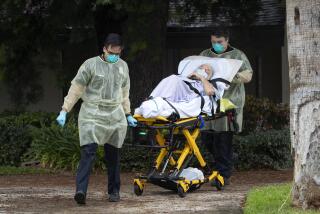
Letters to the Editor: Nursing homes are shoestring operations. No wonder elderly patients are dying

- Share via
To the editor: Your article concerning oversight issues at nursing homes gives the wrong impression of this industry. For more than 20 years, I sold to and visited long-term care facilities across the U.S.
First, unlike acute care hospitals, nursing homes are not staffed by registered nurses and do not have a highly trained infection control department. Many of the workers are paid minimum wage and have minimal nursing training. Many of them have little more than previous work at other nursing homes.
Second, nursing homes do not have the space or ability to segregate and isolate residents.
Third, nursing homes are at the bottom of the supply chain in terms of personal protective equipment.
Last, this is pennies-on-the-dollar business, and most residents in long term are not covered by Medicare (except for 100 days after leaving an acute-care hospital). Many are covered by Medicaid, which pays half of the cost to care for a resident.
I do not condone sloppy inspections, but like the article stated, once the inspectors leave, nothing changes. My mother spent two months in a nursing home that put three residents in each room, so it is no wonder that the coronavirus is spreading so easily.
Mike Walsh, Yorba Linda
..
To the editor: Please consider that the reason regulators failed to identify problems in the nursing homes was due to the unpreparedness of the federal government. There was inadequate testing, a shortage of PPE and no contact tracing.
Add this to the fact that underpaid nursing home staff must sometimes work multiple jobs to cobble together an income that’s enough to support a family.
The spiraling cases of COVID-19 should be attributed not to inspectors and nursing staff, but to the lack of resources and planning from the federal government.
Elizabeth Gross, Beverly Hills
The writer is a long-term care pharmacist consultant.
..
To the editor: Since 40% of all California COVID-19 deaths are in our nursing homes, there seems to be a dire shortfall in care.
There must be thousands of terrified seniors in homes watching their fellow patients die, and they cannot escape their fate. The incompetence of the county and state medical authorities has been manifest.
This seems closer to gross negligence than an “oversight issue.”
Warren Larson, Sunland
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.