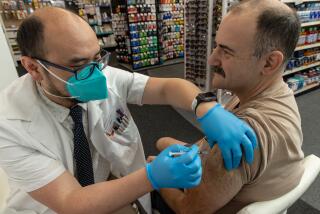
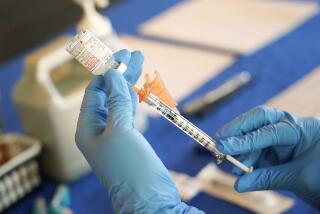
They tell us how to stay safe. But what do experts do to avoid COVID as holidays loom?

- Share via
The Three Kings Day party has been canceled for the second year in a row at Barbara Ferrer’s home in Echo Park. No hilarity, no live music, no 80 or so guests honoring the Magi who brought gifts to the infant Jesus.
Instead, the director of the Los Angeles County Department of Public Health is planning a small outdoor Christmas Eve dinner with family and a few close friends. There will be tamales. Arroz con pollo. And COVID-19 tests all around.
Dr. Peter Chin-Hong, professor of medicine and an infectious-disease specialist at UC San Francisco, is flying to the East Coast with his wife and two teenage daughters to celebrate with family. At just one small dinner, not the usual string of festivities.
And what are UCLA epidemiologist Shira Shafir, her husband and their 3-year-old son planning? Mostly nothing. The grown-ups in the house are vaccinated and boosted. Little Benji won’t be eligible for two more years. “It’s the three of us and maybe a Zoom,” Shafir said, “and that’s it.”
These are among the experts who have guided us through 21 grueling months of fear and death and uncertainty. They have told us when to mask, when to stay home, when to vaccinate, when to get a booster shot.
Many of us have listened. But not all. Which is why we’re here, getting ready to celebrate another COVID-19 Christmas as another variant threatens and another surge looms, as the U.S. death toll crests 800,000 and we fret over which is more dangerous: infection or isolation.
Unlike COVID-19 Christmas No. 1, when precautions were drastic and one-size-fits-all, there are tools today to help keep us safe: vaccines and boosters and easily accessible tests for the virus, better basic information about who is at most risk and why. Now, the precautions to take are as varied as our lives. Now, it’s complicated.
Just ask the experts.

Some, like Ferrer, have received death threats for backing tight early restrictions. Others, like Dr. Monica Gandhi, professor of medicine and associate chief of the Division of HIV, Infectious Diseases and Global Medicine at UC San Francisco, have incited controversy for espousing less strict anti-COVID-19 measures.
Either way, these are women and men whose actions are as closely scrutinized as their words during these tense and polarized times.
But their holiday plans have few common denominators. They are all vaxxed and boosted. Everyone they hope to spend time with also is vaccinated, if eligible. After that, their personal safeguards differ in ways both big and small.
Ferrer follows three rules for staying alive during winter 2021-22, guidance that forms the backbone of her advice to us all:
- Get vaccinated and boosted.
- Get tested when you’re going to be in high-risk situations for you or those around you, or if you’ve been exposed to a COVID-19-positive person or have symptoms yourself.
- Wear a mask when you’re indoors in a public place or with people outside of your household.
Ferrer is 65, which makes her more vulnerable to the virus. Her husband and many of her friends are also older. She’s recently switched to wearing KN95 masks, which offer more protection than cloth masks or the thin, blue surgical numbers. She will not attend nor host large parties during this normally festive season. She stocks up on test kits. She offers them to guests.
“We’re in, I think, decent shape, to manage this winter holiday very differently than last winter holiday,” she said. “But we’ve all got to invest in taking these safety precautions. It doesn’t work if lots of people just sort of say, ‘I’m done. I can’t do this anymore. I’m not going to do anything.’”
That, of course, is the problem. The federal Centers for Disease Control and Prevention figures that 72.3% of the U.S. population has received at least one dose of a vaccine. Which means there are nearly 92 million people out there who have received no protection. In Los Angeles County, about 2.2 million people age 5 and older have yet to receive a first dose, and 3.4 million still need a booster.
UC San Francisco’s Gandhi thought long and hard about whether to get a COVID-19 vaccine booster herself.
She’s a founding member of White Coats for Global COVID Equity, an organization of healthcare providers, researchers and students at academic medical centers that advocates for low-income countries to have greater access to lifesaving vaccines. One concern about boosters is that rich countries like the United States are pushing a third shot when so many people in poorer regions have yet to get even one.
“I wasn’t actually going to get boosted, because of global vaccine solidarity,” Gandhi said. “But then my father got an immunocompromising condition relatively recently. And that’s why I got boosted, so I could see him.”
It’s been several years since Gandhi and her family have had anything near a normal holiday season. In 2019, her husband died of cancer the day after Thanksgiving. In 2020, she and her two sons stayed in the Bay Area. By themselves.
“It was lonely,” she said. They “did nothing. Just ...” she paused, “nothing.”
She was glued to her computer, waiting to see when she could be vaccinated. She wrote an op-ed that outlined an approach called “harm reduction,” which she endorses out of personal experience: She is medical director of UC San Francisco’s Ward 86, the nation’s oldest HIV/AIDS clinic, and, as she was writing the piece, she faced a holiday spent in grief and isolation.
Gandhi defines harm reduction as “trying to mitigate the impacts of a pathogen while still keeping human needs in account.” It is the opposite of California and many counties’ initial guidance, that the only way to be safe was to stay home, alone. It won her friends and foes alike.
“I’ve been on the side of harm reduction and human contact more than other infectious-disease doctors right now,” she said. “I think that’s a fair thing to say. ... I think of the isolation and mental illness and loneliness and how hard it’s been for people. We have gotten to that point where we need to tip the balance toward human contact.”
So, Gandhi got the booster. Her 11-year-old son has had his first dose of the vaccine; her 13-year-old is fully inoculated. They will fly to Boston to be with their totally vaccinated family. The younger boy will take the middle seat where the airplane ventilation is best. They will wear regular surgical masks, not extra-protective N95s. They will only do a COVID-19 test if they experience virus symptoms.
“I would recommend unvaccinated and symptomatic people who are vaccinated but have symptoms, cold-like symptoms, doing a rapid test,” she said. “But I’m really not convinced that asymptomatic, vaccinated people are a major source of spread.”
UCLA’s Shafir begs to differ with Gandhi’s approach.
She is concerned about the Omicron variant. She believes that, in addition to vaccination, it is critical for people to maintain social distance from others, wear masks and ensure there is good ventilation wherever they are. She had a Zoom call for friends before Thanksgiving to guide them as they plan their own holidays.
“It is entirely possible,” she told them, “if everybody is fully vaccinated and they test negative to gather safely indoors. Because a negative antigen test indicates that nobody is infectious. At that moment.”
Nobody goes into their house. They do not go into anybody’s house. The only exception has been Shafir’s mother, who visited in April and October.
Before her mother got on a plane to fly from Arizona to Los Angeles, Shafir instructed her to quarantine for 10 days. She had to take a PCR test — which takes longer to get results than an antigen test but is considered more accurate — and have a negative result. During the flight, she had to wear two masks. And when she landed, she had to take a rapid antigen test and have a negative result.
Only then could she step through her daughter’s door and wrap her arms around her grandson.
Dr. Robert Wachter, professor and chair of the Department of Medicine at UC San Francisco, will observe Christmas the same way he did in 2020. And 2019. And many other years before. He’ll be treating patients at UC San Francisco Medical Center. “I’m Jewish,” he said. “It’s not that important to me.”
Thanksgiving, however, had a deep COVID-19 imprint. He flew to Florida to be with family, wearing an N95 mask and keeping the vent above his seat open. He brought a rapid test kit that he used when he woke up with a sniffle. He is fully vaccinated and boosted, as was everyone else at the holiday dinner — which, he said, cut the chance of contracting the virus by 95%.
Before Omicron, he said he started thinking and writing about our response to the pandemic. He recognized that “a version of COVID will be with us forever. It will ebb and flow, but it will never go away completely.”
Then it hit him: If he does not do the things that bring him joy now, when he’s vaccinated and boosted and the world is not locked down, he never will.
And, barring some dramatic change, that is no way to live.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.