A simple test is helping thousands of diabetics in L.A. County who face an increased risk of going blind
- Share via
After years without an eye exam, patients would show up at Dr. Lauren Daskivich’s clinic suddenly unable to see. They were diabetics who had bled into their eye, marring their vision.
“It’s like a ticking time bomb and patients have no idea, but when the bomb goes off they definitely do,” said Daskivich, an ophthalmologist. “We were just seeing patients far too late.”
The condition, called diabetic retinopathy, is the leading cause of blindness among working-age adults nationwide. A simple test can detect and help treat the problem, but four years ago most diabetics in Los Angeles County’s massive healthcare system weren’t getting screened.
It was a months-long wait to see an eye doctor in the county system. Sometimes people didn’t even know they had diabetes. “You’d get these patients and they’d ask you for their diabetes meds,” said Daskivich, who oversees all eye care services for the county.
A few years ago, Daskivich began testing as a way to help ease the backlog and improve patient care. Medical assistants in primary care clinics can now take photographs of diabetics’ eyes and send those images to ophthalmologists who analyze them. If the photos reveal damage, the patients are sent to eye doctors.
Patients might still wait months for that appointment, but the wait time for the initial screening for those using the new system dropped by 89%, according to data Daskivich published this year.
The project is one of many novel ways healthcare providers are trying to improve access to specialists since the expansion of health insurance under the Affordable Care Act, said Melissa Buckley, who funds technology innovations at the California Health Care Foundation.
The law known as Obamacare assured healthcare coverage for millions of previously uninsured people, but did not guarantee there would be enough doctors to see them.
So some healthcare systems have offered patients or their primary care physicians the chance to use video chat, text or email to get advice from a specialist sooner.
“That’s a huge, huge area that we’re all focused on, primarily because access to specialty care is a huge challenge,” Buckley said. “[These initiatives] are getting lots of traction because there’s such a need.”
Such innovations, however, often illustrate not only the possibilities but also the limitations of using technology to solve physician shortages.
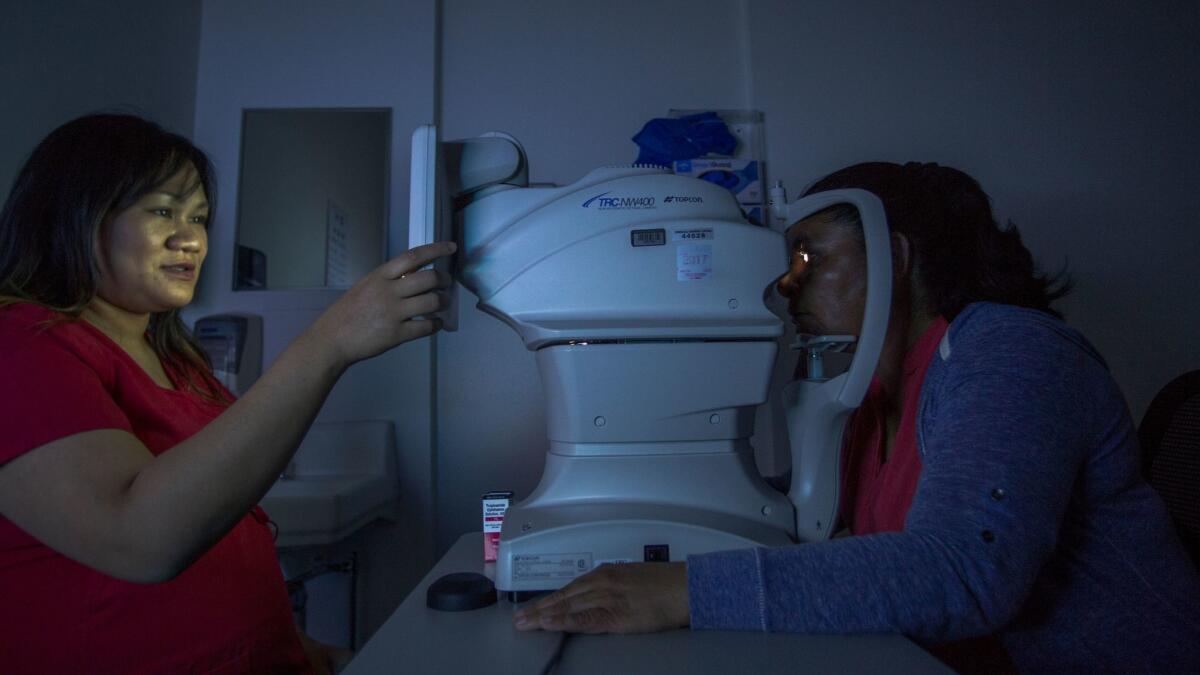
Rosa Guzman, 46, was diagnosed with diabetes on a recent Monday morning at a primary care clinic at Los Angeles County-USC Medical Center in Boyle Heights. Later that morning, she was reading an eye chart as medical assistant Silvia Fletes pointed to smaller and smaller letters.
Fletes then took photos of Guzman’s eyes. A machine flashed in the darkness, and images of cloudy pink circles intersected by red lines appeared on a computer screen. Guzman left a few minutes later.
When Daskivich and Dr. Barbara Rubino, an internist, learned that Guzman had been screened only hours after being diagnosed with diabetes, they high-fived. Getting an eye test on demand was essentially impossible a few years ago.
“That was the ultimate, ultimate goal,” Rubino said.
The high blood sugar levels associated with diabetes can damage the blood vessels in the retina, which makes them leak fluid or bleed and distort vision. But diabetic retinopathy doesn’t usually have symptoms until people begin bleeding into their eye.
Diabetics should be screened annually, but only about 60% nationally get their eyes checked every year.
Four years ago, the situation was even worse in L.A. County’s public health system, the nation’s largest, serving more than 800,000 patients per year. Thousands of diabetic patients from hundreds of primary care clinics were referred to 10 eye clinics, where waits for screenings could be more than eight months, Daskivich said.
When medical assistants began taking photos of diabetic patients’ eyes, screening rates increased from 41% to 57%, according to a paper Daskivich published in March in the journal JAMA Internal Medicine.
For those whose eyes were checked, the median wait time for screening dropped from five months to 2½ weeks, the paper found. They even found eye problems that weren’t diabetes-related, like glaucoma or cataracts, in about one of every 10 patients.
The screening rates have continued to improve and now are about 65%, but they still are far from perfect, Daskivich said. Patients who do end up needing an eye appointment can move to the front of the line if it’s urgent, but there are typically 3,000 people waiting for eye care at any given time.
“In the safety net you’re always going to have limited resources ... we’d love to see a person tomorrow,” Daskivich said. “We certainly do have some work to do to get there, but I think we’re moving in that direction.”
Though public health systems might not be flush with cash, they actually have a natural advantage when it comes to improving care coordination, Buckley said.
Doctors are usually paid every time they see a patient, so they wouldn’t get paid to analyze a photograph for another doctor — even if that might be the most efficient way to divide the work. In Los Angeles County’s public medical system, in which doctors are typically salaried, it’s easier to make these sorts of changes.
“It’s easy to make that happen in L.A. because it’s a closed system … they are just creating a communication bridge,” Buckley said. “Outside of L.A., it’s harder to make that spread.”
For instance, the county has been able to implement a system called eConsult that allows doctors to message each other about patients, reducing unnecessary appointments and wait times to see specialists. That system would be harder to implement elsewhere because each doctor needs to figure out a way to get paid. The Affordable Care Act aimed to move away from the traditional “fee-for-service” model to alleviate some of these problems, but it’s been a slow shift.
For a doctor who has just diagnosed a patient with diabetes, the new systems offer peace of mind. Now they can send them next door to get their eye photo, and they can track the referral through eConsult. Not that long ago, they didn’t have any way of making sure patients’ eyes were actually checked.
“You’d cross your fingers and hope they would get their eyes screened,” Rubino said. “They usually wouldn’t.”
soumya.karlamangla@latimes.com
Twitter: @skarlamangla
ALSO
Can virtual reality reduce high blood pressure at a church in South L.A.?
Doctors turn to the power of peer groups to help diabetics
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














