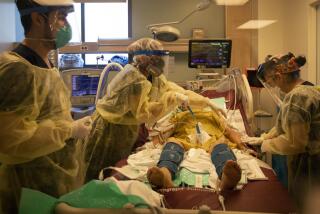
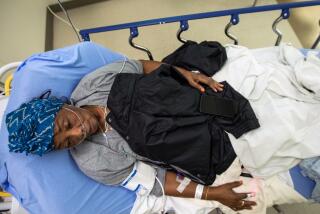
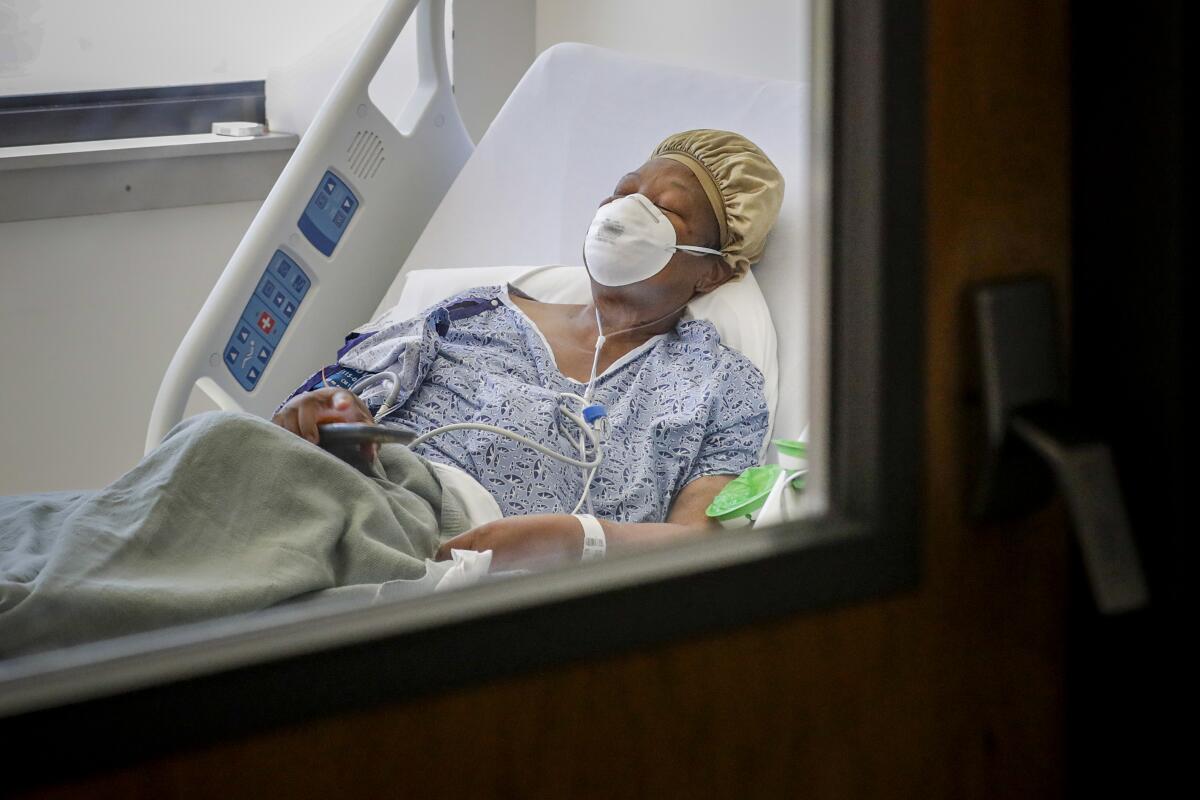
Coronavirus kills Black people at twice the rate as white people: Here’s what we can do about it
- Share via
Dr. Georges Benjamin knew that when the coronavirus landed on U.S. shores, it was going to be especially bad for Black Americans.
“We see it all the time” he said. “We’ve not had a new disease enter the community where this hasn’t happened.”
As the director of the American Public Health Assn. since 2002, he knew there would be differences in who became sick and who died — and that they would break down along racial lines. What he didn’t expect, was the size of those differences.
“That it happened wasn’t a surprise,” he said. “It was the scope of it.”
In Los Angeles County, Black people are dying of COVID-19 at twice the rate of white people, with 26 deaths per 100,000 Black residents compared to 13 deaths per 100,000 white residents.
And across the country, Black people have made up 22% of all COVID-19 even though they represent just 12.7% of the population, according to the Centers for Disease Control and Prevention.
Even before the pandemic, the disparities in health outcomes between Black and white people in the U.S. were staggering.
Black people are 44% more likely to die from a stroke than non-Hispanic whites, twice as likely to suffer from hypertension and 72% more likely to have diabetes, Benjamin said. They’re also 20% more likely to have asthma, and if they do, they’re three times more likely to die as a result.
And there’s more: Black women are 40% more likely to die from breast cancer than white women, 52% more likely to die of cervical cancer, and three times more likely to die from complications related to pregnancy. Black men are twice as likely to die from prostate cancer than their white peers, Benjamin said.
“There has not been a single year since the founding of the United States when people of African descent have not been sicker and died younger than white people,” said Dr. Mary Bassett, a former health commissioner for New York City and professor at Harvard’s T.H. Chan School of Public Health.
Some public health experts are bracing for a spike in COVID-19 cases in the wake of protests against police brutality.
The reason for this is clear, said Barbara Ferrer, director of the L.A. County Department of Public Health.
“The root cause of health inequities is racism and discrimination, and how it limits access to the very opportunities and resources each of us need for optimal health,” she said.
She also blamed the crippling effects of stress and fear that ripple through Black communities every time a Black person is shot, beaten or asphyxiated by the police.
“It is the consequence of that fear that we are seeing when we report on instance after instance of inequality in health outcomes,” she said.
So, now that the pandemic has laid them bare, what can we do about it? And specifically, how do we stop COVID-19, a disease that biologically should pose an equal risk to everyone, from disproportionately killing Black people?
There are no easy answers, but that does not mean we are helpless.
Health experts from around the country said there are concrete steps we can take to create better outcomes for all Americans in this pandemic and beyond.
Here are some of their thoughts.
Name the issue: Structural racism
“The immediate first step is reckoning with the legacy of racism in our country,” said Dr. Aletha Maybank, chief health equity officer of the American Medical Assn. “If we don’t do that, then we don’t get at the root causes of why these inequities show up in the first place.”
The coronavirus has stripped away the veil around all kinds of disparities in this country, not just those related to health, she said.
“The folks who have gotten sick in Black and brown communities are more likely to live in overcrowded housing, and be relegated to jobs that are considered ‘essential work,’” such as driving buses and stocking grocery stores, she said. “This is not brought on by choice, but what they have been forced into due to policies around education, housing and economics that have excluded communities of color.”
The prison system has also been a big driver of the virus’ spread, and that’s another place where Black people are vastly overrepresented.
We can’t dismantle structural racism if we don’t name it, she said: “People need to understand what it is, and how it shows up in their jobs and inside themselves.”
Give better protections to essential workers and others
There are two parts of getting a disease and dying from it, Bassett said. The first is related to exposure, and the second is the risk of dying once you get it.
Black Americans have higher rates of many diseases known to raise a person’s risk of dying from COVID-19, including asthma, hypertension, diabetes and obesity. There are structural reasons for that, and it could take years to address them, she said.
But in the shorter term, we can do a better job of keeping people — including those delivering goods, stocking warehouses, staffing grocery stores and working in meat packing plants — from being exposed to the virus in the first place.
That means ensuring that all essential workers have access to masks and hand-washing stations, and that they can stay away from other people.
“If we could cut down on the likelihood of people getting exposed to COVID, then we wouldn’t have to worry so much about their risk of dying from it,” she said.
Acknowledge that not everyone is effected equally
An idea often repeated in policy circles is that a rising tide lifts all boats, said Reginald Tucker-Seeley, who studies health disparities at USC’s school of gerontology. The idea is that a collective response to a pandemic — such as implementing stay-at-home orders or making testing available to all should helps protect everybody equally from the disease.
But that assumes we all have jobs that allow us to work from home, and that we all have the time and the ability to get to a testing site.
Officials fear protests are ‘super-spreader’ events for coronavirus. Marchers say worth the risk
We are not all on the same ship, Tucker-Seeley said. Some people are riding out the pandemic in yachts, while others are struggling to stay afloat on perilous rafts. As a result, when interventions are introduced, we’re not equally situated to benefit from that “rising tide.”
“If your ship is OK, then you need to be advocating for those on other ships that are not as well-equipped,” he said.
That can be as simple as wearing a mask, abiding by social distancing recommendations even if your own personal risk of dying from the disease is low, or staying home to protect your neighbors who may be more at risk than you are.
It could also mean voting for or donating to candidates who say eliminating health disparities across racial and ethnic groups is a top priority.
“We are all in this together, and as individuals it should be our responsibility to protect those folks who don’t have the same resources to weather this storm,” he said.
Make testing accessible for all
From the earliest days of the pandemic, there were inequities around who was getting tested for the virus and who wasn’t, Benjamin said.
“The mantra was, ‘If you have symptoms go get tested,’” he said. “But there was unequalness in the ability to get tested.”
Many testing sites are drive-through sites, which means you need to have a car to get checked. And if there are no sites in your neighborhood, you might have to take two buses and walk two blocks to get a test. A person who is feeling sick would probably choose to stay home instead.
Early on, some people got the test by calling up their primary care provider. Others didn’t have a primary care provider — and when they went to a hospital emergency room to get a test, they were turned away.
He’d like to see testing sites placed closer to bus lines and train stations, and for tests to be offered at off hours so people don’t have to take time off work to get checked. Mobile test sites could roll into communities that are known to be most at risk, such as those that are crowded or have higher percentages of essential workers, he said.
There also needs to be robust contact tracing so that anyone who was in close contact with an infected person can easily access a test.
If people know they have the virus, they can isolate themselves and keep from passing it along to others in their community, he said. That’s why equal access to testing is so important.
Fight for social justice — it helps
There are many societal and structural factors that have contributed to racial disparities in COVID-19 deaths — address any of them and you will improve outcomes for Black and other marginalized communities, said Tina Sacks, a professor at UC Berkeley’s School of Social Welfare who studies racial inequalities in health.
“I tell my students, ‘Whatever it is that makes you want to get out of bed these days, anything you can do in service of social justice helps,’” she said.
Fair housing would improve COVID-19 disparities by reducing crowding, she said. So would universal healthcare and family-friendly policies to support women who want to work.
“Our society needs to be reorganized,” Sacks said. “This is a wake-up call.”