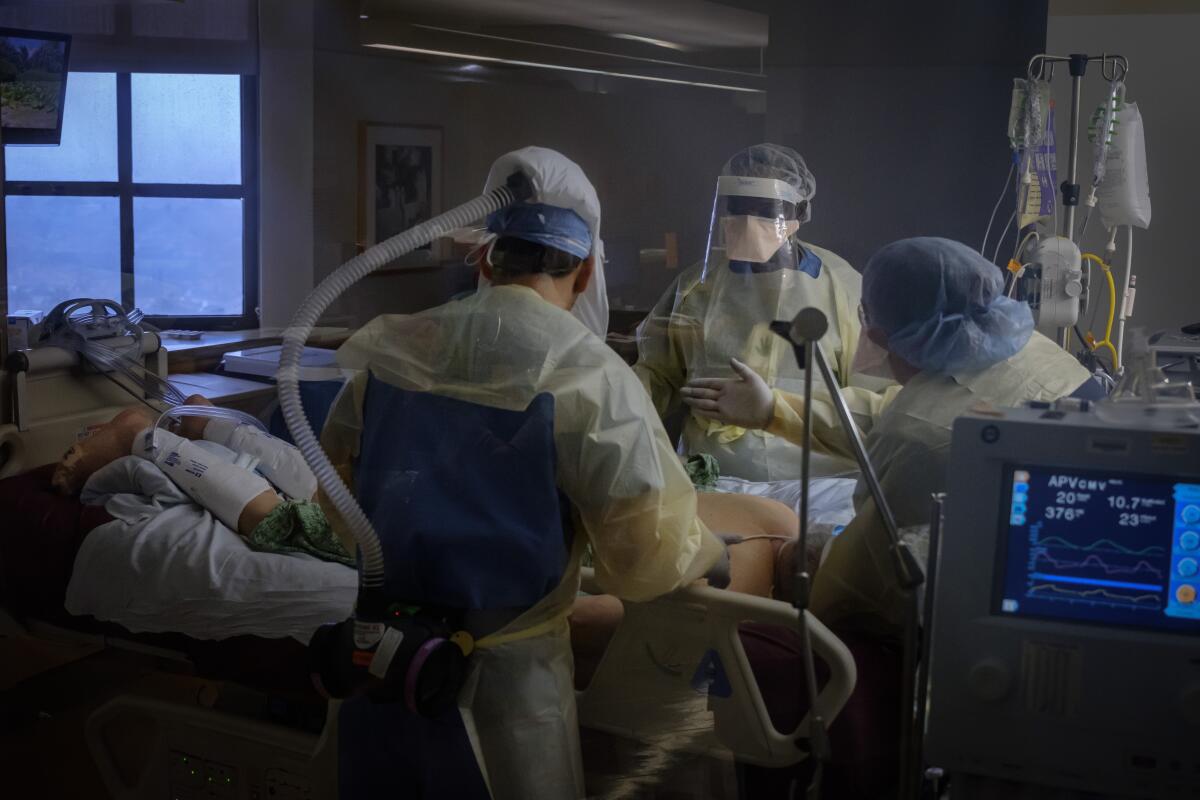
The trauma that comes after surviving COVID-19
- Share via
Since nearly half of all patients with severe respiratory failure who are placed on a ventilator die, we tend to declare victory if a COVID-19 patient comes off the machine alive.
But the reality is that many survivors of severe respiratory failure and other forms of critical illness fare poorly, even if they do beat their underlying disease. Their likelihood of developing PTSD, depression or anxiety is similar to that of soldiers returning from combat.
Many show symptoms of major cognitive dysfunction, some similar to moderate traumatic brain injury, others similar to Alzheimer’s. A multitude of physical and psychological injuries can contribute to this cognitive effect, with delirium showing the strongest influence. Delirium often manifests in patients as agitation or an inability to focus, and it has recently been associated with markers of anatomic brain injury.
After one year of recovery, half of previously employed post-ICU patients will be jobless.
I know these patients. I’m a critical care physician. Well before COVID-19, I counseled patients and their families on what they might expect following an intensive care unit admission.
I’ve learned that life beyond the ICU presents as a variation on a theme — while every patient is unique, there are shared experiences and struggles. There’s a diagnosis for these cognitive, physical and psychiatric consequences: post-intensive care syndrome. Yet most physicians don’t recognize it as a chronic condition nor do they manage it with the rigor it requires.
This is a medical challenge, but increasingly, it’s also a societal one. In the COVID-19 era, we’re going to need to design and support post-ICU recovery programs and then thoroughly evaluate their effectiveness.
Post-ICU recovery programs assemble multidisciplinary teams to address psychiatric and cognitive problems, physical debilitation and family stress. They adjust medications to minimize harmful side effects and ease patient transitions from the hospital to primary care settings.
Comprehensive post-ICU programs remain rare in the U.S., and evidence on their effectiveness is just emerging. Recent studies suggest targeted post-ICU interventions can improve survivors’ quality of life and reduce hospital readmissions.
In developing and strengthening these programs, we should place special emphasis on the problems of job loss and reentry. After lockdowns to prevent the spread of the coronavirus are safely lifted, post-ICU patients will need our assistance more than ever to overcome their unique challenges amid a devastated economy.
Employment isn’t traditionally a healthcare issue, but it has great influence over an individual’s health. Jobless ICU survivors face substantially increased risk of a heart attack and poor mental health outcomes, compared with survivors who are employed. Work confers more than financial stability — it often provides meaning and community.
A program designed by Joanne McPeake, a researcher on critical care outcomes, in Glasgow, Scotland, focused on identifying work needs and accommodations. She helped post-ICU patients partner with their employers to devise ways to handle their limitations. Some 88% of participants in the program returned to work or volunteer roles compared with a historical rate of 46% for similar patients.
Part of the current chasm between healthcare and work stems from our limitations as clinicians. We are excellent at describing certain work restrictions, such as “don’t lift more than 10 pounds for two weeks” after an appendix removal. That’s simple and straightforward. But for someone going home after a prolonged COVID-19 hospital stay, instructions for recovery require more nuance.
These patients may be able to do most home tasks, read short newspaper articles, and write notes to friends, but they are likely to encounter difficulty remembering to pay bills, have short-term memory deficits and experience anxiety.
We clinicians don’t have the language to communicate this effectively to an employer, much less help them adjust a worker’s job appropriately. With thousands of COVID-19 patients admitted to ICUs — and thousands more to follow before the pandemic ends — we need to change this.
COVID-19 is exposing the brutal reality of critical care. For the first time, the idea of being paralyzed on a ventilator is entering people’s conscience as a real possibility. As coronavirus infections and deaths start to plateau, our definition of successful recovery should evolve to account for more than physical survival.
In time, most people will know survivors of this disease, some of whom will have overcome terrible odds and will still struggle to return to a semblance of normal life. We must focus now on meaningful ways to support them along that journey, which doesn’t end after they leave the ICU.
Marissa Wagner Mery is an assistant professor of surgery and perioperative care at the Dell Medical School at the University of Texas at Austin.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.