‘I’m living from day to day’: Isolating for MPX can put people out of work for weeks

- Share via
When a doctor told Ivan that he needed to isolate himself and not share bedsheets to keep the MPX virus from spreading, he wondered: How?
“It would be absurd trying to isolate while sharing a bed,” the Hayward, Calif., resident said in Spanish.
The 43-year-old man, who is gay, had been splitting a bedroom with a female friend to save money in the San Francisco Bay Area, where rents are steep. He was grateful when another friend offered him somewhere else to isolate, but then there was the money: Doctors warned that isolation might last weeks as his lesions healed, and Ivan was out of sick days at the grocery store where he works.
The virus racked him with pain and ultimately kept him away from work for three weeks — and that cost him almost $2,000 in income, said Ivan, who asked to go by only his first name to protect his privacy. Now rent is looming. A friend helped him cover his phone bill, but as of late August, he still needed $500 for a car payment.
Editor's Note:
In light of widespread concerns that the name “monkeypox” is racist and stigmatizing, the World Health Organization has renamed the disease “mpox.”
“I just haven’t gotten the money,” he said.
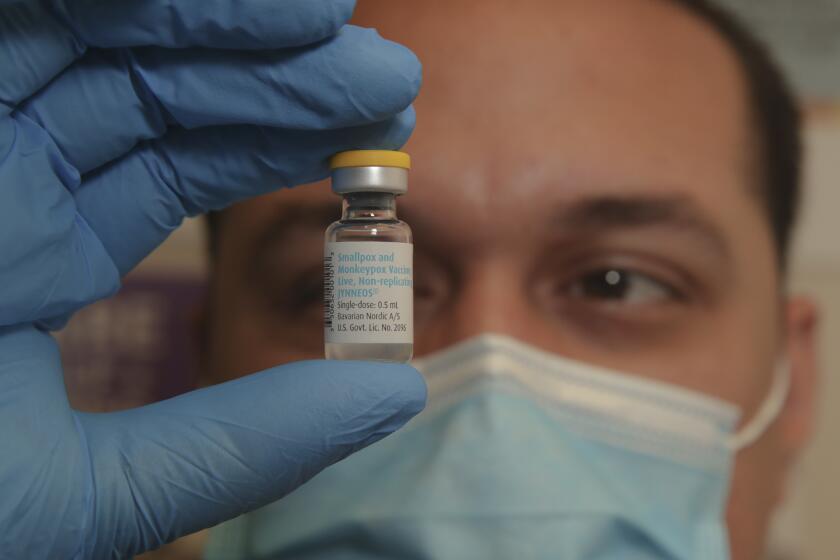
The MPX virus has wreaked financial havoc for workers who have little paid time off to recover from illness. Healing from painful lesions can take weeks — much longer than the three days of sick leave that California generally requires from employers. Government guidelines aimed at stopping the spread of MPX — which is what the California Department of Public Health calls monkeypox — urge people to try to remain isolated at home.
“The best thing would be … for them to be able to stay home and to work remotely,” said Dr. Rita Singhal, chief medical officer for the Los Angeles County Department of Public Health. “But we know that that’s not an option for everyone.”
As the coronavirus sickened and sidelined Californians, state and local lawmakers set up programs that bolstered paid leave for people affected by COVID-19. In Los Angeles, for instance, which requires at least six days of paid sick leave annually for many employers, city officials decided to mandate additional COVID-19 leave for workers at large companies.
Across California, as of this year, some workers at bigger companies are eligible for up to 80 hours of paid leave if they are ill with COVID-19 or caring for a family member with the virus. But so far, state lawmakers have not set up similar programs specifically for MPX, despite an isolation period that can last as long as four weeks.
How monkeypox spreads, how to get a vaccine and more: Your frequently asked questions about monkeypox, and answers from experts.
“No one should be forced to choose between complying with health orders and being able to feed themselves and pay their bills,” said Samuel Garrett-Pate, managing director of external affairs at Equality California, which has advocated to extend more paid leave for people affected by the virus. “There’s no reason that people affected by monkeypox — which requires a longer quarantine period — are any less deserving of that same relief than everyone who was affected by COVID-19.”
Many California workers can also try to access payments for disability insurance — a program that can partially cover lost wages in the short term for Californians who are unable to work because of non-work-related illness — but that process can be cumbersome, Garrett-Pate said.
Restaurant worker Justin Bolding, who first realized he might have gotten the MPX virus when he felt unusually exhausted after a Sunday night shift, said he had phoned a state agency hundreds of times to get help with applying for the program.
“I’m still trying to get some money from losing three weeks of work,” Bolding, 37, said in August, shortly after he submitted a paper application.
Bolding had to isolate for weeks after the virus peppered his body with lesions from his head to the sole of his foot. One popped up on his nose, he said, which made him especially worried about protecting others from infection. Bolding counts himself as luckier than others who got infected, but he still had to dip into his savings as he went without his usual paychecks.
Even if workers can access them, “disability benefits don’t pay your full salary, and folks are already living paycheck to paycheck,” said Kathy Finn, secretary-treasurer for United Food and Commercial Workers Local 770, whose members include grocery and pharmacy workers.
California does require continued pay for healthcare workers who are exposed to some transmissible diseases on the job if a physician recommends they stay out of the workplace, which applies to MPX, said Stephen Knight, executive director of the nonprofit Worksafe.
But for others, “if public health requires workers to isolate for the general good ... then the public needs to compensate those workers to ensure that this is not a ticket to joblessness and homelessness,” he said. “Otherwise people will not report they’re sick.”
Workers who need to take time off for MPX can also face stigma.
The virus has disproportionately affected gay and bisexual men and many cases have spread through intimate or sexual encounters, although health officials have emphasized that anyone can get the virus and that it can also be transmitted through other kinds of skin-to-skin contact.
“They don’t want to tell their employer they have monkeypox — it’s highly stigmatized. They don’t have any protected time off,” said Dr. Adam C. Lake, a physician who practices in Lancaster, Pa. And “even if you do, you have some explaining to do if you’re taking four weeks off.”
Marquiette, a 49-year-old construction worker, said that when he had to isolate for weeks after getting the virus, he quickly lost a job. “They were like, ‘You shouldn’t be taking off for so long,’” said the Los Angeles resident, who asked to use only his first name due to privacy concerns. “I had to tell them why I needed the time off — and that scared the company.”
Marquiette said a construction foreman quizzed him about how he got the virus. He said he didn’t know. “You have people looking at you crazy,” said the worker, who is heterosexual. “The first thing coming to their mind is something negative, and I couldn’t answer the questions that they asked me.”
As of late August, he had been out of work for almost three weeks, he said. “I don’t have gas to get around. I’m living from day to day. I’m having to go to pantries just to get food to survive right now.”
His landlord told him not to worry about being late on the rent. But Marquiette worries about when he will get hired again. Word of mouth travels in his field, he said.
“Now I’m blackballed and I can’t get hired nowhere,” he said.
Paul, 35, who works in the tech industry, said he “had the privilege of making up excuses” when he had to isolate, because he is supposed to come into the office only a few times a week.
“I kept getting asked, ‘When do you think you’ll be coming back in?’ ” said the Los Angeles resident, who asked not to give his last name to protect his medical privacy. On video calls for work, he strategically chose clothing that would conceal his lesions and gritted his teeth through the pain, which he said was so severe that he was prescribed painkillers.
“If you had COVID, you could be honest about what’s going on,” said Paul, who is gay. But even though he works at an LGBTQ-friendly company, he didn’t want to tell co-workers he had MPX and feel them silently speculating about his sex life.
He had to isolate for 31 days as new lesions emerged and healed on his body. “Had I not had a job that allows flexibility,” he said, “I would have been screwed.”
The Centers for Disease Control and Prevention has stated that “ideally, people with monkeypox would remain in isolation for the duration of illness.” The California Department of Public Health has warned that the virus can spread after symptoms begin and until all lesions are fully healed, with a new layer of skin having formed over the lesions.
Under state guidelines, people infected with MPX can return to the workplace after that happens and all other symptoms are gone for at least two days.
However, if their work does not involve physical contact or “settings of concern” such as schools, health facilities and homeless shelters — and virtual work is not possible — the state guidance says they can go back to work a few days after their fever or respiratory symptoms have disappeared, new lesions have stopped popping up for two days, and any lesions that cannot be covered are fully healed.
If they do so, they are still supposed to take precautions, including wearing a mask and covering any unhealed lesions with clothing or bandages.
Dr. Tomás Aragón, director of the California Department of Public Health, said that some MPX lesions may be in areas where there is no risk of exposing other people, and “we wanted to put together guidelines that are more practical for those situations.” Before California set out its guidelines, many patients said they had gotten little leeway to exit isolation before all lesions had healed; some had been issued court orders to remain home.
In this global outbreak, the most common route of transmission has been “direct skin-to-skin contact with monkeypox lesions, and that’s including sexual contact but not limited to that, as well as close contact with household or contaminated items,” said Dr. Muntu Davis, county health officer for the L.A. County Department of Public Health. If lesions can be covered and someone doesn’t have respiratory symptoms, “the risk should be much lower.”
Aragón urged people to take advantage of any local programs that counties and others had already developed to support people amid the COVID-19 pandemic. Los Angeles County, for instance, is offering isolation housing in motels for people who are unhoused or have nowhere to safely isolate in their home during an MPX infection, according to its public health department.
In the Palm Springs area, C.J. Tobe said he knew of at least two people who had lost their jobs after getting the virus. DAP Health, the federally qualified health center where he serves as director of community health and sexual wellness, has delivered food to people unable to afford it and put up unhoused patients in hotel rooms as they wait out their isolation period.
“We’re basically relaunching everything that we did through COVID to make sure that our patients, that our community members, are supported and safe,” Tobe said.
Getting diagnosed with MPX “can and will be financially crippling for those without adequate financial support and/or paid leave,” dozens of health and community groups warned in an August letter to state leaders.
They urged the governor to expand temporary eligibility under the state disability insurance program to cover workers who do not contribute to it, “in much the same way that eligibility for unemployment insurance was expanded during COVID-19.”
Gig workers, people working temporary jobs, and those who are self-employed are unlikely to be covered by the program as it stands, said Phil Curtis, director of government affairs for APLA Health, one of the groups that signed the letter.
The letter also urged state officials to consider providing financial relief for employers to extend paid leave to workers who need time off for MPX vaccination, testing or isolation.
Sex workers are fretting about how to keep themselves safe from the monkeypox virus.
When Juan fell ill with the virus, he decided not to use the five days of sick leave that his company provided because he knew he would need to isolate much longer. “I knew that if I took more than whatever sick days I had, then I would have to be short of that income and I could not afford that,” said the Orange County resident, who asked to use only his first name to protect his privacy.
Instead, the 54-year-old worked from home. His doctor prescribed him painkillers, but Juan avoided taking them during the day, to avoid being groggy while working remotely. During video meetings, he shut off his camera so no one would see lesions on his face. When those meetings finally ended, he would soak in a tub to ease the pain.
“It was the only relief I really felt,” he said.
Juan didn’t lose out on income but had added expenses from getting groceries and other necessities delivered.
An MPX infection can be costly in other ways: Bolding, the restaurant worker, said he had to pay more than $300 out-of-pocket for a testing appointment, skin swabs and lab fees because he didn’t have health insurance. And even after an infection wanes, some patients have been left with visible scars that can be costly to remove.
The financial and emotional burdens of isolating for weeks are one reason that some physicians have argued to expand access to Tpoxx, an investigational drug that has shown promise in sending lesions into retreat. Some researchers have also argued that isolation guidance is excessively strict if MPX is chiefly being spread through sexual contact rather than other forms of transmission, a question that has been the center of ongoing research and debate.
In Hayward, Ivan said that a clinic had helped him out with gift cards to try to soften the financial blow from having to stop working for weeks, but “the economic effect is huge.”
Back at work, he wears a mask to protect himself, but also to hide the scars left over from the virus. As a newcomer to the country, Ivan has been frustrated with the ways it can fail workers who fall ill.
“They say that the United States is No. 1 in terms of resources,” he said in Spanish. “But that’s not true.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.