and a link are available here.
RELATED: Direct-to-consumer genetic tests coming soon to a drug store near you
More to Read
Sign up for The Wild
We’ll help you find the best places to hike, bike and run, as well as the perfect silent spots for meditation and yoga.
You may occasionally receive promotional content from the Los Angeles Times.