With COVID emergency ending, will I have to pay for tests?

- Share via
States of emergency issued in response to the COVID-19 pandemic are fast approaching their expiration dates, but Californians will still be able to get help covering the cost of a key resource: testing.
While a federal requirement that insurers reimburse covered individuals for eight at-home COVID-19 tests per month will end along with the nationwide public health emergency on May 11, state lawmakers have acted to continue this requirement for most health plans regulated by the California Department of Managed Health Care. This covers around 23.5 million people with private insurance or health plans managed by Medi-Cal, the government insurance program for low-income residents.
State lawmakers also have passed legislation requiring health plans and insurers to cover anti-COVID drugs.
Here is what you need to know:
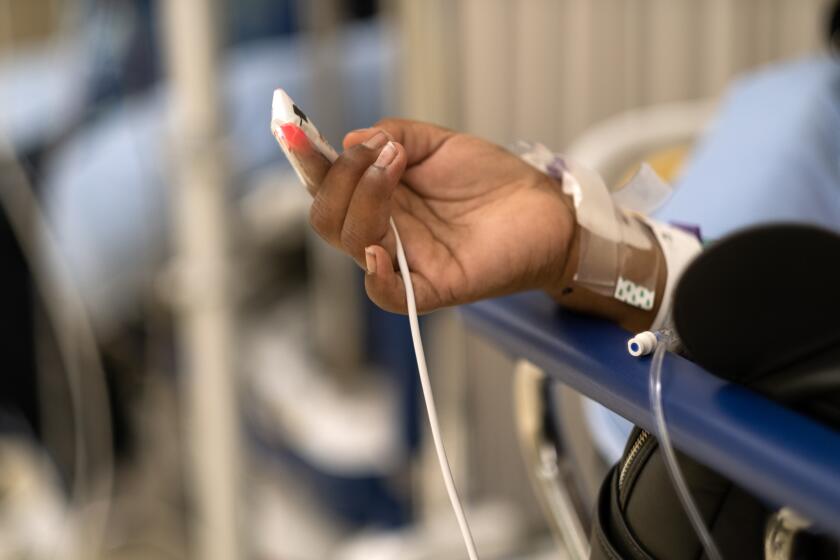
Transitioning out of the COVID emergency phase could eventually spell the end of universal access to free vaccines, treatments and tests.
Will insured Californians still be eligible for free at-home tests?
Yes. Starting in January 2022, federal officials ordered health insurers to reimburse customers for eight over-the-counter home COVID-19 tests per month per covered person. In other words, a family of four would be eligible to be reimbursed for 32 COVID tests per month, at up to $12 per test.
That federal mandate is in place only as long as COVID-19 remains a public health emergency, however.
In California, state lawmakers and Gov. Gavin Newsom acted in recent years to continue this benefit. Senate Bill 510, authored by then-state Sen. Richard Pan, requires health plans to cover costs associated with COVID-19 testing and immunization — even after the federal public health emergency expires. That bill easily cleared both houses of the Legislature, and Newsom signed it in October 2021.
Another Pan-authored bill, SB 1473, was approved in September and requires health insurers to retain current reimbursement rules for six months after the federal public health emergency ends. According to state health officials, this means insured people can still seek reimbursement for at-home COVID-19 tests purchased from stores or online retailers, just as they have for the past year.
More people have suffered severe sepsis in California hospitals in recent years — including a troubling surge in patients who got sepsis inside the hospital itself, state data show.
But starting in early November — six months after the end of the public health emergency — things change slightly. Insured individuals will need to get COVID-19 tests through an “in-network” provider to avoid charges. So it’s best to contact your health insurer to figure out how to continue getting free or reimbursed tests.
“Health plans must continue to provide eight over-the-counter at-home tests per month to enrollees at no cost. Plans can meet this requirement by providing the tests directly to enrollees through in-network providers and pharmacies, which could include [retail outlets] if they are considered in-network for the plan,” the California Health and Human Services Agency said in a statement to The Times. However, if the health insurer considered retail stores such as Amazon, CVS, Walgreens or Rite Aid “out-of-network,” health insurers can begin charging fees to the enrolled person for over-the-counter COVID-19 tests.
Other parts of the U.S. may not maintain such requirements. The federal government will no longer order insurers to keep at-home tests free once the public health emergency expires.
“That does come to an end when the public health emergency ends,” White House COVID-19 response coordinator Dr. Ashish Jha said during an online forum with UC San Francisco Department of Medicine Chair Dr. Robert Wachter.
Jha said that he hopes “every insurance company will continue to cover COVID tests beyond that. ... It is the right thing to do.”
President Biden has informed Congress that he will end the twin national emergencies for addressing COVID-19 on May 11, as most of the world has returned closer to normality.
What about anti-COVID drugs and vaccines?
Even after the federal public health emergency ends, insured Californians will still get access to anti-COVID drugs at no cost. SB 1473 requires health plans to fully cover the costs of therapeutics, including antiviral oral pills that treat COVID.
Through early November, insured individuals can get such drugs from either in-network or out-of-network providers for free. But starting in early November, the insured person will need to stay in-network to avoid paying for COVID drugs.
COVID-19 vaccines will remain free nationwide for insured people since preventive services are free under the Affordable Care Act of 2010, and vaccines are a preventive service, according to Jha.
Unvaccinated people were more than seven times as likely to die from COVID-19 in Los Angeles County as those who received an updated booster during the latest coronavirus spike.
How about uninsured people?
The picture is a little murkier, but officials say nothing should change in the near term.
“On May 12, you can still walk into a pharmacy and get your bivalent vaccine for free,” Jha wrote on Twitter last week. “On May 12, if you get COVID, you can still get your Paxlovid [anti-COVID pills] for free. None of that changes.”
The reason is the U.S. government has already purchased large quantities of vaccines and drugs and can still tap into that supply. But Congress has not funded COVID-19 pandemic efforts for more than a year, and those federal stockpiles will run out at some point.
Eventually, “we will transition from U.S. government-distributed vaccines and treatments to those purchased through the regular healthcare system, the way we do for every other vaccine and treatment,” Jha said last week.
COVID-19 remains a global health emergency, but the pandemic may be nearing an inflection point amid higher levels of immunity, the WHO says.
Federal officials are working to ensure vaccines and treatments remain readily available for the uninsured, he said.
“We’re working on a plan on that. But none of that needs to be implemented like next month because first, the [federal public health emergency] doesn’t end until May. But even after that, this stuff will be available for the uninsured and for everybody else for a while. So at some point over the summer into fall, you’ll see that transition,” Jha said.
Los Angeles County Public Health Director Barbara Ferrer said county health sites will continue to provide vaccines, anti-COVID drugs and test kits at no cost, including to those who are uninsured or underinsured. “We do need to work with the federal government and the state government to ensure that we’re able to continue those services way past the emergency declarations,” Ferrer said.
In the interim, she said, “as access to vaccines, boosters, testing and therapeutics is both easily accessible — and for almost everyone, it’s free — we do urge everyone to appropriately use these life-saving tools.”
While wearing a face covering is still required in certain select settings and still encouraged aboard public transit, the decision for most should now be considered a matter of personal preference.
The California Department of Public Health has urged healthcare providers to prescribe anti-COVID drugs such as Paxlovid and molnupiravir more often. Officials have raised concerns that too many providers have avoided prescribing the treatments despite their lifesaving potential.
“There is ample supply of COVID-19 therapeutic agents, but they have been underused — especially among populations disproportionately impacted by COVID-19, including communities of color, low-income communities, and residents of long-term care facilities,” state health officials said in a recent memo to healthcare providers.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.