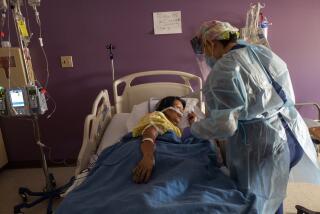Hospitals face tough choices as ICUs fill up with COVID-19 patients
- Share via
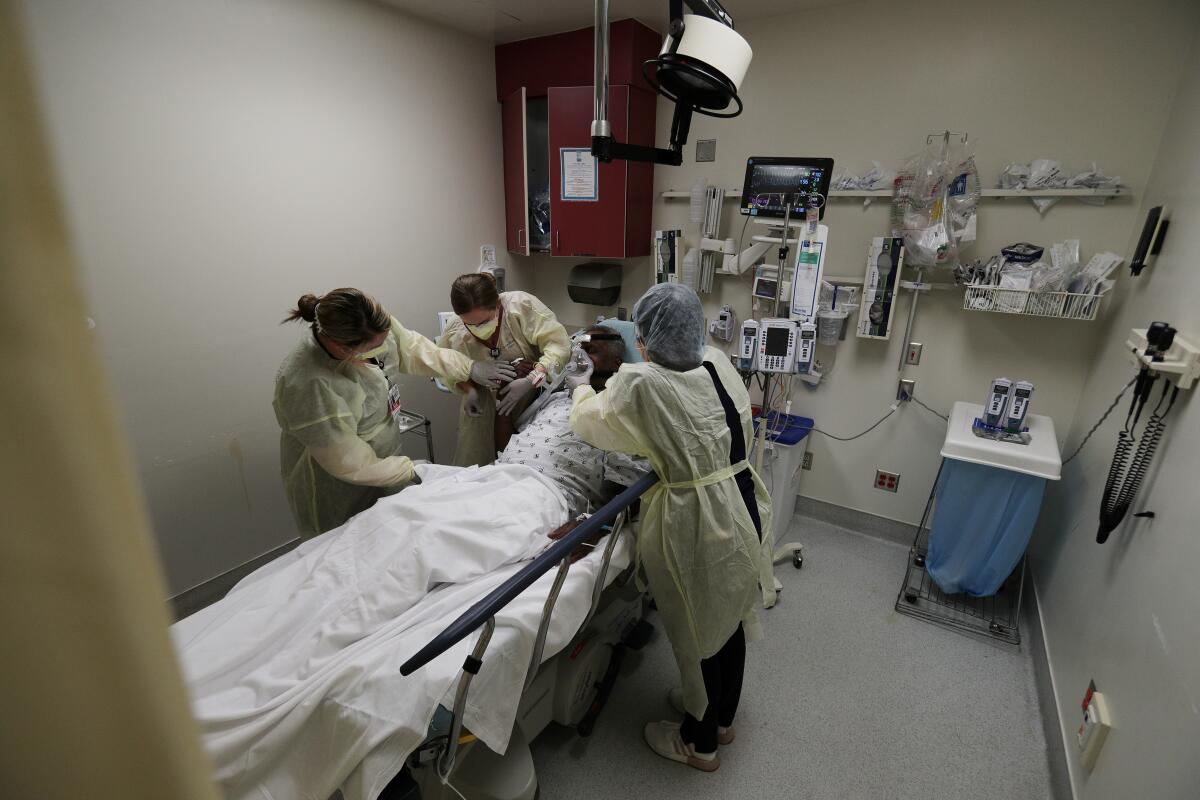
With intensive care units across California rapidly filling with COVID-19 patients, hospitals have a limited number of tools available to free up more capacity in the coming weeks as cases are expected to surge.
Back in the spring, the government opened a so-called “surge” hospital in Los Angeles and even docked a Navy medical ship in San Pedro harbor to take overflow patients if medical centers filled up. But officials found that those supplemental facilities did not treat many patients and did not provide the same level of care as traditional hospitals.
“Hospital ships are wonderful if you’re a 23-year-old wounded sailor. But it’s no place to take care of ICU patients” sick with COVID-19, said Dr. George Rutherford, an epidemiologist and infectious-diseases expert at UC San Francisco. “If they need to be in the ICU, they need to be in the ICU.”
So in the coming weeks in L.A. County, hospitals will try to choreograph their staffing to best meet the needs of critically ill patients, some of whom still might have to be sent to other areas of the hospital that don’t typically treat ICU cases.
But that comes with risks. Should a staff shortage become particularly dire, critically ill patients could end up getting care from nurses and doctors without up-to-date specialized intensive care training.
“Physical beds are not the limiting factor in this, or most other, pandemics,” Dr. Christina Ghaly, the Los Angeles County director of health services, said recently. “What matters is the hospital’s practical ability to take care of the patients that come in the door. And that requires not just a bed, but more importantly it requires people: It requires staff. It requires supplies and equipment.”
Rutherford was more blunt: “If, all of a sudden, you have one nurse taking care of seven patients on ventilators like in New York, the mortality can be astronomical.”
ICU beds are still available even in hard-hit places like Los Angeles County. But the units are filling up fast, as California posts record numbers of new daily coronavirus cases. A Times county-by-county tally Monday recorded more than 34,000 new infections reported on Monday, shattering the previous single-day record of 22,369 cases tallied on Friday.
California has now recorded more than 20,000 cumulative COVID-19 deaths, a milestone recorded Monday by The Times’ coronavirus tracker.
ICU capacity has become tight in several locations around Los Angeles County, including the Westside, the San Gabriel Valley and southeast L.A. County. Among staffed and licensed beds, on Sunday, the Westside had eight ICU beds available; southeast L.A. County had seven, and the San Gabriel Valley had just three.
According to data released Monday, L.A. County hit more than 3,000 COVID-19 hospitalizations on Sunday, and officials say it’s possible that number will rise to 4,000 by next week as more people who were infected during the Thanksgiving holiday fall ill.
ICUs can surge beyond the number of licensed, staffed beds when needed, but the level of expansion is finite.
Hospitals can also redeploy staff from other parts of the healthcare system, such as workers who now work in clinics and other outpatient settings or in other procedures. It does decrease outpatient services, “but it can importantly help add bed capacity when it’s most needed,” Ghaly said.
Hospitals can also cancel scheduled procedures and work to discharge patients who can be cared for in lower-level settings, Ghaly said.
These steps come with consequences.
Delaying scheduled care for other procedures can come at a health cost for other patients who need hospital care for chronic diseases, like heart disease, which could increase mortality for reasons not related to the pandemic. And relying on hospital staff without specialized training in intensive care is not ideal, but the last resort when capacity is overstretched.
Hospitals can do their best to cancel scheduled surgeries to make way for coronavirus patients. But at a certain point, a crush of patients will eventually lead to surging mortality, such as from overwhelmed nurses and doctors taking care of far too many critically ill COVID-19 patients than they normally would.
“This is not an ideal situation and can lead to sub-optimal outcomes for patients,” Ghaly said.
There are also growing concerns about hospital staffing becoming tighter if more personnel get sick from COVID-19.
Healthcare workers are being infected by the virus at a pace never before seen in this pandemic. In the past week, there were 1,745 new coronavirus cases among healthcare workers in L.A. County, more than double what was reported the week before.
“It’s the highest weekly number of healthcare workers testing positive for COVID-19 that we have ever reported,” Ferrer said. “And that has a tremendous impact on our capacity throughout our entire healthcare system to take care of those who are sick.”
Other healthcare systems have come under pressure from worker illnesses or exposure to the virus. The Mayo Clinic Health System, which serves Minnesota, Wisconsin and Iowa, last month said that more than 1,500 of its staff were out due to a diagnosis or exposure to the virus, according to the Associated Press.
The California Department of Public Health on Monday said Southern California has an available ICU capacity of 10.9%, and the San Joaquin Valley, 6.3%.
In previous waves of the pandemic, other parts of California have been able to help other hard-hit spots — San Francisco and San Diego County, for instance, accepted COVID-19 patients from hard-hit Imperial County along the Mexican border. That won’t be possible as much now, with the Bay Area already in the grips of an unprecedented surge.
“If we get in a situation where we don’t collectively take this seriously, we will not have the capacity in other parts of the state to actually help each other out when things get tight,” said Dr. Kirsten Bibbins-Domingo, chair of UC San Francisco’s department of epidemiology and biostatistics.
In Santa Clara County, the number of ICU beds filled with COVID-19 patients has tripled in the last month. The home of Silicon Valley has just 15% of its ICU beds available.
“Unfortunately, we are shattering records, every day,” said Dr. Sara Cody, the health officer for Santa Clara County. “Many of our hospitals have already elected to cancel elective surgeries, and other procedures in order to be able to care for the influx of COVID patients.”
Hospitals that are overloaded with critically ill patients do try to transfer them to other facilities that can accept them. “But, particularly with critical care patients, there are added challenges in in moving patients who are critically ill,” Cody said.
With infections continuing to rise, L.A. County’s average daily death toll could increase by 63%, from 40 deaths a day currently to 65 fatalities daily, Ferrer said. L.A. County is now averaging more than 8,000 new coronavirus cases a day over the past week — a quadrupling in the last month.
Statewide, California’s hospitals exceeded 10,000 COVID-19 patients for the first time. That’s double the number from less than three weeks ago.
Unless trends change, this surge will be unlike the first two waves that have already resulted in thousands of deaths in Los Angeles County. Ghaly projected last week that based on trends, L.A. County will run short of ICU beds before Christmas — a shortage that never occurred in the previous two waves.
One doctor at an L.A. County public hospital said that although there are currently sufficient resources, shortages of beds and staff are expected soon given the recent rapid rise in case counts.
“We’re on the borderline now and the direction it goes is now going to be dependent on society’s willingness to step up and adhere to the restrictions,” the doctor said.
The physician, who asked not to be named because the person was not authorized to speak publicly, said the summer surge was extremely difficult to cope with, due to the flood of patients entering hospitals up and down the state.
“We’re all worried that this next surge is going to be worse than that,” the doctor said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.