Readers React: Collecting on a chemo patient is a side effect of our sick, profit-driven healthcare system
- Share via
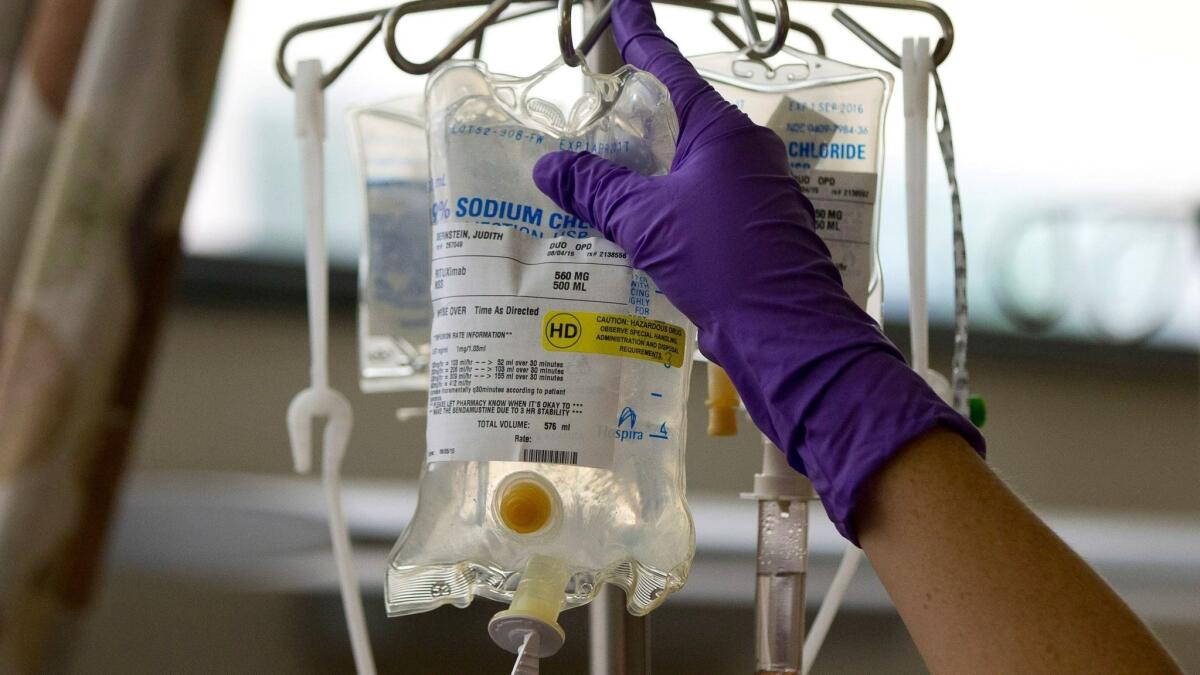
To the editor: I read with interest and chagrin David Lazarus’ column on a cancer patient who was hit up for the full cost of a drug, for which she had been approved by her insurer, in the middle of her treatment. As a physician with more than 50 years of practice behind me, I have seen many similar instances of unconscionable acts by insurance companies.
I take issue with one of Lazarus’ statements: “To be sure, insurance companies are entitled to make money for managing people’s healthcare risk.”
The profit motive is at the core of what I believe to be the major problem with healthcare in the United States. Healthcare is not a commodity and it should not be the source of profit for insurance companies. It should be the right of all residents to receive care through a government-funded, single-payer system.
As more instances like these come to light, I believe the political will to enact a single-payer system will strengthen and change healthcare in this country.
Ronald F Young, MD, Laguna Beach
..
To the editor: My wife is also going through chemotherapy treatments for breast cancer. For us, this has been a very hard and lengthy process.
I’m a bit unclear as to why the insurer is to blame here. It agreed to cover a particular immunity-boosting drug purchased through the Express Scripts pharmacy, with the injections to be administered by a caregiver rather than the oncologist. This is an increasingly common cost-cutting practice among insurers.
My wife is on the same type of injected medication. She is being treated by Kaiser Permanente, which requires us to use its pharmacies and supplies us with the syringes. I administer one injection per day for five days after each round of chemotherapy. We have no problem with this.
To me, the real issue is the exorbitant cost of the injections for someone who has no choice but to pay for it themselves. Fortunately, insurance is covering the cost for us, but with the dismantling of the Patient Protection and Affordable Care Act by the Trump administration, people dealing with this life-threatening illness in the future may not be so fortunate.
Larry Levy, Winnetka
..
To the editor: I’m convinced Express Scripts created its subsidiary specialty pharmacy, Accredo, specifically to produce so many obstacles to obtaining prescribed medications that coverage is effectively denied.
If just a few percent of insured patients give up after repeated, lengthy phone calls and Accredo’s other rope-a-dope techniques, Express Scripts saves untold millions of dollars.
We earned our coverage. Why do we have to fight for it?
Thomas Bliss, Sherman Oaks
Follow the Opinion section on Twitter @latimesopinion and Facebook
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.









