He was symptom-free. But the coronavirus stayed in his body for 40 days

- Share via
SINGAPORE — By his second day in the hospital with COVID-19, Charles Pignal’s mild cough and 102-degree fever had disappeared. Bored and “bouncing off the walls” of his room in the isolation ward at Singapore’s National Center for Infectious Diseases, he felt like he could go out and play a set of tennis.
The 42-year-old footwear executive told his mother on the phone, “I’ll be out of here in a couple of days.”
But Pignal would test positive for the coronavirus for five more weeks, despite developing no further symptoms. He wasn’t released until the 40th day after he first fell ill, when he finally tested negative two days in a row.
Cases like his are coming under increasing scrutiny as medical researchers worldwide puzzle over why the coronavirus — which typically lasts about two to three weeks in the body — appears to endure longer in some patients, even relatively young, healthy ones.
With studies showing that asymptomatic patients can transmit the SARS-CoV-2 virus, understanding how the virus leaves the body is among the most urgent mysteries facing researchers as governments in the United States and across the world begin to reopen their economies.
It marks a perilous time in the evolution of a virus that has killed more than 210,000 people. As restrictions on daily life begin to ease, people who don’t know they are carrying the virus could unwittingly infect others. Patients who have recovered could have the virus in their systems weeks or months later.
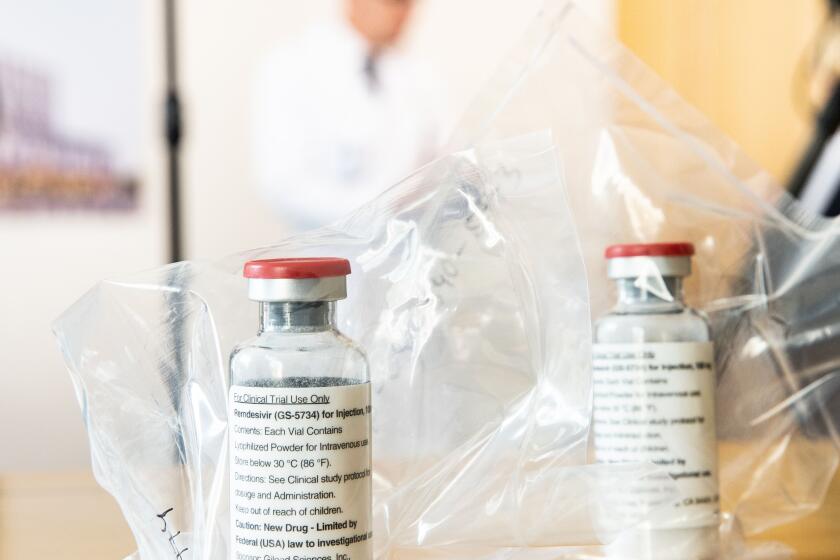
In a clinical trial, the drug remdesivir shortened recovery time for patients with advanced cases of COVID-19, the disease caused by the coronavirus.
Although studies show that the average recovery time from COVID-19 is two weeks, and nearly all patients are virus-free within a month, “less than 1% to 2%, for reasons that we do not know, continue to shed virus after that,” said Hsu Li Yang, a physician specializing in infectious diseases at the Saw Swee Hock School of Public Health at the National University of Singapore.
In recent weeks, China and South Korea have reported that some patients who had recovered from COVID-19 tested positive again in follow-up visits. In extreme cases, patients in the Chinese city of Wuhan, where the outbreak began late last year, reportedly tested positive 70 days after recovery.
Doctors in both countries said they didn’t believe the patients had been reinfected, a worrisome possibility because of its implications for building widespread immunity to a disease for which there is no vaccine. They also had no evidence that the patients had infected others.
South Korean doctors have played down the results, saying that their standard genetic tests are designed to detect even small quantities of the virus and don’t always distinguish between dead fragments of the virus and particles that are still infectious. Patients who were diagnosed as recovered could still have had fragments of SARS-CoV-2 in their system.
“Many of the so-called relapsed cases in South Korea probably reflect this phenomenon,” Hsu said.
Can you get the coronavirus twice? Scientists say it’s highly unlikely, but China is tightening hospital discharge standards as “recovered” patients in multiple provinces appear to get sick again.
Studies indicate that COVID-19 patients are most infectious at the start of the illness, when their viral load is highest, but researchers don’t yet know whether people who shed the virus for several weeks remain contagious until the end.
One study from Hong Kong found the virus’ nucleic acid in the saliva of a patient whose symptoms had appeared 25 days earlier. A Southern California man who was infected aboard the Diamond Princess cruise ship took 29 days to test negative despite showing almost no symptoms.
“If these people can continue to transmit the virus, that in part could fuel this pandemic,” said Lokesh Kumar Sharma, an instructor at the Yale School of Medicine.
In a study last month of 16 patients from Beijing who had mild infections, half of the patients continued to shed the virus even after their fevers, coughs and other symptoms went away. The study’s authors, including Sharma, said the results were a reminder that recovered patients needed to be treated “as carefully as symptomatic patients.”
That poses a challenge for health systems dealing with growing epidemics.
In Singapore, coronavirus infections have swelled from 1,000 at the start of April to more than 15,000 because of a giant outbreak among low-wage foreign workers. Authorities in the city-state are racing to expand temporary isolation facilities at hotels and convention centers for patients with mild symptoms so that hospital beds can be reserved for more serious cases.
New infections among Singapore’s migrant workers offer a stark illustration of the risks to marginalized groups in densely inhabited parts of Asia.
As of Wednesday, at least 200 patients remained in hospitals or isolation facilities more than a month after admission.
Pignal, a Frenchman who first developed symptoms while flying from London to his home in Singapore in early March, asked a doctor around his 15th day in the hospital whether he was still infectious even though he felt perfectly healthy.
“He said we don’t know, but there’s no evidence that what you’re shedding is contagious,” Pignal said.
Yet the daily nasal swabs continued to show the virus was in his system. A negative test on Day 23 was nullified by a positive result the next day.
He passed the time by reading and posting videos to his Instagram account, where he normally reviews books but suddenly found himself discussing his illness and confinement with thousands of new followers.
“I feel absolutely great,” he said in one post. “It’s just that the virus is still positive, right here in my nose. It’s not going anywhere…. I could be here another day, another week, another two weeks — nobody knows. So that’s really quite distressing.”
Then, told that beds in the isolation ward were scarce and that he was considered low risk, Pignal was moved to a hotel where he shared a room with another infected person.
But no doctors or nurses were there, tests were administered only every four days, and Pignal began to grow distressed as he entered his second month of confinement. The spartan decor and security guards roaming the grounds added to his sense of isolation.
“Frankly,” he said in a post on Day 27, “I’m starting to get a little bit scared.”
His fiancee put together a lip-sync video featuring friends and family to cheer him up. He plowed through “The Brothers Karamazov.”
On April 11, Day 39, he was told he had tested negative and was administered a second test to confirm the result. The next morning brought relief: negative again. He was virus-free and sent home.
Three weeks later, he remains healthy.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.