Are L.A. County’s new COVID restrictions really necessary? We talk to the experts

- Share via
A limited nightime curfew.
Suspending outdoor restaurant dining in Los Angeles County.
A new “Safer at Home” proposal that would further restrictions.
With coronavirus cases spiking, California — and particularly Los Angeles County — has been ramping up new restrictions on gatherings and venues where people mix with one another. The moves are far less severe than the stay-at-home orders of the spring. But after months of the pandemic, they’re a step backward for a state that is backsliding into its worst surge of coronavirus yet.
Gov. Gavin Newsom has announced a stay-at-home order affecting most of California.
The ban on outdoor restaurant dining in L.A. County has sparked a backlash with owners and others who say it’s too harsh and will devastate an already struggling industry. L.A. County Supervisor Kathryn Barger said such measures would “further devastate local businesses and employees who have been asked to shoulder an unfair burden this year.”
Health officials and epidemiologists say the dangerous trajectory of COVID-19 has given them no choice, and that dithering on actions to keep people from transmitting the virus could worsen the crush of hospital patients in the coming weeks and possibly fuel a higher death toll by Christmas. One influential model forecasts that, based on current policies, California’s cumulative pandemic death toll will double, to more than 37,000 dead, by the end of winter.
In the last seven weeks, L.A. County has more than quadrupled its number of average daily coronavirus cases recorded over a seven-day period, a Times analysis has found, from fewer than 1,000 cases a day to more than 4,000 a day.
COVID-19 hospitalizations have more than doubled in just three weeks, from about 800 on Halloween to about 1,900 on Wednesday. And daily deaths have tripled since election day, to an average of 29 fatalities a day over a seven-day period.
“Los Angeles is on a very dangerous path,” Mayor Eric Garcetti said this week. “And if we don’t make changes soon to our day-to-day lives, we’ll have more infections, more suffering, more hospitalizations and, yes, more death.”
L.A. County is contemplating a new version of a “Safer at Home” order to further discourage gatherings and situations where people from different households interact, which officials say is needed to halt the alarming spike in new cases.
The new wave of coronavirus cases brings L.A. County closer to another stay-at-home order.
Is this the right path?
Here are some answers, and some perspective, from epidemiologists and health officials on the coronavirus surge in Los Angeles County.
Q: What’s the current data?
A: Daily average California coronavirus cases are growing at an exponential rate, with officials reporting larger numbers of cases than at any other point in the pandemic, said Dr. Robert Kim-Farley, medical epidemiologist and infectious diseases expert at the UCLA Fielding School of Public Health.
“With this rapidly increasing number of cases, we are seeing what could be described as a ‘snowball effect,’” Kim-Farley said, “in that the size of the snowball, i.e. community transmission, as it rolls down the hill is gaining momentum and speed, and becoming alarmingly large.”
Another indicator of the reality of the current surge is the broadening transmission.
“We now have widespread community transmission, so transmission is occurring at a number of different venues,” whether it be within homes, restaurants or other workplaces, Kim-Farley said.
Although there’s no one single driver of the surge, all of those settings are contributing, and Kim-Farley said more efforts needed to be taken in multiple areas to get the disease transmission rates down.
Q: Starting Wednesday night, L.A. County ordered the closure of outdoor restaurant dining areas for at least three weeks. What’s the reasoning behind that?
A: Restaurants have been identified around the world as a danger spot for transmitting COVID-19. A Centers for Disease Control and Prevention report found that adults with positive coronavirus test results were about twice as likely to have reported dining at a restaurant than those who tested negative.
The CDC study did not distinguish between indoor and outdoor restaurant settings. Although outdoor settings are safer than indoor settings, you can still get infected with the coronavirus while sitting at an outdoor restaurant, as diners don’t wear masks while eating and the virus can spread through talking and even breathing.
California recorded 20,654 coronavirus cases Monday, surpassing a record of 13,400. L.A. County recorded over 6,000 new cases, also a record.
“You’re sitting across the table from them — and you don’t have a mask on,” Dr. George Rutherford, epidemiologist and infectious diseases expert at UC San Francisco said of potentially coronavirus-carrying dining companions. “It’s all about mixing.”
Eating outside can result in disease transmission just as occurred in the White House Rose Garden ceremony announcing President Trump’s nominee to the Supreme Court.
Another concern among some public health experts is people often come from different households to gather at outdoor restaurant dining tables. A safer approach would be to keep dining parties limited to members of one household at each table, experts say, but such an effort has been impossible to enforce.
Q: Are there any data suggesting that restaurants and other food-related facilities are seeing increased disease transmission?
A: Outbreaks more than tripled between Halloween and Nov. 14 at a category of businesses that includes restaurants, bottling plants, food processing facilities, grocery stores and other food-related businesses, said the L.A. County director of public health, Barbara Ferrer.
There has also been a significant number of violations recently around physical distancing protocols at restaurants, breweries and wineries in L.A. County, Ferrer said. “This leads to overcrowding,” Ferrer said, “and makes it easier for infection transmission in sites where most people are just not wearing face coverings.”
In the first 15 days of November, of 86 citations issued by the county to businesses out of compliance with COVID-19 health orders, 31 were at restaurants.
Critics — including some eatery owners — have demanded the county show stronger evidence that restaurants have been a significant spreader of coronavirus.
Q: Is the cooler weather altering how outdoor dining is managed, and whether it might worsen disease transmission?
A. Those in the know say it’s possible. Because it’s cooling down, some restaurants have begun to erect tent walls to shelter diners from the chill. At one restaurant recently visited by Kim-Farley, an outdoor dining area was surrounded on three sides by plastic sheeting, with the fourth side bordering the exterior of the restaurant.
“It was outside in one respect, but it really wasn’t because of the fact that they were using plastic shields — otherwise it would’ve been too cold for people,” Kim-Farley said. “In a sense, it really is becoming an enclosed area inside the restaurant. It was no longer, quote, ‘outdoors.’”
Surrounding a dining area with plastic sheeting helps keep the coronavirus floating inside what’s basically a tent, instead of the tiny respiratory particles being blown away by the wind. That makes it increasingly likely that other people will breathe in larger quantities of the virus and be infected by their dining companions.
L.A. County rules allow outdoor dining areas to be covered by a canopy and have one side border the restaurant’s wall. But the three other sides of the area must be open. Having three open sides to an outdoor dining area provides “a lot better airflow,” Ferrer said, “and that’s able to, obviously, dissipate virus.”
Q: Are small social gatherings really responsible for much of the surge in cases?
A. Social gatherings are believed to be a factor in the spread of the virus.
Experts say any gathering where people mix can result in transmission of disease. Rutherford said that in Napa County, it’s estimated that 30% of viral transmission occurred in households; 20% in community settings that included restaurants; and 10% at worksites.
Relatively modest social gatherings have been documented to be superspreader incidents. Disease investigators in Arizona who studied an outbreak tied to 60 people found that many of the cases probably stemmed from transmission at an indoor potluck dinner, attended by roughly 15 people, and a subsequent graduation dinner with about 25 attendees. In all, 60 people were found to be infected with the coronavirus. Two of those who fell ill had to go to an emergency room, and one required critical care.
There are also anecdotal reports in which modest social gatherings have been associated with coronavirus transmission.
A truck driver, Tommy Macias, 51, of Lake Elsinore, spent months diligently isolating, then went to a barbecue party with some friends, one of whom had tested positive for COVID-19, showed no symptoms but still attended the gathering despite the diagnosis. More than 10 others who attended tested positive for the virus, and Macias died.
Los Angeles Times columnist Bill Plaschke in August wrote about how he let his guard down after months of fastidiously wearing a mask, refusing to attend cul-de-sac cocktail parties, and avoiding even the grocery store. The weekend before he became ill, he said he briefly let his guard down and met friends at two dinners at two socially distanced patio tables in outdoor restaurant dining areas; neither he nor his dining partners wore masks while they were at the table. That’s where he thinks he contracted the virus.
“When you go to restaurants and you sit outdoors, you take your masks off at the table. So I spent basically four hours without wearing a mask at a dinner table,” Plaschke said in a video interview aired on the news program L.A. Times Today. “None of my companions tested positive. But people came by — waiters, owners — came by to say hello, things like that. That’s where I’m just convinced I got it.”
Q: So who exactly is to blame for the rise in transmission?
A: A blame game is not particularly helpful, said Dr. Kirsten Bibbins-Domingo, chair of the UC San Francisco Department of Epidemiology and Biostatistics.
“We have to accept the fact that community transmission is going up,” Bibbins-Domingo said. “And that means all these activities that we were doing earlier safely while there was less virus around us, we now have to take seriously that we all have to do something more.”
Amid pandemic fatigue, people are questioning the new California COVID-19 lockdown measures. Experts say these rules could help slow the infection rate.
To do that in a large place like L.A. where there’s a lot of people, “you want to be figuring out how to be more cautious before you’re in a part of that rise in cases where you have to take even more drastic measures,” Bibbins-Domingo said. “Everyone has to do a little bit more now because we’re just in a riskier time right now.”
Q: California has imposed a limited overnight stay-at-home order in most areas of the state hit hard by the virus. Do such orders work?
A: In Europe, curfews have been used in combination with broader shutdowns of certain business sectors in recent weeks, and they’ve cumulatively been able to dramatically reduce the daily number of cases. In France, for instance, improvement was seen in a matter of weeks after daily case rates roughly quadrupled.
“It completely turned the corner,” Rutherford said. “The rates are dropping. ... They did this, and it seemed to work.”
A modified stay-at-home order goes into effect for the much of California as of Saturday morning to try to slow the rapid spread of the coronavirus.
Q: Any other reasons for concern that this wave will be worse?
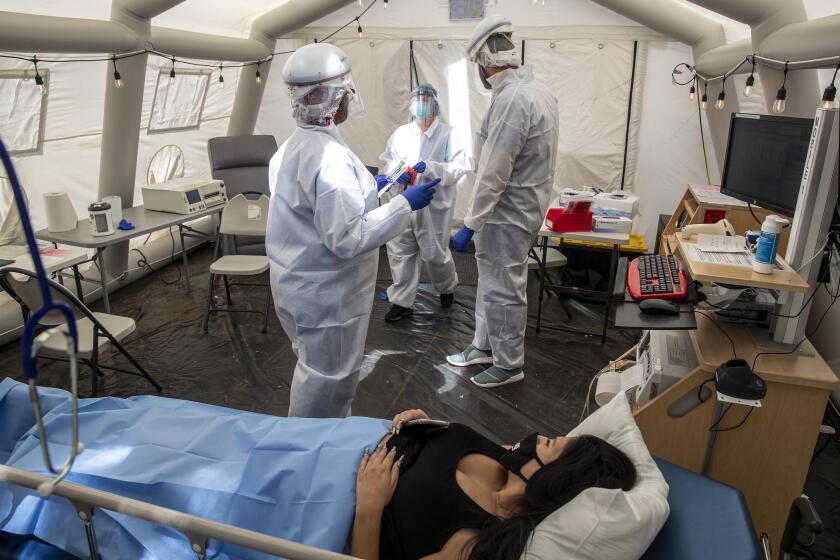
A: There has been a huge increase in the number of healthcare workers infected with the coronavirus. Ferrer said that this week there were an additional 842 new cases among them.
“This is the highest number of weekly cases we have seen in a very, very long time,” Ferrer said. “And it’s a troubling increase.”
Q: What’s the cause of the overall increase in cases?
A: There are likely a lot of factors, experts say, including holiday celebrations such as Halloween; celebrations of the Lakers and Dodgers winning the NBA Finals and World Series; people going out more because they’re fatigued with dealing with the coronavirus; increased travel by people coming from or returning from areas with high transmission rates; and cooler weather, which tends to result in people staying indoors more often, making it easier to transmit the virus.
Q: With the leap in cases, is a surge in deaths expected?
A: Yes. During the surge that began to be detected in L.A. County just after Memorial Day, it took two months before the region experienced a peak in deaths, in late July, and a little over two more months before daily deaths hit a low point. That means that the COVID-19 surge in warmer weather had a four-month lifespan.
Based on what happened in the wave, the surge happening now, which began in late October and rapidly accelerated after election day, could result in a peak in deaths around Christmastime or into the new year.
Dr. Mark Ghaly, the California Health and Human Services secretary, said he expected daily COVID-19 deaths to go up — possibly to a level that California has never seen before.
“Certainly, the numbers of deaths will likely go up,” he said. “Just as we are exceeding our highest-ever numbers of cases, and beginning to see our hospital systems pressed with COVID beyond where they’ve ever been pressed before, the idea that the numbers of deaths could exceed where we’ve been before is also real and true.”
Q: Is the increase in cases showing up simply because more people are getting tested?
A: No. There’s a real increase in disease, because not only are more tests being done, the percentage of people testing positive for the virus is also increasing.”That shows there is real increased community transmission,” Kim-Farley said.
In L.A. County, the rate at which coronavirus tests are coming back positive is now 6.6%, nearly double what it was in late October.
The dire picture painted Wednesday illustrates the ferocity with which COVID-19 has roared back to life over the past few weeks.
Times staff writer Stephanie Lai contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.