Next in line for California’s COVID-19 vaccine? Teachers and first responders, panel says
- Share via
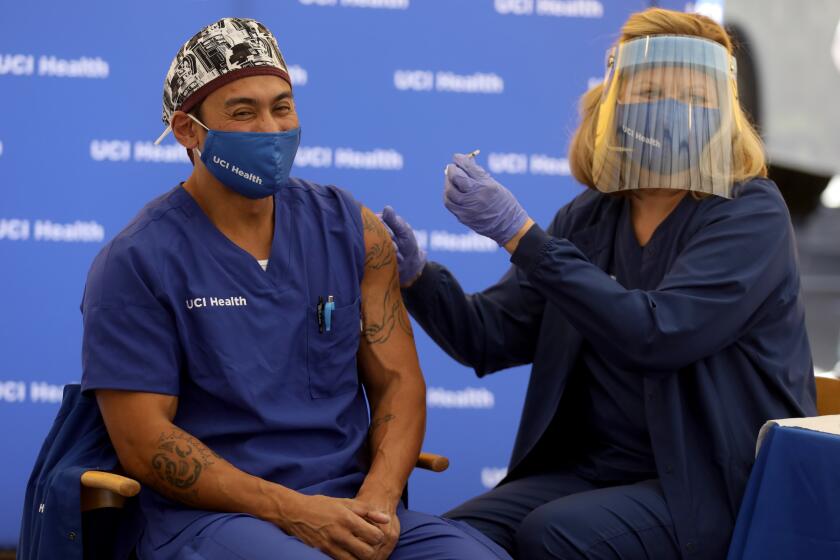
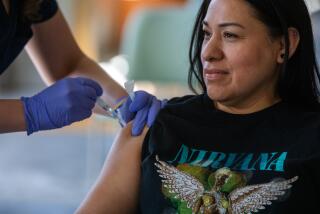
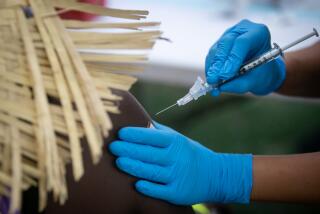
California’s first responders, farmworkers and educators would be among those next in line to be vaccinated against COVID-19 under recommendations a state advisory committee discussed this week.
Should that guidance eventually be put into effect, those workers — as well as others in the broadly defined fields of education and childcare, emergency services, and food and agriculture — would be prioritized within the second major stage of the state’s wider vaccination push.
Roughly 5.9 million Californians work in those sectors.
Though California’s vaccine rollout plans continue to be defined, Wednesday’s meeting of the state Community Vaccine Advisory Committee provided a window into how the process may play out in the weeks to come.
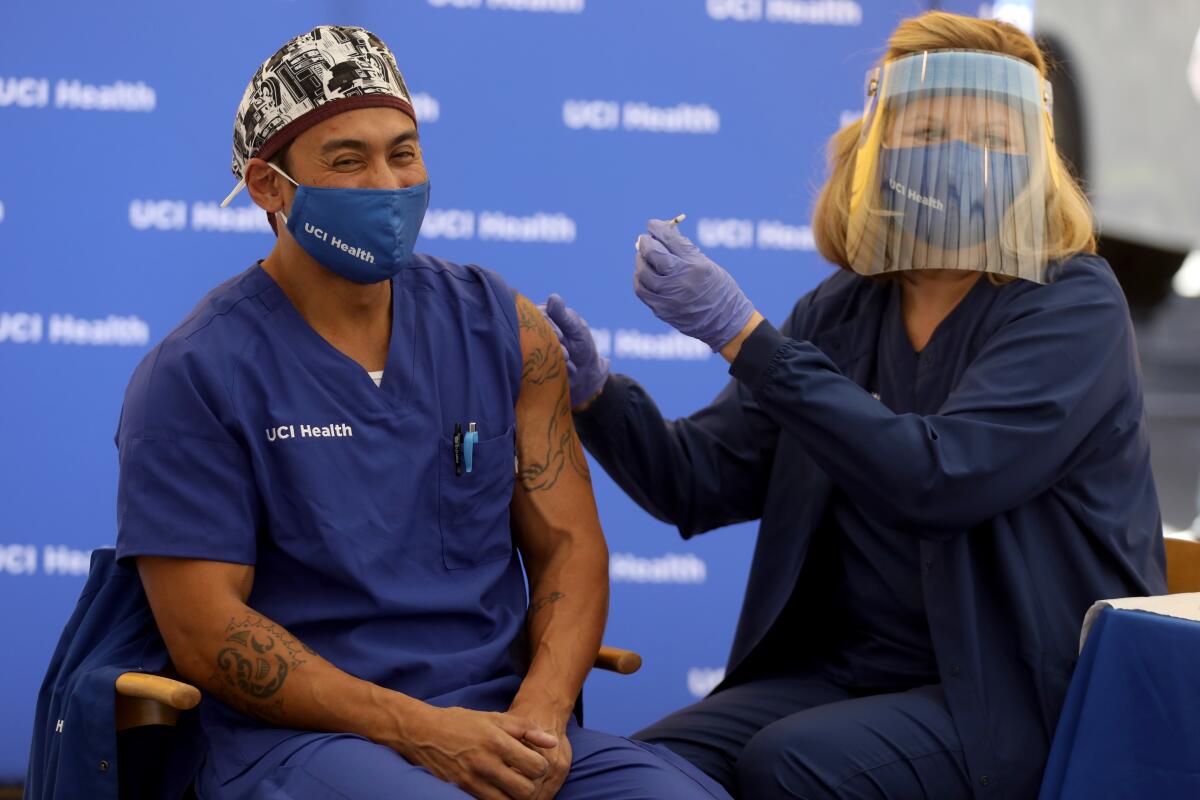
The state’s initial doses of the COVID-19 vaccine are earmarked for front-line healthcare workers and residents of long-term care facilities, such as nursing homes. After that, officials have said essential workers come next.
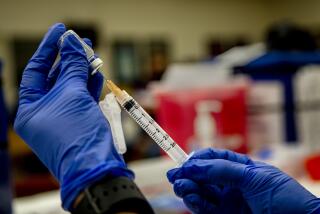
COVID-19 vaccine distribution has begun. There are no exact timelines yet, but here’s a general idea of when you may be able to get it.
But the classification of “essential workers” is expansive — encompassing almost 12 million Californians, roughly two-thirds of the state’s entire workforce, in 13 wide-ranging fields.
“So two-thirds of us are essential. That’s nice to know,” said Dr. Oliver Brooks, co-chairman of the state work group that’s developing guidance on vaccine distribution.
The recommendations presented Wednesday would prioritize workers in some of the following fields:
- Education and childcare: Childcare workers, preschools, elementary and secondary school personnel, community colleges, colleges and universities, and trade schools.
- Emergency services: Nonmedical first responders, law enforcement, firefighters, child and youth services, shelters, nonresidential social services for the elderly and people with disabilities, and justice and safety activities.
- Food and agriculture: Agricultural workers; animal/seafood/bakeries/food manufacturing and slaughtering/processing; fruit, vegetable, dairy and special foods manufacturing; grocery stores/food markets; food and drinking establishments; pharmacies/drugstores; warehouse clubs; community food services; nurseries/florists; and sawmills.
State officials have previously said California’s first allocation of the Pfizer-BioNTech vaccine would total about 327,000 doses. Gov. Gavin Newsom said this week that the state expects to receive 393,900 more doses on top of that, as well as potentially 672,000 additional doses of another vaccine from Moderna, should that receive U.S. authorization, as expected.
But Newsom’s office confirmed Thursday that the next shipment of the Pfizer-BioNTech vaccine will be more in the neighborhood of 233,000 doses, significantly lower than initially thought.
Erin Mellon, a spokeswoman for Newsom’s office, wrote in an email that the original projection “was based on what the federal government had communicated to us” and that “the federal government delayed the number of Pfizer vaccines that California will receive in the next shipment — many states received new estimated shipment amounts.”
The Long Beach City Council voted unanimously Tuesday to draft an urgent ordinance mandating an extra $4 per hour for grocery store workers for at least the next 120 days. Other cities are considering similar measures.
That many doses is a drop in the bucket for a state the size of California.
Though the state expects to receive millions more doses by early next year, and additional vaccines in development could further expand availability, officials face difficult choices about which Californians should be protected next against COVID-19.
“We’ll be grappling with trying to determine criteria that can be used practically and efficiently to sort between worthy recipients of scarce vaccine, whether that’s using age or medical conditions or other factors to be able to give providers and the public and the workers clarity as to ... what are some practical tools that can be used to be able to let the highest risk or those at priority go first,” said Dr. Robert Schechter, the other co-chairman of California’s Drafting Guidelines Workgroup.
Different groups ranging from waste workers to meatpackers to the ride-hailing company Uber are already jockeying to secure early position in the vaccination line.
Debra Duardo, superintendent of the L.A. County Office of Education, sent a letter to the governor Wednesday calling for teachers to be a high priority.
The COVID-19 vaccine continues to roll out throughout Southern California.
“School closures have had a negative impact on our children, particularly those from lower-income families. As you have stated,” Duardo wrote, referring to Newsom, “reopening schools is also a crucial first step in an economic recovery.”
Most public school campuses remain closed in L.A. County. In a poll of more than 500 Los Angeles teachers released Wednesday, 36% rated a widely available vaccine as “critically important” to feeling comfortable in returning to the classroom.
Health officials estimate the vaccine will not be widely available to the general public until the spring or early summer.
The goal is to eventually integrate it into the larger healthcare system and for people to be able to get their vaccinations in pharmacies, clinics and other common locations, Dr. Seira Kurian, director of the L.A. County health department’s Division of Medical Affairs, said in a virtual town hall meeting Thursday evening.
But to get people quickly inoculated during the health emergency, she said, officials are considering setting up vaccination “pods,” or locations similar to current testing sites where many people can get inoculated — something that could be difficult in the midst of a pandemic surge in which people still need to maintain distance.
Among the considerations, she said, are drive-through vaccination sites where people stay in their vehicles and remain for several minutes to be observed by a medical professional after getting their shots, Kurian said.
The vaccine will be provided for free and will be available to people without health insurance, Kurian said.
People who have already tested positive for COVID-19 should still get vaccinated, Dr. Paul Simon, chief science officer for the L.A. County Department of Public Health, said during the town hall.
“Those who’ve had past infections are still encouraged to be vaccinated. However, if we do run into a shortage, we would recommend then that those who’ve had documented infection in the past 90 days delay getting vaccinated,” he said. That is because there is evidence, he said, that people are more protected from getting sick again, at least temporarily, after recent infections.
California is now tallying an average of 203 COVID-19 deaths a day over a weekly period, and 35,200 cases a day — both records, and both quadruple the numbers from mid-November.
Conversations about the vaccine rollout all point to the same hopeful future: a time when California, along with the rest of the world, can finally declare victory over the COVID-19 pandemic. Such long-view optimism, however, is tempered by near-term devastation.
More Californians are becoming infected with, hospitalized by and dying from the coronavirus than at any other point in the outbreak.
Single-day pandemic records were shattered across the state again Wednesday, with 51,724 new coronavirus cases and 393 additional deaths reported.
On Thursday, 51,209 coronavirus cases were reported statewide — the second-highest single-day tally. There were 288 deaths reported Thursday, the third-highest single-day tally.
The state is now recording an average of 220 COVID-19 deaths a day over a weekly period, and about 38,000 daily cases — both records, and both quadruple the numbers from mid-November.
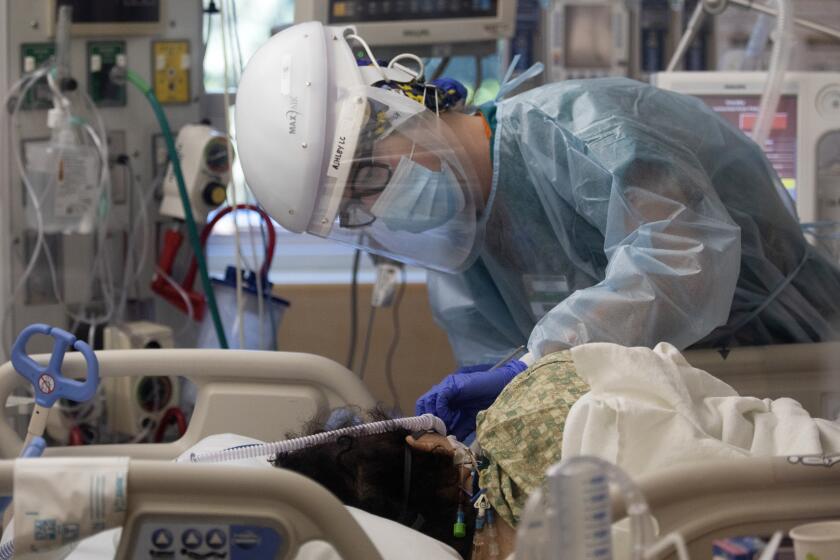
The enormous wave of infections comes as hospitals are already inundated with record numbers of coronavirus-positive patients.
On Wednesday, the most recent data available, 15,431 people across the state were in hospitals with coronavirus infections — more than six times more than the number on Halloween — and a record 3,280 of them were in intensive care.
The most recent record-high hospitalizations do not account for the sky-high numbers of new infections, a chilling prospect for the state’s stretched-thin hospitals and healthcare workers.
On Thursday, ICU bed availability reached 0.0% in Southern California — a sprawling region the state defines as Imperial, Inyo, Los Angeles, Mono, Orange, Riverside, San Bernardino, San Diego, San Luis Obispo, Santa Barbara and Ventura counties, state figures show.
The day before, ICU availability again tumbled to zero in the San Joaquin Valley, though it bounced back to 0.7% on Thursday.
“If the numbers continue to increase the way they have, I am afraid that we may run out of capacity within our hospitals,” said Dr. Denise Whitfield, associate medical director with the L.A. County Emergency Medical Services Agency and an emergency room physician at Harbor-UCLA Medical Center.
Times staff writers Sean Greene and Howard Blume and the Associated Press contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.