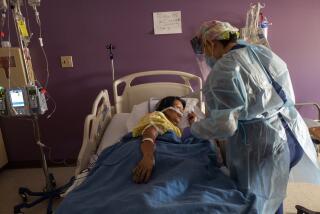Nursing home patients moved after over a dozen workers skip shifts amid pandemic

- Share via
Nearly 100 residents are being removed from a skilled nursing facility in Riverside County after more than a dozen employees missed two consecutive days of work, according to county officials.
The 83 patients at the Magnolia Rehabilitation and Nursing Center were being moved Wednesday to other locations throughout the county. Some were being discharged to be with their families depending on their needs, said Brooke Federico, Riverside County public information officer.
For the record:
6:47 p.m. April 9, 2020A previous version of this story said that 84 patients the Magnolia Rehabilitation and Nursing Center had been moved. On Thursday, healthcare officials said the number was lowered to 83.
The Riverside University Health System and Kaiser Permanente sent 33 licensed vocational nurses and registered nurses to care for the residents at the facility when 13 employees didn’t show up for work Tuesday and Wednesday, Federico said. But the patients had to be moved right away due to staffing demands.
“The team that we were able to send from the county [was] not the long-term solution,” she said. The patients need to be moved “to other facilities that have permanent staff in place to care for residents.”
Late Monday evening, officials reported 34 positive cases of COVID-19, the disease caused by the coronavirus, among patients and five among employees at the Magnolia Rehabilitation and Nursing Center, Federico said. The five employees — who were not among the 13 who didn’t go to work — were sent home to self-quarantine, and the patients who tested positive were isolated from other residents.
As of Wednesday, there were no pending test results for the 90-plus-bed facility.
The nursing facilities that will receive the patients will undergo standard coronavirus containment measures, which include closing enrollment to new patients, prohibiting staff from working at other facilities, isolating sick patients and closely monitoring all patients and employees. All employees will use personal protective equipment, officials said.
Federico said the county had fulfilled — either in part or whole — equipment requests from hospitals and skilled nursing facilities. Officials are working to get more equipment from their federal partners.
“The congregate living facilities do pose a greater risk for COVID-19,” Federico said, “because they are groups of people [living] together, and also, unfortunately, people who are at skilled nursing facilities are in a more vulnerable population because they are older and have underlying health conditions.”
Family members can call (951) 358-5134 to check the status of their loved ones.
As of Tuesday evening in Riverside County, there were 1,016 confirmed COVID-19 cases, 28 deaths and 67 recoveries. Of these cases, 186 people 65 or older were among those who tested positive, according to county records. Riverside County has the fourth-largest case count in the state, said Dr. Cameron Kaiser, the county’s public health officer.
More than 100 local nursing homes and communal living facilities have seen coronavirus cases. Pulling out residents is advisable, county leader says.
The Magnolia Rehabilitation and Nursing Center’s virus outbreak came just a few days after 30 patients and some staff members at the Extended Care Hospital of Riverside — less than 150 feet away from the Magnolia center — tested positive for coronavirus infection.
“With three nursing facilities in the midst of testing and five more reports that we are investigating, it is my belief that the surge will come from the skilled nursing facilities and long-term-care facilities where our most vulnerable patients already reside,” Kaiser said at a Riverside County Board of Supervisors meeting Tuesday. The surge, he said, will be then pushed on to hospitals, with infections mounting in those environments.
“We are trying to test as many facilities as we can,” he said, “but at some point we will not have enough tests to do so.”
As of Tuesday, officials estimated that more than 10,000 coronavirus tests had been performed in the county.
Kaiser said the “best move now is to reduce complications and hospitalizations where we can and support our hospitals in those situations where these individuals must move to higher levels of care.” He also said he was considering placing an order barring healthcare workers from working at multiple facilities but wanted to make sure he didn’t restrict access for critical employees.
Kim Saruwatari, Riverside County public health director, said the county was working with its federal partners to increase testing capacity, obtain more beds in non-traditional settings to treat patients, and have health leaders teach hospitals ways to maximize their equipment
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.