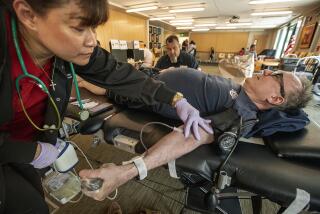
Editorial: Time to ease rule on blood donations from gay men
- Share via
A 1980s-era ban on blood donations by most gay men is out of step with current science, which has developed faster and more accurate tests for HIV-infected blood. An advisory panel to the U.S. Food and Drug Administration, which is considering the blood donation rules Wednesday, should recommend loosening them to reflect actual risks rather than outdated fears.
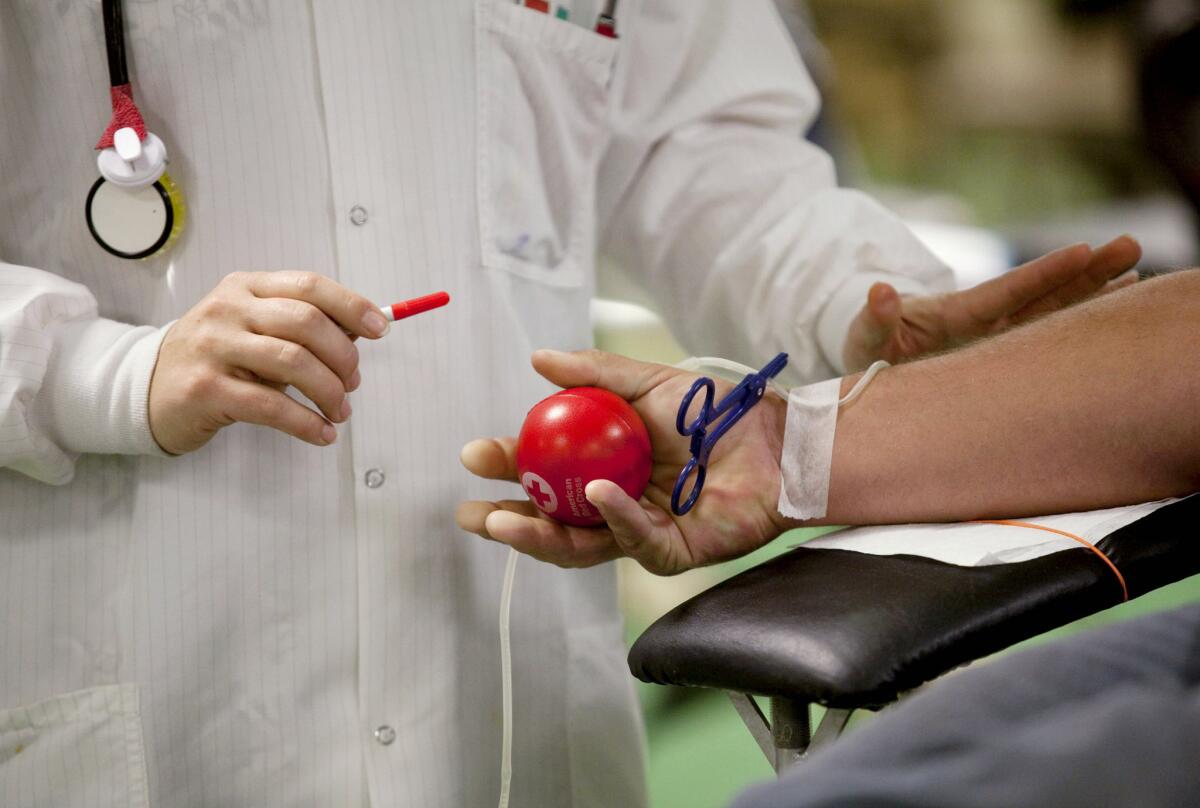
For most people, donating blood is easy. Squeeze a stress ball, suck on a lollipop, move on with the day. But for gay men, the ability to provide this tangible good has become a struggle against stigma. In 1983, the FDA indefinitely deferred donations from any male donor who had had sex with another man at any time since 1977. The ban was justifiable during the early years of the AIDS crisis, when thousands of people each year unknowingly contracted HIV, the virus that causes AIDS, from blood transfusions. The disease was particularly rampant among gay men, and there was no adequate way to test blood for HIV.
Since then, science has made immense strides in blood-screening technology. In August, the FDA approved the first rapid test to detect both the antigen and antibodies for HIV. By pairing this test with another, blood banks can now detect HIV with near certainty if it has been at least 10 days since the donor became infected. The HIV risk from a unit of blood is about 1 in 2 million in the U.S., almost exclusively from blood donated during that “window period.” Several other countries, including Japan and Sweden, have loosened their restrictions to cover only gay men who have been sexually active within the last year. Australia did the same thing in 2000, before the better tests were available, and still found, 13 years later, that there was no evidence of an increase in transfusion-related HIV infections. At minimum, the FDA should relax its restriction to a one-year span, which would put gay men under the same rules as people who have had heterosexual sex with an intravenous drug user or prostitute.
Even that is probably more restrictive than necessary. Gay men in long-term monogamous relationships, married or otherwise, have no higher risk of infection than heterosexual married men. And the safety of all donated blood depends on the honesty of the donor — as well as the laboratory screening that all blood undergoes. In August, when the American Medical Assn. deemed the ban “discriminatory and not based on sound science,” it recommended that the FDA evaluate gay men based on individual risk factors, as Italy does, rather than grouping them all into a high-risk category. Either way, at this point, continuing the 1977 rule would serve only to perpetuate discrimination against gay men, because it clearly no longer serves the necessary purpose of protecting the nation’s blood supply.
Follow the Opinion section on Twitter @latimesopinion
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.