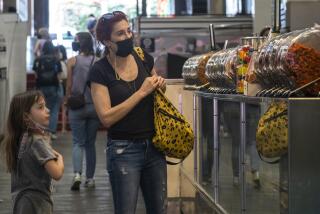Coronavirus ravages poorer L.A. communities while slowing in wealthier ones, data show

- Share via
A major shift was already underway last month as coronavirus deaths were rising across Los Angeles County and officials were trying desperately to prevent a surge in cases.
In mid-April, while officials urged people to stay home, limit shopping trips and wear masks, infection rates in poor communities for the first time overtook wealthy ones, a Times analysis of county health data shows.
Confirmed cases per capita diverged on April 17 and the gap has kept growing since. The analysis found the virus is increasingly ravaging predominantly black and Latino neighborhoods with higher poverty levels, while wealthier, majority-white enclaves that initially reported some of the highest infection rates see much slower growth.

Infection rates across South and Central Los Angeles and the Eastside have increased sharply and now lead all regions in the county, exceeding 600 infections per 100,000 people, the analysis shows.
Poorer areas such as Pico-Union and Westlake in Central L.A., and Vermont Square in South L.A., all reported low infection rates in early April, but now rank among the top 10 communities out of more than 300 countywide.
The Times compared neighborhoods in which more than 25% of the population was living below the poverty line — defined by the Census Bureau as a family of four making less than $26,000 a year — to those in which the poverty rate was lower than 5%.
The shift shows the surge feared by public health officials did come to pass, but was largely concentrated in the poorest, most crowded neighborhoods — areas with a lot of essential workers, more crowded housing and higher rates of underlying health conditions such as asthma, diabetes and heart disease.
Wealthy areas saw an early surge in coronavirus cases in L.A. County. More accessible testing and international travel provide a likely explanation.
Early in the outbreak, health officials and experts warned that numbers showing higher infection rates on the Westside in predominately white, affluent neighborhoods such as Bel-Air, Beverly Crest and Brentwood were skewed by uneven testing that masked the true spread of COVID-19. Those areas have seen their fortunes improve after months of social distancing and economic disruption.
“We’re not seeing a decline in infection rates yet in Central and South L.A.,” said Jim Mangia, chief executive of St. John’s Well Child and Family Center, which operates 18 clinics in those areas and other predominantly low-income communities of color. “I think it speaks to the history of health disparities ... the lack of access to social distancing and the fact that many of our residents have to continue to work in high-risk situations.”
Diana, a 19-year-old college student who lives with her parents in Westlake, said that early on, they didn’t know anyone in their neighborhood who was infected.
But Diana worried from the start. She read articles about the wealthy and celebrities getting access to early testing as cases spiked on the Westside, and watched helplessly as her father continued to go to work packaging essential goods without protective gear. She thought it was only a matter of time before the virus trickled into their neighborhood.
Sure enough, Diana began experiencing symptoms on April 15; her father on April 27. They both tested positive, and on May 5, he was hospitalized for six days.
“He would call us and it felt like he was saying his goodbyes,” said Diana, who did not provide a last name, saying she wanted to protect her parents, who are in the country illegally.
“I don’t know if I’ll make it out alive,” Diana recalled her father saying from the hospital.
L.A. County Department of Public Health Director Barbara Ferrer said the rise in infection rates in low-income communities and the gap compared to wealthier areas is so pronounced that it can’t be caused by increased access to testing alone. She thinks there are other factors driving it, including higher levels of exposure among frontline workers.
“If we’re not careful, and we don’t pay a lot of attention to this,” Ferrer said, “the disproportionality could become even greater, even if you flatten the curve.”
John Kim, executive director of the Advancement Project of California, a civil rights and public policy group that has been studying coronavirus trends in L.A. County, said he thinks the surge in poorer and non-white neighborhoods might represent the “second phase of the virus.”
The group released a study that shows areas with higher percentages of black or Latino residents are seeing more coronavirus cases while areas with a higher share of white residents have less. Also, they found that neighborhoods with higher poverty rates are reporting more COVID-19 cases compared to less impoverished areas.
Dr. Coco Auerswald, associate professor at the UC Berkeley School of Public Health, said L.A. County’s early numbers reflected a nationwide trend of wealthier people being first in line for testing.
“The rich and famous were getting tested first because they had the means to get tested in an environment where testing was scarce,” she said.
Since the outbreak began, Travis Longcore has been working remotely from his Beverly Crest home, ordering food and other items online.
Latinos and blacks under 50 are dying of coronavirus at alarming rate in California
“There is the luxury of being able to stay home and perhaps continue to make a living,” said Longcore, former president of the Bel-Air/Beverly Crest Neighborhood Council. “To be able to pay other people to take on the risk of going to the store and exposing themselves to many more people than you are — it’s a real ‘two Americas’ story in that respect.”
An associate adjunct professor at the UCLA Institute of the Environment and Sustainability, Longcore said the pandemic has exposed the country’s deep-seated economic and racial disparities.
“It’s just laid bare the structural inequalities of the country. It couldn’t be better designed to fillet open the inequality of the country because of the two completely different experiences,” he said.
County health officials, elected leaders and healthcare providers are looking to neighborhood infection data to help target the hardest-hit areas for increased testing and to amplify public information campaigns about wearing masks and social distancing. They say it underscores the need to protect frontline workers who face higher risk of infection.
In his South L.A. district, City Councilman Marqueece Harris-Dawson has heard concerns from his constituents that the disproportionate impact there will be overlooked because it’s a lower-income area with a larger share of disenfranchised black and Latino residents.
“I think people here are poised for the larger society to say ‘we are going to look the other way now that it’s in that community’ and I think people here are geared up for a fight to make sure that doesn’t happen,” Harris-Dawson said.
Before the novel coronavirus was known to have reached American shores, South L.A. resident Yolanda Davidson-Carter described the disease to friends and listeners of her podcast as nothing more than the seasonal flu.
As the early coronavirus numbers rolled in, showing the spread in white, wealthier communities, Davidson-Carter said she felt some solace that the disease seemed to largely skip South L.A.
But she grew nervous when the county released data that showed black people had a higher rate of infection and death.
“I didn’t think for a minute there would be so many cases in South Los Angeles,” said the 47-year-old Hyde Park resident.
From barber shops to shopping malls to restaurants, many businesses shuttered for months began to come back to life this week as government officials rapidly lifted stay-at-home orders that helped slow the spread of coronavirus.

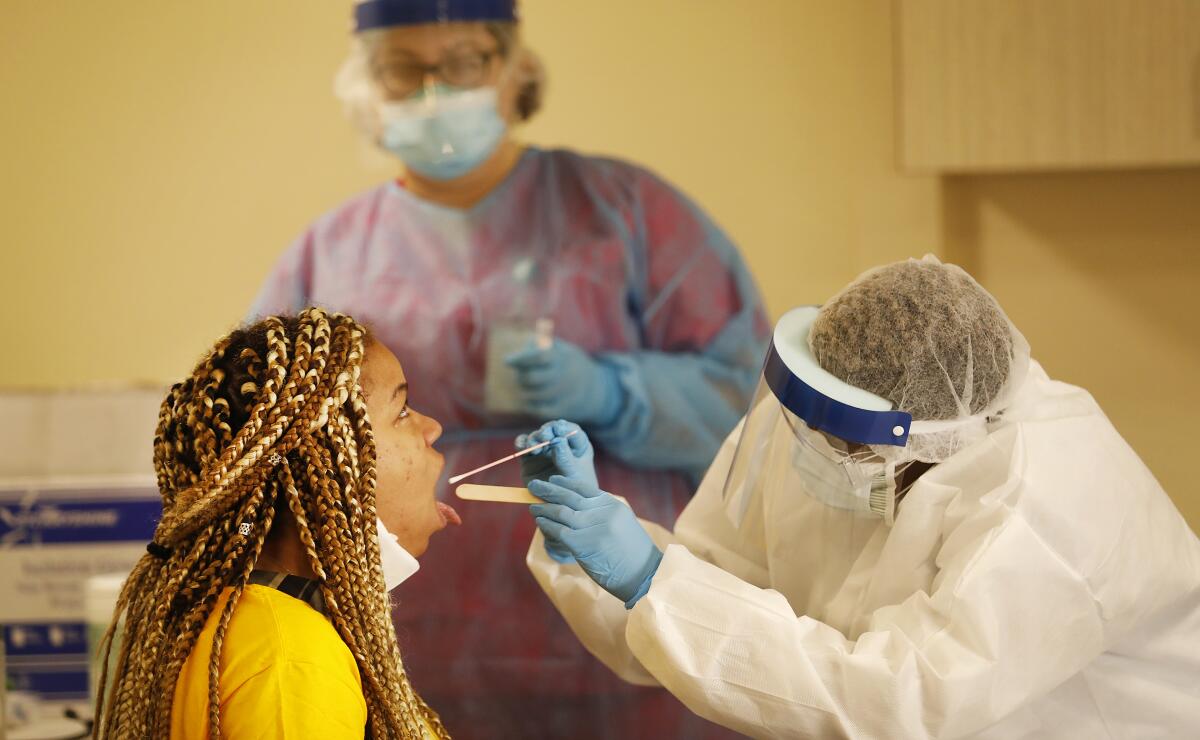
Early on in the outbreak, test kits were so scarce that health clinics and hospitals serving low-income communities struggled to get them.
While testing in low-income communities has improved significantly, it has still not caught up to wealthier areas, according to county health officials.
In Westlake, Diana and her father had wanted to get tested when they first got sick, but they didn’t know where to go. They had heard of a drive-in testing site nearby, but the family doesn’t own a car. So they weren’t tested until after April 29, when Mayor Eric Garcetti announced all residents could access free testing.
Diana’s father was discharged from the hospital and is now recovering from the virus, both of them isolating in one of their bedrooms. There are five people living in the two-bedroom apartment, making it challenging to quarantine. She wonders if her father’s hospitalization could have been prevented had he been tested sooner.
St. John’s went from testing a few dozen people a day in March to more than 500 in May. But Mangia worries that progress could be squandered if the country reopens too quickly.
Many of the poorer neighborhoods now suffering the highest infection rates tend to have larger immigrant populations with a greater share of residents living in crowded conditions, said USC sociology professor Manuel Pastor.
Some of those areas also lead the nation in overcrowding, including Pico-Union and Westlake, where more than a third of housing units are classified as crowded — meaning there is more than one person per room, excluding bathrooms. A recent Times report found that Los Angeles County has five of the 10 most crowded ZIP Codes in the United States, and public health officials said such housing conditions can accelerate the spread of the virus.
Those neighborhoods have also seen the most COVID-19 deaths in Los Angeles. As of May 26, the virus had killed 71 people in Westlake and 56 in Pico-Union, and both have death rates among the top 10 in the county.
Councilman Harris-Dawson said the county’s stay-at-home order has been especially challenging for residents in his district because so many are essential frontline workers who don’t have the option to work remotely.
“You can’t stay home and you’re in a dense housing situation. So you have one person in that household that’s going to work and when that person gets home they can’t really socially distance. I just think that can’t be stated enough,” he said.
Hilda Lopez, 46, a garment worker from Koreatown, said the virus seemed like a faraway threat until her brother fell ill in March, eventually landing in the hospital and in a medically induced coma for 21 days. Lopez said her brother, Alejandro Valeriano, 44, was discharged in May and is relying on an oxygen tank and physical therapy to help get him walking normally again.
Since then, it feels as though a second wave of the virus has targeted her community, Lopez said.
She knows plenty of friends and acquaintances who have been affected now, including mothers, like her, who only want to provide for their families. Lopez hasn’t had steady work since early February, has missed two rent payments and worries she’ll be evicted soon if she doesn’t find work.
“I ask myself a lot why there is more sickness where we are,” Lopez said. “Sometimes I tell my brother: This virus was created to eliminate us.”
Times staff writers Alejandra Reyes-Velarde and Angel Jennings contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.