You’re a parent with COVID-19. Your partner is also sick. What do you do?
- Share via
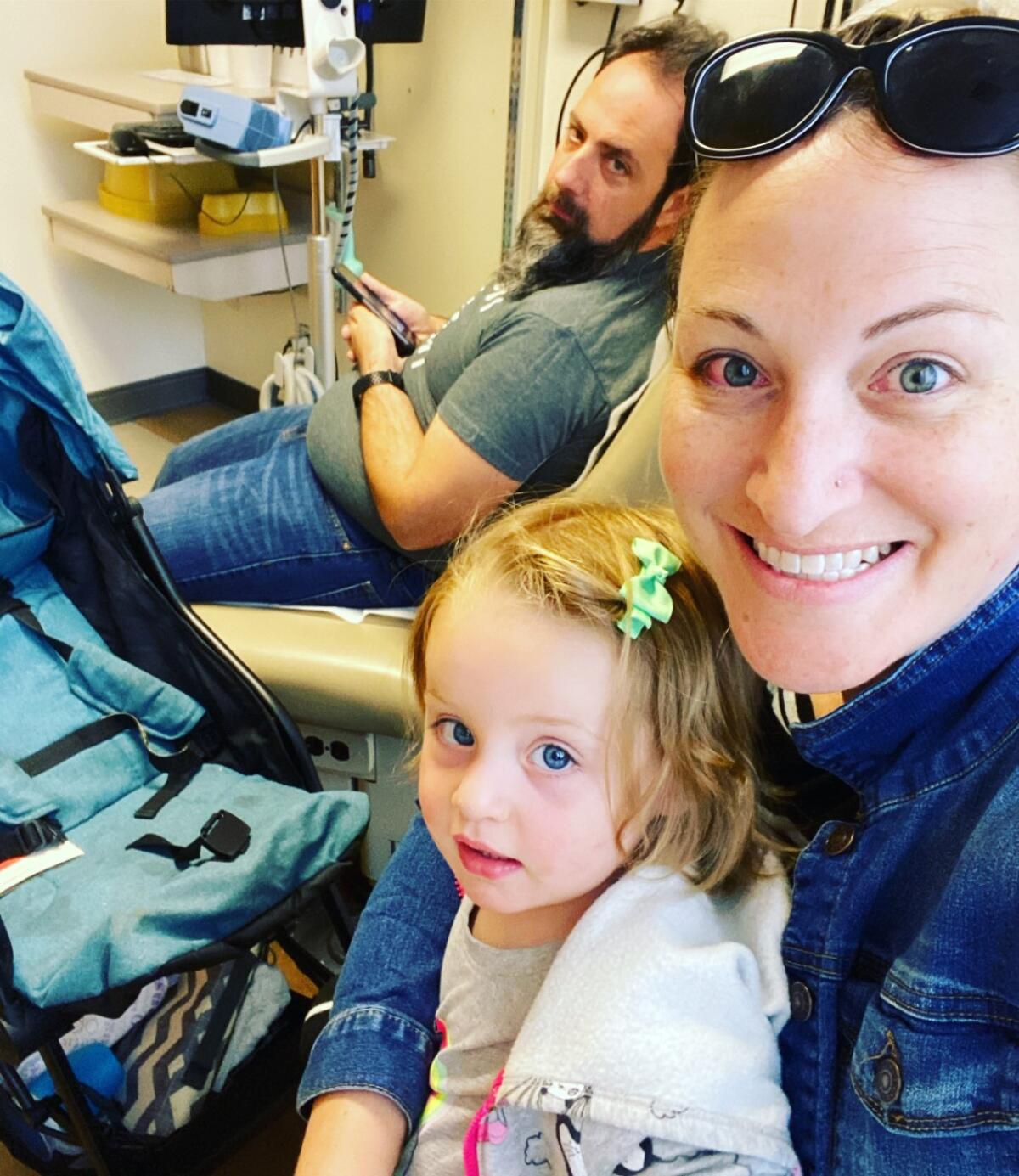
Michael Yeates came home from work one afternoon in early March to pick up his 21-month-old daughter, Zoe, for swim lessons. His wife was sick, and in the few hours he’d been gone, she’d gotten much worse.
Yeates was coming down with something, too — a cold, he thought — but at that moment he was focused on getting his wife help. From their home in Corona, they called their medical provider’s nurse help line.
Yeates’ wife described her symptoms: shortness of breath, dry cough, fever, body aches, intense fatigue. She explained that she’s a labor and delivery nurse at a major hospital in Los Angeles. She had already tested positive for the flu that season.
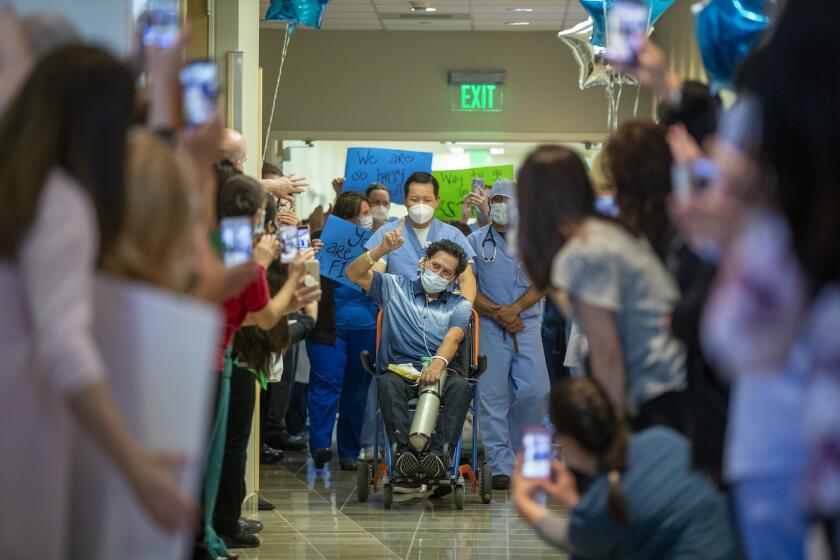
These are some of the unusual new scenes across the Southland during the coronavirus outbreak.
The nurse on the other end of the line was blunt: Testing wasn’t available, but it was likely that Yeates’ wife had contracted the coronavirus.
Yeates’ wife did not want to be identified by name for fear of the stigma associated with continuing to work as a healthcare provider after recovering from COVID-19.
With that tentative diagnosis, the Yeates family faced a dilemma that haunts parents around the world in these uncertain days of the coronavirus outbreak: What will happen if we’re too sick to take care of our child?
A single mother who has contracted the virus, and probably passed it to her child, cannot turn to family or friends during a pandemic without putting them in harm’s way. She cannot drop her child off at day care. Two-parent families, many accustomed to the reliable support that a partnership provides, face the same grim possibility.
And even though there will be thousands, maybe millions, of other parents in the same dire position, there are no easy solutions.
In our effort to cover this pandemic as thoroughly as possible, we’d like to hear from the loved ones of people who have died from the coronavirus.
New York Times correspondent Dana Goldstein, who battled COVID-19 along with her husband and young daughter, put it this way in a Twitter thread: “This virus turns every household into an island.”
That was certainly true for the Yeateses.
They were young, both 36 and healthy, and leaned on the belief that things would stay that way. But within a few days, Michael Yeates fell increasingly ill. When he stood, his limbs seized with pain. He felt as if his skull was being clamped by a trash compactor. Each breath was like trying to draw water from a dry well.
“It felt like there was nothing there in my chest,” he said.
All the while, the couple avoided confronting the possibility that if both of them suddenly took a turn for the worse, it would be incredibly difficult, if not impossible, to look after Zoe.
“We talked about the fact that we had no plan,” Yeates said, “and could not conceive of a plan.”
Yeates went to an urgent care clinic when his breathing became dangerously labored. He was given a shot of prednisone to treat his inflamed lungs. Within the hour, a paper mask given to him by a nurse was damp and torn from the force of his constant coughing.
The day after, Yeates drifted in and out of consciousness. Meanwhile, his wife was still recovering — she would wrestle with a sore throat and fatigue for weeks — but she had to care for little Zoe. Over the next few days, Yeates and his wife, who usually went to bed around 11 p.m., would crash right after Zoe went to bed at 7 p.m. They napped while she napped.
Yeates’ wife returned to work when her symptoms subsided, and Yeates was alone with Zoe. He could barely get off the couch. He counted the steps to the kitchen: 20. He gave Zoe food that didn’t require preparation, snacks usually reserved for road trips.
Yeates put the toddler in the backyard with her toys and “let her go wild.” He gave her paints and paper. “If it meant she wasn’t crying, she was allowed to do it,” Yeates said. She tore the house apart.
Zoe, accustomed to receiving lots of attention from her dad, whined and tugged on Yeates’ beard.
“I was being distant, but I couldn’t help it,” Yeates recalled. “I cried a few times. I felt like I was failing.”
The Yeateses usually depend on their parents, who live nearby, for child care. But his mom and his mother-in-law are in the high-risk category — older than 65 and with underlying health conditions. The Yeateses knew Zoe could be an asymptomatic carrier of the virus. And they couldn’t pinpoint anyone else — healthy or not — whom they would be willing to potentially endanger.
“We chose not to think about it,” Yeates said. “What the hell are you going to do?”
Cullin and Audrey Wible, parents to three young children in the small New Jersey town of Oceanport, faced this dilemma in late March. Both had presumptive cases of COVID-19 but, like the Yeateses, were unable to get tested.
Coronavirus testing is an essential part of slowing the spread. From swab to result, follow along with one very sick patient’s test.
Cullin, 41, got sick first. He had a 103-degree fever for three days.
“I had aches and pains in places where I’ve never hurt before — the joints of my toes, my kidneys,” said Cullin, a construction executive. He fluctuated between shivering and profuse sweating as he lay in bed under several layers of blankets.
Cullin’s mind raced: “What would we do if both of us got really sick? What if we both developed respiratory symptoms?”
His parents in New Hampshire volunteered to drive down and watch the kids if worst came to worst. “No, that’s crazy,” he told them. His mom is a cancer survivor in her 60s. Audrey’s parents in Ohio were also out of the question.
“We really never concluded what we would do,” Cullin said.
Audrey, 37, had a relatively mild case and didn’t feel truly sick until it was clear Cullin was turning a corner. She chalks this up to her body knowing that she needed to be there for her kids.
“I seem to hold on for as long as I possibly can, and then when it’s OK for me to fall apart, that’s what I do,” said Audrey, who is in remission from Crohn’s disease.
Cullin felt like his family had dodged a bullet.
“I’ll be honest, it’s hard to think about,” Cullin said, choking up.
The Wibles know that inevitably, others in their community will find themselves in a similar bind but might not be as lucky. They told their church leaders that they’re able to help those in need, assuming that they have gained immunity, even if it’s temporary.
“We’re open to watching other people’s kids,” Cullin said. “This is how we need to operate now.”
Peter Arcese, a father of three in Brooklyn, began to seriously ponder this issue when his wife, Angela, began experiencing severe COVID-19 symptoms.

Arcese, a trusts and estates lawyer, has helped many clients set up “standby guardianships,” a legal tool developed during the AIDS crisis that ensures the care of minor children if parents become incapacitated. But that safeguard wasn’t built with a pandemic of this sort in mind, he said. HIV, which causes AIDS, can be transmitted only through sex, blood or breast milk, so there was no danger to people taking in the child of someone with the disease.
As Angela’s sore throat progressed to chest aches and ragged breathing, Arcese realized that their standby guardians were all in high-risk segments of the population.
“This goes beyond a problem that law can solve,” Arcese said.
As he feared what would happen if he, too, got sick, the 55-year-old imagined communities building mutual aid networks — run by churches and nonprofits — that could help fill the child-care void. The network would be manned primarily by those who have already been sickened by the virus.
“I expect enough people will develop antibodies and volunteers will come forward,” Arcese said.
He couldn’t think of any other solution.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.