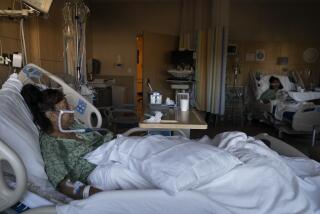
In Louisiana, coronavirus death toll mounts

- Share via
NEW ORLEANS — COVID-19 has moved quickly across Louisiana, killing hundreds and infecting thousands of all ages and walks of life in the Pelican State. Among the dead this last week: A 46-year-old registered nurse, a 33-year-old member of Gov. John Bel Edwards’ staff and 85-year-old Ellis Marsalis Jr., the renowned Jazz patriarch.
On Thursday, the state reported a 40% increase in new cases, 9,150 total infections and 310 deaths. Edwards called the spike “jarring,” but said it resulted from a testing backlog at private labs and was not a measure of how well mitigation efforts like social distancing have worked. Edwards was among governors who issued stay-at-home orders earlier this month to stop the virus from spreading, but some have resisted, including at least one church that has continued to hold services.
“The situation remains concerning, but every Louisianan has the power to change the path we are on,” the Democratic governor said Thursday. “Think of your neighbors, and please stay at home.”
Edwards has warned that the state could run out of hospital beds and ventilators as soon as Sunday. As the governors of nearby states this week forced those leaving Louisiana to quarantine for two weeks, many in New Orleans were reminded of being branded “Katrina refugees” when they evacuated. At Tulane Medical Center, intensive care Dr. Joshua Denson echoed a concern of fellow Katrina survivors: that the federal disaster response to the outbreak in New Orleans would fall short.
“New York is going to get what they need, but I worry we’ll get left out,” said Denson, who emerged from quarantine last week after diagnosing the hospital’s second case of the virus.
The city and state have high rates of obesity, diabetes and other underlying conditions, he noted, so the outbreak has reached more age groups. Of 89 people who died after testing positive for COVID-19 in Louisiana last week, 41% had diabetes; over a third had chronic kidney disease and 28% were obese, state health officials said.
Denson has seen a “slow, steady onslaught” of patients placed on ventilators for several weeks, some in their 20s and 30s. More than half of the intensive care COVID-19 patients he has seen have died; others were near death this week.
“They probably will be left with a severe disability. My recommendation would be a palliative care approach, but it’s hard to have those conversations” with patients isolated from relatives due to the virus, he said.
New Orleans hospitals were converting operating rooms and other units into COVID-19 treatment areas this week, searching for additional staff, ventilators and dialysis machines for the coronavirus patients, whose kidneys often fail. National Guard troops were racing to build a temporary 3,000-bed hospital in the city’s convention center.
The specter of patients converging on the convention center conjured images of the overwhelmed Superdome after Katrina.
“We’re not talking about a shelter; we’re talking about hospital-level care,” with nurses and privacy barriers, said Dr. Joseph Kanter, assistant state health officer and medical director for the New Orleans region.
Kanter said state officials were preparing for up to 4,000 additional patients, a quarter of whom will need ventilators. They ordered 14,000 — 5,000 of them from the federal stockpile. President Trump has promised to send 150. It’s not clear how many will go to New Orleans, Kanter said.
As of Thursday, 47 nursing homes across the state had reported COVID-19 outbreaks, including Lambeth House in New Orleans, where 53 residents have tested positive and 13 have died.
In the city’s Uptown neighborhood, 63-year-old Theresa Elloie died of the virus on March 24. Elloie was a regular at her family’s bar, Sportsman’s Corner, a Mardi Gras second-line parade stop where she would craft holiday corsages. She didn’t have any underlying conditions and initially suffered mild flu-like symptoms before being hospitalized on a ventilator around St. Patrick’s Day, her son said.
“They did everything they could,” said Leon Elloie, 39. “Everything just started failing.”
He and other relatives have self-quarantined.
“It look like anybody can get this,” he said.

Down the street from Sportsman’s Corner last weekend, 10 neighbors who knew Elloie rested in the shade of a community sycamore tree, sipping beer. Two men set up a card table to play dominoes, one with a surgical mask around his neck. No one else had masks or gloves or was practicing social distancing. The group said they didn’t see the difference between gathering under the tree or on someone’s porch, as others had.
Hairstylist Keyoka Perkins said she instructed her five children, ages 5 to 22, to stay home to avoid infection. “But I keep going out, so it may be defeating the purpose,” she said.
Hundreds attended a Pentecostal church Sunday despite the governor’s order to avoid large gatherings.
Kevin Murray, 54, who works for the local sewer and water board, said his 38-year-old daughter was quarantined at home with symptoms.
“I know lots of people that’s infected with it,” he said.
Dr. David Mushatt, head of infectious diseases at Tulane University, was quarantined this week after being exposed to the virus, likely by two men he treated who didn’t initially appear to have it but later tested positive.
“The intensity of the epidemic is very high here,” Mushatt said by phone from home. “Our hospitals are very stressed right now.”
The virus has spread among healthcare workers, even though New Orleans hospitals have set up areas in recent weeks to treat new patients suspected of having the disease. An estimated 25% of those with the virus don’t have symptoms, according to studies from China.
Tulane doctors recently began tracking COVID-19 patients for a study, Denson said. Medical students got thousands of surgical masks from industrial suppliers. The university’s primate center figured out how to decontaminate hundreds of used masks with hydrogen peroxide vapor. Cajun Navy volunteers, accustomed to helping neighbors during hurricanes, brought more.
“The supply bottleneck seems to be improving,” said Ecoee Rooney, president of the New Orleans District Nurses Assn. and president-elect of the state nurses association. “There are resources that are pouring in to our region now.”
But a New Orleans healthcare provider who asked not to be identified because he wasn’t authorized to speak said his hospital was still running low on masks and other protective gear, and “we’re getting new guidelines about how to conserve every day.”
COVID-19 patients outnumbered other admissions to his hospital 10 to 1, he said.
Louisiana’s governor forced historic bars and restaurants to close this week, leaving many unsure when — or if — they will reopen.
“Almost all of our ICU beds are currently dedicated to caring for people with COVID. We have dozens of people on ventilators for COVID,” he said. “Every team has become a COVID team. It’s spooky, and it’s similar to what I hear from New York. New Orleans is a very vulnerable city.”
A New Orleans nurse who also asked not to be identified said she was forced to reuse N95 masks this week with COVID-19 patients in intensive care.
“Anytime you reuse any equipment that has been in the vicinity of a patient who has tested positive, there’s a concern for contracting COVID,” she said. “We have to do the best we can with what we have.”
She hasn’t had to make patients share ventilators, but said colleagues were preparing to. They were only allowing relatives to see dying patients through a window, she said. Nurses had to keep their distance, too.
“Normally If I’m with somebody at end of life and their family can’t be there, I’m going to be in there holding their hand as they pass away,” she said. “But we can’t do that because we’re concerned we might catch this. It would have been using up valuable [protective equipment] that we need to take care of other people.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.